Abstract
Purpose
To assess whether the radiomic features of diffusion tensor imaging (DTI) and conventional postcontrast T1-weighted (T1C) images can differentiate the epidermal growth factor receptor (EGFR) mutation status in brain metastases from non-small cell lung cancer (NSCLC).
Methods
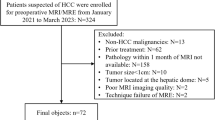
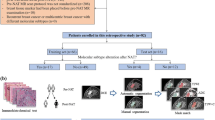
A total of 99 brain metastases in 51 patients who underwent surgery or biopsy with underlying NSCLC and known EGFR mutation statuses (57 from EGFR wild type, 42 from EGFR mutant) were allocated to the training (57 lesions in 31 patients) and test (42 lesions in 20 patients) sets. Radiomic features (n = 526) were extracted from preoperative MR images including T1C and DTI. Radiomics classifiers were constructed by combinations of five feature selectors and four machine learning algorithms. The trained classifiers were validated on the test set, and the classifier performance was assessed by determining the area under the curve (AUC).
Results
EGFR mutation status showed an overall discordance rate of 12% between the primary tumors and corresponding brain metastases. The best performing classifier was a combination of the tree-based feature selection and linear discriminant algorithm and 5 features were selected (1 from ADC, 2 from fractional anisotropy, and 2 from T1C images), resulting in an AUC, accuracy, sensitivity, and specificity of 0.73, 78.6%, 81.3%, and 76.9% in the test set, respectively.
Conclusions
Radiomics classifiers integrating multiparametric MRI parameters may have potential in differentiating the EGFR mutation status in brain metastases from NSCLC.



Similar content being viewed by others
Availability of Data and Material
Our anonymized data can be obtained by any qualified investigator for the purposes of replicating procedures and results after ethics clearance and approval by all authors.
References
Molina JR, Yang P, Cassivi SD, Schild SE, Adjei AA (2008) Non-small cell lung cancer: epidemiology, risk factors, treatment, and survivorship. In: Mayo Clinic Proceedings. vol 5. Elsevier, pp 584-594
Porta R, Sanchez-Torres J, Paz-Ares L, Massuti B, Reguart N, Mayo C, Lianes P, Queralt C, Guillem V, Salinas P (2011) Brain metastases from lung cancer responding to erlotinib: the importance of EGFR mutation. Eur Respir J 37(3):624–631
Soria J-C, Ohe Y, Vansteenkiste J, Reungwetwattana T, Chewaskulyong B, Lee KH, Dechaphunkul A, Imamura F, Nogami N, Kurata T (2018) Osimertinib in untreated EGFR-mutated advanced non–small-cell lung cancer. N Engl J Med 378(2):113–125
Novello S, Barlesi F, Califano R, Cufer T, Ekman S, Levra MG, Kerr K, Popat S, Reck M, Senan S (2016) Metastatic non-small-cell lung cancer: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol 27(suppl_5):v1–v27
Gow C-H, Chien C-R, Chang Y-L, Chiu Y-H, Kuo S-H, Shih J-Y, Chang Y-C, Yu C-J, Yang C-H, Yang P-C (2008) Radiotherapy in lung adenocarcinoma with brain metastases: effects of activating epidermal growth factor receptor mutations on clinical response. Clin Cancer Res 14(1):162–168
Mok TS, Wu Y-L, Thongprasert S, Yang C-H, Chu D-T, Saijo N, Sunpaweravong P, Han B, Margono B, Ichinose Y (2009) Gefitinib or carboplatin–paclitaxel in pulmonary adenocarcinoma. N Engl J Med 361(10):947–957
Tomiyama N, Yasuhara Y, Nakajima Y, Adachi S, Arai Y, Kusumoto M, Eguchi K, Kuriyama K, Sakai F, Noguchi M (2006) CT-guided needle biopsy of lung lesions: a survey of severe complication based on 9783 biopsies in Japan. Eur J Radiol 59(1):60–64
Rivera MP, Mehta AC, Wahidi MM (2013) Establishing the diagnosis of lung cancer: diagnosis and management of lung cancer: American College of Chest Physicians evidence-based clinical practice guidelines. Chest 143(5):e142S–e165S
Monaco SE, Nikiforova MN, Cieply K, Teot LA, Khalbuss WE, Dacic S (2010) A comparison of EGFR and KRAS status in primary lung carcinoma and matched metastases. Hum Pathol 41(1):94–102
Han H-S, Eom D-W, Kim JH, Kim K-H, Shin H-M, An JY, Lee KM, Choe KH, Lee KH, Kim ST (2011) EGFR mutation status in primary lung adenocarcinomas and corresponding metastatic lesions: discordance in pleural metastases. Clin Lung Cancer 12(6):380–386
Italiano A, Vandenbos FB, Otto J, Mouroux J, Fontaine D, Marcy P-Y, Cardot N, Thyss A, Pedeutour F (2006) Comparison of the epidermal growth factor receptor gene and protein in primary non-small-cell-lung cancer and metastatic sites: implications for treatment with EGFR-inhibitors. Ann Oncol 17(6):981–985
Gow C-H, Chang Y-L, Hsu Y-C, Tsai M-F, Wu C-T, Yu C-J, Yang C-H, Lee Y-C, Yang P-C, Shih J-Y (2008) Comparison of epidermal growth factor receptor mutations between primary and corresponding metastatic tumors in tyrosine kinase inhibitor-naive non-small-cell lung cancer. Ann Oncol 20(4):696–702
Chen Z-Y, Zhong W-Z, Zhang X-C, Su J, Yang X-N, Chen Z-H, Yang J-J, Zhou Q, Yan H-H, An S-J (2012) EGFR mutation heterogeneity and the mixed response to EGFR tyrosine kinase inhibitors of lung adenocarcinomas. Oncologist 17(7):978–985
Brastianos PK, Carter SL, Santagata S, Cahill DP, Taylor-Weiner A, Jones RT, Van Allen EM, Lawrence MS, Horowitz PM, Cibulskis K (2015) Genomic characterization of brain metastases reveals branched evolution and potential therapeutic targets. Cancer Discov 5(11):1164–1177
Hu N, Wang G, Wu Y-H, Chen S-F, Liu G-D, Chen C, Wang D, He Z-S, Yang X-Q, He Y (2015) LDA-SVM-based EGFR mutation model for NSCLC brain metastases: an observational study. Medicine 94(5):e375
Gillies RJ, Kinahan PE, Hricak H (2015) Radiomics: images are more than pictures, they are data. Radiology 278(2):563–577
Park Y, Han K, Ahn S, Choi Y, Chang J, Kim S, Kang S-G, Kim E, Lee S-K (2018) Whole-tumor histogram and texture analyses of DTI for evaluation of IDH1-mutation and 1p/19q-codeletion status in World Health Organization grade II gliomas. Am J Neuroradiol 39(4):693–698
Kickingereder P, Burth S, Wick A, Götz M, Eidel O, Schlemmer H-P, Maier-Hein KH, Wick W, Bendszus M, Radbruch A (2016) Radiomic profiling of glioblastoma: identifying an imaging predictor of patient survival with improved performance over established clinical and radiologic risk models. Radiology 280(3):880–889
Lal A, Glazer CA, Martinson HM, Friedman HS, Archer GE, Sampson JH, Riggins GJ (2002) Mutant epidermal growth factor receptor up-regulates molecular effectors of tumor invasion. Cancer Res 62(12):3335–3339
Jung W, Park C, Hong C-K, Suh S, Ahn S (2018) Diffusion-weighted imaging of brain metastasis from lung cancer: correlation of MRI parameters with the histologic type and gene mutation status. Am J Neuroradiol 39(2):273–279
Kniep HC, Madesta F, Schneider T, Hanning U, Schönfeld MH, Schön G, Fiehler J, Gauer T, Werner R, Gellissen S (2019) Radiomics of brain MRI: utility in prediction of metastatic tumor type. Radiology 290(2):479–487. https://doi.org/10.1148/radiol.2018180946
Travis WD, Brambilla E, Nicholson AG, Yatabe Y, Austin JH, Beasley MB, Chirieac LR, Dacic S, Duhig E, Flieder DB (2015) The 2015 World Health Organization classification of lung tumors: impact of genetic, clinical and radiologic advances since the 2004 classification. J Thorac Oncol 10(9):1243–1260
Cha YJ, Kim HR, Shim HS (2016) Clinical outcomes in ALK-rearranged lung adenocarcinomas according to ALK fusion variants. J Transl Med 14(1):296
Kang SM, Kang HJ, Shin JH, Kim H, Shin DH, Kim SK, Kim JH, Chung KY, Kim SK, Chang J (2007) Identical epidermal growth factor receptor mutations in adenocarcinomatous and squamous cell carcinomatous components of adenosquamous carcinoma of the lung. Cancer 109(3):581–587
Jellison BJ, Field AS, Medow J, Lazar M, Salamat MS, Alexander AL (2004) Diffusion tensor imaging of cerebral white matter: a pictorial review of physics, fiber tract anatomy, and tumor imaging patterns. AJNR Am J Neuroradiol 25(3):356–369
Shinohara RT, Sweeney EM, Goldsmith J, Shiee N, Mateen FJ, Calabresi PA, Jarso S, Pham DL, Reich DS, Crainiceanu CM (2014) Statistical normalization techniques for magnetic resonance imaging. Neuroimage Clin 6:9–19
Fedorov A, Beichel R, Kalpathy-Cramer J, Finet J, Fillion-Robin J-C, Pujol S, Bauer C, Jennings D, Fennessy F, Sonka M (2012) 3D Slicer as an image computing platform for the Quantitative Imaging Network. Magn Reson Imaging 30(9):1323–1341
Bahrami N, Piccioni D, Karunamuni R, Chang Y-H, White N, Delfanti R, Seibert T, Hattangadi-Gluth J, Dale A, Farid N (2018) Edge contrast of the FLAIR hyperintense region predicts survival in patients with high-grade gliomas following treatment with bevacizumab. Am J Neuroradiol 39(6):1017–1024
Tibshirani R (1996) Regression shrinkage and selection via the lasso. J R Stat Soc Ser B Methodol 58(1):267–288
Liu Y, Kim J, Qu F, Liu S, Wang H, Balagurunathan Y, Ye Z, Gillies RJ (2016) CT features associated with epidermal growth factor receptor mutation status in patients with lung adenocarcinoma. Radiology 280(1):271–280
Liu Y, Kim J, Balagurunathan Y, Li Q, Garcia AL, Stringfield O, Ye Z, Gillies RJ (2016) Radiomic features are associated with EGFR mutation status in lung adenocarcinomas. Clin Lung Cancer 17(5):441–448 e446
Lambregts DM, Beets GL, Maas M, Curvo-Semedo L, Kessels AG, Thywissen T, Beets-Tan RG (2011) Tumour ADC measurements in rectal cancer: effect of ROI methods on ADC values and interobserver variability. Eur Radiol 21(12):2567–2574. https://doi.org/10.1007/s00330-011-2220-5
Chen BT, Jin T, Ye N, Mambetsariev I, Daniel E, Wang T, Wong CW, Rockne RC, Colen R, Holodny AI, Sampath S, Salgia R (2020) Radiomic prediction of mutation status based on MR imaging of lung cancer brain metastases. Magn Reson Imaging 69:49–56. https://doi.org/10.1016/j.mri.2020.03.002
Park JE, Park SY, Kim HJ, Kim HS (2019) Reproducibility and generalizability in radiomics modeling: possible strategies in radiologic and statistical perspectives. Korean J Radiol 20(7):1124–1137. https://doi.org/10.3348/kjr.2018.0070
Sequist LV, Waltman BA, Dias-Santagata D, Digumarthy S, Turke AB, Fidias P, Bergethon K, Shaw AT, Gettinger S, Cosper AK (2011) Genotypic and histological evolution of lung cancers acquiring resistance to EGFR inhibitors. Sci Transl Med 3(75):75ra26
Soffietti R, Abacioglu U, Baumert B, Combs SE, Kinhult S, Kros JM, Marosi C, Metellus P, Radbruch A, Villa Freixa SS (2017) Diagnosis and treatment of brain metastases from solid tumors: guidelines from the European Association of Neuro-Oncology (EANO). Neuro-Oncology 19(2):162–174
Klein CA (2009) Parallel progression of primary tumours and metastases. Nat Rev Cancer 9(4):302–312
Jamal-Hanjani M, Quezada SA, Larkin J, Swanton C (2015) Translational implications of tumor heterogeneity. Clin Cancer Res 21(6):1258–1266
Li S, Ding C, Zhang H, Song J, Wu L (2019) Radiomics for the prediction of EGFR mutation subtypes in non-small cell lung cancer. Med Phys 46(10):4545–4552. https://doi.org/10.1002/mp.13747
Tu W, Sun G, Fan L, Wang Y, Xia Y, Guan Y, Li Q, Zhang D, Liu S, Li Z (2019) Radiomics signature: a potential and incremental predictor for EGFR mutation status in NSCLC patients, comparison with CT morphology. Lung Cancer 132:28–35. https://doi.org/10.1016/j.lungcan.2019.03.025
Mei D, Luo Y, Wang Y, Gong J (2018) CT texture analysis of lung adenocarcinoma: can radiomic features be surrogate biomarkers for EGFR mutation statuses. Cancer Imaging 18(1):52. https://doi.org/10.1186/s40644-018-0184-2
Kang D, Park JE, Kim Y-H, Kim JH, Oh JY, Kim J, Kim Y, Kim ST, Kim HS (2018) Diffusion radiomics as a diagnostic model for atypical manifestation of primary central nervous system lymphoma: development and multicenter external validation. Neuro-Oncology 20(9):1251–1261
Yan P-F, Yan L, Hu T-T, Xiao D-D, Zhang Z, Zhao H-Y, Feng J (2017) The potential value of preoperative mri texture and shape analysis in grading meningiomas: a preliminary investigation. Transl Oncol 10(4):570–577
Zhang Z, Yang J, Ho A, Jiang W, Logan J, Wang X, Brown PD, McGovern SL, Guha-Thakurta N, Ferguson SD (2018) A predictive model for distinguishing radiation necrosis from tumour progression after gamma knife radiosurgery based on radiomic features from MR images. Eur Radiol 28(6):2255–2263
Wu J, Gensheimer MF, Dong X, Rubin DL, Napel S, Diehn M, Loo BW Jr, Li R (2016) Robust intratumor partitioning to identify high-risk subregions in lung cancer: a pilot study. Int J Radiat Oncol Biol Phys 95(5):1504–1512
Funding
This research received funding from the Basic Science Research Program through the National Research Foundation of Korea (NRF), which is funded by the Ministry of Science, Information and Communication Technologies & Future Planning (2017R1D1A1B03030440 and 2020R1A2C1003886). This research was also supported by the Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education (2020R1I1A1A01071648).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this retrospective study, the Yonsei University Institutional Review Board waived the need for obtaining informed patient consent for this retrospective study.
Consent to participate
As this is a retrospective study, the institutional review board waived the need for obtaining informed patient consent.
Consent for publication
All of the authors gave consent for publication of the article.
Code availability
The python code for machine learning can be obtained by any qualified investigator for the purposes of replicating procedures and results after approval by all authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Park, Y.W., An, C., Lee, J. et al. Diffusion tensor and postcontrast T1-weighted imaging radiomics to differentiate the epidermal growth factor receptor mutation status of brain metastases from non-small cell lung cancer. Neuroradiology 63, 343–352 (2021). https://doi.org/10.1007/s00234-020-02529-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-020-02529-2