Abstract
Purpose
To detect the cerebral blood vessels and perfusion using neuroimaging modalities including computed tomography angiography (CTA), computed tomography perfusion (CTP), and arterial spin labeling (ASL) in children with brain death (BD).
Methods
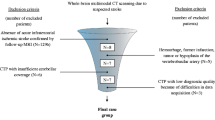
According to the current children’s BD criteria, 5 children (3 males, 2 females, mean age of 5.65 years) with BD were enrolled from January 2019 to December 2020. The imaging features of CTA, CTP, and ASL were evaluated to analyze the visualization of important intracranial blood vessels and the states of the cerebral blood flow (CBF) and cerebral blood volume (CBV) related to the region of interest (ROI) brain tissue during the two clinical assessments for BD.
Results
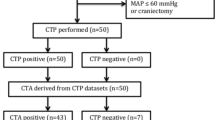
The “4-point scale” scoring system of CTA was applied to evaluate BD and no negative results were detected. The CTP results of the 5 children suggested the cessation of cerebral circulation with 100% positive results. The ranges of CBF and CBV were 0.00–9.52 ml/100 g/min (mean value 4.95 ± 1.69 ml/100 g/min) and 0.00–1.34 ml/100 g (mean value 0.36 ± 0.20 ml/100 g), respectively. One patient also underwent ASL examination, which demonstrated a significant reduction in whole brain perfusion, indicating the absence of cerebral circulation. The CBF values of the brainstem, basal ganglia, and prefrontal lobe were 11.61 ± 1.49 ml/100 g/min, 7.81 ± 2.42 ml/100 g/min, and 9.94 ± 2.01 ml/100 g/min, respectively.
Conclusion
Neuroimaging examinations particularly CTA and CTP reveal well the hemodynamic and cerebral blood vessels changes of BD, which can be used as supplementary supportive evidence for the declaration of brain death in children.





Similar content being viewed by others
References
Wijdicks EF, Varelas PN, Gronseth GS, Greer DM (2010) American Academy of Neurology. Evidence-based guideline update: determining brain death in adults: report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology 74(23):1911–1918
Wijdicks EF (2002) Brain death worldwide: accepted fact but no global consensus in diagnostic criteria. Neurology 58(1):20–25
Wahlster S, Wijdicks EF, Patel PV et al (2015) Brain death declaration: practices and perceptions worldwide. Neurology 84(18):1870–1879
Lewis A, Greer D (2017) Current controversies in brain death determination. Nat Rev Neurol 13(8):505–509
Braksick SA, Robinson CP, Gronseth GS, Hocker S, Wijdicks EFM, Rabinstein AA (2019) Variability in reported physician practices for brain death determination. Neurology 92(9):e888–e894
Greer DM, Shemie SD, Lewis A et al (2020) Determination of brain death/death by neurologic criteria: the world brain death project. JAMA 324(11):1078–1097
Lovrencic-Huzjan A, Vukovic V, Gopcevic A, Vucic M, Kriksic V, Demarin V (2011) Transcranial Doppler in brain death confirmation in clinical practice. Ultraschall Med 32(1):62–66
Pedicelli A, Bartocci M, Lozupone E et al (2019) The role of cervical color Doppler ultrasound in the diagnosis of brain death. Neuroradiology 61(2):137–145
Welschehold S, Boor S, Reuland K et al (2012) Technical aids in the diagnosis of brain death: a comparison of SEP, AEP, EEG, TCD and CT angiography. Dtsch Arztebl Int 109(39):624–630
Sawicki M, Sołek-Pastuszka J, Chamier-Ciemińska K, Walecka A, Walecki J, Bohatyrewicz R (2019) Computed tomography perfusion is a useful adjunct to computed tomography angiography in the diagnosis of brain death. Clin Neuroradiol 29(1):101–108
Akdogan AI, Pekcevik Y, Sahin H, Pekcevik R (2021) Assessment of cerebral circulatory arrest via CT angiography and CT perfusion in brain death confirmation. Korean J Radiol 22(3):395–404
Ekinci F, Yıldızdaş D, Horoz ÖÖ, İncecik F (2021) Evaluation of pediatric brain death and organ donation: 10-year experience in a pediatric intensive care unit in Turkey. Turk Arch Pediatr 56(6):638–645
Bohatyrewicz R, Sołek-Pastuszka J, Walas W et al (2021) Invitation to participate in a multi-center study for validation of cerebral computed tomography angiography and computed tomography perfusion in the determination of cerebral circulatory arrest during brain death/death by neurological criteria diagnosis procedure in paediatric population below 12 years of age. Anaesthesiol Intensive Ther 53(2):97–102
(2019) Brain Injury Evaluation Quality Control Center of National Health Commission. Zhonghua Er Ke Za Zhi 57(5):331–335
Greer DM, Strozyk D, Schwamm LH (2009) False positive CT angiography in brain death. Neurocrit Care 11(2):272–275
Wijdicks EF, Varelas PN, Gronseth GS, Greer DM, Academy A, of Neurology, (2010) Evidence-based guideline update: determining brain death in adults: report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology 74(23):1911–1918
Frampas E, Videcoq M, de Kerviler E et al (2009) CT angiography for brain death diagnosis. AJNR Am J Neuroradiol 30(8):1566–1570
Kramer AH, Roberts DJ (2014) Computed tomography angiography in the diagnosis of brain death: a systematic review and meta-analysis. Neurocrit Care 21(3):539–550
Sawicki M, Bohatyrewicz R, Walecka A, Sołek-Pastuszka J, Rowiński O, Walecki J (2014) CT Angiography in the Diagnosis of Brain Death. Pol J Radiol 79:417–421
Leclerc X, Taschner CA, Vidal A et al (2006) The role of spiral CT for the assessment of the intracranial circulation in suspected brain-death. J Neuroradiol 33(2):90–95
Rieke A, Regli B, Mattle HP et al (2011) Computed tomography angiography (CTA) to prove circulatory arrest for the diagnosis of brain death in the context of organ transplantation. Swiss Med Wkly 141:w13261
(2002) The ALARA (as low as reasonably achievable) concept in pediatric CT intelligent dose reduction. Multidisciplinary conference organized by the Society of Pediatric Radiology. August 18–19, 2001. Pediatr Radiol 32(4), 217–313.
Dupas B, Gayet-Delacroix M, Villers D, Antonioli D, Veccherini MF, Soulillou JP (1998) Diagnosis of brain death using two-phase spiral CT. AJNR Am J Neuroradiol 19(4):641–647
Combes JC, Chomel A, Ricolfi F, d’Athis P, Freysz M (2007) Reliability of computed tomographic angiography in the diagnosis of brain death. Transplant Proc 39(1):16–20
Sawicki M, Bohatyrewicz R, Safranow K et al (2014) Computed tomographic angiography criteria in the diagnosis of brain death-comparison of sensitivity and interobserver reliability of different evaluation scales. Neuroradiology 56(8):609–620
Şahin H, Pekçevik Y (2015) CT angiography as a confirmatory test in diagnosis of brain death: comparison between three scoring systems. Diagn Interv Radiol 21(2):177–183
Welschehold S, Kerz T, Boor S et al (2013) Detection of intracranial circulatory arrest in brain death using cranial CT-angiography. Eur J Neurol 20(1):173–179
Nunes DM, Maia ACM Jr, Boni RC, da Rocha AJ (2019) Impact of skull defects on the role of CTA for brain death confirmation. AJNR Am J Neuroradiol 40(7):1177–1183
Sawicki M, Bohatyrewicz R, Safranow K et al (2013) Dynamic evaluation of stasis filling phenomenon with computed tomography in diagnosis of brain death. Neuroradiology 55(9):1061–1069
Wu B, Yang Y, Zhou S et al (2018) Could arterial spin labeling distinguish patients in minimally conscious state from patients in vegetative state? Front Neurol 9:110
Powers WJ, Grubb RL Jr, Darriet D, Raichle ME (1985) Cerebral blood flow and cerebral metabolic rate of oxygen requirements for cerebral function and viability in humans. J Cereb Blood Flow Metab 5(4):600–608
Latchaw RE, Yonas H, Hunter GJ et al (2003) Guidelines and recommendations for perfusion imaging in cerebral ischemia: a scientific statement for healthcare professionals by the writing group on perfusion imaging, from the Council on Cardiovascular Radiology of the American Heart Association. Stroke 34(4):1084–1104
Astrup J (1982) Energy-requiring cell functions in the ischemic brain. Their critical supply and possible inhibition in protective therapy. J Neurosurg 56(4):482–497
Taylor T, Dineen RA, Gardiner DC, Buss CH, Howatson A, Pace NL (2014) Computed tomography (CT) angiography for confirmation of the clinical diagnosis of brain death. Cochrane Database Syst Rev 2014(3):CD009694
Kang KM, Yun TJ, Yoon BW et al (2015) Clinical utility of arterial spin-labeling as a confirmatory test for suspected brain death. AJNR Am J Neuroradiol 36(5):909–914
Heran MK, Heran NS, Shemie SD (2008) A review of ancillary tests in evaluating brain death. Can J Neurol Sci 35(4):409–419
Buxton RB, Frank LR (1997) A model for the coupling between cerebral blood flow and oxygen metabolism during neural stimulation. J Cereb Blood Flow Metab 17(1):64–72
Wieler H, Marohl K, Kaiser KP, Klawki P, Frössler H (1993) Tc-99m HMPAO cerebral scintigraphy. A reliable, noninvasive method for determination of brain death. Clin Nucl Med. 18(2):104–109
Orrison WW Jr, Champlin AM, Kesterson OL, Hartshorne MF, King JN (1994) MR “hot nose sign” and “intravascular enhancement sign” in brain death. AJNR Am J Neuroradiol 15(5):913–916
Sinha P, Conrad GR (2012) Scintigraphic confirmation of brain death. Semin Nucl Med 42(1):27–32
Qiu D, Straka M, Zun Z, Bammer R, Moseley ME, Zaharchuk G (2012) CBF measurements using multidelay pseudocontinuous and velocity-selective arterial spin labeling in patients with long arterial transit delays: comparison with xenon CT CBF. J Magn Reson Imaging 36(1):110–119
Alsop DC, Detre JA, Golay X et al (2015) Recommended implementation of arterial spin-labeled perfusion MRI for clinical applications: a consensus of the ISMRM perfusion study group and the European consortium for ASL in dementia. Magn Reson Med 73(1):102–116
Wang R, Yu S, Alger JR et al (2014) Multi-delay arterial spin labeling perfusion MRI in moyamoya disease–comparison with CT perfusion imaging. Eur Radiol 24(5):1135–1144
Fan AP, Guo J, Khalighi MM et al (2017) Long-delay arterial spin labeling provides more accurate cerebral blood flow measurements in Moyamoya patients: a simultaneous positron emission tomography/MRI Study. Stroke 48(9):2441–2449
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethics approval
All procedures performed in the studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, Q., Yu, T., Wu, J. et al. Cerebral blood vessels and perfusion in the pediatric brain death: five cases studied by neuroimaging. Neuroradiology 64, 1661–1669 (2022). https://doi.org/10.1007/s00234-022-02955-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-022-02955-4