Abstract
Summary
Caution is necessary when using symptom or physical examination findings to localize the osteoporotic vertebral fractures (VFs) attributable to the discrepant colocalized relationship.
Introduction
Whether the location of symptoms or physical examination findings delineates the appropriate spinal range for imaging has not been thoroughly investigated for VFs. The present study aims to analyze the consistency between the fractural vertebrae location and the location suggested by patient-reported pain or physical examination findings.
Methods
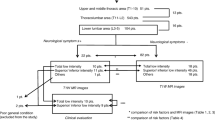
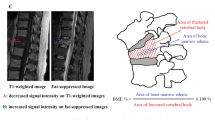
This observational study, following a prospective design, enrolled 358 patients with VFs. The locations of two symptoms (patient-reported back pain [P-RBP], radiating pain [RP]) and findings from two physical examinations (spinal palpation tenderness [SPT], axial spinal percussion pain [ASPP]) were used to locate the VF segments identified using whole-spine magnetic resonance imaging (MRI). The percentage of agreements and kappa coefficient were calculated.
Results
In 20.7% (74/358), the P-RBP site and VF segments were in the same location (kappa = 0.153); 21.2% (76/358) presented with concomitant RP in 93.4% (71/76) of whom the RP dermatome was colocalized with the VF segments (kappa = 0.924); 55.0% (197/358) and 23.2% (83/358) of patients presented with positive SPT and ASPP, respectively; and in 49.2% (97/197) and 96.4% (80/83) of patients with positive SPT (kappa = 0.435) and ASPP (kappa = 0.963), the positive finding and the VF segments were consistently colocalized.
Conclusions
The positive finding of RP or ASPP is useful in determining the spinal range for imaging tests, while an MRI scan covering the whole thoracic and lumbar spine is necessary in VF-suspected patients with P-RBP or positive SPT, indicating that caution is necessary when using symptoms or physical examination findings to localize VFs.


Similar content being viewed by others
References
Schousboe JT (2016) Epidemiology of vertebral fractures. J Clin Densitom 19:8–22
Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A (2007) Incidence and economic burden of osteoporosis-related fractures in the United States, 2005-2025. J Bone Miner Res 22:465–475
Center JR, Nguyen TV, Schneider D, Sambrook PN, Eisman JA (1999) Mortality after all major types of osteoporotic fracture in men and women: an observational study. Lancet 353:878–882
Fink HA, Ensrud KE, Nelson DB, Kerani RP, Schreiner PJ, Zhao Y, Cummings SR, Nevitt MC (2003) Disability after clinical fracture in postmenopausal women with low bone density: the fracture intervention trial (FIT). Osteoporos Int 14:69–76
Kanis JA, Johnell O, De Laet C, Johansson H, Oden A, Delmas P, Eisman J, Fujiwara S, Garnero P, Kroger H, McCloskey EV, Mellstrom D, Melton LJ, Pols H, Reeve J, Silman A, Tenenhouse A (2004) A meta-analysis of previous fracture and subsequent fracture risk. Bone 35:375–382
Siris ES, Genant HK, Laster AJ, Chen P, Misurski DA, Krege JH (2007) Enhanced prediction of fracture risk combining vertebral fracture status and BMD. Osteoporos Int 18:761–770
Delmas PD, van de Langerijt L, Watts NB, Eastell R, Genant H, Grauer A, Cahall DL, IMPACT Study Group (2005) Underdiagnosis of vertebral fractures is a worldwide problem: the IMPACT study. J Bone Miner Res 20:557–563
Marongiu G, Congia S, Verona M, Lombardo M, Podda D, Capone A (2018) The impact of magnetic resonance imaging in the diagnostic and classification process of osteoporotic vertebral fractures. Injury 49(Suppl 3):S26–26S31
Bougioukli S, Κollia P, Koromila T, Varitimidis S, Hantes M, Karachalios T, Malizos ΚΝ, Dailiana ZH (2019) Failure in diagnosis and under-treatment of osteoporosis in elderly patients with fragility fractures. J Bone Miner Metab 37:327–335
Friedrich M, Gittler G, Pieler-Bruha E (2006) Misleading history of pain location in 51 patients with osteoporotic vertebral fractures. Eur Spine J 15:1797–1800
Niu J, Song D, Gan M, Liu B, Tan C, Yang H, Meng B (2018) Percutaneous kyphoplasty for the treatment of distal lumbosacral pain caused by osteoporotic thoracolumbar vertebral fracture. Acta Radiol 59:1351–1357
Gaughen JR Jr, Jensen ME, Schweickert PA, Kaufmann TJ, Marx WF, Kallmes DF (2002) Lack of preoperative spinous process tenderness does not affect clinical success of percutaneous vertebroplasty. J Vasc Interv Radiol 13:1135–1138
Rad AE, Kallmes DF (2008) Pain relief following vertebroplasty in patients with and without localizing tenderness on palpation. AJNR Am J Neuroradiol 29:1622–1626
Lenski M, Büser N, Scherer M (2017) Concomitant and previous osteoporotic vertebral fractures. Acta Orthop 88:192–197
Takahashi S, Hoshino M, Takayama K, Iseki K, Sasaoka R, Tsujio T, Yasuda H, Sasaki T, Kanematsu F, Kono H, Toyoda H, Nakamura H (2017) Time course of osteoporotic vertebral fractures by magnetic resonance imaging using a simple classification: a multicenter prospective cohort study. Osteoporos Int 28:473–482
Park SY, Lee SH, Suh SW, Park JH, Kim TG (2013) Usefulness of MRI in determining the appropriate level of cement augmentation for acute osteoporotic vertebral compression fractures. J Spinal Disord Tech 26:E80–E85
Harlick JC, Milosavljevic S, Milburn PD (2007) Palpation identification of spinous processes in the lumbar spine. Man Ther 12:56–62
Beynon AM, Hebert JJ, Walker BF (2018) The interrater reliability of static palpation of the thoracic spine for eliciting tenderness and stiffness to test for a manipulable lesion. Chiropr Man Therap 26:49
Schneider M, Erhard R, Brach J, Tellin W, Imbarlina F, Delitto A (2008) Spinal palpation for lumbar segmental mobility and pain provocation: an interexaminer reliability study. J Manip Physiol Ther 31:465–473
Christensen HW, Vach W, Vach K, Manniche C, Haghfelt T, Hartvigsen L, Høilund-Carlsen PF (2002) Palpation of the upper thoracic spine: an observer reliability study. J Manip Physiol Ther 25:285–292
Inaba K, DuBose JJ, Barmparas G, Barbarino R, Reddy S, Talving P, Lam L, Demetriades D (2011) Clinical examination is insufficient to rule out thoracolumbar spine injuries. J Trauma 70:174–179
Shahrami A, Shojaee M, Tabatabaee SM, Mianehsaz E (2016) Diagnostic value of clinical findings in evaluation of thoracolumbar blunt traumas. Emerg (Tehran) 4:127–131
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Jin H, Ma X, Liu Y, Yin X, Zhu J, Wang Z, Fan W, Jin Y, Pu J, Zhao J, Liu M, Liu P (2020) Back pain-inducing test, a novel and sensitive screening test for painful osteoporotic vertebral fractures: a prospective clinical study. J Bone Miner Res 35(3):488–497
Patel U, Skingle S, Campbell GA, Crisp AJ, Boyle IT (1991) Clinical profile of acute vertebral compression fractures in osteoporosis. Br J Rheumatol 30:418–421
Doo TH, Shin DA, Kim HI, Shin DG, Kim HJ, Chung JH, Lee JO (2008) Clinical relevance of pain patterns in osteoporotic vertebral compression fractures. J Korean Med Sci 23:1005–1010
Hatgis J, Granville M, Jacobson RE (2017) Delayed recognition of thoracic and lumbar vertebral compression fractures in minor accident cases. Cureus 9:e1050
Gibson JE, Pilgram TK, Gilula LA (2006) Response of nonmidline pain to percutaneous vertebroplasty. AJR Am J Roentgenol 187:869–872
Eloqayli H (2018) Clinical decision-making in chronic spine pain: dilemma of image-based diagnosis of degenerative spine and generation mechanisms for nociceptive, radicular, and referred pain. Biomed Res Int 2018:8793843
Jinkins JR, Whittemore AR, Bradley WG (1989) The anatomic basis of vertebrogenic pain and the autonomic syndrome associated with lumbar disk extrusion. AJR Am J Roentgenol 152:1277–1289
Maigne R (1980) Low back pain of thoracolumbar origin. Arch Phys Med Rehabil 61:389–395
Thakur M, Dickenson AH, Baron R (2014) Osteoarthritis pain: nociceptive or neuropathic. Nat Rev Rheumatol 10:374–380
Waddell G, Main CJ, Morris EW, Venner RM, Rae PS, Sharmy SH, Galloway H (1982) Normality and reliability in the clinical assessment of backache. Br Med J (Clin Res Ed) 284:1519–1523
Schofield P (2018) The assessment of pain in older people: UK National Guidelines. Age Ageing 47:i1–1i22
McHugh ML (2012) Interrater reliability: the kappa statistic. Biochem Med (Zagreb) 22:276–282
Acknowledgments
We thank Dr. Hui Lin (Department of Gastroenterology, Xinqiao Hospital, Army Medical University, Chongqing, China) for reviewing the statistical analysis and interpretation of the results. We thank Dr. Chunyan Lu (Department of Endocrinology, Huaxi Hospital, Sichuan University, Chengdu, China) for the help in drafting the manuscript. We would like to thank all the professors and staffs (Department of Radiology, Daping Hospital, Chongqing, China) for their tremendous efforts in performing imaging examinations. Last but not the least, we acknowledge the study participants for their cooperation throughout the whole study procedure.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Written informed consent was obtained from each participant. The Human Ethics Committee of the Third Affiliated Hospital of Army Medical University approved the study procedures and consent form (approval number 2016-16).
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Huaijian Jin and Xiaoyuan Ma are the first author
Electronic supplementary material
ESM 1
(DOCX 21 kb)
Rights and permissions
About this article
Cite this article
Jin, H., Ma, X., Liu, Y. et al. Back pain from painful osteoporotic vertebral fractures: discrepancy between the actual fracture location and the location suggested by patient-reported pain or physical examination findings. Osteoporos Int 31, 1721–1732 (2020). https://doi.org/10.1007/s00198-020-05434-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-020-05434-9