Abstract
Summary
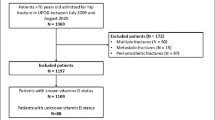
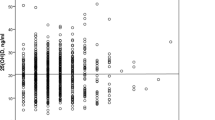
Low vitamin D in patients with hip fracture is common. In the present study, 407 of 872 (47%) patients had serum calcidiol less than 50 nmol/L. Patients with low vitamin D had more delirium, more new hip fractures, and more medical readmissions, but not more orthopedic complications after 1 year.
Introduction
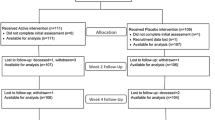
We wanted to study the relation between vitamin D level and postoperative orthopedic and medical complications in patients with hip fracture. In addition, we investigated the effect of giving a single-dose cholecalciferol 100.000 IU.
Methods
Data were taken from the local hip fracture register. Logistic regression analyses including vitamin D level and potentially confounding variables were performed for complications and readmissions.
Results
A total of 407 (47%) of 872 included hip fractures had low vitamin D at baseline. A total of 155 (18%) developed delirium, and the risk was higher in vitamin D-deficient patients (odds ratio (OR) 1.48, 95% confidence interval (CI) 1.04 to 2.12; p = 0.03). A total of 261 (30%) were readmitted for non-hip-related conditions. Low vitamin D was associated with a higher risk of medical readmissions within 30 days (OR 1.64 (1.03 to 2.61); p = 0.036) and 12 weeks (OR 1.47 (95% CI 1.02 to 2.12); p = 0.039). There was a higher risk of a new hip fracture (OR 2.84 (95% CI 1.15 to 7.03) p = 0.024) in vitamin D-deficient patients. A total of 105 (12%) developed at least one orthopedic complication, with no correlation to baseline vitamin D. Among vitamin D-deficient patients, those receiving a single-dose of 100.000 IU cholecalciferol had fewer orthopedic complications (OR 0.32 (95% CI 0.11 to 0.97) p = 0.044) the first 30 days after surgery.
Conclusion
Low vitamin D at admission for hip fracture increased the risk of delirium, a new hip fracture, and medical readmissions, but not orthopedic complications. The role of vitamin D supplementation to prevent orthopedic complications requires further study.

Similar content being viewed by others
Data availability
The database is available on request from the last author (ffrihagen@gmail.com).
References
Gullberg B, Johnell O, Kanis JA (1997) World-wide projections for hip fracture. Osteoporos Int 7(5):407–413. https://doi.org/10.1007/pl00004148
Omsland TK, Holvik K, Meyer HE, Center JR, Emaus N, Tell GS, Schei B, Tverdal A, Gjesdal CG, Grimnes G, Forsmo S, Eisman JA, Sogaard AJ (2012) Hip fractures in Norway 1999-2008: time trends in total incidence and second hip fracture rates: a NOREPOS study. Eur J Epidemiol 27(10):807–814. https://doi.org/10.1007/s10654-012-9711-9
Sogaard AJ, Holvik K, Meyer HE, Tell GS, Gjesdal CG, Emaus N, Grimnes G, Schei B, Forsmo S, Omsland TK (2016) Continued decline in hip fracture incidence in Norway: a NOREPOS study. Osteoporos Int 27(7):2217–2222. https://doi.org/10.1007/s00198-016-3516-8
Watne LO, Torbergsen AC, Conroy S, Engedal K, Frihagen F, Hjorthaug GA, Juliebo V, Raeder J, Saltvedt I, Skovlund E, Wyller TB (2014) The effect of a pre- and postoperative orthogeriatric service on cognitive function in patients with hip fracture: randomized controlled trial (Oslo Orthogeriatric Trial). BMC Med 12:63. https://doi.org/10.1186/1741-7015-12-63
Haentjens P, Magaziner J, Colon-Emeric CS, Vanderschueren D, Milisen K, Velkeniers B, Boonen S (2010) Meta-analysis: excess mortality after hip fracture among older women and men. Ann Intern Med 152(6):380–390. https://doi.org/10.7326/0003-4819-152-6-201003160-00008
Ali AM, Gibbons CE (2017) Predictors of 30-day hospital readmission after hip fracture: a systematic review. Injury 48(2):243–252. https://doi.org/10.1016/j.injury.2017.01.005
Vochteloo AJ, Moerman S, Tuinebreijer WE, Maier AB, de Vries MR, Bloem RM, Nelissen RG, Pilot P (2013) More than half of hip fracture patients do not regain mobility in the first postoperative year. Geriatr Gerontol Int 13(2):334–341. https://doi.org/10.1111/j.1447-0594.2012.00904.x
Teixeira A, Trinquart L, Raphael M, Bastianic T, Chatellier G, Holstein J (2009) Outcomes in older patients after surgical treatment for hip fracture: a new approach to characterise the link between readmissions and the surgical stay. Age Ageing 38(5):584–589. https://doi.org/10.1093/ageing/afp124
Sprague S, Petrisor B, Scott T, Devji T, Phillips M, Spurr H, Bhandari M, Slobogean GP (2016) What is the role of vitamin D supplementation in acute fracture patients? A systematic review and meta-analysis of the prevalence of hypovitaminosis D and supplementation efficacy. J Orthop Trauma 30(2):53–63. https://doi.org/10.1097/bot.0000000000000455
Torbergsen AC, Watne LO, Wyller TB, Frihagen F, Stromsoe K, Bohmer T, Mowe M (2015) Vitamin K1 and 25(OH)D are independently and synergistically associated with a risk for hip fracture in an elderly population: a case control study. Clin Nutr 34(1):101–106. https://doi.org/10.1016/j.clnu.2014.01.016
Binkley N, Coursin D, Krueger D, Iglar P, Heiner J, Illgen R, Squire M, Lappe J, Watson P, Hogan K (2017) Surgery alters parameters of vitamin D status and other laboratory results. Osteoporos Int 28(3):1013–1020. https://doi.org/10.1007/s00198-016-3819-9
Ettehad H, Mirbolook A, Mohammadi F, Mousavi M, Ebrahimi H, Shirangi A (2014) Changes in the serum level of vitamin d during healing of tibial and femoral shaft fractures. Trauma Mon 19(1):e10946. https://doi.org/10.5812/traumamon.10946
Fischer V, Haffner-Luntzer M, Amling M, Ignatius A (2018) Calcium and vitamin D in bone fracture healing and post-traumatic bone turnover. Eur Cell Mater 35:365–385. https://doi.org/10.22203/eCM.v035a25
Ray M (2019) Vitamin D and fracture healing: an ongoing puzzle. Int J of Orth 6(5):1050–1060. https://doi.org/10.17554/j.issn.2311-5106.2019.06.302
Lips P (2001) Vitamin D deficiency and secondary hyperparathyroidism in the elderly: consequences for bone loss and fractures and therapeutic implications. Endocr Rev 22(4):477–501. https://doi.org/10.1210/edrv.22.4.0437
Flicker L, Mead K, MacInnis RJ, Nowson C, Scherer S, Stein MS, Thomasx J, Hopper JL, Wark JD (2003) Serum vitamin D and falls in older women in residential care in Australia. J Am Geriatr Soc 51(11):1533–1538. https://doi.org/10.1046/j.1532-5415.2003.51510.x
Faulkner KA, Cauley JA, Zmuda JM, Landsittel DP, Newman AB, Studenski SA, Redfern MS, Ensrud KE, Fink HA, Lane NE, Nevitt MC (2006) Higher 1,25-dihydroxyvitamin D3 concentrations associated with lower fall rates in older community-dwelling women. Osteoporos Int 17(9):1318–1328. https://doi.org/10.1007/s00198-006-0071-8
Bischoff-Ferrari HA, Willett WC, Wong JB, Giovannucci E, Dietrich T, Dawson-Hughes B (2005) Fracture prevention with vitamin D supplementation: a meta-analysis of randomized controlled trials. JAMA 293(18):2257–2264. https://doi.org/10.1001/jama.293.18.2257
Bischoff-Ferrari HA, Dawson-Hughes B, Staehelin HB, Orav JE, Stuck AE, Theiler R, Wong JB, Egli A, Kiel DP, Henschkowski J (2009) Fall prevention with supplemental and active forms of vitamin D: a meta-analysis of randomised controlled trials. BMJ 339:b3692. https://doi.org/10.1136/bmj.b3692
Patton CM, Powell AP, Patel AA (2012) Vitamin D in orthopaedics. J Am Acad Orthop Surg 20(3):123–129. https://doi.org/10.5435/JAAOS-20-03-123
Dawson-Hughes B, Heaney RP, Holick MF, Lips P, Meunier PJ, Vieth R (2005) Estimates of optimal vitamin D status. Osteoporos Int 16(7):713–716. https://doi.org/10.1007/s00198-005-1867-7
Cashman KD, Dowling KG, Skrabakova Z, Kiely M, Lamberg-Allardt C, Durazo-Arvizu RA, Sempos CT, Koskinen S, Lundqvist A, Sundvall J, Linneberg A, Thuesen B, Husemoen LL, Meyer HE, Holvik K, Gronborg IM, Tetens I, Andersen R (2015) Standardizing serum 25-hydroxyvitamin D data from four Nordic population samples using the vitamin D standardization program protocols: shedding new light on vitamin D status in Nordic individuals. Scand J Clin Lab Invest 75(7):549–561. https://doi.org/10.3109/00365513.2015.1057898
Yao P, Bennett D, Mafham M, Lin X, Chen Z, Armitage J, Clarke R (2019) Vitamin D and calcium for the prevention of fracture: a systematic review and meta-analysis. JAMA Netw Open 2(12):e1917789. https://doi.org/10.1001/jamanetworkopen.2019.17789
Bolland MJ, Grey A, Avenell A (2018) Effects of vitamin D supplementation on musculoskeletal health: a systematic review, meta-analysis, and trial sequential analysis. Lancet Diabetes Endocrinol 6(11):847–858. https://doi.org/10.1016/S2213-8587(18)30265-1
Bolland MJ, Grey A (2014) A case study of discordant overlapping meta-analyses: vitamin d supplements and fracture. PLoS One 9(12):e115934. https://doi.org/10.1371/journal.pone.0115934
Bischoff-Ferrari HA, Dawson-Hughes B, Orav EJ, Staehelin HB, Meyer OW, Theiler R, Dick W, Willett WC, Egli A (2016) Monthly high-dose vitamin D treatment for the prevention of functional decline: a randomized clinical trial. JAMA Intern Med 176(2):175–183. https://doi.org/10.1001/jamainternmed.2015.7148
Bodendorfer BM, Cook JL, Robertson DS, Della Rocca GJ, Volgas DA, Stannard JP, Crist BD (2016) Do 25-hydroxyvitamin D levels correlate with fracture complications? J Orthop Trauma 30(9):e312–e317. https://doi.org/10.1097/BOT.0000000000000639
Haining SA, Atkins RM, Guilland-Cumming DF, Sharrard WJ, Russell RG, Kanis JA (1986) Vitamin D metabolites in patients with established non-union of fracture. Bone Miner 1(3):205–209
Boszczyk AM, Zakrzewski P, Pomianowski S (2013) Vitamin D concentration in patients with normal and impaired bone union. Pol Orthop Traumatol 78:1–3
Pourfeizi HH, Tabriz A, Elmi A, Aslani H (2013) Prevalence of vitamin D deficiency and secondary hyperparathyroidism in nonunion of traumatic fractures. Acta Med Iran 51(10):705–710
Brinker MR, O’Connor DP, Monla YT, Earthman TP (2007) Metabolic and endocrine abnormalities in patients with nonunions. J Orthop Trauma 21(8):557–570. https://doi.org/10.1097/BOT.0b013e31814d4dc6
Ravindra VM, Godzik J, Dailey AT, Schmidt MH, Bisson EF, Hood RS, Cutler A, Ray WZ (2015) Vitamin D levels and 1-year fusion outcomes in elective spine surgery: a prospective observational study. Spine (Phila Pa 1976) 40(19):1536–1541. https://doi.org/10.1097/BRS.0000000000001041
Gorter EA, Hamdy NA, Appelman-Dijkstra NM, Schipper IB (2014) The role of vitamin D in human fracture healing: a systematic review of the literature. Bone 64:288–297. https://doi.org/10.1016/j.bone.2014.04.026
Fakler JK, Grafe A, Dinger J, Josten C, Aust G (2016) Perioperative risk factors in patients with a femoral neck fracture - influence of 25-hydroxyvitamin D and C-reactive protein on postoperative medical complications and 1-year mortality. BMC Musculoskelet Disord 17:51. https://doi.org/10.1186/s12891-016-0906-1
Kroner Jde C, Sommer A, Fabri M (2015) Vitamin D every day to keep the infection away? Nutrients 7(6):4170–4188. https://doi.org/10.3390/nu7064170
Miller RR, Cappola AR, Shardell MD, Hawkes WG, Yu-Yahiro JA, Hebel JR, Magaziner J (2006) Persistent changes in interleukin-6 and lower extremity function following hip fracture. J Gerontol A Biol Sci Med Sci 61(10):1053–1058. https://doi.org/10.1093/gerona/61.10.1053
Torbergsen AC, Watne LO, Frihagen F, Wyller TB, Brugaard A, Mowe M (2015) Vitamin deficiency as a risk factor for delirium. Eur Geriatr Med 6(4):314–318. https://doi.org/10.1016/j.eurger.2014.09.002
Annweiler C, Montero-Odasso M, Llewellyn DJ, Richard-Devantoy S, Duque G, Beauchet O (2013) Meta-analysis of memory and executive dysfunctions in relation to vitamin D. J Alzheimers Dis 37(1):147–171. https://doi.org/10.3233/JAD-130452
MacLullich AMJ, Ferguson KJ, Miller T, de Rooij SEJA, Cunningham C (2008) Unravelling the pathophysiology of delirium: a focus on the role of aberrant stress responses. J Psychosom Res 65(3):229–238. https://doi.org/10.1016/j.jpsychores.2008.05.019
Khademvatani K, Seyyed-Mohammadzad MH, Akbari M, Rezaei Y, Eskandari R, Rostamzadeh A (2014) The relationship between vitamin D status and idiopathic lower-extremity deep vein thrombosis. Int J Gen Med 7:303–309. https://doi.org/10.2147/IJGM.S64812
Koyama T, Shibakura M, Ohsawa M, Kamiyama R, Hirosawa S (1998) Anticoagulant effects of 1alpha,25-dihydroxyvitamin D3 on human myelogenous leukemia cells and monocytes. Blood 92(1):160–167
Hansen J-B, Jorde R, Svartberg J, Brox J, Vik A, Brækkan SK, Grimnes G, Lerstad G, Brodin EE (2017) Serum levels of vitamin D are not associated with future risk of venous thromboembolism. Thromb Haemost 109(05):885–890. https://doi.org/10.1160/th12-10-0728
Vuckovic BA, van Rein N, Cannegieter SC, Rosendaal FR, Lijfering WM (2015) Vitamin supplementation on the risk of venous thrombosis: results from the MEGA case-control study. Am J Clin Nutr 101(3):606–612. https://doi.org/10.3945/ajcn.114.095398
Kearns MD, Alvarez JA, Tangpricha V (2014) Large, single-dose, oral vitamin D supplementation in adult populations: a systematic review. Endocr Pract 20(4):341–351. https://doi.org/10.4158/EP13265.RA
Autier P, Boniol M, Pizot C, Mullie P (2014) Vitamin D status and ill health: a systematic review. Lancet Diabetes Endocrinol 2(1):76–89. https://doi.org/10.1016/S2213-8587(13)70165-7
Acknowledgments
Elise Berg Vesterhus, Oslo University Hospital, for database maintenance.
Funding
Oslo University Hospital.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Ethics approval
The hip fracture register and data collection were approved by the Hospital Data Protection Officer (2014/12309) and Regional Ethics Committee South Eastern Norway (2014/1433).
Consent to participate
Preapproved waiver for quality audit Hospital Data Protection Officer (PVO 2014/12309, PVO 2015/18831, and PVO 2020/11011) and Regional Ethics Committee South Eastern Norway (2014/1433).
Consent for publication
Preapproved waiver for quality audit Hospital Data Protection Officer (PVO 2014/12309, PVO 2015/18831, and PVO 2020/11011) and Regional Ethics Committee South Eastern Norway (2014/1433).
Code availability
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ingstad, F., Solberg, L.B., Nordsletten, L. et al. Vitamin D status and complications, readmissions, and mortality after hip fracture. Osteoporos Int 32, 873–881 (2021). https://doi.org/10.1007/s00198-020-05739-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-020-05739-9