Abstract
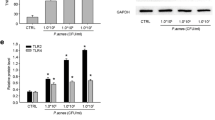
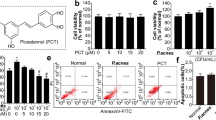
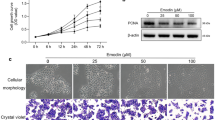
Viaminate, a retinoic acid derivative developed in China, has been clinically used for acne treatment to regulate and control keratinocyte cell differentiation and proliferation, inhibit keratinization, reduce sebum secretion, and regulate immune and anti-inflammatory functions; however, its potential molecular mechanism has not yet been elucidated. Therefore, we induced ear acne in rats using Propionibacterium acnes and sebum application. Symptoms of ear redness, epidermal thickening, inflammatory reaction, keratin overproduction, subcutaneous oil, and triglyceride (TG) accumulation improved significantly in acne model rats treated with viaminate for 30 days. Transcriptome analysis of rat skin tissues suggested that viaminate had significant regulatory effects on fatty acid metabolism and cellular keratinization pathways. Molecular target prediction suggested that toll-like receptor 2 (TLR2) may be a key target of viaminate’s therapeutic mechanism. Western blotting results confirmed that viaminate inhibited the TLR2 and its downstream pathways, nuclear factor-kappa B (NF-κB) [NF-κB inhibitor alpha (IκBα)/NF-κB-p65] and mitogen-activated protein kinases (MAPKs) [MAPK p38/c-Jun N-terminal kinase (JNK)/extracellular regulated kinase 1/2 (ERK1/2)] in acne vulgaris rats. In vitro studies revealed that viaminate treatment attenuated P. acnes proliferation and P. acnes-induced inflammatory response in human keratinocytes and has an inhibitory effect on the activation of NF-κB and MAPKs, while overexpression of TLR2 attenuated these effects. In conclusion, viaminate ameliorates P. acnes-induced acne by inhibiting the proliferation and inflammatory response of keratinocytes, ascribed to the deactivation of the TLR2-mediated NF-κB and MAPK pathways.








Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Balkrishna A, Nain P, Chauhan A, Sharma N, Gupta A, Ranjan R, Varshney A (2020) Super critical fluid extracted fatty acids from Withania somnifera seeds repair psoriasis-like skin lesions and attenuate pro-inflammatory cytokines (TNF-α and IL-6) release. Biomolecules 10(2). https://doi.org/10.3390/biom10020185
Cao L, Zheng F, Ma P, Liu W, Sun D, Chen X, ... Gou, M (2008) LC-APCI-MS-MS method for the tissue distribution of viaminate after oral administrations to rats. J Chromatogr Sci 46(8): 701-706. https://doi.org/10.1093/chromsci/46.8.701
Cursons J, Gao J, Hurley DG, Print CG, Dunbar PR, Jacobs MD, Crampin EJ (2015) Regulation of ERK-MAPK signaling in human epidermis. BMC Syst Biol 9:41. https://doi.org/10.1186/s12918-015-0187-6
El-Zayat SR, Sibaii H, Mannaa FA (2019) Toll-like receptors activation, signaling, and targeting: an overview. Bull Natl Res Cent 43(1):187. https://doi.org/10.1186/s42269-019-0227-2
Franz S, Ertel A, Engel KM, Simon JC, Saalbach A (2022) Overexpression of S100A9 in obesity impairs macrophage differentiation via TLR4-NFkB-signaling worsening inflammation and wound healing. Theranostics 12(4):1659–1682. https://doi.org/10.7150/thno.67174
Graham GM, Farrar MD, Cruse-Sawyer JE, Holland KT, Ingham E (2004) Proinflammatory cytokine production by human keratinocytes stimulated with Propionibacterium acnes and P. acnes GroEL. Br J Dermatol 150(3): 421–428. https://doi.org/10.1046/j.1365-2133.2004.05762.x
Grange PA, Raingeaud J, Calvez V, Dupin N (2009) Nicotinamide inhibits Propionibacterium acnes-induced IL-8 production in keratinocytes through the NF-kappaB and MAPK pathways. J Dermatol Sci 56(2):106–112. https://doi.org/10.1016/j.jdermsci.2009.08.001
Huang YC, Yang CH, Li TT, Zouboulis CC, Hsu HC (2015) Cell-free extracts of Propionibacterium acnes stimulate cytokine production through activation of p38 MAPK and toll-like receptor in SZ95 sebocytes. Life Sci 139:123–131. https://doi.org/10.1016/j.lfs.2015.07.028
Hwang DH, Lee DY, Koh PO, Yang HR, Kang C, Kim E (2020) Rosa davurica Pall. Improves Propionibacterium acnes-induced inflammatory responses in mouse ear edema model and suppresses pro-inflammatory chemokine production via MAPK and NF-κB pathways in HaCaT cells. Int J Mol Sci 21(5). https://doi.org/10.3390/ijms21051717
Jha P, Claudel T, Baghdasaryan A, Mueller M, Halilbasic E, Das SK, ... Trauner M (2014) Role of adipose triglyceride lipase (PNPLA2) in protection from hepatic inflammation in mouse models of steatohepatitis and endotoxemia. Hepatology 59(3): 858-869. https://doi.org/10.1002/hep.26732
Ji J, Zhu J, Hu X, Wang T, Zhang X, Hou AJ, Wang H (2015) (2S)-7,4′-dihydroxy-8-prenylflavan stimulates adipogenesis and glucose uptake through p38MAPK pathway in 3T3-L1 cells. Biochem Biophys Res Commun 460(3):578–582. https://doi.org/10.1016/j.bbrc.2015.03.072
Jonak C, Mildner M, Klosner G, Paulitschke V, Kunstfeld R, Pehamberger H, ... Trautinger F (2011) The hsp27kD heat shock protein and p38-MAPK signaling are required for regular epidermal differentiation. J Dermatol Sci 61(1): 32-37. https://doi.org/10.1016/j.jdermsci.2010.10.009
Jugeau S, Tenaud I, Knol AC, Jarrousse V, Quereux G, Khammari A, Dreno B (2005) Induction of toll-like receptors by Propionibacterium acnes. Br J Dermatol 153(6):1105–1113. https://doi.org/10.1111/j.1365-2133.2005.06933.x
Keeling MC, Gavara N (2020) Withaferin-A can be used to modulate the keratin network of intermediate filaments in human epidermal keratinocytes. Int J Mol Sci 21(12). https://doi.org/10.3390/ijms21124450
Kim J, Ochoa MT, Krutzik SR, Takeuchi O, Uematsu S, Legaspi AJ, ... Modlin RL (2002) Activation of toll-like receptor 2 in acne triggers inflammatory cytokine responses. J Immunol 169(3): 1535-1541. https://doi.org/10.4049/jimmunol.169.3.1535
Kim J, Shin YK, Kim KY (2018) Promotion of keratinocyte proliferation by tracheloside through ERK1/2 stimulation. Evid Based Complement Alternat Med 2018:4580627. https://doi.org/10.1155/2018/4580627
Kolar SL, Tsai CM, Torres J, Fan X, Li H, Liu GY (2019) Propionibacterium acnes-induced immunopathology correlates with health and disease association. JCI Insight 4(5). https://doi.org/10.1172/jci.insight.124687
Köllisch G, Kalali BN, Voelcker V, Wallich R, Behrendt H, Ring J ... Ollert M (2005) Various members of the toll-like receptor family contribute to the innate immune response of human epidermal keratinocytes. Immunology 114(4): 531-541. https://doi.org/10.1111/j.1365-2567.2005.02122.x
Kovács D, Fazekas F, Oláh A, Törőcsik D (2020) Adipokines in the skin and in dermatological diseases. Int J Mol Sci 21(23). https://doi.org/10.3390/ijms21239048
Kwon HC, Kim TY, Lee CM, Lee KS, Lee KK (2019) Active compound chrysophanol of Cassia tora seeds suppresses heat-induced lipogenesis via inactivation of JNK/p38 MAPK signaling in human sebocytes. Lipids Health Dis 18(1):135. https://doi.org/10.1186/s12944-019-1072-x
Leung AK, Barankin B, Lam JM, Leong KF, Hon KL (2021) Dermatology: how to manage acne vulgaris. Drugs Context 10. https://doi.org/10.7573/dic.2021-8-6
Lheure C, Grange PA, Ollagnier G, Morand P, Désiré N, Sayon S ... Dupin N (2016) TLR-2 recognizes Propionibacterium acnes CAMP factor 1 from highly inflammatory strains. PLoS ONE 11(11): e0167237. https://doi.org/10.1371/journal.pone.0167237
Liu C, Li L, Guo D, Lv Y, Zheng X, Mo Z, Xie W (2018) Lipoprotein lipase transporter GPIHBP1 and triglyceride-rich lipoprotein metabolism. Clin Chim Acta 487:33–40. https://doi.org/10.1016/j.cca.2018.09.020
Liu PT, Krutzik SR, Kim J, Modlin RL (2005) Cutting edge: all-trans retinoic acid down-regulates TLR2 expression and function. J Immunol 174(5):2467–2470. https://doi.org/10.4049/jimmunol.174.5.2467
Lopez S, Jaramillo S, Varela LM, Ortega A, Bermudez B, Abia R, Muriana FJ (2013) p38 MAPK protects human monocytes from postprandial triglyceride-rich lipoprotein-induced toxicity. J Nutr 143(5):620–626. https://doi.org/10.3945/jn.113.174656
Ma Y, Cao X, Zhang L, Zhang JY, Qiao ZS, Feng WL (2021) Neuropathy and chloracne induced by 3,5,6-trichloropyridin-2-ol sodium: report of three cases. World J Clin Cases 9(5): 1079–1086. https://doi.org/10.12998/wjcc.v9.i5.1079
Meisgen F, Xu Landén N, Wang A, Réthi B, Bouez C, Zuccolo M ... Pivarcsi A (2014) MiR-146a negatively regulates TLR2-induced inflammatory responses in keratinocytes. J Invest Dermatol 134(7): 1931-1940. https://doi.org/10.1038/jid.2014.89
Meng X, Qiu L, Song H, Dang N (2018) MAPK pathway involved in epidermal terminal differentiation of normal human epidermal keratinocytes. Open Med (wars) 13:189–195. https://doi.org/10.1515/med-2018-0029
Nabatanzi A, Mafuru M, Male M, Tian C, Zhang L, Wu T ... Huang C (2020) Feasibility study for the long-term management of refractory hyperkeratotic eczema with calcipotriol and betamethasone dipropionate (Daivobet(®)), viaminate and concomitant conventional therapies: a retrospective study. Clin Cosmet Investig Dermatol 13: 789-794. https://doi.org/10.2147/ccid.S276148
Rao X, Huang X, Zhou Z, Lin X (2013) An improvement of the 2ˆ(-delta delta CT) method for quantitative real-time polymerase chain reaction data analysis. Biostat Bioinforma Biomath 3(3):71–85
Törőcsik D, Kovács D, Póliska S, Szentkereszty-Kovács Z, Lovászi M, Hegyi K ... Ståhle M (2018) Genome wide analysis of TLR1/2- and TLR4-activated SZ95 sebocytes reveals a complex immune-competence and identifies serum amyloid A as a marker for activated sebaceous glands. PLoS ONE 13(6): e0198323. https://doi.org/10.1371/journal.pone.0198323
Usuki S, Tamura N, Tamura T, Yuyama K, Mikami D, Mukai K, Igarashi Y (2022) Konjac ceramide (kCer)-mediated signal transduction of the Sema3A pathway promotes HaCaT keratinocyte differentiation. Biology (Basel) 11(1). https://doi.org/10.3390/biology11010121
Wang Y, Zhang Z, Chen L, Guang H, Li Z, Yang H ... Lai R (2011) Cathelicidin-BF, a snake cathelicidin-derived antimicrobial peptide, could be an excellent therapeutic agent for acne vulgaris. PLoS ONE 6(7): e22120. https://doi.org/10.1371/journal.pone.0022120
Wöll S, Windoffer R, Leube RE (2007) p38 MAPK-dependent shaping of the keratin cytoskeleton in cultured cells. J Cell Biol 177(5):795–807. https://doi.org/10.1083/jcb.200703174
Yin J, Ni KY, Shen Y, Ma PC, Cao L, Wang WP, Wang Y (2007) Development and validation of a LC-MS/MS method for the determination of viaminate in human plasma. J Chromatogr B Analyt Technol Biomed Life Sci 856(1–2):376–380. https://doi.org/10.1016/j.jchromb.2007.06.033
Yuki T, Yoshida H, Akazawa Y, Komiya A, Sugiyama Y, Inoue S (2011) Activation of TLR2 enhances tight junction barrier in epidermal keratinocytes. J Immunol 187(6):3230–3237. https://doi.org/10.4049/jimmunol.1100058
Zhu T, Wu W, Yang S, Li D, Sun D, He L (2019) Polyphyllin I inhibits Propionibacterium acnes-induced inflammation in vitro. Inflammation 42(1):35–44. https://doi.org/10.1007/s10753-018-0870-z
Author information
Authors and Affiliations
Contributions
JC and SX contributed to the study conception and design. All authors collected the data and performed the data analysis. All authors contributed to the interpretation of the data and the completion of figures and tables. All authors contributed to the drafting of the article and final approval of the submitted version. The authors declare that all data were generated in-house and that no paper mill was used.
Corresponding author
Ethics declarations
Ethical approval
Ethical approval was given by the Ethics Committee of the Second Affiliated Hospital of Xi’an Jiaotong University (No.2022–1469).
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cao, J., Xu, M., Zhu, L. et al. Viaminate ameliorates Propionibacterium acnes-induced acne via inhibition of the TLR2/NF-κB and MAPK pathways in rats. Naunyn-Schmiedeberg's Arch Pharmacol 396, 1487–1500 (2023). https://doi.org/10.1007/s00210-022-02379-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-022-02379-0