Abstract
Purpose
The aim of this study is to evaluate the safety and effectiveness of endovascular treatment (EVT) for acute ischemic stroke caused by large-vessel obstruction or stenosis (AIS-LVO/S) over 24 h after first AIS symptom recognition (FAISSR).
Methods
A total of 33 AIS-LVO/S cases with EVT over 24 h after FAISSR during the period from January 2019 to February 2022 in our hospital were divided into the 90d mRS ≤ 2 group [favorable outcome (FO) group] and 90d mRS > 2 group [unfavorable outcome (UFO) group] and retrospectively analyzed.
Results
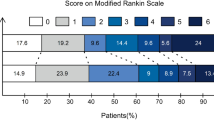
The reperfusion was successfully established with EVT in 97% (32/33) of cases, and most (63.6%, 21/33) had 90d mRS ≤ 2 and only 36.4% (12/33) had 90d mRS > 2. Preoperative DWI-ASPECT and ASITN/SIR scores were significantly higher and NIHSS scores were significantly lower in the FO group than those in the UFO group (P < 0.05). In addition, the FAISSR to exacerbation time, FAISSR to groin puncture time, and FAISSR to reperfusion time were significantly longer, and the groin puncture to reperfusion time was significantly shorter in the FO group than those in the UFO group (P < 0.05), but there was no significant difference in the stroke exacerbation to groin puncture time (P > 0.05). The patients with cerebral infarction due to artery dissection had more favorable EVT outcomes, but the patients with posterior cerebral circulation infarction had very poor EVT outcomes.
Conclusions
The FAISSR to groin puncture time over 24 h may not be a taboo for EVT and it may be safe and effective for AIS-LVO/S in anterior cerebral circulation, especially with lower preoperative NIHSS scores.




Similar content being viewed by others
Data availability
The dataset supporting the conclusions of this paper is shown within the article.
References
Berkhemer OA, Fransen PS, Beumer D et al (2015) A randomized trial of intraarterial treatment for acute ischemic stroke. N Engl J Med 372(1):11–20. https://doi.org/10.1056/NEJMoa1411587
Campbell BC, Mitchell PJ, Kleinig TJ et al (2015) Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med 372(11):1009–1018. https://doi.org/10.1056/NEJMoa1414792
Saver JL, Goyal M, Bonafe A et al (2015) Stent-retriever thrombectomy after intravenous t-PA vs. t-PA alone in stroke. N Engl J Med 372(24):2285–2295. https://doi.org/10.1056/NEJMoa1415061
Jovin TG, Chamorro A, Cobo E et al (2015) Thrombectomy within 8 hours after symptom onset in ischemic stroke. N Engl J Med 372(24):2296–2306. https://doi.org/10.1056/NEJMoa1503780
Goyal M, Demchuk AM, Menon BK et al (2015) Randomized assessment of rapid endovascular treatment of ischemic stroke. N Engl J Med 372(11):1019–1030. https://doi.org/10.1056/NEJMoa1414905
Albers GW, Marks MP, Kemp S et al (2018) Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med 378(8):708–718. https://doi.org/10.1056/NEJMoa1713973
Nogueira RG, Jadhav AP, Haussen DC et al (2018) Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N Engl J Med 378(1):11–21. https://doi.org/10.1056/NEJMoa1706442
Desai SM, Haussen DC, Aghaebrahim A et al (2018) Thrombectomy 24 hours after stroke: beyond DAWN. J Neurointerv Surg 10(11):1039–1042. https://doi.org/10.1136/neurintsurg-2018-013923
Hirai T, Sasaki M, Maeda M et al (2009) Diffusion-weighted imaging in ischemic stroke: effect of display method on observers’ diagnostic performance. Acad Radiol 16(3):305–312. https://doi.org/10.1016/j.acra.2008.09.012
Higashida RT, Furlan AJ, Roberts H et al (2003) Trial design and reporting standards for intra-arterial cerebral thrombolysis for acute ischemic stroke. Stroke 34(8):e109-137. https://doi.org/10.1161/01.STR.0000082721.62796.09
Seet RC, Rabinstein AA (2012) Symptomatic intracranial hemorrhage following intravenous thrombolysis for acute ischemic stroke: a critical review of case definitions. Cerebrovasc Dis 34(2):106–114. https://doi.org/10.1159/000339675
Shan G, Gerstenberger S (2017) Fisher’s exact approach for post hoc analysis of a chi-squared test. PLoS ONE 12(12):e0188709. https://doi.org/10.1371/journal.pone.0188709
Goyal M, Menon BK, van Zwam WH et al (2016) Endovascular thrombectomy after large-vessel ischaemic stroke: a meta-analysis of individual patient data from five randomised trials. Lancet 387(10029):1723–1731. https://doi.org/10.1016/S0140-6736(16)00163-X
Purrucker JC, Ringleb PA, Seker F et al (2022) Leaving the day behind: endovascular therapy beyond 24 h in acute stroke of the anterior and posterior circulation. Ther Adv Neurol Disord 15:17562864221101084. https://doi.org/10.1177/17562864221101083
Zi W, Qiu Z, Li F et al (2021) Effect of endovascular treatment alone vs intravenous alteplase plus endovascular treatment on functional independence in patients with acute ischemic stroke: The DEVT Randomized Clinical Trial. JAMA 325(3):234–243. https://doi.org/10.1001/jama.2020.23523
Yang P, Zhang Y, Zhang L et al (2020) Endovascular thrombectomy with or without intravenous alteplase in acute stroke. N Engl J Med 382(21):1981–1993. https://doi.org/10.1056/NEJMoa2001123
Markus HS, Levi C, King A et al (2019) Antiplatelet therapy vs anticoagulation therapy in cervical artery dissection: the Cervical Artery Dissection in Stroke Study (CADISS) randomized clinical trial final results. JAMA Neurol 76(6):657–664. https://doi.org/10.1001/jamaneurol.2019.0072
Leng X, Fang H, Leung TW et al (2016) Impact of collaterals on the efficacy and safety of endovascular treatment in acute ischaemic stroke: a systematic review and meta-analysis. J Neurol Neurosurg Psychiatry 87(5):537–544. https://doi.org/10.1136/jnnp-2015-310965
Liebeskind DS, Saber H, Xiang B et al (2022) Collateral circulation in thrombectomy for stroke after 6 to 24 hours in the DAWN Trial. Stroke 53(3):742–748. https://doi.org/10.1161/STROKEAHA.121.034471
Hashimoto T, Kunieda T, Honda T et al (2022) Reduced leukoaraiosis, noncardiac embolic stroke etiology, and shorter thrombus length indicate good leptomeningeal collateral flow in embolic large-vessel occlusion. AJNR Am J Neuroradiol 43(1):63–69. https://doi.org/10.3174/ajnr.A7360
Jovin TG, Nogueira RG, Lansberg MG et al (2022) Thrombectomy for anterior circulation stroke beyond 6 h from time last known well (AURORA): a systematic review and individual patient data meta-analysis. Lancet 399(10321):249–258. https://doi.org/10.1016/S0140-6736(21)01341-6
Dreixler JC, Poston JN, Shaikh AR et al (2011) Delayed post-ischemic conditioning significantly improves the outcome after retinal ischemia. Exp Eye Res 92(6):521–527. https://doi.org/10.1016/j.exer.2011.03.015
England TJ, Hedstrom A, O’Sullivan S et al (2017) RECAST (Remote Ischemic Conditioning After Stroke Trial): a pilot randomized placebo controlled phase II trial in acute ischemic stroke. Stroke 48(5):1412–1415. https://doi.org/10.1161/STROKEAHA.116.016429
An JQ, Cheng YW, Guo YC et al (2020) Safety and efficacy of remote ischemic postconditioning after thrombolysis in patients with stroke. Neurology 95(24):e3355–e3363. https://doi.org/10.1212/WNL.0000000000010884
Schonewille WJ, Wijman CA, Michel P et al (2009) Treatment and outcomes of acute basilar artery occlusion in the Basilar Artery International Cooperation Study (BASICS): a prospective registry study. Lancet Neurol 8(8):724–730. https://doi.org/10.1016/S1474-4422(09)70173-5
Liu X, Dai Q, Ye R et al (2020) Endovascular treatment versus standard medical treatment for vertebrobasilar artery occlusion (BEST): an open-label, randomised controlled trial. Lancet Neurol 19(2):115–122. https://doi.org/10.1016/S1474-4422(19)30395-3
Langezaal LCM, van der Hoeven EJRJ, Mont’Alverne FJA et al (2022) Endovascular therapy for stroke due to basilar-artery occlusion. N Engl J Med 384(20):1910–1920. https://doi.org/10.1056/NEJMoa2030297
Jovin TG, Ji X, BAOCHE investigators (2022) Basilar Artery Occlusion Chinese Endovascular trial. European Stroke Congress (ESOC 2022). https://2022.eso-conference.org/wp-content/uploads/2022/05/BAOCHEsummaryslides.pdf. Accessed 4 May 2022
Acknowledgements
The authors are grateful to all of the patients and/or their next of kin for their consent to publication of this study and accompanying images.
Funding
This study was supported by Jiangxi Provincial People’s Hospital Grant 2019–009.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest in relation to this study.
Ethics approval
All procedures and research protocols were approved by the Research Ethics Committee of Jiangxi Provincial People’s Hospital (No. 2022–035).
Informed consent
Informed consent was obtained from all the patients and/or their next of kin for publication of this study and accompanying images.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, S., Cao, W., Wu, L. et al. Endovascular treatment over 24 hours after ischemic stroke onset: a single-center retrospective study. Neuroradiology 65, 793–804 (2023). https://doi.org/10.1007/s00234-022-03105-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-022-03105-6