Abstract
Purpose
Acute hydrocephalus is a common complication after aneurysmal subarachnoid hemorrhage (aSAH). It can be self-limiting or require cerebrospinal fluid diversion. We aimed to determine the transient acute hydrocephalus (TAH) rate in patients with aSAH treated endovascularly and evaluate its predictive factors.
Methods
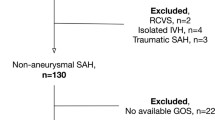
A retrospective review of 357 patients with aSAH who underwent endovascular treatment from March 2013 to December 2019 was performed. Clinical and radiographic data were analyzed and risk factors with potential significance for acute hydrocephalus were identified. We constructed a new risk score, the Drainage Or Transiency of Acute Hydrocephalus after Aneurysmal SAH (DOTAHAS) score, that may differentiate patients who would experience TAH from those needing surgical interventions.
Results
Acute hydrocephalus occurred in 129 patients (36%), out of whom in 66 patients (51%) it was self-limiting while 63 patients (49%) required external ventricular drainage placement. As independent risk factors for acute hydrocephalus, we identified older age, poor initial clinical condition, aSAH from posterior circulation, and the extent of cisternal and intraventricular hemorrhage. The following three factors were shown to predict acute hydrocephalus transiency and therefore included in the DOTAHAS score, ranging from 0 to 7 points: Hunt and Hess grade ≥ 3 (1 point), modified Fisher grade 4 (2 points), and Ventricular Hijdra Sum Score (vHSS) ≥ 6 (4 points). Patients scoring ≥ 3 points had significantly higher risk for EVD (P < 0.0001) than other patients.
Conclusion
The newly developed DOTAHAS score can be useful in identifying patients with transient acute hydrocephalus. Further score evaluation is needed.



Similar content being viewed by others
References
Chen S, Luo J, Reis C et al (2017)Hydrocephalus after subarachnoid hemorrhage: pathophysiology, diagnosis, and treatment.Biomed Res Int 2017.https://doi.org/10.1155/2017/8584753
Wilson CD, Safavi-Abbasi S, Sun H et al (2017) Meta-analysis and systematic review of risk factors for shunt dependency after aneurysmal subarachnoid hemorrhage. J Neurosurg 126:586–595. https://doi.org/10.3171/2015.11.JNS152094
Adams H, Ban VS, Leinonen V et al (2016) Risk of shunting after aneurysmal subarachnoid hemorrhage: a collaborative study and initiation of a consortium. Stroke 47:2488–2496. https://doi.org/10.1161/STROKEAHA.116.013739
Connolly ES, Rabinstein AA, Carhuapoma JR et al (2012) Guidelines for the management of aneurysmal subarachnoid hemorrhage: a guideline for healthcare professionals from the American heart association/American stroke association. Stroke 43:1711–1737. https://doi.org/10.1161/STR.0b013e3182587839
Gigante P, Hwang BY, Appelboom G et al (2010) External ventricular drainage following aneurysmal subarachnoid haemorrhage. Br J Neurosurg 24:625–632. https://doi.org/10.3109/02688697.2010.505989
Jabbarli R, Bohrer AM, Pierscianek D et al (2016) The CHESS score: a simple tool for early prediction of shunt dependency after aneurysmal subarachnoid hemorrhage. Eur J Neurol 23:912–918. https://doi.org/10.1111/ene.12962
van Gijn J, Hijdra A, Wijdicks EFM et al (1985) Acute hydrocephalus after aneurysmal subarachnoid hemorrhage. J Neurosurg 63:355–362. https://doi.org/10.3171/jns.1985.63.3.0355
Hasan D, Tanghe HLJ (1992) Distribution of cisternal blood in patients with acute hydrocephalus after subarachnoid hemorrhage. Ann Neurol 31:374–378. https://doi.org/10.1002/ana.410310405
Mehta V, Holness RO, Connolly K et al (1996) Acute hydrocephalus following aneurysmal subarachnoid hemorrhage. Can J Neurol Sci 23:40–45. https://doi.org/10.1017/S0317167100039160
Graff Radford NR, Torner J, Adams HP, Kassell NF (1989) Factors associated with hydrocephalus after subarachnoid hemorrhage: a report of the cooperative aneurysm study. Arch Neurol 46:744–752. https://doi.org/10.1001/archneur.1989.00520430038014
Hasan D, Vermeulen M, Wijdicks EFM et al (1989) Management problems in acute hydrocephalus after subarachnoid hemorrhage. Stroke 20:747–753. https://doi.org/10.1161/01.STR.20.6.747
Diesing D, Wolf S, Sommerfeld J et al (2018) A novel score to predict shunt dependency after aneurysmal subarachnoid hemorrhage. J Neurosurg 128:1273–1279. https://doi.org/10.3171/2016.12.JNS162400
Fisher CM, Kistler JP, Davis JM (1980) Relation of cerebral vasospasm to subarachnoid hemorrhage visualized by computerized tomographic scanning. Neurosurgery 6:1–9. https://doi.org/10.1227/00006123-198001000-00001
Frontera JA, Claassen J, Schmidt JM et al (2006) Prediction of symptomatic vasospasm after subarachnoid hemorrhage: the modified Fisher scale. Neurosurgery 59:21–26. https://doi.org/10.1227/01.NEU.0000218821.34014.1B
Wilson DA, Nakaji P, Abla AA et al (2012) A simple and quantitative method to predict symptomatic vasospasm after subarachnoid hemorrhage based on computed tomography: beyond the Fisher scale. Neurosurgery 71:869–875. https://doi.org/10.1227/NEU.0b013e318267360f
Hijdra A, Brouwers P, Vermeulen M, Van GJ (1990) Grading the amount of blood on computed tomograms after subarachnoid hemorrhage. Stroke 21:1156–1161. https://doi.org/10.1161/01.STR.21.8.1156
Bretz JS, Von Dincklage F, Woitzik J et al (2017) The Hijdra scale has significant prognostic value for the functional outcome of Fisher grade 3 patients with subarachnoid hemorrhage. Clin Neuroradiol 27:361–369. https://doi.org/10.1007/s00062-016-0509-0
Molyneux AJ, Kerr RS, Yu LM, International Subarachnoid Aneurysm Trial (ISAT) Collaborative Group et al (2005) International subarachnoid aneurysm trial (ISAT) of neurosurgical clipping versus endovascular coiling in 2143 patients with ruptured intracranial aneurysms: a randomised comparison of effects on survival, dependency, seizures, rebleeding, subgroups, and aneurysm occlusion. Lancet 366:809–817. https://doi.org/10.1016/S0140-6736(05)67214-5
Jartti P, Karttunen A, Jartti A et al (2004) Factors related to acute hydrocephalus after subarachnoid hemorrhage. Acta Radiol 45:333–339. https://doi.org/10.1080/02841850410004274
Toma AK, Holl E, Kitchen ND, Watkins LD (2011) Evans’ index revisited: the need for an alternative in normal pressure hydrocephalus. Neurosurgery 68:939–944. https://doi.org/10.1227/NEU.0b013e318208f5e0
Dupont S, Rabinstein AA (2013) CT evaluation of lateral ventricular dilatation after subarachnoid hemorrhage: baseline bicaudate index values. Neurol Res 35:103–106. https://doi.org/10.1179/1743132812Y.0000000121
Kukuljan M, Kolic Z, Bonifacic D et al (2009) Normal bicaudate index by aging. Curr Med Imaging Rev 5:72–74. https://doi.org/10.2174/157340509788185351
Fried HI, Nathan BR, Rowe AS et al (2016) The insertion and management of external ventricular drains: an evidence-based consensus statement: a statement for healthcare professionals from the Neurocritical Care Society. Neurocrit Care 24:61–81. https://doi.org/10.1007/s12028-015-0224-8
Konovalov A, Shekhtman O, Pilipenko Y et al (2021) External ventricular drainage in patients with acute aneurysmal subarachnoid hemorrhage after microsurgical clipping: Our 2006–2018 Experience and a Literature Review. Cureus 13:1–9. https://doi.org/10.7759/cureus.12951
Orešković D, Klarica M (2011) Development of hydrocephalus and classical hypothesis of cerebrospinal fluid hydrodynamics: facts and illusions. Prog Neurobiol 94:238–258. https://doi.org/10.1016/j.pneurobio.2011.05.005
Funding
No funding was received for this study
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
All the authors declare that they have no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
Ethics approval
Study was conducted after the Institutional Ethics Committee approved the study.
Informed consent
Written informed consent was obtained from all patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jovanović, I., Nemir, J., Gardijan, D. et al. Transient acute hydrocephalus after aneurysmal subarachnoid hemorrhage and aneurysm embolization: a single-center experience. Neuroradiology 63, 2111–2119 (2021). https://doi.org/10.1007/s00234-021-02747-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-021-02747-2