Abstract
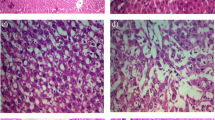
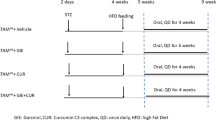
To observe the therapeutic effect of berberine (BBR) on non-alcoholic steatohepatitis (NASH) in rats and the underlying mechanism. A rat model of NASH was established by a high-fat diet, and BBR was used as treatment. Haematoxylin-eosin staining and Oil Red O staining were used to observe the pathological changes in the liver tissue. Western blotting and real-time PCR were used to measure the mRNA and protein levels in the liver. Flow cytometry was performed to detect the number of intrahepatic lymphocyte subtypes. The expression of pro-inflammatory cytokines in the peripheral blood was measured by ELISA. An automatic biochemical method was used to examine the level of blood lipids in the blood. Compared with the rats in the model group, the rats in the BBR group showed significantly improved liver histopathology and serum pro-inflammatory cytokines and free fatty acid (FFA) levels. Moreover, the protein and mRNA expression of chemerin, CMKLR1 and CCR2 in the liver were obviously reduced by BBR treatment. In addition, the high-fat diet remarkably reduced the intrahepatic Treg/Th17 ratio, which could be recovered by BBR treatment. Berberine can ameliorate non-alcoholic steatohepatitis, and its mechanism may be related to restoring the Treg/Th17 ratio, regulating the chemerin/CMKLR1 signalling pathway to reduce liver inflammation and reducing lipid deposition.





Similar content being viewed by others
References
Anty R, Gual P (2019) Pathogenesis of non-alcoholic fatty liver disease. Presse Med 48:1468–1483. https://doi.org/10.1016/j.lpm.2019.09.051
Buechler C, Feder S, Haberl EM, Aslanidis C (2019) Chemerin isoforms and activity in obesity. Int J Mol Sci 20. https://doi.org/10.3390/ijms20051128
Cao Y, Pan Q, Cai W, Shen F, Chen GY, Xu LM, Fan JG (2016) Modulation of gut microbiota by berberine improves steatohepatitis in high-fat diet-fed BALB/C mice. Arch Iran Med 19:197–203
Chang X, Wang Z, Zhang J, Yan H, Bian H, Xia M, Lin H, Jiang J, Gao X (2016) Lipid profiling of the therapeutic effects of berberine in patients with nonalcoholic fatty liver disease. J Transl Med 14:266. https://doi.org/10.1186/s12967-016-0982-x
Cicero AF, Baggioni A (2016) Berberine and its role in chronic disease. Adv Exp Med Biol 928:27–45. https://doi.org/10.1007/978-3-319-41334-1_2
Docke S, Lock JF, Birkenfeld AL, Hoppe S, Lieske S, Rieger A, Raschzok N, Sauer IM, Florian S, Osterhoff MA, Heller R, Herrmann K, Lindenmuller S, Horn P, Bauer M, Weickert MO, Neuhaus P, Stockmann M, Mohlig M, Pfeiffer AF, von Loeffelholz C (2013) Elevated hepatic chemerin mRNA expression in human non-alcoholic fatty liver disease. Eur J Endocrinol 169:547–557. https://doi.org/10.1530/eje-13-0112
Ernst MC, Haidl ID, Zuniga LA, Dranse HJ, Rourke JL, Zabel BA, Butcher EC, Sinal CJ (2012) Disruption of the chemokine-like receptor-1 (CMKLR1) gene is associated with reduced adiposity and glucose intolerance. Endocrinology 153:672–682. https://doi.org/10.1210/en.2011-1490
Farrell GC, Haczeyni F, Chitturi S (2018) Pathogenesis of NASH: how metabolic complications of overnutrition favour lipotoxicity and pro-inflammatory fatty liver disease. Adv Exp Med Biol 1061:19–44. https://doi.org/10.1007/978-981-10-8684-7_3
Hadinia A, Doustimotlagh AH, Goodarzi HR, Arya A, Jafarinia M (2019) Circulating levels of pro-inflammatory cytokines in patients with nonalcoholic fatty liver disease and non-alcoholic steatohepatitis. Iran J Immunol 16:327–333. https://doi.org/10.22034/iji.2019.80284
Kennedy AJ, Davenport AP (2018) International Union of Basic and Clinical Pharmacology CIII: Chemerin receptors CMKLR1 (Chemerin1) and GPR1 (Chemerin2) nomenclature, pharmacology, and function. Pharmacol Rev 70:174–196. https://doi.org/10.1124/pr.116.013177
Krautbauer S, Wanninger J, Eisinger K, Hader Y, Beck M, Kopp A, Schmid A, Weiss TS, Dorn C, Buechler C (2013) Chemerin is highly expressed in hepatocytes and is induced in non-alcoholic steatohepatitis liver. Exp Mol Pathol 95:199–205. https://doi.org/10.1016/j.yexmp.2013.07.009
Leamy AK, Egnatchik RA, Young JD (2013) Molecular mechanisms and the role of saturated fatty acids in the progression of non-alcoholic fatty liver disease. Prog Lipid Res 52:165–174. https://doi.org/10.1016/j.plipres.2012.10.004
Li J, Liu Z, Guo M (2015) Metabolomics profiling to investigate the pharmacologic mechanisms of berberine for the treatment of high-fat diet-induced nonalcoholic steatohepatitis. Evid Based Complement Alternat Med 2015:897914–897919. https://doi.org/10.1155/2015/897914
Liu J, Li W, Zhu W, He W, Zhao H, Xiang Y, Liu C, Wu W (2018a) Chronic intermittent hypoxia promotes the development of experimental non-alcoholic steatohepatitis by modulating Treg/Th17 differentiation. Acta Biochim Biophys Sin 50:1200–1210. https://doi.org/10.1093/abbs/gmy131
Liu XJ, Duan NN, Liu C, Niu C, Liu XP, Wu J (2018b) Characterization of a murine nonalcoholic steatohepatitis model induced by high fat high calorie diet plus fructose and glucose in drinking water. Lab Investig 98:1184–1199. https://doi.org/10.1038/s41374-018-0074-z
Machado MV, Diehl AM (2016) Pathogenesis of nonalcoholic steatohepatitis. Gastroenterology 150:1769–1777. https://doi.org/10.1053/j.gastro.2016.02.066
Mirmajidi S, Izadi A, Saghafi-Asl M, Vahid F (2019) Inflammatory potential of diet: association with chemerin, omentin, lipopolysaccharide-binding protein, and insulin resistance in the apparently healthy obese. J Am Coll Nutr 38:302–310. https://doi.org/10.1080/07315724.2018.1504348
Nati M, Haddad D, Birkenfeld AL, Koch CA, Chavakis T, Chatzigeorgiou A (2016) The role of immune cells in metabolism-related liver inflammation and development of non-alcoholic steatohepatitis (NASH). Rev Endocr Metab Disord 17:29–39. https://doi.org/10.1007/s11154-016-9339-2
Ogawa Y, Yoneda M, Kobayashi T, Honda Y, Kessoku T, Imajo K, Saito S, Nakajima A (2019) Present and emerging pharmacotherapies for non-alcoholic steatohepatitis in adults. Expert Opin Pharmacother 20:69–82. https://doi.org/10.1080/14656566.2018.1543403
Povsic M, Wong OY, Perry R, Bottomley J (2019) A structured literature review of the epidemiology and disease burden of non-alcoholic steatohepatitis (NASH). Adv Ther 36:1574–1594. https://doi.org/10.1007/s12325-019-00960-3
Ramadori P, Kroy D, Streetz KL (2015) Immunoregulation by lipids during the development of non-alcoholic steatohepatitis. Hepatobiliary Surg Nutr 4:11–23. https://doi.org/10.3978/j.issn.2304-3881.2015.01.02
Stojek M (2017) The role of chemerin in human disease. Postepy Hig Med Dosw (Online) 71:110–117. https://doi.org/10.5604/01.3001.0010.3795
Swiderska M, Jaroszewicz J, Stawicka A, Parfieniuk-Kowerda A, Chabowski A, Flisiak R (2017) The interplay between Th17 and T-regulatory responses as well as adipokines in the progression of non-alcoholic fatty liver disease. Clin Exp Hepatol 3:127–134. https://doi.org/10.5114/ceh.2017.68466
Xu K, Jiang M, Lu A, Gao X, Ghareeb DA, Khalil S, Hafez HS, Bajorath J, Ahmed HE, Sarhan E, Elwakeel E, El-Demellawy MA (2015) Berberine reduces neurotoxicity related to nonalcoholic steatohepatitis in rats. Evid Based Complement Alternat Med 2015:361847–361849. https://doi.org/10.1155/2015/897914
Yan HM, Xia MF, Wang Y, Chang XX, Yao XZ, Rao SX, Zeng MS, Tu YF, Feng R, Jia WP, Liu J, Deng W, Jiang JD, Gao X (2015) Efficacy of berberine in patients with non-alcoholic fatty liver disease. PLoS One 10:e0134172. https://doi.org/10.1371/journal.pone.0134172
Yang W, She L, Yu K, Yan S, Zhang X, Tian X, Ma S, Zhang X (2016) Jatrorrhizine hydrochloride attenuates hyperlipidemia in a high-fat diet-induced obesity mouse model. Mol Med Rep 14:3277–3284. https://doi.org/10.3892/mmr.2016.5634
Yang J, Ma XJ, Li L, Wang L, Chen YG, Liu J, Luo Y, Zhuang ZJ, Yang WJ, Zang SF, Shi JP (2017) Berberine ameliorates non-alcoholic steatohepatitis in ApoE(-/-) mice. Exp Ther Med 14:4134–4140. https://doi.org/10.3892/etm.2017.5051
Ye F, Zhou Q, Tian L, Lei F, Feng D (2017) The protective effect of berberine hydrochloride on LPSinduced osteoclastogenesis through inhibiting TRAF6Ca2+calcineurinNFATcl signaling pathway. Mol Med Rep 16:6228–6233. https://doi.org/10.3892/mmr.2017.7338
Zhu L, Gu P, Shen H (2019) Protective effects of berberine hydrochloride on DSS-induced ulcerative colitis in rats. Int Immunopharmacol 68:242–251. https://doi.org/10.1016/j.intimp.2018.12.036
Funding
The study was supported by the Medical Health Science and Technology Project of Zhejiang Provincial Health Commission (2018KY322), the Scientific Research Foundation of State Administration of Traditional Chinese Medicine of Zhejiang Province (2016ZB004, 2019ZA024, 2020ZB056) and the Program of Zhejiang Province Natural Science Foundation (LQ20H290002).
Author information
Authors and Affiliations
Contributions
Liyan Wu designed the experiment and revised the manuscript. Zengsheng Lu and Fengbin Lu drafted the article and analysed the data. Zhiyun Chen revised it critically for important intellectual content. Liyan Wu, Fengbin Lu, Beihui He and Maoxiang Yan performed the experiment. All authors promise all data are generated in-house, and did not use a paper mill. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
The experimental protocols were established according to the Declaration of Helsinki. All animals used in this study complied with the ARRIVE guidelines and the protocols were approved by the institutional animal committee of Zhejiang Academy of Traditional Chinese Medicine.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Zengsheng Lu and Fengbin Lu share first authorship.
Rights and permissions
About this article
Cite this article
Lu, Z., Lu, F., Wu, L. et al. Berberine attenuates non-alcoholic steatohepatitis by regulating chemerin/CMKLR1 signalling pathway and Treg/Th17 ratio. Naunyn-Schmiedeberg's Arch Pharmacol 394, 383–390 (2021). https://doi.org/10.1007/s00210-020-01914-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-020-01914-1