Abstract
Introduction
This study seeks to describe the predictive value of the signal intensity ratio (SIR) in magnetic resonance imaging-turbo inversion recovery magnitude (MRI-TIRM) in patients with Graves’ orbitopathy (GO) with regard to predictability of therapy response.
Methods
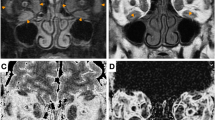
Included in this prospective pilot study were 36 consecutive patients with GO and 25 control subjects. Patients were clinically assessed according to the European Group on Graves’ Orbitopathy recommendations with active GO defined by a clinical activity score (CAS) ≥ 3. On magnetic resonance (MR) imaging, muscle inflammation was measured with a region of interest set within the brightest extra-ocular muscle both on coronal turbo inversion recovery magnitude (TIRM) and on fat suppressed gadolinium-enhanced T1-weighted sequences. To calculate the SIR, the measured signal intensity was set in proportion to that of the ipsilateral temporalis muscle.
Results
Signal intensity ratio in coronal T2-weighted TIRM sequences in either group ranged from 1.22 to 4.92 (mean 2.04) in patients with GO and from 1.18 to 2.4 (mean 1.63) in controls without GO. The observed differences were significant on the TIRM sequences (right eye p = 0.023; left eye p = 0.022), whereas, no significant differences could be detected on the T1-weighted sequences (right eye p = 0.396; left eye p = 0.498). A cut off value of SIR > 2.5 for a CAS ≥ 4 to discriminate active from inactive patients was statistically calculated.
Conclusion
T2 relaxation time is a reliable tool in detecting active GO. The difference in T2-SIR versus T1-SIR is helpful to distinguish inflammatory oedema of the extra ocular muscles from intra-orbital congestion due to reduced venous outflow.


Similar content being viewed by others
References
Mourits MP, Prummel MF, Wiersinga WM, Koornneef L (1997) Clinical activityscore as a guide in the management of patients with Graves’ ophthalmopathy. Clin Endocrinol 47:9–14
Gerding MN, Prummel MF, Wiersinga WM (2000) Assessment of disease activity in Graves’ ophthalmopathy by orbital ultrasonography and clinical parameters. Clin Endocrinol 52:641–646
Young IR, Bydder GM, Hajnal JV (1997) Contrast properties of the inversion recovery sequence. In: Bradley WG Jr, Bydder GM (eds) Advanced MR Imaging Techniques. Martin Dunitz Ltd, London, pp 143–162
European Group on Graves’ Orbitopathy (EUGOGO), Wiersinga WM, Perros P, Kahaly GJ, Mourits MP, Baldeschi L, Boboridis K, Boschi A, Dickinson AJ, Kendall-Taylor P, Krassas GE, Lane CM, Lazarus JH, Marcocci C, Marino M, Nardi M, Neoh C, Orgiazzi J, Pinchera A, Pitz S, Prummel MF, Sartini MS, Stahl M, von Arx G (2006) Clinical assessment of patients with Graves’ orbitopathy: the European Group on Graves’ Orbitopathy recommendations to generalists, specialists and clinical researchers. Eur J Endocrinol 155:387–389
Chang E, Wilson MW, Smith ME (2002) Orbital Imaging in Thyroid Eye Disease.In: Dutton JJ, Haik BG.Thyroid Eye Disease. Diagnosis and Treatment 30:301–308
Bartalena L, Wiersinga WM, Pinchera A (2004) Graves’ ophthalmopathy: state of the art and perspectives. J Endocrinol Invest 27:295–301
Salvi M, Dazzi D, Pellistri I, Neri F, Wall JR (2002) Classification and prediction of the progression of thyroid-associated ophthalmopathy by an artificial neural network. Ophthalmology 109:1703–1708
Eckstein A, Plicht M, Lax H, Neuhäuser M, Mann K, Lederbogen S, Heckmann C, Esser J, Morgenthaler NG (2006) Thyrotropin receptor autoantibodies are independent risk factors for Graves’ ophthalmopathy and help to predict severity and outcome of the disease. J Clin Endocrinol Metab 91:3464–3470
Eckstein AK, Lax H, Lösch C, Glowacka D, Plicht M, Mann K, Esser J, Morgenthaler NG (2007) Patients with severe Graves’ ophthalmopathy have a higher risk of relapsing hyperthyroidism and are unlikely to remain in remission. Clin Endocrinol (Oxf) 67:607–612
Noth D, Gebauer M, Müller B, Bürgi U, Diem P (2001) Graves’ ophthalmopathy: natural history and treatment outcomes. Swiss Med Wkly 131:603–609
Takasu N, Yamashiro K, Komiya I, Ochi Y, Sato Y, Nagata A (2000) Remission of Graves’ hyperthyroidism predicted by smooth decreases of thyroid-stimulating antibody and thyrotropin-binding inhibitor immunoglobulin during antithyroid drug treatment. Thyroid 10:891–896
Villadolid MC, Yokoyama N, Izumi M, Nishikawa T, Kimura H, Ashizawa K, Kiriyama T, Uetani M, Nagataki S (1995) Untreated Graves’ disease patients without clinical ophthalmopathy demonstrate a high frequency of extraocular muscle (EOM) enlargement by magnetic resonance. J Clin Endocrinol Metab 80:2830–2833
Ohnishi T, Noguchi S, Murakami N, Tajiri J, Harao M, Kawamoto H, Hoshi H, Jinnouchi S, Futami S, Nagamachi S (1994) Extraocular muscles in Graves ophthalmopathy: usefulness of T2 relaxation time measurements. Radiology 190:857–862
Pauleit D, Schüller H, Textor J, Leutner C, Keller E, Sommer T, Träber F, Block W, Boldt I, Schild H (1997) MR relaxation time measurements with and without selective fat suppression (SPIR) in endocrine orbitopathy. ROFO 167:557–564
Laitt RD, Hoh B, Wakely C, Kabala J, Harrad R, Potts M (1994) The value of the short tau inversion recovery sequence in magnetic resonance imaging of thyroid eye disease. Br J Radiol 67:244–247
Amano Y, Amano M, Kumazaki T (1997) Normal contrast enhancement of extraocular muscles: fat-suppressed MR findings. Am J Neuroradiol 18:161–164
Link TM, Reimer P, Rummeny EJ, Schuierer G, Grenzebach U, Peters PE (1995) The MRT of the orbit: the value of T1-weighted frequency-selective fat saturation at 1.0 and 1.5 tesla. ROFO 163:406–410
Cakirer S, Cakirer D, Basak M, Durmaz S, Altuntas Y, Yigit U (2004) Evaluation of extraocular muscles in the edematous phase of Graves ophthalmopathy on contrast-enhanced fat-suppressed magnetic resonance imaging. J Comput Assist Tomogr 28:80–86
Yanik B, Conkbayir I, Acaroglu G, Hekimoglu B (2005) Graves’ ophthalmopathy: comparison of the Doppler sonography parameters with the clinical activity score. J Clin Ultrasound 33:375–380
Alp MN, Ozgen A, Can I, Cakar P, Gunalp I (2000) Colour Doppler imaging of the orbital vasculature in Graves’ disease with computed tomographic correlation. Br J Ophthalmol 84:1027–1030
Ott M, Breiter N, Albrecht CF, Pradier O, Hess CF, Schmidberger H (2002) Can contrast enhanced MRI predict the response of Graves’ ophthalmopathy to orbital radiotherapy? Br J Radiol 75:514–517
Taoka T, Sakamoto M, Nakagawa H, Fukusumi A, Iwasaki S, Taoka K, Kichikawa K (2005) Evaluation of extraocular muscles using dynamic contrast enhanced MRI in patients with chronic thyroid orbitopathy. J Comput Assist Tomogr 29:115–120
Mayer EJ, Fox DL, Herdmann G, Hsuan J, Kabala J, Goddard P, Potts MJ, Lee RWJ (2005) Signal intensity, clinical activity and cross-sectional areas on MRI scans in thyroid eye disease. Eur J Radiol 56:20–24
Conflict of interest statement
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Financial support
There was no outside financial support or other financial or personal relationships in connection with the submitted manuscript from any of the authors.
Rights and permissions
About this article
Cite this article
Kirsch, E.C., Kaim, A.H., De Oliveira, M.G. et al. Correlation of signal intensity ratio on orbital MRI-TIRM and clinical activity score as a possible predictor of therapy response in Graves’ orbitopathy—a pilot study at 1.5 T. Neuroradiology 52, 91–97 (2010). https://doi.org/10.1007/s00234-009-0590-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-009-0590-z