Abstract
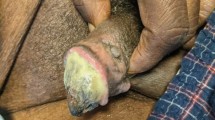
Calciphylaxis is a rare systemic condition usually seen in patients with end-stage renal disease. It is characterised by pathological calcification of dermal blood vessels, causing ischaemia and necrosis in the skin and subcutaneous fat. The lesions are usually small but, in extreme cases, may be very extensive and may mimic necrotising fasciitis, prompting extensive surgical debridement. We describe the challenges faced in managing such a case. A 38-year-old female patient was admitted to another hospital with widespread progressive truncal skin necrosis. A provisional diagnosis of necrotising fasciitis was made, and she underwent debridement of 32% of her total body surface area (TBSA). However, her condition rapidly deteriorated and she was transferred to our burn centre for further management. Diagnosis of calciphylaxis was based on clinical features and confirmed by tissue biopsy. Characteristic findings of progressive skin and fat necrosis at the wound margins with healthy underlying fascia and muscle were recognised from previously treated cases of calciphylaxis; however, the absence of renal disease proved misleading. Non-uraemic calciphylaxis is very rare but can, as in this case, be associated with alcoholic liver disease. At our centre, the patient required prolonged ventilation and supportive treatment in burns critical care, combined with intensive wound management, repeated episodes of debridement, temporary wound cover using human skin allografts and reconstruction using split-thickness autograft. We report this case to alert others to this rare condition as a possible diagnosis in patients presenting with extensive panniculitis. We discuss associations, diagnostic difficulties, novel therapies and the importance of multidisciplinary care in managing these complex cases.
Level of evidence: Level V, diagnostic study.



Similar content being viewed by others
References
Wichienkuer P, Naugler W, Wusirika R (2011) Calciphylaxis in a patient with acute kidney injury and alcoholic cirrhosis. Clin Nephrol 76(6):499–503
Weenig RH, Sewell LD, Davis MD, McCarthy JT, Pittelkow MR (2007) Calciphylaxis: natural history, risk factor analysis, and outcome. J Am Acad Dermatol 56(4):569–579
Rogers NM, Coates PTH (2008) Calcific uraemic arteriolopathy: an update. Curr Opin Nephrol Hypertens 17(6):629–634
Nigwekar S, Kroshinsky D, Nazarian R, Goverman J, Malhotra R, Jackson V, Thadhani R (2015) Calciphylaxis: risk factors, diagnosis and treatment. Am J Kidney Dis 66(1):133–146
Nigwekar S, Wolf M, Sterns R, Hix J (2008) Calciphylaxis from nonuremic causes: a systematic review. Clin J Am Soc Nephrol 3(4):1139–1143
Ahmed S, Hood AF, Evan AP, Moe SM (2001) Calciphylaxis is associated with hyperphosphatemia and increased osteopontin expression by vascular smooth muscle cells. Am J Kidney Dis 37(6):1267–1276
Bleyer AJ, Choi M, Igwemezie B, de la Torre E, White WL (1998) A case control study of proximal calciphylaxis. Am J Kidney Dis 32(3):376–383
Fine A, Zacharias J (2002) Calciphylaxis is usually non-ulcerating: risk factors, outcome and therapy. Kidney Int 61(6):2210–2217
Vedvyas C, Winterfield LS, Vleugels RA (2012) Calciphylaxis: a systematic review of existing and emerging therapies. J Am Acad Dermatol 67(6):e253–e260
Selye H, Gentile G, Prioreschi P (1961) Cutaneous molt induced by calciphylaxis in the rat. Science 134(3493):1876–1877
Anderson D, Stewart W, Piercy D (1968) Calcifying panniculitis with fat and skin necrosis in a case of uraemia with autonomous hyperparathyroidism. Lancet 292(7563):323–325
Angelis M, Wong LL, Myers SA, Wong LM (1997) Calciphylaxis in patients on hemodialysis: a prevalence study. Surgery 122(6):1083–1090
Ng AT, Peng DH (2011) Calciphylaxis. Dermatol Ther 24(2):256–262
Mochel MC, Arakaki RY, Wang G, Kroshinsky D, Hoang MP (2013) Cutaneous calciphylaxis: a retrospective histopathologic evaluation. Am J Dermatopathol 35(5):582–586
Auriemma M, Carbone A, Di Liberato L, Cupaiolo A, Caponio C, De Simone C et al (2011) Treatment of cutaneous calciphylaxis with sodium thiosulfate. Am J Clin Dematol 12(5):339–346
Ning MS, Dahir KM, Castellanos EH, McGirt LY (2013) Sodium thiosulfate in the treatment of non-uremic calciphylaxis. J Dermatol 40(8):649–652
Nigwekar SU, Brunelli SM, Meade D, Wang W, Hymes J, Lacson E (2013) Sodium thiosulfate therapy for calcific uremic arteriolopathy. Clin J Am Soc Nephrol 8(7):1162–1170
MHRA drug information for sodium thiosulphate. http://www.mhra.gov.uk/home/groups/spcpil/documents/spcpil/con1489732048176.pdf
Wollina U, Helm C, Hansel G, Koch A, Schönlebe J, Haroske G, Köstler E (2008) Deep ulcer shaving combined with split-skin transplantation in distal calciphylaxis. Int J Low Extrem Wounds 7(2):102–107
Acknowledgements
The authors are grateful to the patient for consenting to the publication of this case report and photographs.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The authors have not received any funding for this case report.
Conflict of interest
Jonathan Cubitt, Anthony Short, Linsday Shanks, Allan Dawson, Claire Ware, Peter Drew, and David Williams declare that they have no conflict of interest.
Ethical approval
This case did not require ethical approval.
Informed consent
The patient has consented to publication of this case report.
Rights and permissions
About this article
Cite this article
Cubitt, J., Short, A., Shanks, L. et al. Non-uraemic calciphylaxis: a diagnostic and management challenge for the burns team. Eur J Plast Surg 41, 359–364 (2018). https://doi.org/10.1007/s00238-017-1358-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00238-017-1358-z