Abstract
Purpose
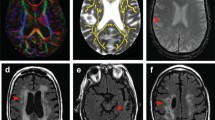
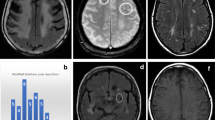
Patients with vanishing white matter (VWM) experience unremitting chronic neurological decline and stress-provoked episodes of rapid, partially reversible decline. Cerebral white matter abnormalities are progressive, without improvement, and are therefore unlikely to be related to the episodes. We determined which radiological findings are related to episodic decline.
Methods
MRI scans of VWM patients were retrospectively analyzed. Patients were grouped into A (never episodes) and B (episodes). Signal abnormalities outside the cerebral white matter were rated as absent, mild, or severe. A sum score was developed with abnormalities only seen in group B. The temporal relationship between signal abnormalities and episodes was determined by subdividing scans into those made before, less than 3 months after, and more than 3 months after onset of an episode.
Results
Five hundred forty-three examinations of 298 patients were analyzed. Mild and severe signal abnormalities in the caudate nucleus, putamen, globus pallidus, thalamus, midbrain, medulla oblongata, and severe signal abnormalities in the pons were only seen in group B. The sum score, constructed with these abnormalities, depended on the timing of the scan (χ2(2, 400) = 22.8; p < .001): it was least often abnormal before, most often abnormal with the highest value shortly after, and lower longer than 3 months after an episode.
Conclusion
In VWM, signal abnormalities in brainstem, thalamus, and basal ganglia are related to episodic decline and can improve. Knowledge of the natural MRI history in VWM is important for clinical interpretation of MRI findings and crucial in therapy trials.








Similar content being viewed by others
Abbreviations
- IQR:
-
Interquartile range
- VWM:
-
Vanishing white matter
References
Leegwater PA, Vermeulen G, Konst AA, Naidu S, Mulders J, Visser A et al (2001) Subunits of the translation initiation factor eIF2B are mutant in leukoencephalopathy with vanishing white matter. Nat Genet 29(4):383–388
van der Knaap MS, Leegwater PA, Konst AA, Visser A, Naidu S, Oudejans CB et al (2002) Mutations in each of the five subunits of translation initiation factor eIF2B can cause leukoencephalopathy with vanishing white matter. Ann Neurol 51(2):264–270
Hamilton EMC, van der Lei HDW, Vermeulen G, Gerver JAM, Lourenco CM, Naidu S et al (2018) Natural history of vanishing white matter. Ann Neurol 84(2):274–288
van der Knaap MS, Pronk JC, Scheper GC (2006) Vanishing white matter disease. Lancet Neurol 5(5):413–423
Bugiani M, Boor I, van Kollenburg B, Postma N, Polder E, van Berkel C et al (2011) Defective glial maturation in vanishing white matter disease. J Neuropathol Exp Neurol 70(1):69–82
Stellingwerff MD, Al-Saady ML, van de Brug T, Barkhof F, Pouwels PJW, van der Knaap MS (2021) MRI Natural History of the Leukodystrophy Vanishing White Matter. Radiology 300(3):671–680. https://doi.org/10.1148/radiol.2021210110
van der Knaap MS, Breiter SN, Naidu S, Hart AA, Valk J (1999) Defining and categorizing leukoencephalopathies of unknown origin: MR imaging approach. Radiology 213(1):121–133
Hanefeld F, Holzbach U, Kruse B, Wilichowski E, Christen HJ, Frahm J (1993) Diffuse white matter disease in three children: an encephalopathy with unique features on magnetic resonance imaging and proton magnetic resonance spectroscopy. Neuropediatrics 24(5):244–248
Tedeschi G, Schiffmann R, Barton NW, Shih HH, Gospe SM Jr, Brady RO et al (1995) Proton magnetic resonance spectroscopic imaging in childhood ataxia with diffuse central nervous system hypomyelination. Neurology 45(8):1526–1532
van der Knaap MS, Barth PG, Gabreels FJ, Franzoni E, Begeer JH, Stroink H et al (1997) A new leukoencephalopathy with vanishing white matter. Neurology 48(4):845–855
van der Knaap MS, Kamphorst W, Barth PG, Kraaijeveld CL, Gut E, Valk J (1998) Phenotypic variation in leukoencephalopathy with vanishing white matter. Neurology 51(2):540–547
Alorainy IA, Patenaude YG, O’Gorman AM, Black DN, Meagher-Villemure K (1999) Cree leukoencephalopathy: neuroimaging findings. Radiology 213(2):400–406
Bugiani M, Postma N, Polder E, Dieleman N, Scheffer PG, Sim FJ et al (2013) Hyaluronan accumulation and arrested oligodendrocyte progenitor maturation in vanishing white matter disease. Brain 136(Pt 1):209–222
Bruck W, Herms J, Brockmann K, Schulz-Schaeffer W, Hanefeld F (2001) Myelinopathia centralis diffusa (vanishing white matter disease): evidence of apoptotic oligodendrocyte degeneration in early lesion development. Ann Neurol 50(4):532–536
Rodriguez D, Gelot A, dellaGaspera B, Robain O, Ponsot G, Sarlieve LL et al (1999) Increased density of oligodendrocytes in childhood ataxia with diffuse central hypomyelination (CACH) syndrome: neuropathological and biochemical study of two cases. Acta Neuropathol. 97(5):469–80
Jacobson S, Marcus EM, Pugsley S. (2018) Myelin-Stained. Neuroanatomy for the Neuroscientist. Cham: Springer International Publishing; 679–89
Dooves S, Bugiani M, Postma NL, Polder E, Land N, Horan ST et al (2016) Astrocytes are central in the pathomechanisms of vanishing white matter. J Clin Invest 126(4):1512–1524
Bugiani M, Plug BC, Man JHK, Breur M, van der Knaap MS (2022) Heterogeneity of white matter astrocytes in the human brain. Acta Neuropathol 143(2):159–177
van der Lei HD, Steenweg ME, Barkhof F, de Grauw T, d’Hooghe M, Morton R et al (2012) Characteristics of early MRI in children and adolescents with vanishing white matter. Neuropediatrics 43(1):22–26
Acknowledgements
The authors thank all referring physicians and IT staff for technical support in digitizing radiologic films. MSvdK is a member of the European reference network for rare neurological disorders (ERN-RND), project ID 739510.
Funding
Not applicable.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
MSvdK receives research funding from NWO (Spinoza award), ZonMw (TOP 91217006 and 10140261910004/80–86600-98–84001), Hersenstichting (DR-2019–00285), and European Leukodystrophy Foundation (2019-P001 and 2020-017I2). She has a patent P112686CA00, therapeutic effects of Guanabenz treatment in vanishing white matter, pending to VU University Medical Center. MDS and MAvdW declare no competing interests.
Ethics approval
The local ethics committee approved this retrospective study.
Informed consent
Informed consent was obtained from patients and/or parents.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Stellingwerff, M.D., van de Wiel, M.A. & van der Knaap, M.S. Radiological correlates of episodes of acute decline in the leukodystrophy vanishing white matter. Neuroradiology 65, 855–863 (2023). https://doi.org/10.1007/s00234-022-03097-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-022-03097-3