Abstract
Purpose
To describe the neuroanatomical correlates of unilateral congenital isolated oculomotor palsy by means of high-resolution MRI.
Methods
Children with a clinical diagnosis of congenital isolated oculomotr palsy and with a high-resolution MRI acquisition targeted on the orbits and cranial nerves were selected and included in the study. An experienced pediatric neuroradiologist evaluated all the exams, assessing the integrity and morphology of extraocular muscles, oculomotor, trochlear and abducens nerves as well as optic nerves and globes. Clinical data and ophthalmologic evaluations were also collected.
Results
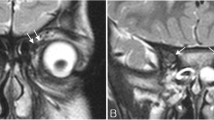
Six children (age range: 1-16 years; males: 3) were selected. All patients showed, on the affected side (left:right = 5:1), anomalies of the III nerve and extraocular muscles innervated by the pathological nerve. One patient had complete nerve agenesis, two patients showed a diffuse thinning of the nerve, from the brainstem to the orbit and 3 patients showed a distal thinning of the oculomotor nerve, starting at the level of the cavernous sinus. In all cases atrophy of corresponding muscles was noticed, but the involvement of the affected muscles varied with the nervous pattern of injury.
Conclusions
High-resolution MRI represents a valuable tool for the diagnosis of III nerve anomalies in unilateral congenital IOP, showing different patterns of nerve involvement and muscular atrophy.



Similar content being viewed by others
References
Richards BW, Jones FRJ, Younge BR (1992) Causes and prognosis in 4,278 cases of paralysis of the oculomotor, trochlear, and abducens cranial nerves. Am J Ophthalmol 113:489–496. https://doi.org/10.1016/s0002-9394(14)74718-x
Miller NR (1977) Solitary oculomotor nerve palsy in childhood. Am J Ophthalmol 83:106–111. https://doi.org/10.1016/0002-9394(77)90197-0
Kau H-C, Tsai C-C, Ortube MC, Demer JL (2007) High-resolution magnetic resonance imaging of the extraocular muscles and nerves demonstrates various etiologies of third nerve palsy. Am J Ophthalmol 143:280–287. https://doi.org/10.1016/j.ajo.2006.10.035
Ng YSP, Lyons CJ (2005) Oculomotor nerve palsy in childhood. Can J Ophthalmol 40:645–653. https://doi.org/10.1016/S0008-4182(05)80062-6
Keith CG (1987) Oculomotor nerve palsy in childhood. Aust N Z J Ophthalmol 15:181–184. https://doi.org/10.1111/j.1442-9071.1987.tb00068.x
Gutowski NJ, Bosley TM, Engle EC (2003) 110th ENMC International Workshop: the congenital cranial dysinnervation disorders (CCDDs). Naarden, The Netherlands, 25–27 October, 2002. Neuromuscul Disord 13:573–578
Gutowski NJ, Chilton JK (2015) The congenital cranial dysinnervation disorders. Arch Dis Child 100:678–681. https://doi.org/10.1136/archdischild-2014-307035
Singh A, Pandey PK, Agrawal A et al (2017) Congenital cranial dysinnervation disorders. Int Ophthalmol 37:1369–1381
Razek AAKA, Maher H, Kasem MA, Helmy E (2021) Imaging of congenital cranial dysinnervation disorders: What radiologist wants to know? Clin Imaging 71:106–116
Yang HK, Kim JH, Hwang JM (2020) Magnetic resonance imaging in 14 patients with congenital oculomotor nerve palsy. Clin Neuroradiol 30:237–242. https://doi.org/10.1007/s00062-019-00781-5
Kim JH, Hwang J-M (2009) Magnetic resonance imaging in three patients with congenital oculomotor nerve palsy. Br J Ophthalmol 93:1266–1267
Wu TJ, Isenberg SJ, Demer JL (2006) Magnetic resonance imaging demonstrates neuropathology in congenital inferior division oculomotor palsy. J AAPOS 10:473–475. https://doi.org/10.1016/j.jaapos.2006.04.007
Demer JL, Ortube MC, Engle EC, Thacker N (2006) High-resolution magnetic resonance imaging demonstrates abnormalities of motor nerves and extraocular muscles in patients with neuropathic strabismus. J AAPOS 10:135–142. https://doi.org/10.1016/j.jaapos.2005.12.006
Gottlob I, Catalano RA, Reinecke RD (1991) Surgical management of oculomotor nerve palsy. Am J Ophthalmol 111:71–76. https://doi.org/10.1016/s0002-9394(14)76900-4
von Noorden GK, Campos EC (2002) Binocular vision and ocular motility, 6th edn. Mosby, St Louis
Ganger A, Yadav S, Singh A, Saxena R (2016) A comprehensive review on the management of III nerve palsy. Delhi J Ophthalmol 27:86–91
Kim JH, Hwang JM (2017) Imaging of cranial nerves III, IV, VI in congenital cranial dysinnervation disorders. Korean J Ophthalmol 31:183–193. https://doi.org/10.3341/kjo.2017.0024
Lueck CJ (2011) Infranuclear ocular motor disorder. Handb Clin Neurol 102:281–318. https://doi.org/10.1016/B978-0-444-52903-9.00017-0
Danieli L, Montali M, Remonda L et al (2018) Clinically directed neuroimaging of ophthalmoplegia. Clin Neuroradiol 28:3–16
Corrêa DG, Hygino da Cruz LC, Freddi T de AL (2022) The oculomotor nerve: anatomy and pathology. Semin Ultrasound CT MRI 43:389–399. https://doi.org/10.1053/j.sult.2022.04.009
Whitman MC, Engle EC (2017) Ocular congenital cranial dysinnervation disorders (CCDDs): insights into axon growth and guidance. Hum Mol Genet 26:R37–R44. https://doi.org/10.1093/hmg/ddx168
Schulz E, Jung H (2001) Unilateral congenital oculomotor nerve palsy, optic nerve hypoplasia and pituitary malformation: a preliminary report. In: Strabismus. p 33–35
Langmann A, Lindner S (2004) Congenital third nerve palsy in septo-optic dysplasia [2]. Br J Ophthalmol 88:969
Funding
This study was partially funded by the Italian Ministry of Health, Ricerca Corrente 2019–2022, to the Scientific Institute IRCCS E.Medea.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval
This is a retrospective observational study conducted from data obtained from a larger study on pediatric high-resolution brain MRI, approved by the Ethics Committee of E. Medea Research Institute.
Consent to participate
Informed consent was obtained from legal guardians.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Arrigoni, F., Rombetto, L., Redaelli, D. et al. Congenital isolated unilateral third nerve palsy in children: the diagnostic contribution of high-resolution MR imaging. Neuroradiology 65, 865–870 (2023). https://doi.org/10.1007/s00234-022-03106-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-022-03106-5