Abstract
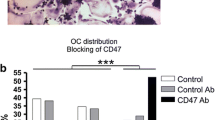
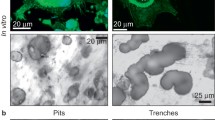
Fusion is the final osteoclast differentiation step leading to bone resorption. In healthy trabecular bone, osteoclast fusion is restricted to bone surfaces undergoing resorption, and necessarily requires site-specific recruitment of mononucleated pre-osteoclasts originating from the bone marrow. However, the spatiotemporal mechanism coordinating recruitment and fusion is poorly investigated. Herein we identify a collagen/vascular network as a likely structure supporting this mechanism. We therefore used multiplex immunohistochemistry and electron microscopy on human iliac crest bone samples, in combination with functional assays performed in vitro with osteoclasts generated from healthy blood donors. First, we found that putative pre-osteoclasts are in close vicinity of a network of collagen fibers associated with vessels and bone remodeling compartment canopies. Based on 3D-reconstructions of serial sections, we propose that this network may serve as roads leading pre-osteoclasts to resorption sites, as reported for cell migration in other tissues. Importantly, almost all these bone marrow pre-osteoclasts, but only some osteoclasts, express the collagen receptor OSCAR, which is reported to induce fusion competence. Furthermore, differentiating osteoclasts cultured on collagen compared to mineral show higher fusion rates, higher expression of fusogenic cytokines, and a CD47 plasma membrane distribution pattern reported to be typical of a pre-fusion state—thus collectively supporting collagen-induced fusion competence. Finally, these in vitro assays show that collagen induces high cell mobility. The present data lead to a model where collagen fibers/vasculature support the coordination between traffic and fusion of pre-osteoclasts, by serving as a physical road and inducing fusion competence as well as cell mobility.








Similar content being viewed by others
References
Boyce BF (2013) Advances in the regulation of osteoclasts and osteoclast functions. J Dent Res 92:860–867. https://doi.org/10.1177/0022034513500306
Jaworski ZF, Duck B, Sekaly G (1981) Kinetics of osteoclasts and their nuclei in evolving secondary Haversian systems. J Anat 133:397–405
Marks SC, Seifert MF (1985) The lifespan of osteoclasts: experimental studies using the giant granule cytoplasmic marker characteristic of beige mice. Bone 6:451–455. https://doi.org/10.1016/8756-3282(85)90223-6
Jacome-Galarza CE, Percin GI, Muller JT et al (2019) Developmental origin, functional maintenance and genetic rescue of osteoclasts. Nature 568:541–545. https://doi.org/10.1038/s41586-019-1105-7
Xing L, Xiu Y, Boyce BF (2012) Osteoclast fusion and regulation by RANKL-dependent and independent factors. World J Orthop 3:212–222
Ishii M, Egen JG, Klauschen F et al (2009) Sphingosine-1-phosphate mobilizes osteoclast precursors and regulates bone homeostasis. Nature 458:524–528. https://doi.org/10.1038/nature07713
Søe K, Hobolt-Pedersen A-S, Delaisse J-M (2015) The elementary fusion modalities of osteoclasts. Bone 73:181–189. https://doi.org/10.1016/j.bone.2014.12.010
Hobolt-Pedersen AS, Delaissé JM, Søe K (2014) Osteoclast fusion is based on heterogeneity between fusion partners. Calcif Tissue Int 95:73–82. https://doi.org/10.1007/s00223-014-9864-5
Levaot N, Ottolenghi A, Mann M et al (2015) Osteoclast fusion is initiated by a small subset of RANKL-stimulated monocyte progenitors, which can fuse to RANKL-unstimulated progenitors. Bone 79:21–28
Mensah KA, Ritchlin CT, Schwarz EM (2010) RANKL induces heterogeneous DC-STAMPlo and DC-STAMPhi osteoclast precursors of which the DC-STAMPlo precursors are the master fusogens. J Cell Physiol 223:76–83. https://doi.org/10.1002/jcp.22012
Møller AMJ, Delaisse J-M, Søe K (2017) Osteoclast fusion: time-lapse reveals involvement of cd47 and syncytin-1 at different stages of nuclearity. J Cell Physiol 232:1396–1403. https://doi.org/10.1002/jcp.25633
Baron R, Neff L, Tran VP et al (1986) Kinetic and cytochemical identification of osteoclast precursors and their differentiation into multinucleated osteoclasts. Am J Pathol 122:363–378
Mizoguchi T, Muto A, Udagawa N et al (2009) Identification of cell cycle-arrested quiescent osteoclast precursors in vivo. J Cell Biol 184:541–554
Gritsenko PG, Ilina O, Friedl P (2012) Interstitial guidance of cancer invasion. J Pathol 226:185–199. https://doi.org/10.1002/path.3031
Bajénoff M, Egen JG, Koo LY et al (2006) Stromal cell networks regulate lymphocyte entry, migration, and territoriality in lymph nodes. Immunity 25:989–1001. https://doi.org/10.1016/j.immuni.2006.10.011
Sobocinski GP, Toy K, Bobrowski WF et al (2010) Ultrastructural localization of extracellular matrix proteins of the lymph node cortex: Evidence supporting the reticular network as a pathway for lymphocyte migration. BMC Immunol 11:42. https://doi.org/10.1186/1471-2172-11-42
Friedl P, Bröcker E (2000) T cell migration in three-dimensional extracellular matrix: guidance by polarity and sensations. Dev Immunol 7:249–266
Kuter DJ, Bain B, Mufti G et al (2007) Bone marrow fibrosis: pathophysiology and clinical significance of increased bone marrow stromal fibres. Br J Haematol 139:351–362
Bentley S, Alabaster O, Foidart J (1981) Collagen heterogeneity in normal human bone marrow. Br J Haematol 48:287–291
Andersen TL, Sondergaard TE, Skorzynska KE et al (2009) A physical mechanism for coupling bone resorption and formation in adult human bone. Am J Pathol 174:239–247
Kristensen HB, Andersen TL, Marcussen N et al (2013) Increased presence of capillaries next to remodeling sites in adult human cancellous bone. J Bone Miner Res 28:574–585. https://doi.org/10.1002/jbmr.1760
Kristensen HB, Andersen TL, Marcussen N et al (2014) Osteoblast recruitment routes in human cancellous bone remodeling. Am J Pathol 184:778–789
Gordon H, Sweets HH (1936) A simple method for the silver impregnation of reticulum. Am J Pathol 12(545–552):1
Søe K, Delaisse J-M (2010) Glucocorticoids maintain human osteoclasts in the active mode of their resorption cycle. J Bone Miner Res 25:2184–2192. https://doi.org/10.1002/jbmr.113
Søe K, Merrild DMH, Delaissé J-M (2013) Steering the osteoclast through the demineralization-collagenolysis balance. Bone 56:191–198. https://doi.org/10.1016/j.bone.2013.06.007
Ridley A, Schhwartz M, Burridge K et al (2003) Cell migration : Integrating signals from front to back. Science 302:1704–1710. https://doi.org/10.1126/science.1092053
Søe K, Delaissé J-M (2017) Time-lapse reveals that osteoclasts can move across the bone surface while resorbing. J Cell Sci 130:2026–2035. https://doi.org/10.1242/jcs.202036
Janckila AJ, Slone SP, Lear SC et al (2007) Tartrate-resistant acid phosphatase as an immunohistochemical marker for inflammatory macrophages. Am J Clin Pathol 127:556–566. https://doi.org/10.1309/DGEA9BE2VE5VCFYH
Ushiki T (2002) Collagen fibers, reticular fibers and elastic fibers. A comprehensive understanding from a morphological viewpoint. Arch Histol Cytol 65:109–126
Nakamura I, Tanaka H, Rodan GA, Duong LT (1998) Echistatin inhibits the migration of murine prefusion osteoclasts and the formation of multinucleated osteoclast-like cells 1. Endocrinology 139:5182–5193
Nakamura I, Pilkington MF, Lakkakorpi PT et al (1999) Role of alpha(v)beta(3) integrin in osteoclast migration and formation of the sealing zone. J Cell Sci 112(Pt 2):3985–3993
Lundberg P, Koskinen C, Baldock PA et al (2007) Osteoclast formation is strongly reduced both in vivo and in vitro in the absence of CD47/SIRPalpha-interaction. Biochem Biophys Res Commun 352:444–448
Bendre MS, Montague DC, Peery T et al (2003) Interleukin-8 stimulation of osteoclastogenesis and bone resorption is a mechanism for the increased osteolysis of metastatic bone disease. Bone 33:28–37
Kopesky P, Tiedemann K, Alkekhia D et al (2014) Autocrine signaling is a key regulatory element during osteoclastogenesis. Biol Open 3:767–776
Yao Z, Xing L, Qin C et al (2008) Osteoclast precursor interaction with bone matrix induces osteoclast formation directly by an interleukin-1-mediated autocrine mechanism. J Biol Chem 283:9917–9924
Hotokezaka H, Sakai E, Ohara N et al (2007) Molecular analysis of RANKL-independent cell fusion of osteoclast-like cells induced by TNF-α, lipopolysaccharide, or peptidoglycan. J Cell Biochem 101:122–134. https://doi.org/10.1002/jcb.21167
Barrow AD, Raynal N, Andersen TL et al (2011) OSCAR is a collagen receptor that costimulates osteoclastogenesis in DAP12-deficient humans and mice. J Clin Invest 121:3505–3516
Tezuka K, Tezuka Y, Maejima A et al (1994) Molecular cloning of a possible cysteine proteinase predominantly expressed in osteoclasts. J Biol Chem 269:1106–1109
Wolf K, Alexander S, Schacht V et al (2009) Collagen-based cell migration models in vitro and in vivo. Semin Cell Dev Biol 20:931–941. https://doi.org/10.1016/j.semcdb.2009.08.005
Takahashi N, Ejiri S, Yanagisawa S, Ozawa H (2007) Regulation of osteoclast polarization. Odontology 95:1–9
Saltel F, Destaing O, Bard F et al (2004) Apatite-mediated actin dynamics in resorbing osteoclasts. Mol Biol Cell 15:5231–5241
Helming L, Tomasello E, Kyriakides TR et al (2008) Essential role of DAP12 signaling in macrophage programming into a fusion-competent state. Sci Signal 1:ra11
Humphrey MB, Daws MR, Spusta SC et al (2006) TREM2, a DAP12-associated receptor, regulates osteoclast differentiation and function. J Bone Miner Res 21:237–245. https://doi.org/10.1359/JBMR.051016
Tani-Ishii N, Tsunoda A, Teranaka T, Umemoto T (1999) Autocrine regulation of osteoclast formation and bone resorption by IL-la and TNFa. J Dent Res 78:1617–1623. https://doi.org/10.1177/00220345990780100601
Yu X, Huang Y, Collin-osdoby P, Osdoby P (2003) Stromal cell-derived factor-1 (SDF-1) recruits osteoclast precursors by inducing chemotaxis, matrix metalloproteinase-9 (MMP-9) activity, and collagen transmigration. J Bone Miner Res 18:1404–1418
Henriksen K, Karsdal M, Delaissé JM, Engsig MT (2003) RANKL and vascular endothelial growth factor (VEGF) induce osteoclast chemotaxis through an ERK1/2-dependent mechanism. J Biol Chem 278:48745–48753. https://doi.org/10.1074/jbc.M309193200
Fuller K, Owens JM, Chambers TJ (1995) Macrophage inflammatory protein-1 alpha and IL-8 stimulate the motility but suppress the resorption of isolated rat osteoclasts. J Immunol 154:6065–6072
Pereira M, Petretto E, Gordon S et al (2018) Common signalling pathways in macrophage and osteoclast multinucleation. J Cell Sci. https://doi.org/10.1242/jcs.216267
Acknowledgements
We wish to thank Jacob Bastholm Olesen, Birgit MacDonald, Kaja Søndergaard Laursen, Karin Trampedach, and Vibeke Nielsen for their excellent technical assistance. This study was financed through general funding by Lillebaelt Hospital, Aarhus University Hospital, and Odense University Hospital.
Author information
Authors and Affiliations
Contributions
Designing research study: KS, TLA, and JMD; conducting experiments: KS and TLA; acquiring data: KS, TLA, MH, LR, and NM; analyzing data: KS, TLA, and JMD; writing the manuscript: KS, TLA, and JMD; editing and correcting the manuscript: KS, TLA, MH, LR, NM, and JMD; final approval of manuscript: KS, TLA, MH, LR, NM, and JMD.
Corresponding authors
Ethics declarations
Conflict of interest
Kent Søe, Thomas Levin Andersen, Maja Hinge, Lars Rolighed, Niels Marcussen, and Jean-Marie Delaisse declare that they have no conflict of interests.
Human and Animal Rights and Informed Consent
All procedurse performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (The Scientific Eithical Committee for the Region of Southern Denmark S-20070121 and S20070019) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Søe, K., Andersen, T.L., Hinge, M. et al. Coordination of Fusion and Trafficking of Pre-osteoclasts at the Marrow–Bone Interface. Calcif Tissue Int 105, 430–445 (2019). https://doi.org/10.1007/s00223-019-00575-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00223-019-00575-4