Abstract
Purpose
Idiopathic intracranial hypertension (IIH) is a disorder of increased intracranial pressure in the absence of any known causative factor. Sinus stenosis is common in these patients. Stenting of stenotic dural sinuses has gained popularity as a treatment option, since these stenoses may contribute to an obstruction of the venous return, and, thereby may contribute to IIH via an increase in venous sinus pressure. We evaluated the safety and efficacy of endovascular treatment in IIH with venous sinus stenosis.
Methods
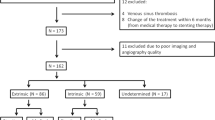
Fifty-one patients with IIH underwent stenting. Median age was 40 years. Clinical manifestation was headache in 74.5% of the patients and visual obscurations in 78.5%. Papilledema was present in 50/51 patients (98%), and lumbar puncture documented elevated CSF opening pressure in all but one patient (98%). Sinus stenoses were observed in all patients.
Results
Endovascular treatment was successfully performed in all patients. There were no major complications encountered (i.e., live threatening or causing a deterioration of a patient’s condition equivalent to mRS 3–6). Improvement or resolution of papilledema was observed in 88% of the patients, and 84% reported improvement or resolution of the headache. Follow-up angiographies were performed in 48 patients at a median interval of 49 months and demonstrated in stent-stenosis or a de novo stenosis in 12 patients, eight of them needed re-treatment.
Conclusion
Venous sinus stenting is a safe and effective alternative to other invasive treatments (e.g., optic nerve sheath fenestration, CSF diversion) in patients with IIH. The majority of patients have a persistent clinical benefit.



Similar content being viewed by others
References
Corbett JJ, Savino PJ, Thompson HS et al (1982) Visual loss in pseudotumor cerebri: follow-up of 57 patients from five to 41 years and a profile of 14 patients with permanent severe visual loss. Arch Neurol 39:461–474
Brodsky MC, Vaphiades M (1998) Magnetic resonance imaging in pseudotumor cerebri. Ophthalmology 105:1686–1693
Degnan AJ, Levy LM (2011) Pseudotumor cerebri: brief review of clinical syndrome and imaging findings. AJNR Am J Neuroradiol 32:1986–1993
Saindane AM, Bruce BB, Riggeal BD, Newman NJ, Biousse V (2013) Association of MRI findings and visual outcome in idiopathic intracranial hypertension. AJR Am J Roentgenol 201:412–418
Farb RI, Vanek I, Scott JN et al (2003) Idiopathic intracranial hypertension: the prevalence and morphology of sinovenous stenosis. Neurology 60:1418–1424
Arac A, Lee M, Steinberg GK et al (2009) Efficacy of endovascular stenting in dural venous sinus stenosis for the treatment of idiopathic intracranial hypertension. Neurosurg Focus 27:E14
Friedman DJ, Liu GT, Digre KB (2013) Revised diagnostic criteria for the pseudotumor cerebri syndrome in adults and children. Neurology 81:1159–1165
King JO, Mitchell PJ, Thomson KR et al (1995) Cerebral venography and manometry in idiopathic intracranial hypertension. Neurology 45:2224–2228
King JO, Mitchell PJ, Thomson KR et al (2002) Manometry combined with cervical puncture in idiopathic intracranial hypertension. Neurology 58:26–30
De Simone R, Marano E, Fiorilio C et al (2005) Sudden re-opening of collapsed transverse sinuses and longstanding clinical remission after a single lumbar puncture in a case of idiopathic intracranial hypertension. Pathogenetic implications. Neurol Sci 25:342–344
Rohr A, Dörner L, Stingele R et al (2007) Reversibility of venous sinus obstruction in idiopathic intracranial hypertension. AJNR Am J Neuroradiol 28:656–659
Celebisoy N, Gokcay F, Sirin H et al (2007) Treatment of idiopathic intracranial hypertension: topiramate vs acetazolamide, an open-label study. Acta Neurol Scand 116:322–327
Johnston I, Paterson A (1974) Benign intracranial hypertension. II CSF pressure and circulation. Brain 97:301–312
Corbett JJ, Thompson HS (1989) The rational management of idiopathic intracranial hypertension. Arch Neurol 1046–51
Lueck C, McIlwaine F (2005) Interventions for idiopahic intrcranial hypertension. Cochrane Database Syst Rev CD003434
Higgins JN, Owler BK, Cousins C et al (2002) Venous sinus stenting for refractory benign intracranial hypertension. Lancet 359:228–230
Ogungbo B, Roy D, Gholkar A et al (2003) Endovascular stenting of the transverse sinus in a patient presenting with benign intracranial hypertension. Br J Neurosurg 17:565–568
Rajpal S, Niemann DB, Turk AS (2005) Transverse venous sinus stent placement as treatment for benign intracranial hypertension in a young male: case report and review of the literature. J Neurosurg 102:342–346
Métellus P, Levrier O, Fuentes S et al (2005) Endovascular treatment of benign intracranial hypertension by stent placement in the transverse sinus: therapeutic and pathophysiological considerations illustrated by a case report. Neurochirurgie 5:113–120
Higgins JN, Cousins C, Owler BK et al (2003) Idiopathic intracranial hypertension: 12 cases treated by venous sinus stenting. J Neurol Neurosurg Psychiatry 74:1662–1666
Owler BK, Parker G, Halmagyi GM et al (2003) Pseudotumour cerebri syndrome: venous sinus obstruction and its treatment with stent placement. J Neurosurg 98:1045–1055
Donnet A, Metellus P, Levrier O et al (2008) Endovascular treatment of idiopathic intracranial hypertension: clinical and radiologic outcome of 10 consecutive patients. Neurology 70:641–647
Bussiere M, Falero R, Nicolle D et al (2010) Unilateral transverse sinus stenting of patients with idiopathic intracranial hypertension. AJNR Am J Neuroradiol 31:645–650
Puffer RC, Mustafa W, Lanzino G (2013) Venous sinus stenting for idiopathic intracranial hypertension: a review of the literature. J Neurointerv Surg 5:483–486
Ahmed RM, Wilkinson M, Parker GD et al (2011) Transverse sinus stenting for idiopathic intracranial hypertension: a review of 52 patients and of model predictions. AJNR Am J Neuroradiol 32:1408–1414
Lenck S, Vallée F, Labeyrie MA, et al. (2017) Stenting of the lateral sinus in idiopathic intracranial hypertension according to the type of stenosis. Neurosurgery 1–8
Tsumoto T, Miyamoto T, Shimizi M et al (2003) Restenosis of the sigmoid sinus after stenting for treatment of intracranial venous hypertension: case report. Neuroradiology 45:911–915
Kumpe DA, Bennett JL, Seinfeld J et al (2012) Dural sinus stent placement for idiopathic intracranial hypertension. J Neurosurg 116:538–548
Ahmed RM, Zmudzki F, Parker GD, et al. (2014) Transverse sinus stenting for pseudotumor cerebri: A cost comparison with CSF shunting. AJNR Am J Neuroradol 35:952–958
Acknowledgment
The authors are most grateful to James Lago for language revision of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
We declare that this retrospective analysis of a series of patients treated according to clinical routine did not follow a pre-given protocol. The Guidelines of the Declaration of Helsinki of the World Medical Association in its current version (WMA, 2004), the Guidelines of Good Clinical Practice (CPMP/ICH/135/95) and demands of the national medical and data protection laws were followed. We declare that the ethics committee waived the obligation of a legal consultation.
Conflict of Interest
MAP serves as a proctor and consultant for phenox and Medtronic; RMM and WK consult for phenox; HH has proctoring and consulting agreements with Medtronic and Balt, and is co-founder and shareholder of phenox.
Rights and permissions
About this article
Cite this article
Aguilar-Pérez, M., Martinez-Moreno, R., Kurre, W. et al. Endovascular treatment of idiopathic intracranial hypertension: retrospective analysis of immediate and long-term results in 51 patients. Neuroradiology 59, 277–287 (2017). https://doi.org/10.1007/s00234-017-1783-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-017-1783-5