Abstract
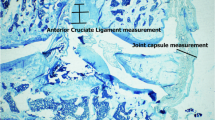
To show the effects of tranexamic acid, which is a drug frequently used to control bleeding, on the hip joint and sciatic nerve in animal experiments. There were 15 rats in each of the 3 groups, with a total of 45 rats. Topical saline injections were applied to the first group, topical TXA injections to the second group, and intravenous (IV) TXA injections to the third group. In the samples taken from the hip joint 3 weeks later, femoral head cartilage, sciatic nerve, and joint capsule thicknesses were analyzed histologically. Statistically significantly more cartilage degradation was detected in the femoral head cartilage in both the IV and intraarticular TXA group when compared to the control group. The groups were also compared in terms of acetabular cartilage; however, no histological difference was found between the groups. It was seen that when the femoral head cartilage thickness (the average of the measurements made from 3 different points were used) was examined, the cartilage thickness in the topical TXA group was less when compared to the other 2 groups. However, this difference was determined to not be statistically significant. The data of the hip joint capsule thickness measurement, it was found that the capsule thickness in the topical TXA applied group was less when compared to the other 2 groups. However, this difference was not statistically significant. When the sciatic nerves in all 3 groups were compared, no different staining characteristics were found in the immunofluorescence examination. TXA, which is frequently used in orthopedic practice, shows negative effects on hip joint cartilage in both topical and intravenous application.





Similar content being viewed by others
Data availability
Not applicable.
References
Adak BM, Laçin N, Şimşek F et al (2022) Evaluation of the effects of different hemostatic agent applications on mental nerve. Eur Arch Otorhinolaryngol. https://doi.org/10.1007/S00405-022-07434-3
Aguilera-Roig X, Jordán-Sales M, Natera-Cisneros L et al (2014) Tranexamic acid in orthopedic surgery. Rev Esp Cir Ortop Traumatol 58:52–56. https://doi.org/10.1016/J.RECOT.2013.08.005
Akcan G, Alimogullari E, Abu-Issa R, Cayli S (2020) Analysis of the developmental expression of small VCP-interacting protein and its interaction with steroidogenic acute regulatory protein in Leydig cells. Reprod Biol 20:88–96. https://doi.org/10.1016/J.REPBIO.2020.01.006
Alshryda S, Sukeik M, Sarda P et al (2014) A systematic review and meta-analysis of the topical administration of tranexamic acid in total hip and knee replacement. Bone Joint J 96-B:1005–1015. https://doi.org/10.1302/0301-620X.96B8.33745
Ambra LF, de Girolamo L, Niu W et al (2019) No effect of topical application of tranexamic acid on articular cartilage. Knee Surg Sports Traumatol Arthrosc 27:931–935. https://doi.org/10.1007/S00167-017-4746-9
Belk JW, McCarty EC, Houck DA et al (2021) Tranexamic acid use in knee and shoulder arthroscopy leads to improved outcomes and fewer hemarthrosis-related complications: a systematic review of level I and II studies. Arthros J Arthros Relat Surg 37:1323–1333. https://doi.org/10.1016/J.ARTHRO.2020.11.051
Bi̇ri̇si̇k F, Bayram S, Çakmak M et al (2021) Investigation of the effects of intra-articular tranexamic acid on intact cartilage tissue and cartilage formation in osteochondral defects of the rabbit knee: an experimental study. Cureus 13.https://doi.org/10.7759/CUREUS.14873
Bolam SM, O’Regan-Brown A, Konar S et al (2022) Cytotoxicity of tranexamic acid to tendon and bone in vitro: Is there a safe dosage? J Orthop Surg Res 17. https://doi.org/10.1186/S13018-022-03167-5
Bolam SM, O’Regan-Brown A, Paul Monk A et al (2021) Toxicity of tranexamic acid (TXA) to intra-articular tissue in orthopaedic surgery: a scoping review. Knee Surg Sports Traumatol Arthrosc 29:1862–1871. https://doi.org/10.1007/S00167-020-06219-7
Br L, Bd H, Mn B, ZH G, (2014) Weighted versus uniform dose of tranexamic acid in patients undergoing primary, elective knee arthroplasty: a prospective randomized controlled trial. J Arthroplasty 29:186–188. https://doi.org/10.1016/J.ARTH.2014.01.038
Brouwer AJ, Kempink DRJ, de Witte PB (2021) Tranexamic acid reduces blood loss in paediatric proximal femoral and/or pelvic osteotomies. J Child Orthop 15:241–247. https://doi.org/10.1302/1863-2548.15.200249
Buckwalter JA, Lane NE (1997) Athletics and osteoarthritis. Am J Sports Med 25:873–881. https://doi.org/10.1177/036354659702500624
Dereli Can G, Akcan G, Can ME et al (2020) Surgical and immunohistochemical outcomes of scleral reconstruction with autogenic, allogenic and xenogenic grafts: an experimental rabbit model. Curr Eye Res 45:1572–1582. https://doi.org/10.1080/02713683.2020.1764976
Ekici M, Balkaya M (2021) Protective effects of oxytocin and progesterone on paclitaxel-induced neuropathy in rats. Neurol Sci Neurophysiol 38:262. https://doi.org/10.4103/NSN.NSN_113_21
Farah H, Wijesinghe SN, Nicholson T et al (2022) Differential metabotypes in synovial fibroblasts and synovial fluid in hip osteoarthritis patients support inflammatory responses. Int J Mol Sci 23. https://doi.org/10.3390/IJMS23063266
Goderecci R, Giusti I, Necozione S et al (2019) Short exposure to tranexamic acid does not affect, in vitro, the viability of human chondrocytes. Eur J Med Res 24. https://doi.org/10.1186/S40001-019-0373-X
Jones SW, Brockbank SMV, Mobbs ML et al (2006) The orphan G-protein coupled receptor RDC1: evidence for a role in chondrocyte hypertrophy and articular cartilage matrix turnover. Osteoarthr Cartil 14:597–608. https://doi.org/10.1016/J.JOCA.2006.01.007
Kanno K, Narita M, Kawarai Y et al (2022) Analgesic effects and arthritic changes following tramadol administration in a rat hip osteoarthritis model. J Orthop Res 40. https://doi.org/10.1002/JOR.25208
Konig G, Hamlin BR, Waters JH (2013) Topical tranexamic acid reduces blood loss and transfusion rates in total hip and total knee arthroplasty. J Arthroplasty 28:1473–1476. https://doi.org/10.1016/J.ARTH.2013.06.011
Li N, Qin LW, Jiang HJ (2021) Clinical effects of tranexamic acid in arthroscope for femoroacetabular impingement. Zhongguo Gu Shang 34:121–125. https://doi.org/10.12200/J.ISSN.1003-0034.2021.02.005
Lins LAB, Miller PE, Samineni A et al (2020) The use of tranexamic acid (TXA) in neuromuscular hip reconstruction: can we alter the need for blood transfusion? J Pediatr Orthop 40:e766–e771. https://doi.org/10.1097/BPO.0000000000001534
Loeser RF, Goldring SR, Scanzello CR, Goldring MB (2012) Osteoarthritis: a disease of the joint as an organ. Arthritis Rheum 64:1697. https://doi.org/10.1002/ART.34453
Loeuille D, Chary-Valckenaere I, Champigneulle J et al (2005) Macroscopic and microscopic features of synovial membrane inflammation in the osteoarthritic knee correlating magnetic resonance imaging findings with disease severity. Arthritis Rheum 52:3492–3501. https://doi.org/10.1002/art.21373
McLean M, McCall K, Smith IDM et al (2019) Tranexamic acid toxicity in human periarticular tissues. Bone Joint Res 8:11. https://doi.org/10.1302/2046-3758.81.BJR-2018-0181.R1
Miangul S, Oluwaremi T, El Haddad J et al (2023) Update on the efficacy and safety of intravenous tranexamic acid in hip fracture surgery: a systematic review and meta-analysis. Eur J Orthop Surg Traumatol 33:2179–2190. https://doi.org/10.1007/S00590-022-03387-9
Morrison RJM, Tsang B, Fishley W et al (2017) Dose optimisation of intravenous tranexamic acid for elective hip and knee arthroplasty: the effectiveness of a single pre-operative dose. Bone Joint Res 6:499–505. https://doi.org/10.1302/2046-3758.68.BJR-2017-0005.R1
Myers CA, Register BC, Lertwanich P et al (2011) Role of the acetabular labrum and the iliofemoral ligament in hip stability: an in vitro biplane fluoroscopy study. Am J Sports Med 39(Suppl):85S-91S. https://doi.org/10.1177/0363546511412161
Ng W, Jerath A, Wasowicz M (2015) Tranexamic acid: a clinical review. Anaesthesiol Intensive Ther 47:339–350. https://doi.org/10.5603/AIT.A2015.0011
Nilsson IM (1980) Clinical pharmacology of aminocaproic and tranexamic acids. J Clin Pathol Suppl (r Coll Pathol) 14:41. https://doi.org/10.1136/jcp.33.Suppl-14.41
O’Neill DC, Mortensen AJ, Cannamela PC, Aoki SK (2020) Clinical and radiographic presentation of capsular iatrogenic hip instability after previous hip arthroscopy. Am J Sports Med 48:2927–2932. https://doi.org/10.1177/0363546520949821
Parker JD, Lim KS, Kieser DC et al (2018) Is tranexamic acid toxic to articular cartilage when administered topically? What is the safe dose? Bone Joint J 100-B:404–412. https://doi.org/10.1302/0301-620X.100B3.BJJ-2017-1135.R1
Pimenta FS, de Oliveira Campos TV, de Abreu e Silva GM, et al (2023) Chondrotoxic effects of tranexamic acid and povidone-iodine on the articular cartilage of rabbits. Int Orthop. https://doi.org/10.1007/S00264-023-05820-Y
Salmon JH, Rat AC, Sellam J et al (2016) Economic impact of lower-limb osteoarthritis worldwide: a systematic review of cost-of-illness studies. Osteoarthr Cartil 24:1500–1508. https://doi.org/10.1016/J.JOCA.2016.03.012
Schwarzkopf R, Dang P, Luu M et al (2015) Topical tranexamic acid does not affect electrophysiologic or neurovascular sciatic nerve markers in an animal model. Clin Orthop Relat Res 473:1074. https://doi.org/10.1007/S11999-014-4098-4
Shang J, Z, Zhang, D, Luo et al (2020) Effectiveness of multi-modal blood management in bernese periacetabular osteotomy and periacetabular osteotomy with proximal femoral osteotomy. Orthop Surg 12:1748–1752. https://doi.org/10.1111/OS.12794
Song J, Wu J, Poulet B et al (2021) Proteomics analysis of hip articular cartilage identifies differentially expressed proteins associated with osteonecrosis of the femoral head. Osteoarthritis Cartilage 29:1081–1092. https://doi.org/10.1016/J.JOCA.2021.04.005
Sun X, Zhu X, Zeng Y et al (2020) The effect of posterior capsule repair in total hip arthroplasty: a systematic review and meta-analysis. BMC Musculoskelet Disord 21. https://doi.org/10.1186/S12891-020-03244-Y
Taljanovic MS, Graham AR, Benjamin JB et al (2008) Bone marrow edema pattern in advanced hip osteoarthritis: quantitative assessment with magnetic resonance imaging and correlation with clinical examination, radiographic findings, and histopathology. Skeletal Radiol 37:423–431. https://doi.org/10.1007/S00256-008-0446-3
Tuttle JR, Feltman PR, Ritterman SA, Ehrlich MG (2015) Effects of tranexamic acid cytotoxicity on in vitro chondrocytes. Am J Orthop (belle Mead NJ) 44:E497–E502
Vles GF, Corten K, Driesen R et al (2021) Hidden blood loss in direct anterior total hip arthroplasty: a prospective, double blind, randomized controlled trial on topical versus intravenous tranexamic acid. Musculoskelet Surg 105:267–273. https://doi.org/10.1007/S12306-020-00652-0
Wang S, Gao X, An Y (2017) Topical versus intravenous tranexamic acid in total knee arthroplasty: a meta-analysis of randomized controlled trials. Int Orthop 41:739–748. https://doi.org/10.1007/S00264-016-3296-Y
WHO model list of essential medicines - 22nd list, 2021.https://www.who.int/publications/i/item/WHO-MHP-HPS-EML-2021.02. Accessed 4 Aug 2022
Author information
Authors and Affiliations
Contributions
All of the authors contributed to the study’s conception and design. Material preparation, data collection, and analysis were performed by Serhat Akcaalan, Gulben Akcan, Ahmet Çevik Tufan, Ceyhun Caglar, Yasemin Akcaalan, Mustafa Akkaya, and Metin Dogan. The first draft of the manuscript was written by Serhat Akcaalan and all of the authors commented on previous versions of the manuscript. All of the authors read and approved the final manuscript. The authors declare that all data were generated in-house and that no paper mill was used.
Corresponding author
Ethics declarations
Ethics committee approval
Approval of the institutional review board of the current study was obtained from the Ankara Training and Research Hospital Animal Experiments Ethics Committee (Date: 20/01/2022, Number: 684).
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Akcaalan, S., Akcan, G., Tufan, A.C. et al. Is tranexamic acid safe for the hip joint?. Naunyn-Schmiedeberg's Arch Pharmacol 397, 1197–1207 (2024). https://doi.org/10.1007/s00210-023-02693-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-023-02693-1