Abstract
Purpose
Transcatheter aortic valve replacement (TAVR) is increasingly carried out in patients with aortic valvular conditions. Atrial fibrillation (AF) is a common comorbidity among patients undergoing TAVR. Despite this, there remains a paucity of data and established guidelines regarding anticoagulation use post-TAVR in patients with AF.
Methods
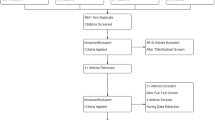
Four databases were searched from inception until 12 October 2021. A title and abstract sieve, full-text review and data extraction were conducted by independent authors, and articles including patients without AF were excluded. The Review Manager (Version 5.4) was utilised in data analysis.
Results
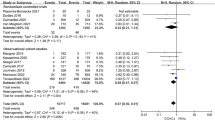
A total of 25,199 post-TAVR patients with AF were included from seven articles, with 9764 patients on non-vitamin K antagonist oral anticoagulants (NOAC) and 15,435 patients on vitamin K antagonists (VKA). In this analysis, there was a significantly lower risk of all-cause mortality at 1 year (RR: 0.75, CI: 0.58–0.97, p = 0.04, I2 = 56%), and bleeding at 1 year (RR: 0.73, CI: 0.68–0.79, p = < 0.00001, I2 = 0%), between patients on NOAC and VKA. There were no detectable differences between patients on NOAC and VKA for all-cause mortality at 2 years, stroke within 30 days, stroke within 1 year, ischaemic stroke at 1 year and life-threatening bleeding at 30 days.
Conclusion
While the results of this analysis reveal NOAC as a potential alternate treatment modality to VKA in post-TAVR patients with AF, further research is needed to determine the full safety and efficacy profile of NOAC (PROSPERO: CRD42021283548).









Similar content being viewed by others
Data availability
Data sharing is not applicable to this article as no datasets were generated or analysed during the current study.
References
Mahmaljy H, Tawney A, MY. Transcatheter aortic valve replacement. StatPearls [Internet]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK431075/. Accessed 10 Dec 2021.
Carroll JD, Mack MJ, Vemulapalli S et al (2020) STS-ACC TVT Registry of Transcatheter Aortic Valve Replacement. J Am Coll Cardiol 76(21):2492–2516. https://doi.org/10.1016/j.jacc.2020.09.595
Soong E, Jing O, Ho J et al (2021) Transcatheter aortic valve replacement for aortic regurgitation in Asians: TAVR for aortic regurgitation in Asians. AsiaIntervention 7(2):103–11. https://doi.org/10.4244/aij-d-21-00007
Ancona R, Pinto SC (2020) Epidemiology of aortic valve stenosis (AS) and of aortic valve incompetence (AI): is the prevalence of AS/AI similar in different parts of the world? Available from: https://www.escardio.org/Journals/E-Journal-of-Cardiology-Practice/Volume-18/epidemiology-of-aortic-valve-stenosis-as-and-of-aortic-valve-incompetence-ai. Accessed 22 Dec 2021
Organisation WH Ageing and Health (2021) Available from: https://www.who.int/news-room/fact-sheets/detail/ageing-and-health. Accessed 22 Dec 2021
Bana A (2019) TAVR-present, future, and challenges in developing countries. Indian J Thorac Cardiovasc Surg 35(3):473–484. https://doi.org/10.1007/s12055-018-00786-8
Mojoli M, Gersh BJ, Barioli A et al (2017) Impact of atrial fibrillation on outcomes of patients treated by transcatheter aortic valve implantation: a systematic review and meta-analysis. Am Heart J 192:64–75. https://doi.org/10.1016/j.ahj.2017.07.005
Jeong HK, Yoon N, Kim JH et al (2021) Post-operative atrial fibrillation impacts on outcomes in transcatheter and surgical aortic valve replacement. Front Cardiovasc Med 8:789548–789648. https://doi.org/10.3389/fcvm.2021.789548
Hindricks G, Potpara T, Dagres N et al (2021) 2020 ESC guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS): the task force for the diagnosis and management of atrial fibrillation of the European Society of Cardiology (ESC) developed with the special contribution of the European Heart Rhythm Association (EHRA) of the ESC. Eur Heart J 42(5):373–498. https://doi.org/10.1093/eurheartj/ehaa612
McRae HL, Militello L, Refaai MA (2021) Updates in anticoagulation therapy monitoring. Biomedicines 9(3):262. https://doi.org/10.3390/biomedicines9030262
Hart RG, Pearce LA, Aguilar MI (2007) Meta-analysis: antithrombotic therapy to prevent stroke in patients who have nonvalvular atrial fibrillation. Ann Intern Med 146(12):857–867. https://doi.org/10.7326/0003-4819-146-12-200706190-00007
Tadros R, Shakib S (2010) Warfarin–indications, risks and drug interactions. Aust Fam Physician 39(7):476–479
Kimmel SE (2008) Warfarin therapy: in need of improvement after all these years. Expert Opin Pharmacother 9(5):677–686. https://doi.org/10.1517/14656566.9.5.677
Kozieł M, Teutsch C, Bayer V et al (2021) Changes in anticoagulant prescription patterns over time for patients with atrial fibrillation around the world. J Arrhythmia 37(4):990–1006. https://doi.org/10.1002/joa3.12588
Bauer KA (2013) Pros and cons of new oral anticoagulants. Hematology Am Soc Hematol Educ Program 2013(1):464–470. https://doi.org/10.1182/asheducation-2013.1.464
Ruff CT, Giugliano RP, Braunwald E et al (2014) Comparison of the efficacy and safety of new oral anticoagulants with warfarin in patients with atrial fibrillation: a meta-analysis of randomised trials. The Lancet 383(9921):955–962. https://doi.org/10.1016/S0140-6736(13)62343-0
Patel MR, Mahaffey KW, Garg J et al (2011) Rivaroxaban versus warfarin in nonvalvular atrial fibrillation. N Engl J Med 365(10):883–891. https://doi.org/10.1056/NEJMoa1009638
Connolly SJ, Ezekowitz MD, Yusuf S et al (2009) Dabigatran versus warfarin in patients with atrial fibrillation. N Engl J Med 361(12):1139–1151. https://doi.org/10.1056/NEJMoa0905561
Granger CB, Alexander JH, McMurray JJ et al (2011) Apixaban versus warfarin in patients with atrial fibrillation. N Engl J Med 365(11):981–992. https://doi.org/10.1056/NEJMoa1107039
Giugliano RP, Ruff CT, Braunwald E et al (2013) Edoxaban versus warfarin in patients with atrial fibrillation. N Engl J Med 369(22):2093–2104. https://doi.org/10.1056/NEJMoa1310907
Jochheim D, Barbanti M, Capretti G et al (2019) Oral anticoagulant type and outcomes after transcatheter aortic valve replacement. JACC Cardiovasc Interv 12(16):1566–1576. https://doi.org/10.1016/j.jcin.2019.03.003
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred Reporting Items for Systematic Reviews And Meta-Analyses: the PRISMA statement. BMJ 339:b2535. https://doi.org/10.1136/bmj.b2535
Review Manager (RevMan) (2020) Version 5.4 ed: The Cochrane Collab
Higgins JPT, Thomas J, Chandler J et al (2019) Cochrane Handbook for Systematic Reviews of Interventions. The Cochrane Collab
Sterne JAC, Savović J, Page MJ et al (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898. https://doi.org/10.1136/bmj.l4898
McGuinness LA, Higgins JPT (2020) Risk-of-bias VISualization (robvis): an R package and Shiny web app for visualizing risk-of-bias assessments. Res Synth Methods n/a(n/a). https://doi.org/10.1002/jrsm.1411
Wells GA, Shea B, O'Connell D et al (2021) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. Available from: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed 20 Dec 2021
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. Bmj 315(7109):629–34. https://doi.org/10.1136/bmj.315.7109.629
Butt JH, De Backer O, Olesen JB et al (2021) Vitamin K antagonists vs. direct oral anticoagulants after transcatheter aortic valve implantation in atrial fibrillation. Eur Heart J Cardiovasc Pharmacother 7(1):11–19. https://doi.org/10.1093/ehjcvp/pvz064
Kawashima H, Watanabe Y, Hioki H et al (2020) Direct oral anticoagulants versus vitamin K antagonists in patients with atrial fibrillation after TAVR. JACC Cardiovasc Interv 13(22):2587–2597. https://doi.org/10.1016/j.jcin.2020.09.013
Van Mieghem NM, Unverdorben M, Hengstenberg C et al (2021) Edoxaban versus vitamin K antagonist for atrial fibrillation after TAVR. N Engl J Med 385(23):2150–2160. https://doi.org/10.1056/NEJMoa2111016
Seeger J, Gonska B, Rodewald C, Rottbauer W, Wöhrle J (2017) Apixaban in patients with atrial fibrillation after transfemoral aortic valve replacement. JACC Cardiovasc Interv 10(1):66–74. https://doi.org/10.1016/j.jcin.2016.10.023
Kosmidou I, Liu Y, Alu MC et al (2019) Antithrombotic therapy and cardiovascular outcomes after transcatheter aortic valve replacement in patients with atrial fibrillation. JACC Cardiovasc Interv 12(16):1580–1589. https://doi.org/10.1016/j.jcin.2019.06.001
Mangner N, Crusius L, Haussig S et al (2019) Continued versus interrupted oral anticoagulation during transfemoral transcatheter aortic valve implantation and impact of postoperative anticoagulant management on outcome in patients with atrial fibrillation. Am J Cardiol 123(7):1134–1141. https://doi.org/10.1016/j.amjcard.2018.12.042
Tanawuttiwat T, Stebbins A, Marquis-Gravel G et al (2022) Use of direct oral anticoagulant and outcomes in patients with atrial fibrillation after transcatheter aortic valve replacement: insights from the STS/ACC TVT Registry. J Am Heart Assoc 11(1):e023561. https://doi.org/10.1161/jaha.121.023561
Herold J, Herold-Vlanti V, Sherif M et al (2017) Analysis of cardiovascular mortality, bleeding, vascular and cerebrovascular events in patients with atrial fibrillation vs. sinus rhythm undergoing transfemoral transcatheter aortic valve implantation (TAVR). BMC Cardiovasc Disord 17(1):298–98. https://doi.org/10.1186/s12872-017-0736-6
Chen Y-F, Liu F, Li X-W et al (2022) Non-vitamin K oral anticoagulants versus vitamin K antagonists in post transcatheter aortic valve replacement patients with clinical indication for oral anticoagulation: a meta-analysis. Clin Cardio n/a(n/a). https://doi.org/10.1002/clc.23793
Bassand JP, Virdone S, Badoz M et al (2021) Bleeding and related mortality with NOACs and VKAs in newly diagnosed atrial fibrillation: results from the GARFIELD-AF registry. Blood Adv 5(4):1081–1091. https://doi.org/10.1182/bloodadvances.2020003560
Mentias A, Saad M, Girotra S et al (2019) Impact of pre-existing and new-onset atrial fibrillation on outcomes after transcatheter aortic valve replacement. JACC Cardiovasc Interv 12(21):2119–2129. https://doi.org/10.1016/j.jcin.2019.06.019
Collet J-P, Van Belle E, Thiele H et al (2022) Apixaban vs. standard of care after transcatheter aortic valve implantation: the ATLANTIS trial. Euro Heart. https://doi.org/10.1093/eurheartj/ehac242
Dangas GD, Tijssen JGP, Wöhrle J et al (2019) A controlled trial of rivaroxaban after transcatheter aortic-valve replacement. N Engl J Med 382(2):120–129. https://doi.org/10.1056/NEJMoa1911425
Guimarães HP, Lopes RD, de Barros e Silva PGM et al (2020) Rivaroxaban in patients with atrial fibrillation and a bioprosthetic mitral valve. N Engl J Med 383(22):2117–26. https://doi.org/10.1056/NEJMoa2029603.
Ruile P, Neumann F-J (2017) Valve thrombosis after TAVI. Eur Heart Journal 38(36):2700–2701. https://doi.org/10.1093/eurheartj/ehx472
Sondergaard L, De Backer O, Kofoed KF et al (2017) Natural history of subclinical leaflet thrombosis affecting motion in bioprosthetic aortic valves. Eur Heart Journal 38(28):2201–2207. https://doi.org/10.1093/eurheartj/ehx369
Auffret V, Regueiro A, Del Trigo M et al (2016) Predictors of early cerebrovascular events in patients with aortic stenosis undergoing transcatheter aortic valve replacement. J Am Coll Cardiol 68(7):673–684. https://doi.org/10.1016/j.jacc.2016.05.065
Mentias A, Saad M, Girotra S et al (2019) Impact of pre-existing and new-onset atrial fibrillation on outcomes after transcatheter aortic valve replacement. JACC Cardiovasc Interv 12(21):2119–2129. https://doi.org/10.1016/j.jcin.2019.06.019
Biviano AB, Nazif T, Dizon J et al (2016) Atrial fibrillation is associated with increased mortality in patients undergoing transcatheter aortic valve replacement. Circ Cardiovasc Interv 9(1):e002766. https://doi.org/10.1161/CIRCINTERVENTIONS.115.002766.
O’Gara PT, Kushner FG, Ascheim DD et al (2013) 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 61(4):e78–e140. https://doi.org/10.1016/j.jacc.2012.11.019
Funding
Ching-Hui Sia was supported by the National University of Singapore Yong Loo Lin School of Medicine’s Junior Academic Faculty Scheme.
Author information
Authors and Affiliations
Contributions
Conceptualization, Amanda Jia Qi Ooi, Chloe Wong, Timothy Wei Ern Tan, Trina Priscilla Ng, Yao Neng Teo, Yao Hao Teo, Nicholas L. Syn, Andie H. Djohan, Yinghao Lim, Leonard L. L. Yeo, Benjamin Y. Q. Tan, Mark Yan-Yee Chan, Kian-Keong Poh, William K. F. Kong, Ping Chai, Tiong-Cheng Yeo, James W. Yip, Ivandito Kuntjoro and Ching-Hui Sia. Methodology, Amanda Jia Qi Ooi, Chloe Wong, Timothy Wei Ern Tan, Trina Priscilla Ng, Yao Neng Teo, Yao Hao Teo, Nicholas L. Syn, Andie H. Djohan, Yinghao Lim, Leonard L. L. Yeo, Benjamin Y. Q. Tan, Mark Yan-Yee Chan, Kian-Keong Poh, William K. F. Kong, Ping Chai, Tiong-Cheng Yeo, James W. Yip, Ivandito Kuntjoro and Ching-Hui Sia. Formal analysis and investigation, Amanda Jia Qi Ooi, Chloe Wong, Timothy Wei Ern Tan, Trina Priscilla Ng, Yao Neng Teo, Yao Hao Teo, Nicholas L. Syn, Andie H. Djohan, Yinghao Lim, Leonard L. L. Yeo, Benjamin Y. Q. Tan, Mark Yan-Yee Chan, Kian-Keong Poh, William K. F. Kong, Ping Chai, Tiong-Cheng Yeo, James W. Yip, Ivandito Kuntjoro and Ching-Hui Sia. Writing — original draft preparation, Amanda Jia Qi Ooi, Chloe Wong, Timothy Wei Ern Tan, Trina Priscilla Ng and Ching-Hui Sia. Writing — review and editing, Amanda Jia Qi Ooi, Chloe Wong, Timothy Wei Ern Tan, Trina Priscilla Ng, Yao Neng Teo, Yao Hao Teo, Nicholas L. Syn, Andie H. Djohan, Yinghao Lim, Leonard L. L. Yeo, Benjamin Y. Q. Tan, Mark Yan-Yee Chan, Kian-Keong Poh, William K. F. Kong, Ping Chai, Tiong-Cheng Yeo, James W. Yip, Ivandito Kuntjoro and Ching-Hui Sia. Funding acquisition, Ching-Hui Sia. Resources, Ching-Hui Sia. Supervision, Ching-Hui Sia.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Both Ivandito Kuntjoro and Ching-Hui Sia co-supervised this paper.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ooi, A.J.Q., Wong, C., Tan, T.W.E. et al. A systematic review and meta-analysis of non-vitamin K antagonist oral anticoagulants vs vitamin K antagonists after transcatheter aortic valve replacement in patients with atrial fibrillation. Eur J Clin Pharmacol 78, 1589–1600 (2022). https://doi.org/10.1007/s00228-022-03371-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-022-03371-6