Abstract
Purpose
The aim of the study was to assess the prevalence and characteristics of spinal cord cavernous malformations (SCCM) and intraosseous spinal vascular malformations (ISVM) in a pediatric familial cerebral cavernous malformation (FCCM) cohort and evaluate clinico-radiological differences between children with (SCCM +) and without (SCCM-) SCCM.
Methods
All patients with a pediatric diagnosis of FCCM evaluated at three tertiary pediatric hospitals between January 2010 and August 2021 with \(\ge\) 1 whole spine MR available were included. Brain and spine MR studies were retrospectively evaluated, and clinical and genetic data collected. Comparisons between SCCM + and SCCM- groups were performed using student-t/Mann–Whitney or Fisher exact tests, as appropriate.
Results
Thirty-one children (55% boys) were included. Baseline spine MR was performed (mean age = 9.7 years) following clinical manifestations in one subject (3%) and as a screening strategy in the remainder. Six SCCM were detected in five patients (16%), in the cervico-medullary junction (n = 1), cervical (n = 3), and high thoracic (n = 2) regions, with one appearing during follow-up. A tendency towards an older age at first spine MR (P = 0.14) and \(\ge\) 1 posterior fossa lesion (P = 0.13) was observed in SCCM + patients, lacking statistical significance. No subject demonstrated ISVM.
Conclusion
Although rarely symptomatic, SCCM can be detected in up to 16% of pediatric FCCM patients using diverse spine MR protocols and may appear de novo. ISVM were instead absent in our cohort. Given the relative commonality of asymptomatic SCCM, serial screening spine MR should be considered in FCCM starting in childhood.



Similar content being viewed by others
Abbreviations
- CM:
-
Cavernous malformation
- FCCM:
-
Familial cerebral cavernous malformation syndrome
- ISVM:
-
Intraosseous spinal vascular malformations
- SCCM:
-
Spinal cord cavernous malformation
References
Zafar A, Quadri SA, Farooqui M et al (2019) Familial cerebral cavernous malformations. Stroke 50:1294–1301
Choquet H, Pawlikowska L, Lawton MT, Kim H (2015) Genetics of cerebral cavernous malformations: current status and future prospects. Neurosurg Sci 59:211–220
Strickland CD, Eberhardt SC, Bartlett MR et al (2017) Familial cerebral cavernous malformations are associated with adrenal calcifications on CT scans: an imaging biomarker for a hereditary cerebrovascular condition. Radiology 284:443–450
Manole AK, Forrester VJ, Zlotoff BJ et al (2020) Cutaneous findings of familial cerebral cavernous malformation syndrome due to the common Hispanic mutation. Am J Med Genet A 182:1066–1072
Toldo I, Drigo P, Mammi I et al (2009) Vertebral and spinal cavernous angiomas associated with familial cerebral cavernous malformation. Surg Neurol 71:167–171
de Vos IJHM, Vreeburg M, Koek GH, van Steensel MAM (2017) Review of familial cerebral cavernous malformations and report of seven additional families. Am J Med Genet A 173:338–351
Mabray MC, Starcevich J, Hallstrom J et al (2020) High prevalence of spinal cord cavernous malformations in the familial cerebral cavernous malformations type 1 cohort. AJNR Am J Neuroradiol 41:1126–1130
Cohen-Gadol AA, Jacob JT, Edwards DA, Krauss WE (2006) Coexistence of intracranial and spinal cavernous malformations: a study of prevalence and natural history. J Neurosurg 104:376–381
Badhiwala JH, Farrokhyar F, Alhazzani W et al (2014) Surgical outcomes and natural history of intramedullary spinal cord cavernous malformations: a single-center series and meta-analysis of individual patient data. J Neurosurg Spine 21:662–676
Ren J, Hong T, He C, et al (2019) Coexistence of intracranial and spinal cord cavernous malformations predict aggressive clinical presentation. Front Neurol 10:
Clatterbuck RE, Cohen B, Gailloud P et al (2002) Vertebral hemangiomas associated with familial cerebral cavernous malformation: segmental disease expression. Case report J Neurosurg 97:227–230
Lanfranconi S, Ronchi D, Ahmed N, et al (2014) A novel CCM1 mutation associated with multiple cerebral and vertebral cavernous malformations. BMC Neurol 14:
Tandberg SR, Bocklage T, Bartlett MR et al (2020) Vertebral intraosseous vascular malformations in a familial cerebral cavernous malformation population: prevalence, histologic features, and associations with CNS disease. AJR Am J Roentgenol 214:428–436
Ren J, Hong T, Zeng G et al (2020) Characteristics and long-term outcome of 20 children with intramedullary spinal cord cavernous malformations. Neurosurgery 86:817–824
Zhang L, Qiao G, Yang W et al (2021) Clinical features and long-term outcomes of pediatric spinal cord cavernous malformation-a report of 18 cases and literature review. Childs Nerv Syst 37:235–242
Merello E, Pavanello M, Consales A et al (2016) Genetic Screening of pediatric cavernous malformations. J Mol Neurosci 60:232–238
Lanfranconi S, Scola E, Bertani GA et al (2020) Propranolol for familial cerebral cavernous malformation (Treat_CCM): Study protocol for a randomized controlled pilot trial. Trials 21:401
Oldenburg J, Malinverno M, Globisch MA et al (2021) Propranolol reduces the development of lesions and rescues barrier function in cerebral cavernous malformations: a preclinical study. Stroke 52:1418–1427
Polster SP, Stadnik A, Akers AL et al (2019) Atorvastatin treatment of cavernous angiomas with symptomatic hemorrhage exploratory proof of concept (AT CASH EPOC) trial. Neurosurgery 85:843–853
Mespreuve M, Vanhoenacker F, Lemmerling M (2016) Familial multiple cavernous malformation syndrome: MR features in this uncommon but silent threat. J Belg Soc Radiol 100:51
Zabramski JM, Wascher TM, Spetzler RF et al (1994) The natural history of familial cavernous malformations: results of an ongoing study. J Neurosurg 80:422–432
Panda A, Diehn FE, Kim DK et al (2020) Spinal cord cavernous malformations: MRI commonly Shows adjacent intramedullary hemorrhage. J Neuroimaging 30:690–696
Al-Shahi Salman R, Berg MJ, Morrison L et al (2008) Hemorrhage from cavernous malformations of the brain: definition and reporting standards. Stroke 39:3222–3230
Bilguvar K, Bydon M, Bayrakli F et al (2007) A novel syndrome of cerebral cavernous malformation and Greig cephalopolysyndactyly: Laboratory investigation. J Neurosurg 107:495–499
Ogilvy CS, Louis DN, Ojemann RG (1992) Intramedullary cavernous angiomas of the spinal cord: clinical presentation, pathological features, and surgical management. Neurosurgery 31:219–230
Akers AL, Johnson E, Steinberg GK et al (2009) Biallelic somatic and germline mutations in cerebral cavernous malformations (CCMs): evidence for a two-hit mechanism of CCM pathogenesis. Hum Mol Genet 18:919–930
Pagenstecher A, Stahl S, Sure U, Felbor U (2009) A two-hit mechanism causes cerebral cavernous malformations: complete inactivation of CCM1, CCM2 or CCM3 in affected endothelial cells. Hum Mol Genet 18:911–918
Riant F, Bergametti F, Fournier HD et al (2013) CCM3 mutations are associated with early-onset cerebral hemorrhage and multiple meningiomas. Mol Syndr 4:165–172
Shenkar R, Shi C, Rebeiz T et al (2015) Exceptional aggressiveness of cerebral cavernous malformation disease associated with PDCD10 mutations. Genet Med 17:188–196
Akers A, Al-Shahi Salman R, Awad IA et al (2017) Synopsis of guidelines for the clinical management of cerebral cavernous malformations: consensus recommendations based on systematic literature review by the angioma alliance scientific advisory board clinical experts panel. Neurosurgery 80:665–680
Funding
Twelve months research fellowship in diagnostic neuroradiology, European Society of Neuroradiology (AF Geraldo).
Author information
Authors and Affiliations
Contributions
AF Geraldo, S Reimao, Severino M: study concept and design. AF Geraldo, A Luis, CAPF Alves, D Tortora, E S Shwartz, K Mankad, A Rossi, M Severino: analysis and interpretation of imaging data. AF Geraldo: statistical analysis. AF Geraldo: drafting the manuscript. AF Geraldo, A Luis, CAPFAlves, D Tortora, J Guimarães, S Reimão, A Rossi, M Pavanello, P De Marco, M Scala, V Capra, Rossi A, E S Shwartz, K Mankad, M Severino: revising the manuscript.
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study, formal consent is not required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
234_2022_2958_MOESM1_ESM.png
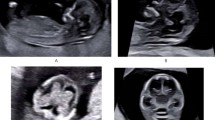
Supplementary file1 Supplemental Figure 1. Spine MR (a–e) performed in a 10-year-old boy with familial cerebral cavernous malformation syndrome due to a proven CCM1 mutation (SCCM patient #1) including sagittal T2 TSE (a), T1 TSE (b), and GRE (c) as well as axial T2 TSE (d) and GRE (e) demonstrates an intramedullary cavernous malformation located posteriorly and lateralized to the right at the level of T1-T2 (white arrowheads and empty white arrows). Note the absence of hypointense T2 rim, spinal cord expansion, or edema (PNG 1100 KB)
234_2022_2958_MOESM2_ESM.png
Supplementary file2 Supplemental Figure 2. Follow-up spine MR studies of the same patient presented in Supplemental Figure 1 (SCCM patient #1) performed 7 (a,b) and 36 (c,d) months after including sagittal T2 TSE (a,c) and GRE (b,d) reveal initial subtle growth of the spinal cord cavernous malformation (white arrowheads and empty white arrows) and mild perilesional edema (white thin arrows) followed by size reduction and development of adjacent intramedullary flame-like hemorrhage (thick white arrows). Brain MR obtained at the time of the initial diagnosis including axial SWI (e,f) images reveals two intracranial cavernous malformations, one in the left parietal lobe (black arrowhead) and another in the ipsilateral mesial-temporal region (thin black arrow) (PNG 1153 KB)
Rights and permissions
About this article
Cite this article
Geraldo, A.F., Luis, A., Alves, C.A.P.F. et al. Spinal involvement in pediatric familial cavernous malformation syndrome. Neuroradiology 64, 1671–1679 (2022). https://doi.org/10.1007/s00234-022-02958-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-022-02958-1