Abstract
Purpose
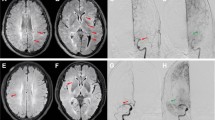
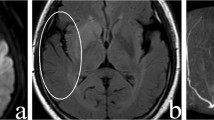
Fluid-attenuated inversion recovery vascular hyperintensity (FVH) is often observed in conjunction with acute ischemic stroke (AIS) of the carotid system. Despite its bearing on patient care outcomes, factors influencing FVH and its clinical significance in patients with transient ischemic attacks (TIAs) of the carotid arterial system have yet to be evaluated.
Methods
Consecutive inpatients (N = 154) diagnosed with TIAs of the carotid system in a 2-year period (2012–2014) were enrolled in our study. Each had undergone magnetic resonance imaging (MRI) within 72 h of symptom onset, followed by intracranial and extracranial vascular imaging. We investigated the frequency and nature of factors associated with FVH, also examining its clinical significance in the 30-day prognosis of TIA.
Results
Of the 154 patients enrolled (male, 92; mean age 63.0 ± 11.9), FVH was confirmed in 61 patients (39.6%). In logistic regression analysis, intracranial large-artery disease (LAD) (OR = 2.39, 95% CI 1.16–4.92; p = 0.018) and prior stroke (OR = 3.33, 95% CI 1.48–7.51; p = 0.004) emerged as factors independently associated with FVH positivity. Ultimately, 25 patients (16.2%) progressed to AIS within a 30-day follow-up period. Logistic regression analysis indicated that contralateral FVH positivity (OR = 5.98, 95% CI 1.81–19.76; p = 0.003), atrial fibrillation (OR = 7.05, 95% CI 1.33–37.40; p = 0.022), and extracranial LAD (OR = 4.12, 95% CI 1.26–13.41; p = 0.019) were independently associated with AIS during the 30-day follow-up of TIAs in these patients.
Conclusion
Intracranial LAD and previous stroke are independently associated with FVH in patients experiencing carotid system TIAs. If present, FVH may predict an oncoming AIS in the 30 days following a TIA.


Similar content being viewed by others
References
(1990) Special report from the National Institute of Neurological Disorders and Stroke. Classification of cerebrovascular diseases III. Stroke 21(4):637–676
Johnston SC, Gress DR, Browner WS, Sidney S (2000) Short-term prognosis after emergency department diagnosis of TIA. JAMA-J Am Med Assoc 284(22):2901–2906. doi:10.1001/jama.284.22.2901
Rothwell PM, Giles MF, Chandratheva A, Marquardt L, Geraghty O, JNE R, Lovelock CE, Binney LE, Bull LM, Cthbertson FC, SJV W, Bosch S, Carasco-Alexander F, Silver LE, Gutnikov SA, Mehta Z, Study E (2007) Effect of urgent treatment of transient ischaemic attack and minor stroke on early recurrent stroke (EXPRESS study): a prospective population-based sequential comparison. Lancet 370(9596):1432–1442. doi:10.1016/s0140-6736(07)61448-2
Merwick A, Albers GW, Amarenco P, Arsava EM, Ay H, Calvet D, Coutts SB, Cucchiara BL, Demchuk AM, Furie KL, Giles MF, Labreuche J, Lavallee PC, Mas J-L, Olivot JM, Purroy F, Rothwell PM, Saver JL, Sheehan OC, Stack JP, Walsh C, Kelly PJ (2010) Addition of brain and carotid imaging to the ABCD(2) score to identify patients at early risk of stroke after transient ischaemic attack: a multicentre observational study. Lancet Neurol 9(11):1060–1069. doi:10.1016/s1474-4422(10)70240-4
Giles MF, Rothwell PM (2007) Risk of stroke early after transient ischaemic attack: a systematic review and meta-analysis. Lancet Neurol 6(12):1063–1072. doi:10.1016/s1474-4422(07)70274-0
Giles MF, Albers GW, Amarenco P, Arsava EM, Asimos AW, Ay H, Calvet D, Coutts SB, Cucchiara BL, Demchuk AM, Johnston SC, Kelly PJ, Kim AS, Labreuche J, Lavallee PC, Mas JL, Merwick A, Olivot JM, Purroy F, Rosamond WD, Sciolla R, Rothwell PM (2011) Early stroke risk and ABCD2 score performance in tissue- vs time-defined TIA: a multicenter study. Neurology 77(13):1222–1228. doi:10.1212/WNL.0b013e3182309f91
Kobayashi J, Uehara T, Toyoda K, Endo K, Ohara T, Fujinami J, Nagatsuka K, Minematsu K (2013) Clinical significance of fluid-attenuated inversion recovery vascular hyperintensities in transient ischemic attack. Stroke 44(6):1635–1640. doi:10.1161/strokeaha.111.000787
Kamran S, Bates V, Bakshi R, Wright P, Kinkel W, Miletich R (2000) Significance of hyperintense vessels on FLAIR MRI in acute stroke. Neurology 55(2):265–269
Toyoda K, Ida M, Fukuda K (2001) Fluid-attenuated inversion recovery intraarterial signal: an early sign of hyperacute cerebral ischemia. Am J Neuroradiol 22(6):1021–1029
Lee KY, Latour LL, Luby M, Hsia AW, Merino JG, Warach S (2009) Distal hyperintense vessels on FLAIR an MRI marker for collateral circulation in acute stroke? Neurology 72(13):1134–1139. doi:10.1212/01.wnl.0000345360.80382.69
Sanossian N, Saver JL, Alger JR, Kim D, Duckwiler GR, Jahan R, Vinuela F, Ovbiagele B, Liebeskind DS (2009) Angiography reveals that fluid-attenuated inversion recovery vascular hyperintensities are due to slow flow, not thrombus. Am J Neuroradiol 30(3):564–568. doi:10.3174/ajnr.A1388
Lam WWM, Wong KS, So NMC, Yeung TK, Gao S (2004) Plaque volume measurement by magnetic resonance imaging as an index of remodeling of middle cerebral artery: correlation with transcranial color Doppler and magnetic resonance angiography. Cerebrovasc Dis 17(2–3):166–169. doi:10.1159/000075786
Oates CP, Naylor AR, Hartshorne T, Charles SM, Fail T, Humphries K, Aslam M, Khodabakhsh P (2009) Joint recommendations for reporting carotid ultrasound investigations in the United Kingdom. Eur J Vasc Endovasc Surg 37(3):251–261. doi:10.1016/j.ejvs.2008.10.015
Adams HP Jr, Bendixen BH, Kappelle LJ, Biller J, Love BB, Gordon DL, Marsh EE 3rd (1993) Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24(1):35–41
Sanossian N, Ances BM, Shah SH, Kim D, Saver JL, Liebeskind DS (2007) FLAIR vascular hyperintensity may predict stroke after TIA. Clin Neurol Neurosurg 109(7):617–619. doi:10.1016/j.clineuro.2007.05.004
Cheng B, Ebinger M, Kufner A, Koehrmann M, Wu O, Kang D-W, Liebeskind D, Tourdias T, Singer OC, Christensen S, Warach S, Luby M, Fiebach JB, Fiehler J, Gerloff C, Thomalla G, Stroke Imaging Repository S (2012) Hyperintense vessels on acute stroke fluid-attenuated inversion recovery imaging associations with clinical and other MRI findings. Stroke 43(11):2957–2961. doi:10.1161/strokeaha.112.658906
Yoshioka K, Ishibashi S, Shiraishi A, Yokota T, Mizusawa H (2013) Distal hyperintense vessels on FLAIR images predict large-artery stenosis in patients with transient ischemic attack. Neuroradiology 55(2):165–169. doi:10.1007/s00234-012-1092-y
Liu W, Xu G, Yue X, Wang X, Ma M, Zhang R, Wang H, Zhou C, Liu X (2011) Hyperintense vessels on FLAIR: a useful non-invasive method for assessing intracerebral collaterals. Eur J Radiol 80(3):786–791. doi:10.1016/j.ejrad.2010.09.043
Iancu-Gontard D, Oppenheim C, Touze E, Meary E, Zuber M, Mas JL, Fredy D, Meder JF (2003) Evaluation of hyperintense vessels on FLAIR MRI for the diagnosis of multiple intracerebral arterial stenoses. Stroke 34(8):1886–1891. doi:10.1161/01.str.0000080382.61984.fe
Wong KS, Huang YN, Gao S, Lam WW, Chan YL, Kay R (1998) Intracranial stenosis in Chinese patients with acute stroke. Neurology 50(3):812–813
Vilela MD, Newell DW (2008) Superficial temporal artery to middle cerebral artery bypass: past, present, and future. Neurosurg Focus 24(2). doi:10.3171/foc/2008/24/2/e2
Chatzikonstantinou A, Wolf ME, Schaefer A, Hennerici MG (2013) Risk prediction of subsequent early stroke in patients with transient ischemic attacks. Cerebrovasc Dis 36(2):106–109. doi:10.1159/000352060
Calvet D, Touze E, Oppenheim C, Turc G, Meder J-F, Mas J-L (2009) DWI lesions and TIA etiology improve the prediction of stroke after TIA. Stroke 40(1):187–192. doi:10.1161/strokeaha.108.515817
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this study.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in the studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Dong, X., Bai, C. & Nao, J. Influential factors and clinical significance of fluid-attenuated inversion recovery vascular hyperintensities in transient ischemic attacks of carotid arterial system. Neuroradiology 59, 1093–1099 (2017). https://doi.org/10.1007/s00234-017-1906-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-017-1906-z