Abstract
Introduction
Embolization of intracranial tumor is widely performed in Japan, mainly before neurosurgical resection. A retrospective, multicenter, observational study in Japan was conducted to clarify the nature, frequency, and risk factors of complications in intracranial tumor embolization.
Methods
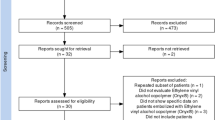
Patients were derived from the Japanese Registry of NeuroEndovascular Therapy 2 (JR-NET2). A total of 20,854 patients were enrolled in JR-NET2, of which 1,018 patients (4.88 %) with intracranial tumors underwent embolization. The primary end point was the proportion of patients with a modified Rankin scale (mRS) score of 0–2 (independency) at 30 days. The secondary end point was the occurrence of complications related to the procedures. The risk factors of the occurrence of complications were studied.
Results
The proportion of patients with mRS scores ≤2 at 30 days after procedure was 91.3 %. Complications occurred in 15 of the 1,012 patients (1.48 %). Multivariate analysis showed that embolization for tumors other than meningioma (OR, 4.626; 95 % CI, 1.347–14.59; p = 0.0105) was significantly associated with the development of complications.
Conclusion
The frequency of complications after intracranial tumor embolization was relatively low in this large Japanese cohort. Embolization for tumors other than meningioma was the only significant risk factor for the occurrence of complications.
Similar content being viewed by others
Abbreviations
- ECA:
-
External carotid artery
- ICA:
-
Internal carotid artery
- IQR:
-
Interquartile range
- JR-NET:
-
Japanese Registry of NeuroEndovascular Therapy
- mRS:
-
Modified Rankin scale
- VBA:
-
Vertebrobasilar artery
References
Hieshima GB, Everhart FR, Mehringer M, Tsai F, Hasso AH, Grinnell VS, Pribram HF, Mok M (1980) Preoperative embolization of meningiomas. Surg Neurol 14:119–127
Manelfe C, Lasjaunias P, Ruscalleda J (1986) Preoperative embolization of intracranial meningiomas. AJNR Am J Neuroradiol 7:963–972
Richter HP, Schachenmayr W (1983) Preoperative embolization of intracranial meningiomas. Neurosurgery 13:261–268
Teasdalf E, Patterson J, Mclellan D, Macpherson P (1984) Subselective preoperative embolization for meningiomas. A radiological and pathological assessment. J Neurosurg 60:506–511
Bendszus M, Rao G, Burger R, Schaller C, Scheineman K, Warmuth-Metz M, Hofmann E, Schramm J, Roosen K, Solymosi L (2000) Is there a benefit of preoperative meningioma embolization? Neurosurgery 47:1306–1312
Bendszus M, Monoranu CM, Schutz A, Nolte I, Vince GH, Solymosi L (2005) Neurologic complications after particle embolization of intracranial meningiomas. AJNR Am J Neuroradiol 26:1413–1419
Rosen CL, Ammerman JM, Sekhar LN, Bank WO (2002) Outcome analysis of preoperative embolization in cranial base surgery. Acta Neurochir 144:1157–1164. doi:10.1007/s00701-002-0965-y
Hyogo T, Taki W, Negoro M, Takahashi A, Edura M, Hyodo A, Kobayashi S, Komiyama M, Kuwayama N, Matsumaru Y, Miyachi S, Murao K, Murayama Y, Nakahara I, Nemoto S, Sakai N, Satoh K, Sonobe M, Sugiu K, Terada T, Yoshimura S, Abe T, Itoh Y, Kiyosue H, Nagashima H, Nakamura M, Matsushima S (2008) Japanese society of neuro-endovascular treatment specialist quantification system. Six years’ experience and introduction of an animal model examination. Interv Neuroradiol 14:235–240
Carli DFM, Sluzewski M, Beute GN, van Rooij WJ (2010) Complications of particle embolization of meningiomas: frequency, risk factors, and outcome. AJNR Am J Neuroradiol 31:152–154. doi:10.3174/ajnr.A1754
Gupta R, Thomas AJ, Horowits M (2006) Intracranial head and neck tumors: endovascular considerations, present and future. Neurosurgery 59:S3-251–S3-260. doi:10.1227/01.NEU.0000239249.65742.1C
Kai Y, Hamada JI, Morioka M, Yano S, Todaka T, Ushio Y (2002) Appropriate interval between embolization and surgery in patients with meningioma. AJNR Am J Neuroradiol 23:139–142
Kai Y, Hamada JI, Morioka M, Yano S, Nakamura H, Makino K, Mizuno T, Takeshima H, Kuratsu JI (2006) Clinical evaluation of cellulose porous beads for the therapeutic embolization of meningiomas. AJNR Am J Neuroradiol 27:1146–1150
Sluzewski M, van Rooji WJ, Lohle PN, Beute GN, Peluso JP (2013) Embolization of meningiomas: comparison of safety between calibrated microspheres and polyvinyl-alcohol particles as embolic agents. AJNR Am J Neuroradiol 34:727–729. doi:10.3174/ajnr.A3311
Dean BL, Fiom RA, Wallace RC, Khayata MH, Obuchowski NA, Hodak JA, Zabramski JM, Spetzler RF (1994) Efficacy of endovascular treatment of meningiomas: evaluation with matched samples. AJNR Am J Neuroradiol 15:1675–1680
Cornelius JF, Saint-Maurice JP, Bresson D, George B, Houdart E (2007) Hemorrhage after particle emboilization of hemangioblastomas: comparison of outcomes in spinal and cerebellar lesions. J Neurosurg 106:994–998
Pauliah M, Saxena V, Haris M, Husain N, Rathore RKS, Gupta RK (2007) Improved T1-weighted contrast-enhanced MRI to probe microvascularity and heterogeneity of human glioma. Magn Reson Imaging 25:1292–1299. doi:10.1016/j.mri.2007.03.027
Yu SCH, Boet R, Wong GKC, Lam WW, Poon WS (2004) Postembolization hemorrhage of a large and necrotic meningioma. AJNR Am J Neuroradiol 25:506–508
Dowd CI, Halbach VV, Higashida T (2003) Meningiomas: the role of preoperative angiography and embolization. Neurosurg Focus 15: article 10
Acknowledgments
This study was supported by research grants for cardiovascular diseases (17C-1, 20C-2) from the Ministry of Health, Labor, and Welfare of Japan. The authors would like to express heartfelt thanks to doctors who devoted their time to this investigation. The JR-NET Study Group: principal investigator Nobuyuki Sakai, Kobe City Medical Center General Hospital, Kobe, Japan; investigators Akio Hyodo, Dokkyo Medical University Koshigaya Hospital, Koshigaya, Japan (17C-1, 20C-2); Shigeru Miyachi, Nagoya University, Nagoya, Japan (17C-1, 20C-2); Yoji Nagai, Translational Research Informatics Center, Kobe, Japan (17C-1, 20C-2); Chiaki Sakai, Institute of Biomedical Research and Innovation, Kobe, Japan (17C-1, 20C-2); Tetsu Satoh, National Cerebral and Cardiovascular Center, Suita, Japan (17C-1, 20C-2); Waro Taki, Mie University, Tsu, Japan (17C-1, 20C-2); Tomoaki Terada, Wakayama Rosai Hospital, Wakayama, Japan (17C-1, 20C-2); Masayuki Ezura, Sendai Medical Center, Sendai, Japan (17C-1); Toshio Hyogo, Nakamura Memorial Hospital, Sapporo, Japan (17C-1); Shunji Matsubara, Tokushima University, Tokushima, Japan (17C-1); Kentaro Hayashi, Nagasaki University, Nagasaki Japan (20C-2); co-investigators Toshiyuki Fujinaka, Osaka University, Suita, Japan; Yasushi Ito, Niigata University, Niigata, Japan; Shigeki Kobayashi, Chiba Emergency Medical Center, Chiba, Japan; Masaki Komiyama, Osaka City General Hospital, Osaka, Japan; Naoya Kuwayama, Toyama University, Toyama, Japan; Yuji Matsumaru, Toranomon Hospital, Japan; Yasushi Matsumoto, Konan Hospital, Sendai, Japan; Yuichi Murayama, Jikei Medical University, Tokyo, Japan; Ichiro Nokahara, Kokura Memorial Hospital, Kokura, Japan; Shigeru Nemoto, Jichi Medical University, Shimotsuke, Japan; Koichi Sato, Tokushima Red Cross Hospital, Tokushima, Japan; Kenji Sugiu, Okayama University, Okayama, Japan; Shinichi Yoshimura, Gifu University, Gifu, Japan; and the certified specialist of Japanese Society of Neuroendovascular Therapy.
Conflict of interest
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hishikawa, T., Sugiu, K., Hiramatsu, M. et al. Nationwide survey of the nature and risk factors of complications in embolization of meningiomas and other intracranial tumors: Japanese Registry of NeuroEndovascular Therapy 2 (JR-NET2). Neuroradiology 56, 139–144 (2014). https://doi.org/10.1007/s00234-013-1300-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-013-1300-4