Abstract
VX, a potent inhibitor of cholinesterase (ChE), is considered as one of the most toxic, persistent and least volatile nerve agents. VX is absorbed in various environmental surfaces and is gradually released long after its initial dispersal. Its toxicity is mainly caused by disrupting central and peripheral cholinergic nervous system activity, leading to potential long-term detrimental effects on health. The primary objective of the present study was to assess the threshold VX dose leading to minimal physiological alterations following prolonged VX exposure. Characterization of such a threshold is crucial for dealing with unresolved operative dilemmas such as when it is safe enough to resettle a population that has been evacuated from a VX-contaminated area. Rats, continuously exposed to various doses of VX (0.225–45 µg/kg/day) for 4 weeks via implanted mini-osmotic pumps, showed a dose-dependent and continuous decrease in ChE activity in whole blood, brain and muscles, ranging between 20 and 100%. Exposure to 13.5 µg/kg/day led to a stable low ChE activity level (~ 20%), accompanied by transient and negligible electrocorticogram spectral power transformations, especially in the theta and alpha brain wave frequencies, and a significant decrease in total brain M2 receptor density. These changes were neither accompanied by observable signs of intoxication nor by changes in motor function, circadian rhythm or TSPO level (a reliable marker of brain damage). Following exposure to lower doses of 2.25 and 0.225 µg/kg/day, the only change measured was a reduction in ChE activity of 60 and 20%, respectively. Based on these results, we delineate ChE inhibition as the physiological measure most susceptible to alterations following prolonged VX exposure, and determine for the first time the threshold sub-acute VX dose for minimal physiological effects (up to 20% reduction in ChE activity) in the rat as 0.225 µg/kg/day.









Similar content being viewed by others
Abbreviations
- ACh:
-
Acetylcholine
- AChE:
-
Acetylcholinesterase
- AEL:
-
Airborne exposure limits
- EEG:
-
Electroencephalogram
- ECoG:
-
Electrocorticogram
- FFT:
-
Fast Fourier transform
- OP:
-
Organophosphate
- OPNA:
-
Organophosphorus nerve agents
- TSPO:
-
Translocator protein
References
Abou-Donia MB, Goldstein LB, Bullman S, Tu T, Khan WA, Dechkovskaia AM, Abdel-Rahman AA (2008) Imidacloprid induces neurobehavioral deficits and increases expression of glial fibrillary acidic protein in the motor cortex and hippocampus in offspring rats following in utero exposure. J Toxicol Environ Health A 71:119–123
Allon N, Chapman S, Egoz I, Rabinovitz I, Kapon J, Weissman BA, Yacov G, Bloch-Shilderman E, Grauer E (2011) Deterioration in brain and heart functions following a single sub-lethal (0.8 LCt50) inhalation exposure of rats to sarin vapor: a putative mechanism of the long term toxicity. Toxicol Appl Pharmacol 253:31–37
Ashani Y, Pistiner S (2004) Estimation of the upper limit of human butyrylcholinesterase dose required for protection against organophosphates toxicity: a mathematically based toxokinetic model. Toxicol Sci 77:358–367
Atchison CR, Sheridan RE, Duniho SM, Shih TM (2004) Development of a guinea pig model for low-dose, long-term exposure to organophosphorus nerve agents. Toxicol Mech Meth 14:183–194
Benavides J, Dubois A, Scatton B (1999) Peripheral type benzodiazepine binding sites as a tool for the detection and quantification of CNS injury. Curr Prot Neurosci 16:1–7
Bennion BJ, Lau EY, Fattebert JL, Huang P, Schwegler P, Corning W, Lightstone FC (2013) Modeling the binding of CWAs to AChE and BuChE. Mil Med Sci Lett 82:102–114
Benton BJ, McGuire JM, Sommerville DR, Dabisch PA, Jakubowski EM, Matson KL, Mioduszewski RJ, Thomson SA (2006) Effects of whole-body VX vapor exposure on lethality in rats. Inhal Toxicol 18:1091–1099
Black RM, Harrison JM (1996) The chemistry of organophosphorus chemical warfare agents. In: Hartley FR (ed) The chemistry of organophosphorus compounds, vol 4. Wiley, Chichester, pp 783–798
Bloch-Shilderman E, Kadar T, Levy A, Sahar R, Rabinovitz I, Gilat E (2005) Subcellular alterations of protein kinase C isozymes in the rat brain after organophosphate poisoning. J Pharmacol Exp Ther 313:1–8
Bloch-Shilderman E, Rabinovitz I, Egoz I, Raveh L, Allon N, Grauer E, Gilat E, Weissman BA (2008) Chronic exposure of rats to low doses of the nerve-agent VX: physiological, behavioral, histopathological and neurochemical studies. Toxicol Appl Pharmacol 231:17–23
Bomser JA, Casida JE (2001) Diethylphosphorylation of rat cardiac M2 muscarinic receptor by chlorpyrifos oxon in vitro. Toxicol Lett 119:21–26
Bosković B (1979) The influence of 2-/o-cresyl/-4 H-1:3:2-benzodioxa-phosphorin-2-oxide (CBDP) on organophosphate poisoning and its therapy. Arch Toxicol 42:207–216
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72:248–254
Brown MA, Brix KA (1998) Review of health consequences from high-, intermediate-, and low-level exposure of organophosphate nerve agents. J Appl Toxicol 18:393–408
Bueters TJH, Joosen MJA, Van Helden HPM, Ijzerman AP, Danhof M (2003) Adenosine A1 receptor agonist N6-cyclopentyladenosine affects the inactivation of acetylcholinesterase in blood and brain by sarin. J Pharmacol Exp Ther 304:1307–1313
Burchfiel JL, Duffy FH (1982) Organophosphate neurotoxicity: chronic Effects of sarin on the electroencephalogram of monkey and man. Neurobehav Toxicol Teratol 4:767–778
Cape EG, Manns ID, Alonso A, Beaudet A, Jones BE (2000) Neurotensin-induced bursting of cholinergic basal forebrain neurons promotes γ and θ cortical activity together with waking and paradoxical sleep. J Neurosci 20:8452–8461
Churchill L, Pazdernik TL, Jackson JL, Nelson SR, Samson FE, McDonough JH Jr, McLeod CG Jr (1985) Soman-induced brain lesions demonstrated by muscarinic receptor autoradiography. Neurotoxicology 6:81–90
Collombet JM (2011) Nerve agent intoxication: recent neuropathophysiological findings and subsequent impact on medical management prospects. Toxicol Appl Pharmacol 255:229–241
Columbus I, Waysbort D, Marcovitch I, Yehezkel L, Mizrahi DM (2012) VX fate on common matrices: evaporation versus degradation. Environ Sci Technol 46:3921–3927
Duffy FH, Burchfiel JL, Bartels PH, Gaon M, Sim VM (1979) Long-term effects of an organophosphate upon the human electroencephalogram. Toxicol Appl Pharmacol 47:161–176
Ellin R (1982) Anomalies in theories and therapy of intoxication by potent organophosphorus anticholinesterase compounds. Gen Pharmacol 13:457–466
Ellman GL, Courtney KD, Andres V, Featherstone RM (1961) A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem Pharmacol 7:88–95
Federal Register (2003) Final recommendations for protecting human health from potential adverse effects of exposure to agents GA, GB, and VX. Fed Reg 68(196):58348–58351
Fonnum F, Sterri SH (1981) Factors modifying the toxicity of organophosphorous compounds including soman and sarin. Fundam Appl Toxicol 1(2):143–147
Genovese RF, Benton BJ, Lee EH, Shippee SJ, Jakubowski EM (2007) Behavioral and biochemical evaluation of sub-lethal inhalation exposure to VX in rats. Toxicology 232:109–118
Gordon CJ, Padnos BK (2002) Dietary exposure to chlorpyrifos alters core temperature in the rat. Toxicology 177:215–226
Graziani S, Christin D, Daulon S, Breton P, Perrier N, Taysse L (2014) Effects of repeated low-dose exposure of the nerve agent VX on monoamine levels in different brain structures in mice. Neurochem Res 39:911–921
Gundavarapu S, Zhuang J, Barrett EG, Xu F, Russell RG, Sopori ML (2014) A critical role of acute bronchoconstriction in the mortality associated with high-dose sarin inhalation: effects of epinephrine oxygen therapies. Toxicol Appl Pharmacol 274:200–208
Gura S, Tzanani N, Herschkovitz M, Barak R, Dagan S (2006) Fate of chemical warfare agent VX in asphalt: a novel approach for quantitation of VX in organic surfaces. Arch Environ Contam Toxicol 51:1–10
Hulet SW, Sommerville DR, Miller DB, Scotto JA, Muse WT, Burnett DC (2014) Comparison of sarin and cyclosarin toxicity by subcutaneous, intravenous and inhalation exposure in Gottingen minipigs. Inhal Toxicol 26:175–184
Jamal GA (1997) Neurological syndromes of organophosphorous compounds. Adverse Drug React Toxicol Rev 16:133–170
Jamal GA, Hansen S, Julu PO (2002) Low level exposures to organophosphorus esters may cause neurotoxicity. Toxicology 181–182:23–33
Jimmerson VR, Shih TM, Mailman RB (1989) Variability in soman toxicity in the rat: correlation with biochemical and behavioral measures. Toxicology 57:241–254
Johnson CD, Russell RL (1975) A rapid simple radiometric assay for cholinesterase suitable for multiple determinations. Anal Biochem 64:229–238
Jokanovic M (2009) Current understanding of the mechanism involved in metabolic detoxification of warfare nerve agents. Toxicol Lett 188:1–10
Kamel F, Hoppin JA (2004) Association of pesticide exposure with neurologic dysfunction and disease. Environ Health Perspect 112:950–958
Kassa J, Kunesova G (2006) The influence of antidotal treatment of low-level tabun exposure on cognitive functions in rats using a water maze. Neurotox Res 9:39–45
Kassa J, Pecka M, Tichy M, Bajgar J, Koupilova M, Herink J, Krocova Z (2001) Toxic effects of sarin in rats at 3 months following single or repeated low-level inhalation exposure. Pharmacol Toxicol 88:209–212
Kryger M, Monjan A, Bliwise D, Ancoli-Israel S (2004) Sleep, health, and aging. Bridging the gap between science and clinical practice. Geriatrics 59(24–26):29–30
Lee MG, Manns ID, Alonso A, Jones BE (2004) Sleep-wake related discharge properties of basal forebrain neurons recorded with micropipettes in head-fixed rats. J Neurophysiol 92:1182–1198
Lee MG, Hassani OK, Alonso A, Jones BE (2005) Cholinergic basal forebrain neurons burst with theta during waking and paradoxical sleep. J Neurosci 25:4365–4369
Lenz DE, Maxwell DM, Austin LW (1997) Development of a rat model for subacute exposure to the toxic organophosphate VX. J Am Coll Toxicol 15:s69–s77
Macilwain C (1993) Study proves Iraq used nerve gas. Nature 363:3
Marrs TC (2007) Toxicology of organophosphate nerve agents. In: Marrs TC, Maynard RL, Sidell F (eds) Chemical warfare agents: toxicology and treatment, 2nd edn. Wiley, Chichester, pp 191–222
Meeter E, Wolthuis OL (1968) The spontaneous recovery of respiration and neuromuscular transmission in the rat after anticholinesterase poisoning. Eur J Pharmacol 2:377–386
Metcalf DR, Holmes JH (1969) EEG, psychological and neurological alterations in humans with organophosphate exposure. Ann NY Acad Sci 160:357–365
Miller JH, Gibson VA, McKinney M (1991) Binding of [3H]AF-DX 384 to cloned and native muscarinic receptors. J Pharmacol Exp Ther 259:601–607
Moore DH (1998) Health effects of exposure to low doses of nerve agents—a review of present knowledge. Drug Chem Toxicol 21:123–130
Munro NB, Ambrose KR, Watson AP (1994) Toxicity of the organophosphate chemical warfare agents GA, GB, and VX: implications for public protection. Environ Health Perspect 102:18–38
Munro NB, Talmage SS, Griffin GD, Waters LC, Watson AP, King JF, Hauschild V (1999) The sources, fate, and toxicity of chemical warfare agent degradation products. Environ Health Perspect 107:933–974
Muse WT, Thomson S, Crouse C, Matson K (2006) Generation, sampling, and analysis for low-level GB (Sarin) and GF (Cyclosarin) vapor for inhalation toxicology studies. Inhal Toxicol 18:1101–1108
Nagao M, Takatori T, Matsuda Y, Nakajima M, Iwase H, Iwadate K (1997) Definitive evidence for the acute sarin poisoning diagnosis in the Tokyo subway. Toxicol Appl Pharmacol 144:198–203
Naik RS, Liu W, Saxena A (2013) Development and validation of a simple assay for the determination of cholinesterase activity in whole blood of laboratory animals. J Appl Toxicol 33:290–300
National Research Council (2005) Impact of revised airborne exposure limits on non-stockpile chemical materiel program activities. The National Academic Press, Washington DC
Nishiwaki Y, Maekawa K, Ogawa Y, Asukai N, Minami M, Omae K, Sarin Health Effects Study Group (2001) Effects of sarin on the nervous system in rescue team staff members and police officers 3 years after the Tokyo subway sarin attack. Environ Health Perspect 109:1169–1173
Oswal DP, Garrett TL, Morris M, Lucot JB (2013) Low-dose sarin exposure produces long term changes in brain neurochemistry of mice. Neurochem Res 38:108–116
Pearce PC, Crofts HS, Muggleton NG, Ridout D, Scott EAM (1999) The effects of acutely administered low dose sarin on cognitive behaviour and the electroencephalogram in the common marmoset. J Psychopharmacol 13:128–135
Peng X, Perkins MW, Simons J, Witriol AM, Rodriguez AM, Benjamin BM, Devorak J, Sciuto AM (2014) Acute pulmonary toxicity following inhalation exposure to aerosolized VX in anesthetized rats. Inhal Toxicol 26:371–379
Pizarro JM, Chang WE, Bah MJ, Wright LKM, Saviolakis GA, Alagappan A, Robison CL, Shah JD, Meyerhoff JL, Cerasoli DM, Midboe EG, Lumley LA (2012) Repeated exposure to sublethal doses of the organophosphorus compound VX activates BDNF expression in mouse brain. Toxicol Sci 126:497–505
Raber E, Carlsen T, Folks K, Kirvel R, Daniels J, Bogen K (2004) How clean is clean enough? Recent developments in response to threats posed by chemical and biological warfare agents. Int J Environ Health Res 14:31–41
Ray DE (1998) Chronic effects of low level exposure to anticholinesterases—a mechanistic review. Toxicol Lett 102–103:527–533
Reiter G, Müller S, Hill I, Weatherby K, Thiermann H, Worek F, Mikler J (2015) In vitro and in vivo toxicological studies of V nerve agents: molecular and stereoselective aspects. Toxicol Lett 232:438–448
Rocksen D, Elfsmark D, Heldestad V, Wallgren K, Cassel G, Nyberg G (2008) An animal model to study health effects during continuous low-dose exposure to the nerve agent VX. Toxicology 250:32–38
Romano JA Jr, McDonough JH, Sheridan R, Sidell FR (2001) Health effects of low-level exposure to nerve agents. In: Somani SM, Romano JA Jr (eds) Chemical warfare agents: toxicity at low levels, 1st edn. CRC Press, Taylor & Francis Group, Boca Raton, pp 1–24
Salvi RM, Lara DR, Ghisolfi ES, Portela LV, Dias RD, Souza DO (2003) Neuropsychiatric evaluation in subjects chronically exposed to organophosphate pesticides. Toxicol Sci 72:267–271
Shih TM, Hulet SW, McDonough JH (2006) The effects of repeated low-dose sarin exposure. Toxicol Appl Pharmacol 215:119–134
Sidell RF, Groff WA (1974) The reactivatibility of cholinesterase inhibited by VX and sarin in man. Toxicol Appl Pharmacol 27:241–252
Signorino M, Pucci E, Brizioli E, Cacchio G, Nolfe G, Angeleri F (1996) EEG power spectrum typical of vascular dementia in a subgroup of Alzheimer patients. Arch Gerontol Geriatr 23:139–151
Sweeny RE, Maxwell DM (2003) A theoretical expression for the protection associated with stoichiometric and catalytic scavengers in a single compartment model of organophosphorus poisoning. Math Biosci 181:133–143
Terry AV Jr (2012) Functional consequences of repeated organophosphate exposure: potential non-cholinergic mechanisms. Pharmacol Ther 134:355–365
Tillman GD, Calley CS, Green TA, Buhl VI, Biggs MM, Spence JS, Briggs RW, Haley RW, Hart J, Kraut MA Jr (2012) Event-related potential patterns associated with hyperarousal in Gulf War illness syndrome groups. Neurotoxicology 33:1096–1105
Timofeeva OA, Gordon CJ (2001) Changes in EEG power spectra and behavioral states in rats exposed to the acetylcholinesterase inhibitor chlorpyrifos and muscarinic agonist oxotremorine. Brain Res 893:165–177
Timofeeva OA, Gordon CJ (2002) EEG spectra, behavioral states and motor activity in rats exposed to the acetylcholinesterase inhibitor chlorpyrifos. Pharmacol Biochem Behav 72:669–679
Tonduli LS, Testylier G, Pernot Marino I, Lallement G (1999) Triggering of soman-induced seizures in rats: multiparametric analysis with special correlation between enzymatic, neurochemical and electrophysiological data. J Neurosci Res 58:464–473
van der Schans MJ, Lander BJ, van der Wiel H, Langenberg JP, Benschop HP (2003) Toxicokinetics of the nerve agent (±)-VX in anesthetized and atropinized hairless guinea pigs and marmosets after intravenous and percutaneous administration. Toxicol Appl Pharmacol 191:48–62
van Helden HPM, Vanwersch RAP, Kuijpers WC, Trap HC, Philippens IHC, Benschop HP (2004) Low levels of sarin affect the EEG in marmoset monkeys: a pilot study. J Appl Toxicol 24:475–483
Watson AP, Jones TD, Adams JD (1992) Relative potency estimates of acceptable residues and reentry intervals after nerve agent release. Ecotoxicol Environ Saf 23:328–342
Watson AP, Opresko D, Young R, Hauschild V (2006) Development and application of acute exposure guideline levels (AEGLs) for chemical warfare nerve and sulfur mustard agents. J Toxicol Environ Health B Crit Rev 9:173–263
Weissman BA, Raveh L (2003) Peripheral benzodiazepine receptors: on mice and human brain imaging. J Neurochem 84:432–437
Whishaw IQ, Coles BL (1996) Varieties of paw and digit movement during spontaneous food handling in rats: postures, bimanual coordination, preferences, and the effect of forelimb cortex lesions. Behav Brain Res 77:135–148
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
204_2017_2108_MOESM1_ESM.docx
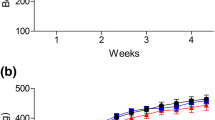
Circadian rhythm of body temperature and motor activity during continuous exposure to 2.25 or 13.5 µg/kg/day of VX. Following baseline recordings, rats were continuously exposed to propylene glycol (Sham) or VX (2.25 (a,b) or 13.5 µg/kg/day (c,d)) via subcutaneously implanted mini osmotic pumps for 4 weeks (n=4/group in both experiments). Recordings from the 7 days pre and 15 days post beginning of exposure are shown. Telemetry data collected every 5 minutes was analyzed and presented using four hour bins. Each data point represents the mean ± SEM of the group’s delta in body temperature (a,c) and motor activity (b,d) relative to the average of these measures along the entire duration of the experiment presented (Black dotted line depicting a delta of zero. For more details regarding the analysis see materials and methods). In all graphs the black arrow denotes beginning of exposure. In two separate additional experiments with both VX doses as compared to Sham (n=4 per group in each experiment) a similar result was obtained (data not shown) (DOCX 73 kb)
Rights and permissions
About this article
Cite this article
Bloch-Shilderman, E., Rabinovitz, I., Egoz, I. et al. Determining a threshold sub-acute dose leading to minimal physiological alterations following prolonged exposure to the nerve agent VX in rats. Arch Toxicol 92, 873–892 (2018). https://doi.org/10.1007/s00204-017-2108-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-017-2108-5