Abstract
Purpose
The purpose of this review is to address the issue of endpoints in paediatric oncology. Oncologists use this term to refer to an outcome they are trying to measure with a clinical trial, which may become accordingly the object of scientific articles. The outcome measured may concern both efficacy and safety, although from different perspectives.
Methods
Based on both literature and experience developed in clinical trials, the different types of endpoints have been critically analysed in their power to provide the highest information of therapeutic interest (efficacy and safety) with the least risk and discomfort for the individual. Primary, secondary and surrogate endpoints have been distinguished. The most relevant differences have been discussed in comparison with adult oncology settings of endpoints.
Results
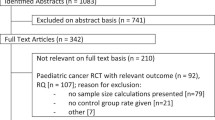
The rarity of cancer in childhood and adolescence and the objective difficulty of enrolling statistically conceivable numbers of individuals have determined the utmost positive development of large scale, multinational clinical trials. The most interesting consequence is that the impact of multiplicity interferences, which is usually present in virtually all clinical trials developed for adults with cancer, is not a common event in paediatric oncology. Nevertheless, many of the questions concerning the different impact on outcome and survival of clinical trials developed in adult oncology remain unanswered due to the objective limitations still existing in terms of cure compared with paediatric oncology. The powerful consistency of cure rate, as the most relevant endpoint of clinical trials developed in paediatric oncology, addresses additional considerations to support the relevant differences existing between adult and paediatric oncology: both the development of clinical trials with different aims (confirmatory versus primary response) and the limited impact of multiplicity limitations may determine different implications regarding the meaning of endpoints in paediatric and adult oncology.
Conclusion
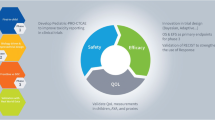
The aim of cancer treatment is to improve survival (SUR) and quality of life (QoL), but some restraints on the conduct of clinical trials may make these goals unattainable. Clinical trial endpoints represent a measure method aimed to grant answers to questions addressed by the clinical trial itself. The effect of the new regulation is expected to stimulate high-quality research and provide robust information on paediatric drugs to increase the availability of such drugs to children.
Similar content being viewed by others
References
EMEA (2003) Committee for Medicinal Products for Human Use. Note for guidance on evaluation of anticancer medicinal products in man—addendum on paediatric oncology; London, 24 July 2003. http://www.emea.europa.eu.int CPMP/EWP/569/02. Accessed 15 March 2010
Oeffinger KC, Mertens AC, Sklar CA, Kawashima T, Hudson MM, Meadows AT, Friedman DL, Marina N, Hobbie W, Kadan-Lottick NS, Schwartz CL, Leisenring W, Robison LL for the Childhood Cancer Survivor Study (2006) Chronic health conditions in adult survivors of childhood cancer. N Engl J Med 355(15):1572–1582
Oeffinger KC, Hudson MM (2004) Long-term complications following childhood and adolescent cancer: foundations for providing risk-based health care for survivors. CA Cancer J Clin 54:208–236
EMEA (2006) Committee for Medicinal Products for Human Use. Guideline on clinical trials in small populations; London, 27 July 2006. http://www.emea.europa.eu.int Ref. CHMP/EWP/83561/2005. Accessed 15 March 2010
European Parliament and Council Directive 2001/20/EC on the approximation of the laws, regulations and administrative provisions of the Member States relating to the implementation of Good Clinical Practice in conduct of clinical trials on medical products for human use. Official Journal of the European Union 1.5.2000; L 121/34
Regulation (EC) n. 1901/2006 of the European Parliament and of the Council of 12 December 2006 on medicinal products for paediatric use and amending Regulation (EEC) No 1768/92, Directive 2001/20/EC, Directive 2001/83/EC and Regulation (EC) No 726/2004. Official Journal of the European Union 27.12.2006, L378/1-L378/19
Regulation (EC) n. 1902/2006 of the European Parliament and of the Council of 20 December 2006 amending Regulation 1901/2006 on medicinal products for paediatric use. Official Journal of the European Union 27.12.2006, L378/20-L378/21
CancerGuide. Endpoints: how the results of clinical trials are measured; http://www.CancerGuide.org/endpoints.html. Accessed 15 March 2010
Guidance for Industry (2007) Clinical trial endpoints for the approval of cancer drugs and biologics. US Department of Health and Human Services Food and Drug Administration. May 2007
EMEA (2006) Committee for Medicinal Products for Human Use. Appendix 1 to the guideline on the evaluation of anticancer medicinal products in man (CHMP/EWP/205/95 REV.3). Methodological consideration for using progression-free survival (PFS) as primary endpoint in confirmatory trials for registration. London, 27 July 2006. http://www.emea.europa.eu.int CHMP/EWP/267575/2006. Accessed 15 March 2010
O’Neill RT (1997) Secondary endpoint cannot be validly analyzed if the primary endpoint does not demonstrate clear statistical significance. Control Clin Trials 18:550–556
Roila F, Cortesi E (2001) Quality of life as primary endpoint in oncology. Ann Oncol 12:3–6
Sullivan R (2004) Clinical trial design in oncology. Lancet Oncol 5(12):759–763
EMEA (2005) Committee for Medicinal Products for Human Use. Guideline on evaluation of anticancer medicinal products in man; London, 14 December 2005; http://www.emea.europa.eu.int CPMP/EWP/205/95. Accessed 15 March 2010
Prentice RL (1989) Surrogate endpoints in clinical trials: definition and operational criteria. Stat Med 8:431–440
Cooper R, Kaanders JHAM (2005) Biological surrogate end-points in cancer trials: potential uses, benefits and pitfalls. Eur J Cancer 41:1261–1266
Acknowledgement
This contribution is part of the Task-force in Europe for Drug Development for the Young (TEDDY) Network of Excellence supported by the European Commission’s Sixth Framework Program (Contract no. 0005216 LSHBCT-2005-005126).
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Part of Teddy Supplement
Rights and permissions
About this article
Cite this article
Paolucci, P., Cioni, V., Bigi, E. et al. Endpoints in paediatric oncology. Eur J Clin Pharmacol 67 (Suppl 1), 33–40 (2011). https://doi.org/10.1007/s00228-010-0923-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-010-0923-1