Abstract
Introduction and hypothesis
The objective was to evaluate the effectiveness of pharmacological hemostatic agents in the reduction of blood loss at vaginal surgery.
Methods
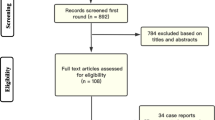
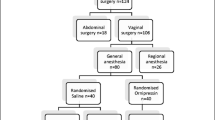
A systematic review of randomized control trials (RCTs) was completed. We searched PubMed (1946–2022), Embase, and CINAHL, using search terms related to vaginal hysterectomies and reconstructive surgeries combined with peri-operative use of hemostatic agents. RCTs comparing hemostatic interventions with placebo or with standard care were analyzed with the primary outcome of estimated blood loss. Secondary outcomes included peri-operative complications, length of stay, blood transfusion, and readmission. Risk of bias was assessed using the Risk of Bias 2 tool.
Results
Nine RCTs were included with a total of 903 participants. All trials were considered to have an overall low risk of bias. Meta-analysis of six RCTs (491 participants) favored the use of vasoconstrictive agent (vasopressin/ornipressin) at the surgical site for an overall effect estimate of decreased blood loss by 70 ml (95% CI −125, −14 ml). There was significant heterogeneity of studies with both dose and technique of vasoconstrictive agents used. Only one RCT evaluated tranexamic acid and found a benefit in the prophylactic use of intravenous tranexamic acid.
Conclusions
Peri-operative use of vasoconstrictive agents slightly reduces bleeding in women undergoing elective vaginal surgery. Additional studies evaluating alternative pharmacological agents such as tranexamic acid may be of benefit.



Similar content being viewed by others
References
Pelvic organ prolapse: ACOG practice bulletin, number 214. Obstet Gynecol. 2019;134(5):e126–42.
Wu JM, Hundley AF, Fulton RG, Myers ER. Forecasting the prevalence of pelvic floor disorders in U.S. women: 2010 to 2050. Obstet Gynecol. 2009;114(6):1278–83.
Muñoz M, Laso-Morales MJ, Gómez-Ramírez S, Cadellas M, Núñez-Matas MJ, García-Erce JA. Pre-operative haemoglobin levels and iron status in a large multicentre cohort of patients undergoing major elective surgery. Anaesthesia. 2017;72(7):826–34.
Bouchard ME, Baker K, Schachter J, et al. Preoperative anemia and complications after surgery for pelvic organ prolapse: an analysis of the national surgical quality improvement program database. Int Urogynecol J. 2022;33(7):1827–31.
Clancy AA, Ilin J, Pascali D, Shehata F, Hickling DR. Outcomes of an overnight-stay unit for urogynecologic surgery: feasibility and risk factors for failure of next-day discharge. Female Pelvic Med Reconstr Surg. 2021;27(2):98–104.
Wysham WZ, Roque DR, Soper JT. Use of topical hemostatic agents in gynecologic surgery. Obstet Gynecol Surv. 2014;69(9):557–63.
Wellington K, Wagstaff AJ. Tranexamic acid: a review of its use in the management of menorrhagia. Drugs. 2003;63(13):1417–33.
Dunn CJ, Goa KL. Tranexamic acid: a review of its use in surgery and other indications. Drugs. 1999;57(6):1005–32.
Relke N, Chornenki NLJ, Sholzberg M. Tranexamic acid evidence and controversies: An illustrated review. Res Pract Thromb Haemost. 2021;5(5):e12546.
Roberts I, Shakur H, Coats T, et al. The CRASH-2 trial: a randomised controlled trial and economic evaluation of the effects of tranexamic acid on death, vascular occlusive events and transfusion requirement in bleeding trauma patients. Health Technol Assess. 2013;17(10):1–79.
Shakur H, Elbourne D, Gülmezoglu M, et al. The WOMAN Trial (World maternal antifibrinolytic trial): tranexamic acid for the treatment of postpartum haemorrhage: an international randomised, double blind placebo controlled trial. Trials. 2010;16(11):40.
Latthe P, Kadian S, Parsons M, Toozs-Hobson P. Survey of use of local infiltration and vasoconstrictors in vaginal surgery. Gynecol Surg. 2007;4(3):187–9.
O’Neal MG, Beste T, Shackelford DP. Utility of preemptive local analgesia in vaginal hysterectomy. Am J Obstet Gynecol. 2003;189(6):1539–41; discussion 1541–2.
Topsoee MF, Bergholt T, Ravn P, et al. Anti-hemorrhagic effect of prophylactic tranexamic acid in benign hysterectomy—a double-blinded randomized placebo-controlled trial. Am J Obstet Gynecol. 2016;215(1):72.e1–8.
Julian TM, Johnson GW, Gosewehr JA, O’Connell BJ. Vasopressin as a chemical tourniquet during vaginal surgery. J Gynecol Surg. 1993;9(3):161–4.
Kammerer-Doak DN, Rogers RG, Johnson Maybach J, Traynor Mickelson M. Vasopressin as an etiologic factor for infection in gynecologic surgery: a randomized double-blind placebo-controlled trial. Am J Obstet Gynecol. 2001;185(6):1344–7; discussion 1347–8.
Nimodia V, Jain S, Rajaram S, Tyagi A, Gupta B. Effect of diluted vasopressin vs saline on intraoperative blood loss during vaginal hysterectomy—a randomised controlled trial. J Clin Diagn Res. 2021;15(6):QC13–6.
Ascher-Walsh CJ, Capes T, Smith J, Michels A. Cervical vasopressin compared with no premedication and blood loss during vaginal hysterectomy: a randomized controlled trial. Obstet Gynecol. 2009;113(2 Pt 1):313–8.
Seow KM, Lin YH, Hwang JL, Huang LW, Pan CP. A simple procedure to prevent chronic vaginal colpotomy wound bleeding after laparoscopically assisted vaginal hysterectomy. Int J Gynaecol Obstet. 2010;109(1):49–51.
Henn EW, Nondabula T, Juul L. Effect of vaginal infiltration with ornipressin or saline on intraoperative blood loss during vaginal prolapse surgery: a randomised controlled trial. Int Urogynecol J. 2016;27(3):407–12.
Bartos P, Popelka P, Adamcová P, Struppl D. Adrenalin versus terlipressin: blood loss and cardiovascular side-effects in the vaginal part of laparoscopically-assisted vaginal hysterectomy or vaginal hysterectomy. Clin Exp Obstet Gynecol. 2000;27(3–4):182–4.
Guilcher SJT, Everall AC, Cadel L, Li J, Kuluski K. A qualitative study exploring the lived experiences of deconditioning in hospital in Ontario, Canada. BMC Geriatr. 2021;21(1):169.
Mount Sinai Hospital, Canada. Does intravenous tranexamic acid reduce blood loss during vaginectomy? A double-blind, placebo-controlled, randomized trial [Internet]. Accessed 17 April 2023. Report No.: NCT03216083. Available from: https://clinicaltrials.gov/ct2/show/NCT03216083
Acknowledgements
We are grateful to Karine Fournier (Research librarian, Health Sciences Library, University of Ottawa) for her assistance with development of the search strategy.
Author information
Authors and Affiliations
Contributions
Y.C. contributed to the conception and design of study, data acquisition and analysis, and the writing of the manuscript. I.C. contributed to writing of the manuscript. A.C. contributed to data acquisition and writing of the manuscript. A.A.C. contributed to the conception, design of study, revision, and statistical analysis. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflicts of interest. No financial support was obtained.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.

Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cui, Y., Chen, I., Chernoff, A. et al. Effectiveness of prophylactic pharmacological hemostatic agents for reduction of blood loss at vaginal surgery: a systematic review and meta-analysis. Int Urogynecol J 34, 2945–2957 (2023). https://doi.org/10.1007/s00192-023-05614-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-023-05614-1