Abstract
Background
Thalassemia may alter the pharmacokinetics of several drugs in thalassemic patients. Paracetamol is a commonly used analgesic and antipyretic drug which is extensively metabolized in the liver via glucuronidation. The aim of this study was to compare the pharmacokinetics of paracetamol (PCM) and its metabolites [paracetamol glucuronide (PCM-G), paracetamol sulfate (PCM-S), and paracetamol cysteine (PCM-C)] in 16 patients with 16 normal subjects.
Method
Following an overnight fast, a single dose of paracetamol (1,000 mg of Tylenol®) was given and blood samples were obtained at predose, 0.5, 1, 1.5, 2, 3, 4, 5, 7, and 9 h after dosing for determination of the plasma levels of PCM and its metabolites by high-performance liquid chromatography.
Results
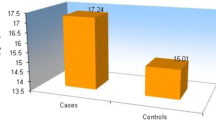
There was no significant difference in maximum concentration of PCM between groups. However, a significantly shorter elimination half-life of PCM was observed in the thalassemic subjects (p<0.001). Total apparent clearance of PCM was significantly faster in thalassemic subjects (p<0.01) while the apparent volume of distribution of PCM did not change. The area under the concentration time curve (AUC0->∞) of PCM-G and PCM-S increased in thalassemic subjects (p<0.05) whereas this parameter for PCM-C was slightly lower in the patients. The half-lives of PCM metabolites were significantly shorter (p<0.01) in thalassemic subjects.
Conclusion
The results indicate that the elimination of PCM and its metabolites in thalassemic subjects is faster than that in normal subjects. Our pharmacokinetic data provide additional evidence that plasma PCM-G is higher in thalassemic patients with hyperbilirubinemia, which could be a casual relationship in regulating the UDP-glucuronosyltransferase expression.



Similar content being viewed by others
References
Fucharoen S, Winichagoon P, Pootrakul P, Piankijagum A, Wasi P (1987) Variable severity of Southeast Asian β-thalassemia/hemoglobin E diseases. Birth Defects Orig Artic Ser 23:241–248
Weatherall DJ (1998) Thalassemia in the next millennium. Ann N Y Acad Sci 850:1–9
Sanchaisuriya K, Fucharoen G, Sae-ung N, Jetsrisuparb A, Fucharoen S (2003) Molecular and hematologic features of hemoglobin E heterozygotes with different forms of alpha-thalassemia in Thailand. Ann Hematol 82(10):612–616
Fucharoen S, Ketvichit P, Pootrakul P et al (2000) Clinical manifestation of beta-thalassemia/hemoglobin E disease. J Pediatr Hematol Oncol 22:552–557
Rund D, Rachmilewitz E (2005) Beta-thalassemia. N Engl J Med 353(11):1135–1146
Blendis LM, Modell CB, Bowdler AJ, Williams R (1974) Some effects of splenectomy in thalassaemia major. Br J Haematol 28:77
Aessopos A, Farmakis D, Karagiorga M, Voskaridou E, Loutradi A, Hatziliami A, Joussef J, Rombos J, Loukopoulos D (2001) Cardiac involvement in thalassemia intermedia: a multicenter study. Blood 97(11):3411–3416
Bessems JG, Vermeulen NP (2001) Paracetamol (acetaminophen)-induced toxicity: molecular and biochemical mechanisms, analogues and protective approaches. Crit Rev Toxicol 31(1):55–138
Manyike PT, Kharasch ED, Kalhorn TF et al (2000) Contribution of CYP2E1 and CYP3A to acetaminophen reactive metabolite formation. Clin Pharmacol Ther 67:275–282
Lau GS, Critchley JAJ (1994) The estimation of paracetamol and its major metabolites in both plasma and urine by a single high-performance liquid chromatography assay. J Pharm Biomed Anal 12(12):1563–1572
Chutamanee CS, Woranuch T, Jongjit A, Julian JAJH (1994) Metabolic profile of paracetamol in healthy Thais. Intern Med 10:72–76
Rifkind AB, Canale V, New MI (1976) Antipyrine clearance in homozygous beta-thalassemia. Clin Pharmacol Ther 20(4):476–483
Bosi G, Crepaz R, Gamberini MR, Fortini M, Scarcia S, Bonsante E, Pitscheider W, Vaccari M (2003) Left ventricular remodelling, and systolic and diastolic function in young adults with beta thalassaemia major: a Doppler echocardiographic assessment and correlation with haematological data. Heart 89(7):762–766
Sitar DS (2004) Pharmacokinetic and other factors influencing drug action. In: Page C, Curtis M, Sutter M, Hoffman B (eds) Integrated pharmacology, 2nd edn. Elsevier, Philadelphia, pp 39–54
Milligan TP, Morris HC, Hammond PM et al (1994) Studies on paracetamol binding to serum proteins. Ann Clin Biochem 31:492–496
Mastrangelo F, Lopez T, Rizzelli S, Manisco G, Corliano C, Alfonso L (1975) Function of the kidney in adult patients with Cooley’s disease. A preliminary report. Nephron 14(3–4):229–236
Al-Obaidy SS, McKiernan PJ, Li Wan Po A, Glasgow JF, Collier PS (1996) Metabolism of paracetamol in children with chronic liver disease. Eur J Clin Pharmacol 50(1–2):69–76
Debinski HS, Mackenzie PI, Lee CS, Mashford ML, Danks JA, Tephly TR et al (1996) UDP glucuronosyltransferase in the cirrhotic rat liver. J Gastroenterol Hepatol 11(4):373–379
Li YQ, Prentice DA, Howard ML, Mashford ML, Desmond PV (2000) Bilirubin and bile acids may modulate their own metabolism via regulating uridine diphosphate-glucuronosyltransferase expression in the rat. J Gastroenterol Hepatol 15(8):865–870
Tukey RH, Strassburg CP (2000) Human UDP-glucuronosyltransferases: metabolism, expression, and disease. Ann Rev Pharmacol Toxicol 40:581–616
Bridger S, Henderson K, Glucksman E, Ellis AJ, Henry JA, Williams R (1998) Deaths from low dose paracetamol poisoning. BMJ 316:1724–1725
de Morais SM, Uetrecht JP, Wells PG (1992) Decreased glucuronidation and increased bioactivation of acetaminophen in Gilbert’s syndrome. Gastroenterology 102(2):577–586
Ciotti M, Marrone A, Potter C, Owens IS (1997) Genetic polymorphism in the human UGT1A6 (planar phenol) UDP-glucuronosyltransferase: pharmacological implications. Pharmacogenetics 7(6):485–495
Krishnaswam S, Hao Q, Al-Rohaimi A, Hesse LM, von Moltke LL, Greenblatt DJ, Court MH (2005) UDP glucuronosyltransferase (UGT) 1A6 pharmacogenetics: II. Functional impact of the three most common nonsynonymous UGT1A6 polymorphisms (S7A, T181A, and R184S). J Pharmacol Exp Ther 313(3):1340–1346
Acknowledgements
This work was supported by Thailand Research Fund and National Center for Genetic Engineering and Biotechnology. Jeeranut Tankanitlert was a recipient of the scholarship from the Ministry of University Affairs. Prof. Suthat Fucharoen is a senior scholar of Thailand Research Fund. The authors thank Dr. T.W. Flegel for carefully checking the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tankanitlert, J., Howard, T.A., Temsakulphong, A. et al. A pharmacokinetic study of paracetamol in Thai β-thalassemia/HbE patients. Eur J Clin Pharmacol 62, 743–748 (2006). https://doi.org/10.1007/s00228-006-0167-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-006-0167-2