Abstract
Introduction and hypothesis
To perform a cost-effectiveness analysis of concurrent posterior repair performed at the time of laparoscopic hysterectomy with sacrocolpopexy over a 7-year time period. We hypothesize it is not cost-effective to perform a posterior colporrhaphy.
Methods
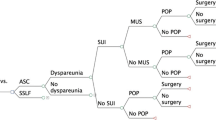
We used TreeAge Pro® to construct a decision model with Markov modeling to compare sacrocolpopexy with and without concurrent posterior repair (SCP and SCP+PR) over a time horizon of 7 years. Outcomes included probability and costs associated with prolapse recurrence, prolapse retreatment, and complications including rectal injury, rectovaginal hematoma requiring reoperation, and postoperative dyspareunia. Cost-effectiveness was defined as an incremental cost-effectiveness ratio (ICER) calculated as ∆ costs /∆ effectiveness and the willingness to pay (WTP) was set at $100,000/QALY.
Results
Our model showed that SCP was the dominant strategy, with lower costs (−$ 2681.06) and higher effectiveness (+0.10) compared to SCP+PR over the 7-year period. In two-way sensitivity analyses, we varied the probability of prolapse recurrence after both strategies. Our conclusions would only change if the probability of recurrence after SCP was at least 29.7% higher than after SCP+PR. When varying the probabilities of dyspareunia for both strategies, SCP+PR only became the dominant strategy if the probability of dyspareunia for SCP+PR was lower than the rate of SCP alone.
Conclusions
In this 7-year Markov cost-effectiveness analysis, SCP without concurrent PR was the dominant strategy. SCP+PR costs more with lower effectiveness than SCP alone, due to higher surgical cost of SCP+PR and higher probability of dyspareunia after SCP+PR.

Similar content being viewed by others
References
Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J. Surgery for women with apical vaginal prolapse. Cochrane Database Syst Rev. 2016;10:CD012376. https://doi.org/10.1002/14651858.CD012376.
Chang OH, Davidson ERW, Thomas TN, Paraiso MFR, Ferrando CA. Predictors for pelvic organ prolapse recurrence after sacrocolpopexy. Female Pelvic Med Reconstructive Surg. 2020;27(1):e165–70. https://doi.org/10.1097/spv.0000000000000874.
Komesu YM, Rogers RG, Kammerer-Doak DN, Barber MD, Olsen AL. Posterior repair and sexual function. Am J Obstet Gynecol. 2007;197:101.e1–e6. https://doi.org/10.1016/j.ajog.2007.03.054.
Kahn MA, Stanton SL. Posterior colporrhaphy: its effects on bowel and sexual function. Br J Obstet Gynaecol. 1997;104:82–6.
Handa VL, Zyczynski HM, Brubaker L, Nygaard I, Janz NK, Richter HE, et al. Sexual function before and after sacrocolpopexy for pelvic organ prolapse. Am J Obstet Gynecol. 2007;197:629.e1–6. https://doi.org/10.1016/j.ajog.2007.08.016.
Paraiso MFR, Barber MD, Muir TW, Walters MD. Rectocele repair: a randomized trial of three surgical techniques including graft augmentation. Am J Obstet Gynecol. 2006;195:1762–71. https://doi.org/10.1016/j.ajog.2006.07.026.
Weber AM, Walters MD, Piedmonte MR. Sexual function and vaginal anatomy in women before and after surgery for pelvic organ prolapse and urinary incontinence. Am J Obstet Gynecol. 2000;182(6):1610–5. https://doi.org/10.1067/mob.2000.107436.
Cundiff GW, Weidner AC, Visco AG, Addison WA, Bump RC, Ballard L. An anatomic and functional assessment of the discrete defect rectocele repair. Am J Obst Gynecol. 1998;179(6):1451–7. https://doi.org/10.1016/S0002-9378(98)70009-2.
Sung VW, Rardin CR, Raker CA, Lasala CA, Myers DL. Porcine subintestinal submucosal graft augmentation for rectocele repair: a randomized controlled trial. Obstet Gynecol. 2012;119:125–33. https://doi.org/10.1097/AOG.0b013e31823d407e.
Chang OH, Shepherd JP, St Martin B, Sokol ER, Wallace S. Surgical correction of the genital hiatus at the time of sacrocolpopexy—are concurrent posterior repairs cost-effective? Female Pelvic Med Reconstruc Surg. 2022;28(5):325–31. https://doi.org/10.1097/SPV.0000000000001130.
Antosh DD, Kim-Fine S, Meriwether KV, Kanter G, Dieter AA, Mamik MM, et al. Changes in sexual activity and function after pelvic organ prolapse surgery: a systematic review. Obstet Gynecol. 2020;136:922–31. https://doi.org/10.1097/AOG.0000000000004125.
Jha S, Gray T. A systematic review and meta-analysis of the impact of native tissue repair for pelvic organ prolapse on sexual function. Int Urogynecol J Pelvic Floor Dysfunct. 2014;26:321–7. https://doi.org/10.1007/s00192-014-2518-3.
Chang OH, Davidson ERW, Thomas TN, Paraiso MFR, Ferrando CA. Does concurrent posterior repair for an asymptomatic rectocele reduce the risk of surgical failure in patients undergoing sacrocolpopexy? Int Urogynecol J. 2020;31(10):2075–80. https://doi.org/10.1007/s00192-020-04268-7.
Meriwether KV, Gold KP, de Tayrac R, Cichowski SB, Minassian VA, Cartwright R, et al. Joint report on terminology for surgical procedures to treat pelvic organ prolapse. Int Urogynecol J. 2020;31:429–63. https://doi.org/10.1007/s00192-020-04236-1.
Barber MD, Brubaker L, Burgio KL, Richter HE, Nygaard I, Weidner AC, et al. Comparison of 2 transvaginal surgical approaches and perioperative behavioral therapy for apical vaginal prolapse: the OPTIMAL randomized trial. JAMA. 2014;311:1023–34. https://doi.org/10.1001/jama.2014.1719.
Nieminen K, Hiltunen KM, Laitinen J, Oksala J, Heinonen PK. Transanal or vaginal approach to rectocele repair: a prospective, randomized pilot study. Dis Colon Rectum. 2004;47:1636–42. https://doi.org/10.1007/s10350-004-0656-2.
Farid M, Madbouly KM, Hussein A, Mahdy T, Moneim HA, Omar W. Randomized controlled trial between perineal and anal repairs of rectocele in obstructed defecation. World J Surg. 2010;34:822–9. https://doi.org/10.1007/s00268-010-0390-y.
van Zanten F, Brem C, Lenters E, Broeders IAMJ, Schraffordt Koops SE. Sexual function after robot-assisted prolapse surgery: a prospective study. Int Urogynecol J. 2018;29:905–12. https://doi.org/10.1007/s00192-018-3645-z.
Portman D, Shulman L, Yeaw J, Zeng S, Uzoigwe C, Maamari R, et al. One-year treatment persistence with local estrogen therapy in postmenopausal women diagnosed as having vaginal atrophy. Menopause. 2015;22:1197–203. https://doi.org/10.1097/GME.0000000000000465.
Weissmann-Brenner A, Bayevsky T, Yoles I. Compliance to vaginal treatment-tablets versus cream: a retrospective 9 years study. Menopause. 2017;24:73–6. https://doi.org/10.1097/GME.0000000000000729.
Biehl C, Plotsker O, Mirkin S. A systematic review of the efficacy and safety of vaginal estrogen products for the treatment of genitourinary syndrome of menopause. Menopause (New York, NY). 2019;26:431–53. https://doi.org/10.1097/GME.0000000000001221.
Bachmann G, Bouchard C, Hoppe D, Ranganath R, Altomare C, Vieweg A, et al. Efficacy and safety of low-dose regimens of conjugated estrogens cream administered vaginally. Menopause (New York, NY). 2009;16:719–27. https://doi.org/10.1097/GME.0B013E3181A48C4E.
Bradley MS, Askew AL, Vaughan MH, Kawasaki A, Visco AG. Robotic-assisted sacrocolpopexy: early postoperative outcomes after surgical reduction of enlarged genital hiatus. Am J Obstet Gynecol. 2018;218:514.e1–8. https://doi.org/10.1016/j.ajog.2018.01.046.
Mueller MG, Jacobs KM, Mueller ER, Abernethy MG, Kenton KS. Outcomes in 450 women after minimally invasive abdominal Sacrocolpopexy for pelvic organ prolapse. Female Pelvic Med Reconstruc Surg. 2016;22:267–71. https://doi.org/10.1097/SPV.0000000000000269.
Culligan PJ, Salamon C, Lewis C, Abell TD. Cost-effectiveness analysis comparing robotic sacrocolpopexy to a vaginal mesh hysteropexy for treatment of uterovaginal prolapse. Open J Obstet Gynecol. 2013;03:613–20. https://doi.org/10.4236/ojog.2013.38110.
Harvie HS, Honeycutt AA, Neuwahl SJ, Barber MD, Richter HE, Visco AG, et al. Responsiveness and minimally important difference of SF-6D and EQ-5D utility scores for the treatment of pelvic organ prolapse. Am J Obstet Gynecol. 2019;220:265.e1–265.e11. https://doi.org/10.1016/j.ajog.2018.11.1094.
Slade E, Daly C, Mavranezouli I, Dias S, Kearney R, Hasler E, et al. Primary surgical management of anterior pelvic organ prolapse: a systematic review, network meta-analysis and cost-effectiveness analysis. BJOG: Int J Obstet Gynaecol. 2020;127:18–26. https://doi.org/10.1111/1471-0528.15959.
DiBonaventura M, Luo X, Moffatt M, Bushmakin AG, Kumar M, Bobula J. The association between vulvovaginal atrophy symptoms and quality of life among postmenopausal women in the United States and Western Europe. J Women's Health. 2015;24:713–22. https://doi.org/10.1089/jwh.2014.5177.
Craig BM, Mitchell SA. Examining the value of menopausal symptom relief among US women. Value Health. 2016;19(2):158–66. https://doi.org/10.1016/J.JVAL.2015.11.002.
GoodRx Premarin prices. https://www.goodrx.com/premarin?dosage=30g‐of‐0.625mg‐g&form=tube‐ofcream&label_override=Premarin&quantity=1&sort_type=popularity. Accessed 14 Feb 2021
Centers for Medicare & Medicaid Services. Physician Fee Schedule Search. 2019. https://www.cms.gov/apps/physician‐fee‐schedule/search/search‐criteria.aspx. Accessed 23 May 2019
Walters SJ, Brazier JE. What is the relationship between the minimally important difference and health state utility values? The case of the SF-6D. Health Qual Life Outcomes. 2003;1:4. https://doi.org/10.1186/1477-7525-1-4.
Siff LN, Barber MD, Zyczynski HM, Rardin CR, Jakus-Waldman S, Rahn DD, et al. Immediate postoperative pelvic organ prolapse quantification measures and 2-year risk of prolapse recurrence. Obstet Gynecol. 2020;136:792–801. https://doi.org/10.1097/AOG.0000000000004043.
Chang O, Yao M, Ferrando C, Paraiso M, Propst K. Determining the ideal intraoperative resting genital hiatus size - balancing surgical and functional outcomes. Female Pelvic Med Reconstruc Surg Urg. 2022;28(10):649–57.
Contributions to authorship
OC, JS, BM, ES, SW — Substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data for the work.
OC, JS, BM, ES, SW — Drafting the work or revising it critically for important intellectual content.
OC, JS, BM, ES, SW — Final approval of the version to be published.
OC, JS, BM, ES, SW — Agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Funding
This study was supported by an unrestricted grant provided by the Foundation for Female Health Awareness, who had no influence on the design of the study and writing of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
Not applicable since the study was based on modeling and previously published data.
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Presentation
This study was presented as an oral presentation at the Society of Gynecologic Surgeons meeting in San Antonio, TX, USA in 2022.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chang, O.H., Shepherd, J.P., St. Martin, B. et al. Surgical correction of the genital hiatus at the time of sacrocolpopexy — a 7-year Markov analysis: a cost-effectiveness analysis. Int Urogynecol J 34, 2969–2975 (2023). https://doi.org/10.1007/s00192-023-05628-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-023-05628-9