Abstract
Introduction and hypothesis
Stress urinary incontinence (SUI) is treated with transobturator tape (TOT) sling procedures, but problems arise with artificial mesh in certain instances. Hence, non-invasive laser therapy may be useful under such circumstances. The current study was aimed at comparing the effects of these two treatments and at checking their applicability in various body mass index (BMI) groups.
Methods
Seventy-nine patients, who were clinically diagnosed with SUI, were divided into two groups, those who preferred TOT and those who preferred the transvaginal fractional micro-ablative CO2 laser system. The SUI symptoms and International Consultation on Incontinence Questionnaire Short Form (ICIQ-SF) scores of the patients were determined before and at the 12th month after the treatment. General linear model, Stuart–Maxwell, and Bonferroni correction for pairwise comparison analyses were performed to compare the efficacy of the treatment type.
Results
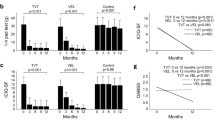
The ICIQ-SF score decreased by 56.8% for laser therapy and 43.5% for TOT therapy (mean ± SE = 5.97 ± 0.16 and 5.09 ± 0.14 respectively). Laser therapy had a better effect on ICIQ-SF than TOT therapy (η2p: 0.176, ptime*group < 0.001). Regardless of the types of treatment, the ICIQ-SF scores of healthy-weight participants decreased more than those of overweight participants (η2p:0.050, ptime*group = 0.045). In the TOT group, healthy-weight participants were more than twice as likely to recover fully from SUI symptoms as overweight participants, 1 year after the treatment. In the laser group, the majority of healthy-weight participants (88.8%) did not report any SUI symptoms after the treatment.
Conclusions
The efficacy of laser therapy for urinary incontinence was confirmed. Furthermore, it was observed that being overweight may be a risk factor for the failure of laser therapy.

Similar content being viewed by others
Data availability
Data may be shared by the corresponding author when necessary.
References
Milsom I, Gyhagen M. The prevalence of urinary incontinence. Climacteric. 2019;22(3):217–22. https://doi.org/10.1080/13697137.2018.1543263.
NCD Risk Factor Collaboration. Trends in adult body-mass index in 200 countries from 1975 to 2014: a pooled analysis of 1698 population-based measurement studies with 19.2 million participants. Lancet. 2016;387(10026):1377–96. https://doi.org/10.1016/S0140-6736(16)30054-X.
Kuh D, Cardozo L, Hardy R. Urinary incontinence in middle aged women: childhood enuresis and other lifetime risk factors in a British prospective cohort. J Epidemiol Community Health. 1999;53(8):453–8. https://doi.org/10.1136/jech.53.8.453.
Burgio KL, Richter HE, Clements RH, Redden DT, Goode PS. Changes in urinary and fecal incontinence symptoms with weight loss surgery in morbidly obese women. Obstet Gynecol. 2007;110(5):1034–40. https://doi.org/10.1097/01.AOG.0000285483.22898.9c.
Abrams P, Andersson K-E, Birder L, et al. Fourth International Consultation on Incontinence Recommendations of the International Scientific Committee: evaluation and treatment of urinary incontinence, pelvic organ prolapse, and fecal incontinence. Neurourol Urodyn. 2010;29(1):213–40. https://doi.org/10.1002/nau.20870.
Wing RR, West DS, Grady D, et al. Effect of weight loss on urinary incontinence in overweight and obese women: results at 12 and 18 months. J Urol. 2010;184(3):1005–10. https://doi.org/10.1016/j.juro.2010.05.031.
Rovner ES, Wein AJ. Treatment options for stress urinary incontinence. Rev Urol. 2004;6(Suppl 3):29–40.
Takahashi S, Takei M, Asakura H, et al. Clinical guidelines for female lower urinary tract symptoms. Int J Urol. 2021;28(5):474–92. https://doi.org/10.1111/iju.14492.
Heneghan C, Aronson JK, Goldacre B, Mahtani KR, Plüddemann A, Onakpoya I. Transvaginal mesh failure: lessons for regulation of implantable devices. BMJ. 2017;359:1–6. https://doi.org/10.1136/bmj.j5515.
Rechberger T, Postawski K, Jakowicki JA, Gunja-Smith Z, Woessner JF Jr. Role of fascial collagen in stress urinary incontinence. Am J Obstet Gynecol. 1998;179(6):1511–4. https://doi.org/10.1016/S0002-9378(98)70017-1.
Zerbinati N, Serati M, Origoni M, et al. Microscopic and ultrastructural modifications of postmenopausal atrophic vaginal mucosa after fractional carbon dioxide laser treatment. Lasers Med Sci. 2015;30(1):429–36. https://doi.org/10.1007/s10103-014-1677-2.
Zivanovic I, Rautenberg O, Lobodasch K, von Bünau G, Walser C, Viereck V. Urethral bulking for recurrent stress urinary incontinence after midurethral sling failure. Neurourol Urodyn. 2017;36(3):722–6. https://doi.org/10.1002/nau.23007.
Krhut J, Zachoval R, Smith PP, et al. Pad weight testing in the evaluation of urinary incontinence. Neurourol Urodyn. 2014;33(5):507–10. https://doi.org/10.1002/nau.22436.
Wlaźlak E, Viereck V, Kociszewski J, et al. Role of intrinsic sphincter deficiency with and without urethral hypomobility on the outcome of tape insertion. Neurourol Urodyn. 2017;36(7):1910–6. https://doi.org/10.1002/nau.23211.
Avery K, Donovan J, Peters TJ, Shaw C, Gotoh M, Abrams P. ICIQ: a brief and robust measure for evaluating the symptoms and impact of urinary incontinence. Neurourol Urodyn. 2004;23(4):322–30. https://doi.org/10.1002/nau.20041.
Çetinel B, Özkan B, Can G. ICIQ-SF Türkçe versiyonu validasyon (geçerlilik) çalışması. Turk J Urol. 2004;30(3):332–8.
Behnia-Willison F, Nguyen TT, Mohamadi B, et al. Fractional CO2 laser for treatment of stress urinary incontinence. Eur J Obstet Gynecol Reprod Biol. 2019;1:1–5. https://doi.org/10.1016/j.eurox.2019.100004.
Foulot H, Uzan I, Chopin N, Borghese B, Chapron C. Monarc transobturator sling system for the treatment of female urinary stress incontinence: results of a post-operative transvaginal ultrasonography. Int Urogynecol J. 2007;18(8):857–61. https://doi.org/10.1007/s00192-006-0244-1.
Glover T, Mitchell K. An introduction to biostatistics. Long Grove, IL: Waveland Press; 2008.
Minassian VA, Yan X, Lichtenfeld MJ, Sun H, Stewart WF. The iceberg of health care utilization in women with urinary incontinence. Int Urogynecol J. 2012;23(8):1087–93. https://doi.org/10.1007/s00192-012-1743-x.
Ogrinc UB, Senčar S, Lenasi H. Novel minimally invasive laser treatment of urinary incontinence in women. Lasers Surg Med. 2015;47(9):689–97. https://doi.org/10.1002/lsm.22416.
Vizintin Z, Lukac M, Kazic M, Tettamanti M. Erbium laser in gynecology. Climacteric. 2015;18(Supp1):4–8. https://doi.org/10.3109/13697137.2015.1078668.
Okui N. Comparison between erbium-doped yttrium aluminum garnet laser therapy and sling procedures in the treatment of stress and mixed urinary incontinence. World J Urol. 2019;37(5):885–9. https://doi.org/10.1007/s00345-018-2445-x.
Erel CT, Fernandez LDC, Inan D, Makul M. Er:YAG laser treatment of urinary incontinence after failed TOT/TVT procedures. Eur J Obstet Gynecol Reprod Biol. 2020;252:399–403. https://doi.org/10.1016/j.ejogrb.2020.07.010.
Fistonić FN, Fistonić I, Lukanovič A, Guštek ŠF, Turina ISB, Franić D. First assessment of short-term efficacy of Er:YAG laser treatment on stress urinary incontinence in women: prospective cohort study. Climacteric. 2015;18(Supp1):37-42.https://doi.org/10.3109/13697137.2015.1071126
Franić D, Fistonić I. Laser therapy in the treatment of female urinary incontinence and genitourinary syndrome of menopause: an update. Biomed Res Int. 2019;1:1–10. https://doi.org/10.1155/2019/1576359.
Subak LL, Richter HE, Hunskaar S. Obesity and urinary incontinence: epidemiology and clinical research update. J Urol. 2009;182(6):2–7. https://doi.org/10.1016/j.juro.2009.08.071.
Hanewinckel R, Ikram MA, Franco OH, Hofman A, Drenthen J, van Doorn PA. High body mass and kidney dysfunction relate to worse nerve function, even in adults without neuropathy. J Peripher Nerv Syst. 2017;22(2):112–20. https://doi.org/10.1111/jns.12211.
Serati M, Sorice P, Bogani G, et al. TVT for the treatment of urodynamic stress incontinence: efficacy and adverse effects at 13-year follow-up. Neurourol Urodyn. 2017;36(1):192–197. https://doi.org/10.1002/nau.22914
Brennand E, Tang S, Williamson T, et al. Twelve-month outcomes following midurethral sling procedures for stress incontinence: impact of obesity. BJOG 2015;122(12):1705–12.
Sun Y, Luo D, Yang L, et al. The efficiency and safety of tension-free vaginal tape (TVT) Abbrevo procedure versus TVT exact in the normal weight and overweight patients affected by stress urinary incontinence. Urology. 2017;110:63–9. https://doi.org/10.1111/1471-0528.13132.
Barco-Castillo C, Plata M, Zuluaga L, et al. Obesity as a risk factor for poor outcomes after sling surgery in women with stress urinary incontinence: a systematic review and meta-analysis. Neurourol Urodyn. 2020;39(8):2153–60. https://doi.org/10.1002/nau.24459.
Acknowledgements
We would like to thank the patients for their participation in the study. I would also like to thank Mustafa Gani Gençer, an academician at Fırat University, for his assistance in manuscript translation and editing.
Author information
Authors and Affiliations
Contributions
F. Çağiran Yilmaz: designed research, conducted research, wrote the paper; M. AAçik: analyzed data or performed statistical analysis, wrote the paper; F. Çağiran: designed research, conducted research. All authors had primary responsibility for the final content and read and approved the final manuscript.
Corresponding author
Ethics declarations
The presented study was conducted according to statements in the Declaration of Helsinki. A detailed consent form was provided. Diyarbakır Gazi Yasargil Training and Research Hospital Clinical Research Ethics Committee authorized the presented study by the number 2022–02-18.
Conflicts of interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yılmaz, F.Ç., Açık, M. & Çağıran, F. Comparison between laser and transobturator tape therapy in the treatment of stress urinary incontinence and role of overweight in treatment: a prospective observational study. Int Urogynecol J 34, 2901–2908 (2023). https://doi.org/10.1007/s00192-023-05625-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-023-05625-y