Abstract
Introduction
Vitamin K has been implicated in increased bone fracture risk. Despite a potential role of vitamin K in bone, little is known about the effects of altered dietary phylloquinone intake on the underlying components of bone and mineral metabolism.
Methods
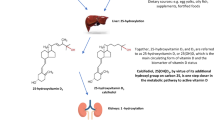
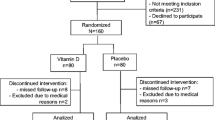
A 84-day in-house dietary phylloquinone (vitamin K) depletion–repletion study was undertaken in 21 postmenopausal women (mean age: 70 years) to assess the effects of altered vitamin K status on intestinal calcium (Ca) absorption, urinary and serum Ca and phosphorus (P), serum calcemic hormones, and serum biomarkers of bone turnover [osteocalcin and N-telopeptide type 1 collagen cross-links (NTx)] and the response to 1,25-dihydroxyvitamin D treatment (1 μg/day×7 d).
Results
The group receiving calcitriol treatment (n=11) had higher Ca absorption, urinary Ca, urinary and serum P and serum osteocalcin and lower serum parathyroid hormone (PTH).There were no significant effects of acute (4-week) phylloquinone depletion on response to 1,25-dihydroxyvitamin D treatment or on measures of bone formation or mineral metabolism. However, phylloquinone treatment had a significant effect (p<0.04) on serum NTx. Phylloquinone repletion, up to five times (450 μg phylloquinone per day) the currently recommended adequate intake level of dietary phylloquinone for women, significantly reduced serum NTx (16.8±0.9 nmol bone collagen equivalents (BCE) per liter following repletion vs 18.4±1.1 nmol BCE per liter following depletion; p< 0.01).
Conclusions
These findings suggest that altering vitamin K status in postmenopausal women by manipulating phylloquinone intake does not have an acute affect on intestinal Ca absorption, renal mineral excretion, or bone formation, but high phylloquinone intake may modestly reduce bone resorption. The impact of high phylloquinone intake on bone mineral density and fracture risk needs to be ascertained in randomized clinical trials.

Similar content being viewed by others
References
Szulc P, Arlot M, Chapuy MC, Duboeuf F, Meunier PJ, Delmas PD (1994) Serum undercarboxylated osteocalcin correlates with hip bone mineral density in elderly women. J Bone Min Res 9:1591–1595
Feskanich D, Weber P, Willett WC, Rockett H, Booth SL, Colditz GA (1999) Vitamin K intake and hip fractures in women: a prospective study. Am J Clin Nutr 69:74–79
Szulc P, Chapuy MC, Meunier PJ, Delmas PD (1993) Serum undercarboxylated osteocalcin is a marker of the risk of hip fracture in elderly women. J Clin Invest 91:1769–1774
Weber P (2001) Vitamin K and bone health. Nutrition 17:880–887
Berkner KL (2000) The vitamin K-dependent carboxylase. J Nutr 130:1877–1880
Suttie JW (1985) Vitamin K-dependent carboxylase. Annu Rev Biochem 54:459–477
Binkley NC, Suttie JW (1995) Vitamin K nutrition and osteoporosis. J Nutr 125:1812–1821
Price PA (1989) Gla-containing proteins of bone. Connect Tissue Res 21:51–57 (discussion 57–60)
Furie BC, Furie B (1997) Structure and mechanism of action of the vitamin K-dependent gamma- glutamyl carboxylase: recent advances from mutagenesis studies. Thromb Haemost 78:595–598
Jie KG, Bots ML, Vermeer C, Witteman JC, Grobbee DE (1996) Vitamin K status and bone mass in women with and without aortic atherosclerosis: a population-based study. Calcif Tissue Int 59:352–356
Vergnaud P, Garnero P, Meunier PJ, Breart G, Kamihagi K, Delmas PD (1997) Undercarboxylated osteocalcin measured with a specific immunoassay predicts hip fracture in elderly women: the EPIDOS Study. J Clin Endocrinol Metab 82:719–724
Dietary reference intakes for vitamin A, vitamin K, arsenic, boron, chromium, copper, iodine, iron, manganese, molybdenum, nickel, silicon, vanadium, and zinc. National Academy Press. Washington DC (2001) Standing committee on the scientific evaluation of dietary reference intakes, food and nutrition board, institute of medicine
Sokoll LJ, Sadowski JA (1996) Comparison of biochemical indexes for assessing vitamin K nutritional status in a healthy adult population. Am J Clin Nutr 63:566–573
Binkley NC, Krueger DC, Engelke JA, Foley AL, Suttie JW (2000) Vitamin K supplementation reduces serum concentrations of under-{gamma}-carboxylated osteocalcin in healthy young and elderly adults. Am J Clin Nutr 72:1523–1528
Braam LA, Knapen MH, Geusens P, Brouns F, Hamulyak K, Gerichhausen MJ, Vermeer C (2003) Vitamin K1 supplementation retards bone loss in postmenopausal women between 50 and 60 years of age. Calcif Tissue Int 73:21–26
Sergeev IN, Norman AW (1992) Vitamin K-dependent gamma-carboxylation of the 1,25-dihydroxyvitamin D3 receptor. Biochem Biophys Res Commun 189:1543–1547
Knapen MH, Hamulyak K, Vermeer C (1989) The effect of vitamin K supplementation on circulating osteocalcin (bone Gla protein) and urinary calcium excretion. Ann Intern Med 111:1001–1005
Kalkwarf HJ, Khoury JC, Bean J, Elliot JG (2004) Vitamin K, bone turnover, and bone mass in girls. Am J Clin Nutr 80:1075–1080
Booth SL, Lichtenstein AH, O’Brien-Morse M, McKeown NM, Wood RJ, Saltzman E, Gundberg CM (2001) Effects of a hydrogenated form of vitamin K on bone formation and resorption. Am J Clin Nutr 74:783–790
Ferland G, Sadowski JA, O’Brien ME (1993) Dietary induced subclinical vitamin K deficiency in normal human subjects. J Clin Invest 91:1761–1768
Booth SL, Martini L, Peterson JW, Saltzman E, Dallal GE, Wood RJ (2003) Dietary phylloquinone depletion and repletion in older women. J Nutr 133:2565–2569
Dietary reference intakes for calcium, phosphorus, magnesium, vitamin D, and fluoride. National Academy Press (1997) Standing committee on the scientific evaluation of dietary reference intakes, institute of medicine, food and nutrition board. Washington DC
Blumsohn A, Morris B, Eastell R (1994) Stable strontium absorption as a measure of intestinal calcium absorption: comparison with the double-radiotracer calcium absorption test. Clin Sci (Colch) 87:363–368
Dijkgraaf-Ten Bolscher M, Netelenbos JC, Barto R, van Der Vijgh WJ (2000) Strontium as a marker for intestinal calcium absorption: the stimulatory effect of calcitriol. Clin Chem 46:248–251
Gundberg CM, Nieman SD, Abrams S, Rosen H (1998) Vitamin K status and bone health: an analysis of methods for determination of undercarboxylated osteocalcin. J Clin Endocrinol Metab 83:3258–3266
Gundberg CM, Hauschka PV, Lian JB, Gallop PM (1984) Osteocalcin: isolation, characterization, and detection. Methods Enzymol 107:516–544
Khosla S, Kleerekoper M (2003) Biochemical markers of bone turnover. In: Favus M (ed) Primer on the metabolic bone diseases and disorders of mineral metabolism. American Society of Bone and Mineral Research, Washington DC, pp 166–172
Duda RJ Jr, Kumar R, Nelson KI, Zinsmeister AR, Mann KG, Riggs BL (1987) 1,25-Dihydroxyvitamin D stimulation test for osteoblast function in normal and osteoporotic postmenopausal women. J Clin Invest 79:1249–1253
Ervin RB, Wang CY, Wright JD, Kennedy-Stephenson J (2004) Dietary intake of selected minerals for the United States population: 1999–2000. Adv Data 1–5
Norman AW (1990) Intestinal calcium absorption: a vitamin D-hormone-mediated adaptive response. Am J Clin Nutr 51:290–300
Acknowledgements
The authors wish to thank the staff of the Nutrition Evaluation Laboratory and the Metabolic Research Unit of the Jean Mayer USDA-HNRCA and the volunteer subjects for their contribution to the study. This work was supported by the U.S. Department of Agriculture, under Cooperative Agreement no. 58-1950-9-001, and by the Cooperative State Research, Education, and Extension Service under agreement No 99-35200-7583 (RJW). LM was supported in part by a postdoctoral fellowship grant from FAPESP-Brazil, under agreement no. 98/6151-9. MRDO was under a research fellowship from CNPq-Brazil no. 300318/97-9. Any options, findings, conclusion, or recommendations expressed in this publication are those of the authors and do not necessarily reflect the view of the U.S. Department of Agriculture.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Martini, L.A., Booth, S.L., Saltzman, E. et al. Dietary phylloquinone depletion and repletion in postmenopausal women: effects on bone and mineral metabolism. Osteoporos Int 17, 929–935 (2006). https://doi.org/10.1007/s00198-006-0086-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-006-0086-1