Abstract
Summary
This research is a cross-sectional study based on the participants aged 50 years and older from National Health and Nutrition Examination Survey (NHANES) database. The metabolic associated fatty liver disease (MAFLD) population has higher BMD and a lower risk of osteoporosis than those without MAFLD.
Introduction
MAFLD is a new definition presented by panel of experts based on non-alcoholic fatty liver disease in 2020. However, the link between MAFLD and bone mineral density (BMD) is uncertain. Thus, the present study aimed to investigate the relationship between MAFLD and BMD.
Methods
This cross-sectional study included subjects aged ≥ 50 years from the National Health and Nutrition Examination Survey 2017–2018. Multivariate linear regression models were performed to investigate the association between MAFLD and BMD. Moreover, the relationship between MAFLD and osteoporosis was assessed using multiple logistic regression models.
Results
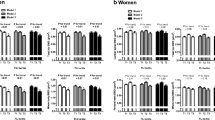
Finally, 817 participants (non-MAFLD, n = 436; MAFLD, n = 381) were included in the final analysis. The results demonstrated that participants with MAFLD showed higher femoral BMDs than those without MAFLD, especially among males aged ≥ 50 years and females aged ≥ 65 years. Moreover, the results showed that obese men (BMI ≥ 30 kg/m2) with MAFLD had higher femoral BMDs than the control group according to subgroup analyses stratified by BMI, but this trend was not present in women. In addition, multiple logistic regression models showed that participants with MAFLD had no increased risks of osteoporosis.
Conclusion
The present study found that the MAFLD population has higher BMD and a lower risk of osteoporosis than those without MAFLD. Because the present study was a cross-sectional study, we could not identify the cause-effect relation between MAFLD and BMD. Therefore, additional research needs to be performed to explore the influences of MAFLD on bone metabolism in the future.

Similar content being viewed by others
Data availability
All data were extracted from National Health and Nutrition Examination Survey (NHANES) 2017–2018 database. The detailed information was provided on the NHANES website.
Code availability
All analyses were performed with R software, V.4.1.3 (R: a language and statistical computing environment [program]. Vienna, Austria: R Foundation for Statistical Computing, 2016) and EmpowerStats (http://www.empowerstats.com).
References
Younossi ZM, Koenig AB, Abdelatif D, Fazel Y, Henry L, Wymer M (2016) Global epidemiology of nonalcoholic fatty liver disease-Meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology 64(1):73–84
Cotter TG, Rinella M (2020) Nonalcoholic fatty liver disease 2020: the state of the disease. Gastroenterology 158(7):1851–1864
Ciardullo S, Perseghin G (2021) Prevalence of NAFLD, MAFLD and associated advanced fibrosis in the contemporary United States population. Liver Int 41(6):1290–1293
Younossi ZM (2019) Non-alcoholic fatty liver disease — a global public health perspective. J Hepatol 70(3):531–544
Eslam M, Newsome PN, Sarin SK, Anstee QM, Targher G, Romero-Gomez M, Zelber-Sagi S, Wai-Sun Wong V, Dufour JF, Schattenberg JM et al (2020) A new definition for metabolic dysfunction-associated fatty liver disease: an international expert consensus statement. J Hepatol 73(1):202–209
Ensrud KE, Crandall CJ (2017) Osteoporosis. Ann Intern Med 167(3):17–32
Wright NC, Looker AC, Saag KG, Curtis JR, Delzell ES, Randall S, Dawson-Hughes B (2014) The recent prevalence of osteoporosis and low bone mass in the United States based on bone mineral density at the femoral neck or lumbar spine. J Bone Miner Res 29(11):2520–2526
Russell LA (2010) Osteoporosis and osteomalacia. Rheum Dis Clin North Am 36(4):665–680
Chen DZ, Xu QM, Wu XX, Cai C, Zhang LJ, Shi KQ, Shi HY, Li LJ (2018) The combined effect of nonalcoholic fatty liver disease and metabolic syndrome on osteoporosis in postmenopausal females in eastern China. Int J Endocrinol 2018:2314769
Lin S, Huang J, Wang M, Kumar R, Liu Y, Liu S, Wu Y, Wang X, Zhu Y (2020) Comparison of MAFLD and NAFLD diagnostic criteria in real world. Liver Int 40(9):2082–2089
Adams LA, Anstee QM, Tilg H, Targher G (2017) Non-alcoholic fatty liver disease and its relationship with cardiovascular disease and other extrahepatic diseases. Gut 66(6):1138–1153
Lee DY, Park JK, Hur KY, Um SH (2018) Association between nonalcoholic fatty liver disease and bone mineral density in postmenopausal women. Climacteric 21(5):498–501
Zhai T, Chen Q, Xu J, Jia X, Xia P (2021) Prevalence and trends in low bone density, osteopenia and osteoporosis in U.S. adults with non-alcoholic fatty liver disease, 2005–2014. Front Endocrinol (Lausanne) 12:825448
CDC (2017) National Health and Nutrition Examination Survey, NHANES 2017–2018. https://wwwn.cdc.gov/nchs/nhanes/continuousnhanes/default.aspx?BeginYear=2017 Accessed 22 April 2022
Weng Z, Ou W, Huang J, Singh M, Wang M, Zhu Y, Kumar R, Lin S (2021) Circadian misalignment rather than sleep duration is associated with MAFLD: a population-based propensity score-matched study. Nat Sci Sleep 13:103–111
Looker AC, Orwoll ES, Johnston CC Jr, Lindsay RL, Wahner HW, Dunn WL, Calvo MS, Harris TB, Heyse SP (1997) Prevalence of low femoral bone density in older U.S. adults from NHANES III. J Bone Miner Res 12(11):1761–1768
Ciardullo S, Muraca E, Zerbini F, Manzoni G, Perseghin G (2021) NAFLD and liver fibrosis are not associated with reduced femoral bone mineral density in the general US population. J Clin Endocrinol Metab 106(8):e2856–e2865
Ahn SH, Seo DH, Kim SH, Nam MS, Hong S (2018) The relationship between fatty liver index and bone mineral density in Koreans: KNHANES 2010–2011. Osteoporos Int 29(1):181–190
Xie R, Liu M (2022) Relationship between non-alcoholic fatty liver disease and degree of hepatic steatosis and bone mineral density. Front Endocrinol (Lausanne) 13:857110
Shen Z, Cen L, Chen X, Pan J, Li Y, Chen W, Yu C (2020) Increased risk of low bone mineral density in patients with non-alcoholic fatty liver disease: a cohort study. Eur J Endocrinol 182(2):157–164
Liang Y, Chen H, Liu Y, Hou X, Wei L, Bao Y, Yang C, Zong G, Wu J, Jia W (2022) Association of MAFLD with diabetes, chronic kidney disease, and cardiovascular disease: a 4.6-year cohort study in China. J Clin Endocrinol Metab 107(1):88–97
Lim GEH, Tang A, Ng CH, Chin YH, Lim WH, Tan DJH, Yong JN, Xiao J, Lee CW, Chan M et al. (2021) An observational data meta-analysis on the differences in prevalence and risk factors between MAFLD vs NAFLD. Clin Gastroenterol Hepatol
Felson DT, Zhang Y, Hannan MT, Anderson JJ (1993) Effects of weight and body mass index on bone mineral density in men and women: the Framingham study. J Bone Miner Res 8(5):567–573
Seeman E, Bianchi G, Khosla S, Kanis JA, Orwoll E (2006) Bone fragility in men—where are we? Osteoporos Int 17(11):1577–1583
Kinjo M, Setoguchi S, Solomon DH (2007) Bone mineral density in adults with the metabolic syndrome: analysis in a population-based U.S. sample. J Clin Endocrinol Metab 92(11):4161–4164
Bagherzadeh M, Sajjadi-Jazi SM, Sharifi F, Ebrahimpur M, Amininezhad F, Ostovar A, Shafiee G, Heshmat R, Mehrdad N, Razi F et al (2020) Effects of metabolic syndrome on bone health in older adults: the Bushehr Elderly Health (BEH) program. Osteoporos Int 31(10):1975–1984
Wiacek M, Skrzek A, Ignasiak Z, Zubrzycki IZ (2010) The changes of bone mineral density in relation to body mass index and aging among Polish and different ethnic women in the United States: cross-sectional studies. J Clin Densitom 13(3):307–314
Evans AL, Paggiosi MA, Eastell R, Walsh JS (2015) Bone density, microstructure and strength in obese and normal weight men and women in younger and older adulthood. J Bone Miner Res 30(5):920–928
Movérare-Skrtic S, Wu J, Henning P, Gustafsson KL, Sjögren K, Windahl SH, Koskela A, Tuukkanen J, Börjesson AE, Lagerquist MK et al (2015) The bone-sparing effects of estrogen and WNT16 are independent of each other. Proc Natl Acad Sci U S A 112(48):14972–14977
Haffner SM, Bauer RL (1993) The association of obesity and glucose and insulin concentrations with bone density in premenopausal and postmenopausal women. Metabolism 42(6):735–738
Goulding A, Taylor RW (1998) Plasma leptin values in relation to bone mass and density and to dynamic biochemical markers of bone resorption and formation in postmenopausal women. Calcif Tissue Int 63(6):456–458
Krishnan A, Muthusami S (2017) Hormonal alterations in PCOS and its influence on bone metabolism. J Endocrinol 232(2):R99-r113
Hla MM, Davis JW, Ross PD, Wasnich RD, Yates AJ, Ravn P, Hosking DJ, McClung MR (1996) A multicenter study of the influence of fat and lean mass on bone mineral content: evidence for differences in their relative influence at major fracture sites Early Postmenopausal Intervention Cohort (EPIC) Study Group. Am J Clin Nutr 64(3):354–360
Thrailkill KM, Lumpkin CK Jr, Bunn RC, Kemp SF, Fowlkes JL (2005) Is insulin an anabolic agent in bone? Dissecting the diabetic bone for clues. Am J Physiol Endocrinol Metab 289(5):E735-745
Napoli N, Chandran M, Pierroz DD, Abrahamsen B, Schwartz AV, Ferrari SL (2017) Mechanisms of diabetes mellitus-induced bone fragility. Nat Rev Endocrinol 13(4):208–219
Wang L, Shi S, Bai R, Wang Y, Guo Z, Li D (2020) Biological properties of bone marrow stem cells and adipose-derived stem cells derived from T2DM rats: a comparative study. Cell Biosci 10:102
Nawata H, Tanaka S, Tanaka S, Takayanagi R, Sakai Y, Yanase T, Ikuyama S, Haji M (1995) Aromatase in bone cell: association with osteoporosis in postmenopausal women. J Steroid Biochem Mol Biol 53(1–6):165–174
Cleland WH, Mendelson CR, Simpson ER (1985) Effects of aging and obesity on aromatase activity of human adipose cells. J Clin Endocrinol Metab 60(1):174–177
Blain H, Vuillemin A, Guillemin F, Durant R, Hanesse B, de Talance N, Doucet B, Jeandel C (2002) Serum leptin level is a predictor of bone mineral density in postmenopausal women. J Clin Endocrinol Metab 87(3):1030–1035
Bocalini DS, Serra AJ, dos Santos L, Murad N, Levy RF (2009) Strength training preserves the bone mineral density of postmenopausal women without hormone replacement therapy. J Aging Health 21(3):519–527
Camhi SM, Bray GA, Bouchard C, Greenway FL, Johnson WD, Newton RL, Ravussin E, Ryan DH, Smith SR, Katzmarzyk PT (2011) The relationship of waist circumference and BMI to visceral, subcutaneous, and total body fat: sex and race differences. Obesity (Silver Spring) 19(2):402–408
Jackson AS, Stanforth PR, Gagnon J, Rankinen T, Leon AS, Rao DC, Skinner JS, Bouchard C, Wilmore JH (2002) The effect of sex, age and race on estimating percentage body fat from body mass index: The Heritage Family Study. Int J Obes Relat Metab Disord 26(6):789–796
Liu YH, Xu Y, Wen YB, Guan K, Ling WH, He LP, Su YX, Chen YM (2013) Association of weight-adjusted body fat and fat distribution with bone mineral density in middle-aged Chinese adults: a cross-sectional study. PLoS ONE 8(5):e63339
Krishnan C, Choksi P, Peterson MD (2017) Abdominal adiposity and low physical activity are independently and inversely associated with bone mineral density. Obes Res Clin Pract 11(6):740–746
Bi X, Loo YT, Henry CJ (2020) Relationships between adiponectin and bone: sex difference. Nutrition 70:110489
Schwartz AV, Ewing SK, Porzig AM, McCulloch CE, Resnick HE, Hillier TA, Ensrud KE, Black DM, Nevitt MC, Cummings SR et al (2013) Diabetes and change in bone mineral density at the hip, calcaneus, spine, and radius in older women. Front Endocrinol (Lausanne) 4:62
Schwartz AV, Garnero P, Hillier TA, Sellmeyer DE, Strotmeyer ES, Feingold KR, Resnick HE, Tylavsky FA, Black DM, Cummings SR et al (2009) Pentosidine and increased fracture risk in older adults with type 2 diabetes. J Clin Endocrinol Metab 94(7):2380–2386
Wells GA, Cranney A, Peterson J, Boucher M, Shea B, Robinson V, Coyle D (2008) Tugwell P 2008 Etidronate for the primary and secondary prevention of osteoporotic fractures in postmenopausal women. Cochrane Database Syst Rev 1:003376
Acknowledgements
We would like to express our gratitude to American Journal Experts (https://www.aje.com/) for the language editing services provided.
Funding
This study was supported by the National Natural Science Foundation of China (81874017, 81960403, and 82060405) and Cuiying Scientific and Technological Innovation Program of Lanzhou University Second Hospital (CY2017-ZD02, CY2021-MS-A07).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
The ethics review board of the National Center for Health Statistics approved the study. The detailed information was provided on the NHANES website.
Consent to participate
Informed consent was obtained from all study participants. The detailed information was provided on the NHANES website.
Consent for publication
Not applicable.
Conflicts of interest
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, J., Tang, Y., Feng, Z. et al. Metabolic associated fatty liver disease and bone mineral density: a cross-sectional study of the National Health and Nutrition Examination Survey 2017–2018. Osteoporos Int 34, 713–724 (2023). https://doi.org/10.1007/s00198-023-06687-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-023-06687-w