Abstract
Summary
This study compares four screening tools in their ability to predict osteoporosis. We found that there was no significant difference between the tools. These results provide support for the use of automated screening tools which work in conjunction with the electronic medical record and help improve screening rates for osteoporosis.
Introduction
The purpose of this study is to compare the performance of four fracture risk assessment tools (FRATs) in identifying osteoporosis by bone mineral density (BMD) T-score: Veterans Affairs Fracture Absolute Risk Assessment Tool (VA-FARA), World Health Organization’s Fracture Risk Assessment Tool (FRAX), electronic FRAX (e-FRAX), and Osteoporosis Self-Assessment Screening Tool (OST).
Methods
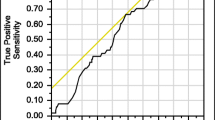
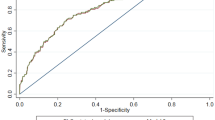
We performed a cross-sectional analysis of all patients enrolled in the VA Salt Lake City bone health team (BHT) who had completed a DXA scan between February 1, 2012, and February 1, 2013. DXA scan results were obtained by chart abstraction. For calculation of FRAX, osteoporosis risk factors were obtained from a screening questionnaire completed prior to DXA. For VA-FARA and e-FRAX, risk factors were derived from the electronic medical record (EMR). Clinical risk scores were calculated and compared against the gold standard of DXA-based osteoporosis. Sensitivity, specificity, and predictive values were calculated. Receiver operator characteristic (ROC) curves were plotted, and areas under the curve (AUC) were compared.
Results
A cohort of 463 patients met eligibility criteria (mean age 80.4 years). One hundred twelve patients (24%) had osteoporosis as defined by DXA T-score ≤−2.5. Sensitivity, specificity, and predictive values were calculated. ROC statistics were compared and did not reach statistical significance difference between FRATs in identifying DXA-based osteoporosis.
Conclusions
Our study suggests that all FRATs tested perform similarly in identifying osteoporosis among elderly, primarily Caucasian, male veterans. If these electronic screening methods perform similarly for fracture outcomes, they could replace manual FRAX and thus improve efficiency in identifying individuals who should be sent for DXA scan.


Similar content being viewed by others
References
Black DM, Rosen CJ (2016) Postmenopausal Osteoporosis. N Engl J Med 374(21):2096–2097. doi:10.1056/NEJMc1602599
Singer A, Exuzides A, Spangler L, O'Malley C, Colby C, Johnston K, Agodoa I, Baker J, Kagan R (2015) Burden of illness for osteoporotic fractures compared with other serious diseases among postmenopausal women in the United States. Mayo Clin Proc 90(1):53–62. doi:10.1016/j.mayocp.2014.09.011
Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A (2007) Incidence and economic burden of osteoporosis-related fractures in the United States, 2005–2025. J Bone Miner Res 22(3):465–475. doi:10.1359/jbmr.061113
Lems WF (2015) Fracture risk estimation may facilitate the treatment gap in osteoporosis. Ann Rheum Dis 74(11):1943–1945. doi:10.1136/annrheumdis-2015-208245
Willson T, Nelson SD, Newbold J, Nelson RE, LaFleur J (2015) The clinical epidemiology of male osteoporosis: a review of the recent literature. Clin Epidemiol 7:65–76. doi:10.2147/CLEP.S40966
Lim SY, Lim JH, Nguyen D, Okamura R, Amiri HM, Calmes M, Nugent K (2013) Screening for osteoporosis in men aged 70 years and older in a primary care setting in the United States. Am J Mens Health 7(4):350–354. doi:10.1177/1557988313478826
Feldstein AC, Nichols G, Orwoll E, Elmer PJ, Smith DH, Herson M, Aickin M (2005) The near absence of osteoporosis treatment in older men with fractures. Osteoporos Int 16(8):953–962. doi:10.1007/s00198-005-1950-0
Report of the Office of the Inspector General: management of Osteoporosis in veterans with fractures (2010) Washington
FRAX. www.shef.ac.uk/frax/
LaFleur J, Nelson RE, Yao Y, Adler RA, Nebeker JR (2012) Validated risk rule using computerized data to identify males at high risk for fracture. Osteoporos Int 23(3):1017–1027. doi:10.1007/s00198-011-1646-6
LaFleur J, Steenhoek CL, Horne J, Meier J, Nebeker JR, Mambourg S, Swislocki A, Carmichael J (2015) Comparing fracture absolute risk assessment (FARA) tools: an osteoporosis clinical informatics tool to improve identification and care of men at high risk of first fracture. Ann Pharmacother 49(5):506–514. doi:10.1177/1060028015572819
Lawrence PT, Grotzke MP, Rosenblum Y, Nelson RE, LaFleur J, Miller KL, Ma J, Cannon GW (2017) The bone health team. J prim care community health 2150131916687888. doi:10.1177/2150131916687888
Hajian-Tilaki K (2014) Sample size estimation in diagnostic test studies of biomedical informatics. J Biomed Inform 48:193–204. doi:10.1016/j.jbi.2014.02.013
Report of a WHO study group (1994) Assessment of fracture risk and its application to screening for postmenopausal osteoporosis. World Health Organ Tech Rep Ser 843:1–129
Pepe M, Longton G, Janes H (2009) Estimation and comparison of receiver operating characteristic curves. Stata J 9(1):1
Bamber D (1975) The area above the ordinal dominance graph and the area below the receiver operating characteristic graph. J Math Psychol 12:287–415
Hanley JA, McNeil BJ (1982) The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology 143:29–36
Cosman F, de Beur SJ, LeBoff MS, Lewiecki EM, Tanner B, Randall S, Lindsay R, National Osteoporosis F (2014) Clinician’s guide to prevention and treatment of osteoporosis. Osteoporos Int 25(10):2359–2381. doi:10.1007/s00198-014-2794-2
Force USPST (2011) Screening for osteoporosis: U.S. preventive services task force recommendation statement. Ann Intern Med 154(5):356–364. doi:10.7326/0003-4819-154-5-201103010-00307
Watts NB, Adler RA, Bilezikian JP, Drake MT, Eastell R, Orwoll ES, Finkelstein JS, Endocrine S (2012) Osteoporosis in men: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 97(6):1802–1822. doi:10.1210/jc.2011-3045
Pang WY, Inderjeeth CA (2014) FRAX without bone mineral density versus osteoporosis self-assessment screening tool as predictors of osteoporosis in primary screening of individuals aged 70 and older. J Am Geriatr Soc 62(3):442–446. doi:10.1111/jgs.12696
Nayak S, Edwards DL, Saleh AA, Greenspan SL (2015) Systematic review and meta-analysis of the performance of clinical risk assessment instruments for screening for osteoporosis or low bone density. Osteoporos Int 26(5):1543–1554. doi:10.1007/s00198-015-3025-1
Marques A, Ferreira RJ, Santos E, Loza E, Carmona L, da Silva JA (2015) The accuracy of osteoporotic fracture risk prediction tools: a systematic review and meta-analysis. Ann Rheum Dis 74(11):1958–1967. doi:10.1136/annrheumdis-2015-207907
Rubin KH, Friis-Holmberg T, Hermann AP, Abrahamsen B, Brixen K (2013) Risk assessment tools to identify women with increased risk of osteoporotic fracture: complexity or simplicity? A systematic review. J Bone Miner Res 28(8):1701–1717. doi:10.1002/jbmr.1956
Rud B, Hilden J, Hyldstrup L, Hrobjartsson A (2009) The osteoporosis self-assessment tool versus alternative tests for selecting postmenopausal women for bone mineral density assessment: a comparative systematic review of accuracy. Osteoporos Int 20(4):599–607. doi:10.1007/s00198-008-0713-0
Steuart Richards J, Lazzari AA, Teves Qualler DA, Desale S, Howard R, Kerr GS (2014) Validation of the osteoporosis self-assessment tool in US male veterans. J Clin Densitom 17(1):32–37. doi:10.1016/j.jocd.2013.02.004
Nayak S, Greenspan SL (2016) Cost-effectiveness of osteoporosis screening strategies for men. J Bone Miner Res 31(6):1189–1199. doi:10.1002/jbmr.2784
Acknowledgements
This material is based on work supported by Specialty Care Center of Innovation, Veterans Health Administration, Department of Veterans Affairs and Office of Research and Development, and Health Services Research and Development Service (grants CDA 11-210 and I50HX001240).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Williams, S.T., Lawrence, P.T., Miller, K.L. et al. A comparison of electronic and manual fracture risk assessment tools in screening elderly male US veterans at risk for osteoporosis. Osteoporos Int 28, 3107–3111 (2017). https://doi.org/10.1007/s00198-017-4172-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-017-4172-3