Abstract
Introduction
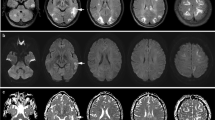
Posterior reversible encephalopathy syndrome (PRES) is a clinico-neuroradiological entity, characterized by typical neurological deficits, distinctive magnetic resonance imaging (MRI) features, and a usually benign clinical course. Although frequently seen in association with hypertensive conditions, many other predisposing factors, notably cytotoxic and immunosuppressant drugs have been associated with PRES. The aim of this study was to determine differences in the MR appearance of PRES according to various risk factors.
Methods
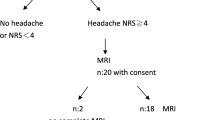
Thirty consecutive patients with clinical and MRI findings consistent with PRES were included. We identified 24 patients with hypertension-related conditions, including 14 patients with preeclampsia–eclampsia, and six patients without hypertension, in whom PRES was associated with exposition to neurotoxic substances. Lesion distribution, extent of disease, and number of affected brain regions were compared between patients with PRES with and without hypertension, and patients with PRES with and without preeclampsia–eclampsia, respectively.
Results
No statistically significant differences in distribution of lesions and extent of disease were observed between patients with PRES with or without hypertension, and patients with or without preeclampsia–eclampsia, respectively. The number of affected brain regions was significantly higher in patients with preeclampsia–eclampsia (p = 0.046), and the basal ganglia region was more frequently involved in these patients (p = 0.066).
Conclusion
Apart from a significant higher number of involved brain regions and a tendency for basal ganglia involvement in patients with PRES associated with preeclampsia–eclampsia, the MRI appearance of patients with PRES does not seem to be influenced by predisposing risk factors.




Similar content being viewed by others
References
Hinchey J, Chaves C, Appignani B, Breen J, Pao L, Wang A, Pessin MS, Lamy C, Mas JL, Caplan LR (1996) A reversible posterior leukoencephalopathy syndrome. N Engl J Med 334:494–500. doi:10.1056/NEJM199602223340803
McKinney AM, Short J, Truwit CL, McKinney ZJ, Kozak OS, SantaCruz KS, Teksam M (2007) Posterior reversible encephalopathy syndrome: incidence of atypical regions of involvement and imaging findings. AJR Am J Roentgenol 189:904–912. doi:10.2214/AJR.07.2024
Covarrubias DJ, Luetmer PH, Campeau NG (2002) Posterior reversible encephalopathy syndrome: prognostic utility of quantitative diffusion-weighted MR images. AJNR Am J Neuroradiol 23:1038–1048
Bartynski WS, Boardman JF (2007) Distinct imaging patterns and lesion distribution in posterior reversible encephalopathy syndrome. AJNR Am J Neuroradiol 28:1320–1327. doi:10.3174/ajnr.A0549
Bartynski WS, Boardman JF, Zeigler ZR, Shadduck RK, Lister J (2006) Posterior reversible encephalopathy syndrome in infection, sepsis, and shock. AJNR Am J Neuroradiol 27:2179–2190
Ito Y, Arahata Y, Goto Y, Hirayama M, Nagamutsu M, Yasuda T, Yanagi T, Sobue G (1998) Cisplatin neurotoxicity presenting as reversible posterior leukoencephalopathy syndrome. AJNR Am J Neuroradiol 19:415–417
Russell MT, Nassif AS, Cacayorin ED, Awwad E, Perman W, Dunphy F (2001) Gemcitabine-associated posterior reversible encephalopathy syndrome: MR imaging and MR spectroscopy findings. Magn Reson Imaging 19:129–132. doi:10.1016/S0730-725X(01)00217-X
Kastrup O, Maschke M, Wanke I, Diener HC (2002) Posterior reversible encephalopathy syndrome due to severe hypercalcemia. J Neurol 249:1563–1566. doi:10.1007/s00415-002-0895-x
Ito Y, Niwa H, Iida T, Nagamatsu M, Yasuda T, Yanagi T, Sobue G (1997) Post-transfusion reversible posterior leukoencephalopathy syndrome with cerebral vasoconstriction. Neurology 49:1174–1175
Strandgaard S, Paulson OB (1984) Cerebral autoregulation. Stroke 15:413–416
Tamaki K, Sadoshima S, Baumbach GL, Iadecola C, Reis DJ, Heistad DD (1984) Evidence that disruption of the blood–brain barrier precedes reduction in cerebral blood flow in hypertensive encephalopathy. Hypertension 6:I75–I81
Mukherjee P, McKinstry RC (2001) Reversible posterior leukoencephalopathy syndrome: evaluation with diffusion-tensor MR imaging. Radiology 219:756–765
Rodgers GM, Taylor RN, Roberts JM (1988) Preeclampsia is associated with a serum factor cytotoxic to human endothelial cells. Am J Obstet Gynecol 159:908–914
National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescent (2004) The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics 114:555–576. doi:10.1542/peds.114.2.S2.555
Port JD, Beauchamp NJ Jr (1998) Reversible intracerebral pathologic entities mediated by vascular autoregulatory dysfunction. Radiographics 18:353–367
Ay H, Buonanno FS, Schaefer PW, Le DA, Wang B, Gonzalez RG, Koroshetz WJ (1998) Posterior leukoencephalopathy without severe hypertension: utility of diffusion-weighted MRI. Neurology 51:1369–1376
Jansen O, Krieger D, Krieger S, Sartor K (1996) Cortical hyperintensity on proton density-weighted images: an MR sign of cyclosporine-related encephalopathy. AJNR Am J Neuroradiol 17:337–344
Rangi PS, Partridge WJ, Newlands ES, Waldman AD (2005) Posterior reversible encephalopathy syndrome: a possible late interaction between cytotoxic agents and general anaesthesia. Neuroradiology 47:586–590. doi:10.1007/s00234-005-1376-6
Benigni A, Morigi M, Perico N, Zoja C, Amuchastegui CS, Piccinelli A, Donadelli R, Remuzzi G (1992) The acute effect of FK506 and cyclosporine on endothelial cell function and renal vascular resistance. Transplantation 54:775–780. doi:10.1097/00007890-199211000-00002
Zoja C, Furci L, Ghilardi F, Zilio P, Benigni A, Remuzzi G (1986) Cyclosporin-induced endothelial cell injury. Lab Invest 55:455–462
Kochi S, Takanaga H, Matsuo H, Naito M, Tsuruo T, Sawada Y (1999) Effect of cyclosporin A or tacrolimus on the function of blood–brain barrier cells. Eur J Pharmacol 372:287–295. doi:10.1016/S0014-2999(99)00247-2
Kochi S, Takanaga H, Matsuo H, Ohtani H, Naito M, Tsuruo T, Sawada Y (2000) Induction of apoptosis in mouse brain capillary endothelial cells by cyclosporin A and tacrolimus. Life Sci 66:2255–2260. doi:10.1016/S0024-3205(00)00554-3
Marsen TA, Weber F, Egink G, Suckau G, Baldamus CA (1999) Cyclosporin A induces prepro endothelin-1 gene transcription in human endothelial cells. Eur J Pharmacol 379:97–106. doi:10.1016/S0014-2999(99)00447-1
Truwit CL, Denaro CP, Lake JR, DeMarco T (1991) MR imaging of reversible cyclosporin A-induced neurotoxicity. AJNR Am J Neuroradiol 12:651–659
Badros A, Goloubeva O, Dalal JS, Can I, Thompson J, Rapoport AP, Heyman M, Akpek G, Fenton RG (2007) Neurotoxicity of bortezomib therapy in multiple myeloma: a single-center experience and review of the literature. Cancer 110:1042–1049. doi:10.1002/cncr.22921
Bartynski WS (2008) Posterior reversible encephalopathy syndrome, part 2: controversies surrounding pathophysiology of vasogenic edema. AJNR Am J Neuroradiol 29:1043–1049. doi:10.3174/ajnr.A0929
Horbinski C, Bartynski WS, Carson-Walter E, Hamilton RL, Tan HP, Cheng S (2009) Reversible Encephalopathy after Cardiac Transplantation: Histologic Evidence of Endothelial Activation, T-cell Specific Trafficking, and Vascular Endothelial Growth Factor Expression. AJNR Am J Neuroradiol. doi:10.3174/ajnr.A1311
Schoch HJ, Fischer S, Marti HH (2002) Hypoxia-induced vascular endothelial growth factor expression causes vascular leakage in the brain. Brain 125:2549–2557. doi:10.1093/brain/awf257
Bartynski WS, Boardman JF (2008) Catheter angiography, MR angiography, and MR perfusion in posterior reversible encephalopathy syndrome. AJNR Am J Neuroradiol 29:447–455. doi:10.3174/ajnr.A0839
Brubaker LM, Smith JK, Lee YZ, Lin W, Castillo M (2005) Hemodynamic and permeability changes in posterior reversible encephalopathy syndrome measured by dynamic susceptibility perfusion-weighted MR imaging. AJNR Am J Neuroradiol 26:825–830
Sundgren PC, Edvardsson B, Holtas S (2002) Serial investigation of perfusion disturbances and vasogenic oedema in hypertensive encephalopathy by diffusion and perfusion weighted imaging. Neuroradiology 44:299–304. doi:10.1007/s00234-001-0721-7
Demirtas O, Gelal F, Vidinli BD, Demirtas LO, Uluc E, Baloglu A (2005) Cranial MR imaging with clinical correlation in preeclampsia and eclampsia. Diagn Interv Radiol 11:189–194
Schwartz RB, Feske SK, Polak JF, DeGirolami U, Iaia A, Beckner KM, Bravo SM, Klufas RA, Chai RY, Repke JT (2000) Preeclampsia–eclampsia: clinical and neuroradiographic correlates and insights into the pathogenesis of hypertensive encephalopathy. Radiology 217:371–376
Watanabe Y, Mitomo M, Tokuda Y, Yoshida K, Choi S, Hosoki T, Ban C (2002) Eclamptic encephalopathy: MRI, including diffusion-weighted images. Neuroradiology 44:981–985. doi:10.1007/s00234-002-0867-y
Servillo G, Striano P, Striano S, Tortora F, Boccella P, De Robertis E, Rossano F, Briganti F, Tufano R (2003) Posterior reversible encephalopathy syndrome (PRES) in critically ill obstetric patients. Intensive Care Med 29:2323–2326. doi:10.1007/s00134-003-1901-1
Rappaport VJ, Hirata G, Yap HK, Jordan SC (1990) Anti-vascular endothelial cell antibodies in severe preeclampsia. Am J Obstet Gynecol 162:138–146
Feekes JA, Cassell MD (2006) The vascular supply of the functional compartments of the human striatum. Brain 129:2189–2201. doi:10.1093/brain/awl158
Conflict of interest statement
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mueller-Mang, C., Mang, T., Pirker, A. et al. Posterior reversible encephalopathy syndrome: do predisposing risk factors make a difference in MRI appearance?. Neuroradiology 51, 373–383 (2009). https://doi.org/10.1007/s00234-009-0504-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-009-0504-0