Abstract
Purpose
We sought to establish a comprehensive imaging score indicating the likelihood of higher WHO grade meningiomas pre-operatively.
Methods
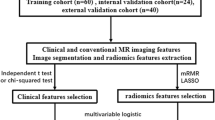
All surgical intracranial meningioma patients at our institution between 2014 and 2018 underwent retrospective chart review. Preoperative MRI sequences were reviewed, and imaging features were included in the score based on statistical and clinical significance. Point values for each significant feature were assigned based on the beta coefficients obtained from multivariate analysis. The imaging score was calculated by adding up the points, for a total score of 0 to 5. The predictive ability of the score to identify higher-grade meningiomas was evaluated.
Results
Ninety patients, 50% of whom had a postoperative diagnosis of WHO grade II meningioma, were included. The mean age for the population was 59.9 years and 70% were female. Tumor volume ≥ 36.0 cc was assigned 2 points, presence of irregular tumor borders was assigned 2 points, and presence of peritumoral edema was assigned 1 point. The probability of having a WHO grade II meningioma was 0% with a score of 0, 25.0% with a score of 1, 38.5% with a score of 2, 65.4% with a score of 3, and 83.3% with a score of 4 or greater. A threshold of ≥ 3 points achieved a recall of 0.80, precision of 0.73, F1-score of 0.77, accuracy of 0.76, and AUC of 0.82.
Conclusion
The proposed imaging scoring system had good predictive capability for WHO grade II meningiomas with good discrimination and calibration. External validation is needed.



Similar content being viewed by others
Data Availability
The deidentified data that support the findings of this study are available from the corresponding author, A.F., upon reasonable request.
Abbreviations
- WHO:
-
World Health Organization
- MRI:
-
Magnetic resonance imaging
- FLAIR:
-
Fluid-attenuated inversion recovery
- SWI:
-
Susceptibility weighted imaging
- DWI:
-
Diffusion-weighted imaging
- CT:
-
Computed tomography
- ADC:
-
Apparent diffusion coefficient
- ROI:
-
Region of interest
- CSF:
-
Cerebrospinal fluid
- qADC:
-
Quantitative apparent diffusion coefficient
- NADC:
-
Normalized apparent diffusion coefficient
- AUC:
-
Area under the curve
- PIMS:
-
Preoperative imaging meningioma score
References
Ostrom QT, Patil N, Cioffi G, Waite K, Kruchko C, Barnholtz-Sloan JS (2020) CBTRUS Statistical Report: primary brain and other central nervous system tumors diagnosed in the United States in 2013–2017. Neuro Oncol 22(12 Suppl 2):iv1–iv96. https://doi.org/10.1093/neuonc/noaa200
Alexiou GA, Gogou P, Markoula S, Kyritsis AP (2010) Management of meningiomas. Clin Neurol Neurosurg 112(3):177–182. https://doi.org/10.1016/j.clineuro.2009.12.011
Whittle IR, Smith C, Navoo P, Collie D (2004) Meningiomas. Lancet 363(9420):1535–1543. https://doi.org/10.1016/s0140-6736(04)16153-9
Buerki RA, Horbinski CM, Kruser T, Horowitz PM, James CD, Lukas RV (2018) An overview of meningiomas. Future Oncol 14(21):2161–2177. https://doi.org/10.2217/fon-2018-0006
Louis DN (2007) WHO classification of tumours of the central nervous system. WHO.
Lin DD, Lin JL, Deng XY et al (2019) Trends in intracranial meningioma incidence in the United States, 2004–2015. Cancer Med 8(14):6458–6467. https://doi.org/10.1002/cam4.2516
Kshettry VR, Ostrom QT, Kruchko C, Al-Mefty O, Barnett GH, Barnholtz-Sloan JS (2015) Descriptive epidemiology of World Health Organization grades II and III intracranial meningiomas in the United States. Neuro Oncol 17(8):1166–1173. https://doi.org/10.1093/neuonc/nov069
Modha A, Gutin PH (2005) Diagnosis and treatment of atypical and anaplastic meningiomas: a review. Neurosurgery 57(3):538–50. https://doi.org/10.1227/01.neu.0000170980.47582.a5. (discussion 538–50)
Marciscano AE, Stemmer-Rachamimov AO, Niemierko A et al (2016) Benign meningiomas (WHO Grade I) with atypical histological features: correlation of histopathological features with clinical outcomes. J Neurosurg 124(1):106–114. https://doi.org/10.3171/2015.1.Jns142228
Ohba S, Kobayashi M, Horiguchi T et al (2011) Long-term surgical outcome and biological prognostic factors in patients with skull base meningiomas. J Neurosurg 114(5):1278–1287. https://doi.org/10.3171/2010.11.Jns10701
Ogasawara C, Philbrick BD, Adamson DC. Meningioma: a review of epidemiology, pathology, diagnosis, treatment, and future directions. Biomedicines. 2021;9(3) https://doi.org/10.3390/biomedicines9030319
Lee EJ, Kim JH, Park ES et al (2017) A novel weighted scoring system for estimating the risk of rapid growth in untreated intracranial meningiomas. J Neurosurg 127(5):971–980. https://doi.org/10.3171/2016.9.Jns161669
Coroller TP, Bi WL, Huynh E et al (2017) Radiographic prediction of meningioma grade by semantic and radiomic features. PLoS One 12(11):e0187908. https://doi.org/10.1371/journal.pone.0187908
Lin BJ, Chou KN, Kao HW et al (2014) Correlation between magnetic resonance imaging grading and pathological grading in meningioma. J Neurosurg 121(5):1201–1208. https://doi.org/10.3171/2014.7.Jns132359
Spille DC, Sporns PB, Heß K, Stummer W, Brokinkel B (2019) Prediction of high-grade histology and recurrence in meningiomas using routine preoperative magnetic resonance imaging: a systematic review. World Neurosurg 128:174–181. https://doi.org/10.1016/j.wneu.2019.05.017
Hale AT, Wang L, Strother MK, Chambless LB (2018) Differentiating meningioma grade by imaging features on magnetic resonance imaging. J Clin Neurosci 48:71–75. https://doi.org/10.1016/j.jocn.2017.11.013
Hashiba T, Hashimoto N, Maruno M et al (2006) Scoring radiologic characteristics to predict proliferative potential in meningiomas. Brain Tumor Pathol 23(1):49–54. https://doi.org/10.1007/s10014-006-0199-4
Nakasu S, Nakajima M, Matsumura K, Nakasu Y, Handa J (1995) Meningioma: proliferating potential and clinicoradiological features. Neurosurgery 37(6):1049–1055. https://doi.org/10.1227/00006123-199512000-00003
Kasuya H, Kubo O, Tanaka M, Amano K, Kato K, Hori T (2006) Clinical and radiological features related to the growth potential of meningioma. Neurosurg Rev 29(4):293–6. https://doi.org/10.1007/s10143-006-0039-3. (discussion 296–7)
Kawahara Y, Nakada M, Hayashi Y et al (2012) Prediction of high-grade meningioma by preoperative MRI assessment. J Neurooncol 108(1):147–152. https://doi.org/10.1007/s11060-012-0809-4
Surov A, Gottschling S, Mawrin C et al (2015) Diffusion-weighted imaging in meningioma: prediction of tumor grade and association with histopathological parameters. Transl Oncol 8(6):517–523. https://doi.org/10.1016/j.tranon.2015.11.012
Nagar VA, Ye JR, Ng WH et al (2008) Diffusion-weighted MR imaging: diagnosing atypical or malignant meningiomas and detecting tumor dedifferentiation. AJNR Am J Neuroradiol 29(6):1147–1152. https://doi.org/10.3174/ajnr.A0996
Moons KG, Harrell FE, Steyerberg EW (2002) Should scoring rules be based on odds ratios or regression coefficients? J Clin Epidemiol 55(10):1054–1055. https://doi.org/10.1016/s0895-4356(02)00453-5
Shin HK, Park JH, Cho YH et al (2021) Risk factors for high-grade meningioma in brain and spine: systematic review and meta-analysis. World Neurosurg 151:e718–e730. https://doi.org/10.1016/j.wneu.2021.04.138
Meyer HJ, Wienke A, Surov A (2020) ADC values of benign and high grade meningiomas and associations with tumor cellularity and proliferation —a systematic review and meta-analysis. J Neurol Sci 415:116975. https://doi.org/10.1016/j.jns.2020.116975
Bozdağ M, Er A, Ekmekçi S (2021) Association of apparent diffusion coefficient with Ki-67 proliferation index, progesterone-receptor status and various histopathological parameters, and its utility in predicting the high grade in meningiomas. Acta Radiol 62(3):401–413. https://doi.org/10.1177/0284185120922142
Agarwal V, McCutcheon BA, Hughes JD et al (2017) Trends in management of intracranial meningiomas: analysis of 49,921 cases from modern cohort. World Neurosurg 106:145–151. https://doi.org/10.1016/j.wneu.2017.06.127
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
This research study was conducted retrospectively from data obtained for clinical purposes. We consulted extensively with the IRB of the Albert Einstein College of Medicine, who determined that our study did not need ethical approval. An IRB official waiver of ethical approval was granted from the IRB of the Albert Einstein College of Medicine.
Informed consent
The requirement for informed consent was officially waived by the IRB of Albert Einstein College of Medicine due to the purely retrospective nature of the study. Additionally, no identifying patient information or images are published below.
Competing interests
The authors have no competing interests to declare that are relevant to the content of this article.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Funari, A., De la Garza Ramos, R., Cezayirli, P. et al. Imaging score for differentiation of meningioma grade. Neuroradiology 65, 453–462 (2023). https://doi.org/10.1007/s00234-022-03101-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-022-03101-w