Abstract
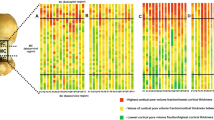
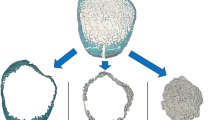
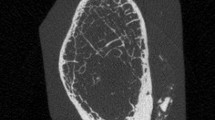
We analyzed the bone microarchitecture of the subcapital and basicervical subregions of the femoral neck in men, to determine whether microarchitectural differences of cortical or trabecular bone can explain differential frequency of subcapital vs. basicervical fractures, especially in aged persons. The study sample encompassed twenty male proximal femora obtained during autopsy. They were divided in two age groups: young (< 40 years, n = 10) and aged (> 60 years, n = 10). Micro-computed tomography was used to evaluate cortical and trabecular microarchitecture of the subcapital and basicervical regions of the superolateral femoral neck–typical fracture initiation site. Basicervical region showed significantly thicker and less porous cortex than subcapital region (p = 0.02, p < 0.001, respectively), along with increased distance between cortical pores (p = 0.004) and smaller pore diameters (p = 0.069). Higher trabecular number (Tb.N: p = 0.042), lower trabecular thickness (Tb.Th: p < 0.001), and lower trabecular separation (p = 0.003) were also hallmarks of the basicervical compared to subcapital region, although BV/TV was similar in both regions (p = 0.133). Age-related deterioration was mostly visible in trabecular bone (for BV/TV, Tb.Th, Tb.N and fractal dimension: p = 0.026, p = 0.049, p = 0.059, p = 0.009, respectively). Moreover, there were tendencies to age-specific patterns of trabecular separation (more pronounced inter-site differences in aged) and cortical thickness (more pronounced inter-site differences in young). Trabecular microarchitecture corresponded to cortical characteristics of each region. Our study revealed the microarchitectural basis for higher incidence of subcapital than basicervical fractures of the femoral neck. This is essential for better understanding of the fracture risk, as well as for future strategies to prevent hip fractures and their complications.




Similar content being viewed by others
Data Availability
The data that support the findings of this study are available from the corresponding author [P.M] upon reasonable request.
References
Alswat KA (2017) Gender disparities in osteoporosis. J Clin Med Res 9(5):382–387
Wright CN, Saag GK, Curtis RJ, Smith KW, Kilgore LM, Morrisey AM, Yun H, Zhang J, Delzell SE (2012) Recent trends in hip fracture rates by race/ethnicity among older US adults. J Bone Miner Res 27(11):2325–2332
Svedbom A, Hernlund E, Ivergård M, Compston J, Cooper C, Stenmark J, McCloskey VE, Jönsson B, Kanis AJ (2013) Osteoporosis in the European Union: a compendium of country-specific reports. Arch Osteoporos 8(1–2):137
Panula J, Pihlajamäki H, Mattila VM, Jaatinen P, Vahlberg T, Aarnio P, Kivelä SL (2011) Mortality and cause of death in hip fracture patients aged 65 or older-a population-based study. BMC Musculoskel Dis 20(12):105
Tanner DA, Kloseck M, Crilly RG, Chesworth B, Gilliland J (2010) Hip fracture types in men and women change differently with age. BMC Geriatr 10:12
Warriner AH, Patkar NM, Curtis JR, Delzell E, Gary L, Kilgore M, Saag K (2011) Which fractures are most attributable to osteoporosis? J Clin Epidemiol 64(1):46–53
Vogt MT, Cauley JA, Tomaino MM, Stone K, Williams JR, Herndon JH (2002) Distal radius fractures in older women: a 10-year follow-up study of descriptive characteristics and risk factors. The study of osteoporotic fractures. J Am Geriatr Soc 50(1):97–103
Saarenpää I, Partanen J, Jalovaara P (2003) Basicervical fracture–a rare type of hip fracture. Arch Orthop Trauma Surg 122(2):69–72
Chen CY, Chiu FY, Chen CM, Huang CK, Chen WM, Chen TH (2008) Surgical treatment of basicervical fractures of femur—a prospective evaluation of 269 patients. J Trauma 64(2):427–429
Dedrick DK, Mackenzie JR, Burney RE (1986) Complications of femoral neck fracture in young adults. J Trauma 26(10):932–937
Mayhew PM, Thomas CD, Clement JG, Loveridge N, Beck TJ, Bonfield W, Burgoyne CJ, Reeve J (2005) Relation between age, femoral neck cortical stability, and hip fracture risk. Lancet 366(9480):129–135
Jo S, Lee SH, Lee HJ (2016) The correlation between the fracture types and the complications after internal fixation of the femoral neck fractures. Hip Pelvis 28(1):35–42
Magu NK, Magu S, Rohilla RK, Batra A, Jaipuria A, Singh A (2014) Computed tomographic evaluation of the proximal femur: a predictive classification in displaced femoral neck fracture management. Indian J Orthop 48(5):476–483
de Bakker PM, Manske SL, Ebacher V, Oxland TR, Cripton PA, Guy P (2009) During sideways falls proximal femur fractures initiate in the superolateral cortex: evidence from high-speed video of simulated fractures. J Biomech 42(12):1917–1925
Kazley JM, Banerjee S, Abousayed MM, Rosenbaum AJ (2018) Classifications in brief: garden classification of femoral neck fractures. Clin Orthop Relat Res 476(2):441–445
Djuric M, Djonic D, Milovanovic P, Nikolic S, Marshall R, Marinkovic J, Hahn M (2010) Region-specific sex-dependent pattern of age-related changes of proximal femoral cancellous bone and its implications on differential bone fragility. Calcif Tissue Int 86(3):192–201
Chen H, Zhou X, Shoumura S, Emura S, Bunai Y (2010) Age-and gender-dependent changes in three-dimensional microstructure of cortical and trabecular bone at the human femoral neck. Osteoporos Int 21(4):627–636
Lochmüller EM, Matsuura M, Bauer J, Hitzl W, Link TM, Müller R, Eckstein F (2008) Site-specific deterioration of trabecular bone architecture in men and women with advancing age. J Bone Miner Res 23(12):1964–1973
Johannesdottir F, Poole KE, Reeve J, Siggeirsdottir K, Aspelund T, Mogensen B, Jonsson BY, Sigurdsson S, Harris TB, Gudnason VG, Sigurdsson G (2011) Distribution of cortical bone in the femoral neck and hip fracture: a prospective case-control analysis of 143 incident hip fractures; the AGES-REYKJAVIK Study. Bone 48(6):1268–1276
Cui WQ, Won YY, Baek MH, Lee DH, Chung YS, Hur JH, Ma YZ (2008) Age-and region-dependent changes in three-dimensional microstructural properties of proximal femoral trabeculae. Osteoporos Int 19(11):1579–1587
Ciarelli TE, Fyhrie DP, Schaffler MB, Goldstein SA (2000) Variations in three-dimensional cancellous bone architecture of the proximal femur in female hip fractures and in controls. J Bone Miner Res 15(1):32–40
Guo XE, Kim CH (2002) Mechanical consequence of trabecular bone loss and its treatment: a three-dimensional model simulation. Bone 30(2):404–411
Kral R, Osima M, Borgen TT, Vestgaard R, Richardsen E, Bjørnerem Å (2017) Increased cortical porosity and reduced cortical thickness of the proximal femur are associated with nonvertebral fracture independent of fracture risk assessment tool and Garvan estimates in postmenopausal women. PLoS ONE 12(9):e0185363
Zebaze R, Seeman E (2015) Cortical bone: a challenging geography. J Bone Miner Res 30(1):24–29
Sundh D, Mellström D, Nilsson M, Karlsson M, Ohlsson C, Lorentzon M (2015) Increased cortical porosity in older men with fracture. J Bone Miner Res 30(9):1692–1700
Sundh D, Nilsson AG, Nilsson M, Johansson L, Mellström D, Lorentzon M (2017) Increased cortical porosity in women with hip fracture. J Intern Med 281(5):496–506
Rolvien T, Vom Scheidt A, Stockhausen KE, Milovanovic P, Djonic D, Hubert J et al (2018) Inter-site variability of the osteocyte lacunar network in the cortical bone underpins fracture susceptibility of the superolateral femoral neck. Bone 112:187–193
Verhulp E, van Rietbergen B, Huiskes R (2008) Load distribution in the healthy and osteoporotic human proximal femur during a fall to the side. Bone 42(1):30–35
Holzer G, von Skrbensky G, Holzer LA, Pichl W (2009) Hip fractures and the contribution of cortical versus trabecular bone to femoral neck strength. J Bone Miner Res 24(3):468–474
Manske SL, Liu-Ambrose T, Cooper DM, Kontulainen S, Guy P, Forster BB et al (2009) Cortical and trabecular bone in the femoral neck both contribute to proximal femur failure load prediction. Osteoporos Int 20(3):445–453
Johannesdottir F, Thrall E, Muller J, Keaveny TM, Kopperdahl DL, Bouxsein ML (2017) Comparison of non-invasive assessments of strength of the proximal femur. Bone 105:93–102
Power J, Loveridge N, Kröger H, Parker M, Reeve J (2018) Femoral neck cortical bone in female and male hip fracture cases: differential contrasts in cortical width and sub-periosteal porosity in 112 cases and controls. Bone 114:81–89
Bell KL, Loveridge N, Power J, Garrahan N, Meggitt BF, Reeve J (1999) Regional differences in cortical porosity in the fractured femoral neck. Bone 24:57–64
Milovanovic P, Djonic D, Marshall RP, Hahn M, Nikolic S, Zivkovic V et al (2012) Micro-structural basis for particular vulnerability of the superolateral neck trabecular bone in the postmenopausal women with hip fractures. Bone 50(1):63–68
Funding
The authors thank the Science Fund of the Republic of Serbia for support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Aleksandar Cirovic, Ana Cirovic, Danijela Djonic, Vladimir Zivkovic, Slobodan Nikolic, Marija Djuric, and Petar Milovanovic declare that they have no conflict of interest.
Ethics Approval
All procedures performed were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The collection of the cadaveric bone specimens was approved by the Ethics Committee of the Faculty of Medicine, University of Belgrade.
Informed Consent
For this type of study consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Cirovic, A., Cirovic, A., Djonic, D. et al. Three-Dimensional Microstructural Basis for Differential Occurrence of Subcapital versus Basicervical Hip Fractures in Men. Calcif Tissue Int 107, 240–248 (2020). https://doi.org/10.1007/s00223-020-00717-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00223-020-00717-z