Abstract
Introduction and hypothesis
Urinary incontinence (UI) is common in the postpartum period; however, most studies focus on the early postpartum period and assess prevalence at only one or two time points. We hypothesized that UI would be prevalent across the first 2 years postpartum. Our secondary objective was to evaluate risk factors for postpartum UI among a nationally representative, contemporary sample.
Methods
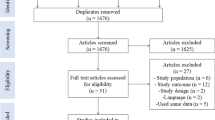
This cross-sectional, population-based study used National Health and Nutrition Examination Survey (2011–2018) data for parous women within 24 months following delivery. Prevalence of UI, UI subtypes, and severity were estimated. Multivariate logistic regression was used to estimate adjusted odds (aOR) of UI for exposures of interest.
Results
Among 560 postpartum women, prevalence of any UI was 43.5%. Stress UI was most common (28.7%), and most women (82.8%) experienced mild symptoms. There was no significant change in prevalence of UI across the 24 months following delivery (R2 = 0.004). Individuals with postpartum UI tended to be older (30.3 ± 0.5 versus 28.8 ± 0.5 years) and had higher BMI (31.1 ± 0.6 versus 28.9 ± 0.6). In multivariate analysis, odds of postpartum UI were higher for women who had had a prior vaginal delivery (aOR 2.0, 95% CI: 1.3–3.3), prior delivery of a baby weighing 9 lb (4 kg) or more (aOR 2.5, 95% CI: 1.3–4.8), or who reported current smoking (aOR 1.5, 95% CI: 1.0–2.3).
Conclusions
During the first 2 years postpartum 43.5% of women report UI, with relatively stable prevalence over this period. This high prevalence supports screening for UI after delivery regardless of risk factors.
Similar content being viewed by others
Data Availability
The data used for this study are publicly available at https://wwwn.cdc.gov/nchs/nhanes/Default.aspx.
References
Datar M, Pan L-C, McKinney JL, Goss TF, Pulliam SJ. Healthcare resource use and cost of burden of urinary incontinence to United States payers. Neurourol Urodyn. 2022;41:1553–62.
Subak LL, Brown JS, Kraus SR, et al. The “costs” of urinary incontinence for women. Obstet Gynecol. 2006;107(4):908–16.
Sinclair AJ, Ramsay IN. The psychosocial impact of urinary incontinence in women. Obstet Gynaecol. 2011;13:143–8.
Nam JY, Park E-C, Cho E. Does urinary incontinence and mode of delivery affect postpartum depression? A nationwide population-based cohort study in Korea. Int J Environ Res Public Health. 2021;18(437):1–9.
Baydock SA, Flood C, Schulz JA, et al. Prevalence and risk factors for urinary and fecal incontinence four months after vaginal delivery. J Obstet Gynaecol Can. 2009;31(1):36–41.
Hatem M, Pasquier J-C, Fraser W, Lepire E. Factors associated with postpartum urinary/anal incontinence in primiparous women in Quebec. J Obstet Gynaecol Can. 2007;29(3):232–9.
Da Silva LL, Lucio A, de Moraes Lopes MHB. Risk factors for postpartum urinary incontinence. Rev Esc Enferm USP. 2016;50(2):200–7.
Arrue M, Diez-Itza I, Ibanez L, Paredes J, Murgiondo A, Sarasqueta C. Factors involved in the persistence of stress urinary incontinence from pregnancy to 2 years post partum. Int J Gynecol Obstet. 2011;115:256–9.
Patel K, Long JB, Boyd SS, Kjerulff KH. Natural history of urinary incontinence from first childbirth to 30-months postpartum. Arch Obstet Gynaecol. 2021;304:713–24.
Thom D, Rortveit G. Prevalence of postpartum urinary incontinence: a systematic review. Acta Obstet Gynecol. 2010;89:1511–22.
Quiboeuf E, Saurel-Cubizolles M-J, Fritel X. Trends in urinary incontinence in women between 4 and 24 months postpartum in the EDEN cohort. BJOG. 2016;123:1222–8.
Pizzoferrato A-C, Fauconnier A, Quiboeuf E, Morel K, Schaal J-P, Fritel X. Urinary incontinence 4 and 12 years after first delivery: risk factors associated with prevalence, incidence, remission, and persistence in a cohort of 236 women. Neurourol Urodyn. 2014;33:1229–34.
Gartland D, MacArthur C, Woolhouse H, McDonald E, Brown SJ. Frequency, severity and risk factors for urinary and faecal incontinence at 4 years postpartum: a prospective cohort. BJOG. 2016;123:1203–11.
Thomason AD, Miller JM, DeLancey JOL. Urinary incontinence symptoms during and after pregnancy in continent and incontinent primiparas. Int Urogynecol J. 2007;18(2):147–51.
Gyhagen M, Bullarbo M, Nielsen TF, Milsom I. The prevalence of urinary incontinence 20 years after childbirth: a national cohort study in singleton primiparae after vaginal or cesarean delivery. BJOG. 2013;120:140–51.
Wesnes SL, Hannestad Y, Rortveit G. Delivery parameters, neonatal parameters and incidence of urinary incontinence six months postpartum: a cohort study. Acta Obstet Gynecol Scand. 2017;96:1214–22.
Wang K, Xu X, Jia G, Jiang H. Risk factors for postpartum stress urinary incontinence: a systematic review and meta-analysis. Reprod Sci. 2020;27:2129–45.
Burgio KL, Zyczynski H, Locher JL, Richter HE, Redden DT, Wright KC. Urinary incontinence in the 12-month postpartum period. Obstet Gynecol. 2003;102(6):1291–8.
National Center for Health Statistics. About the National Health and Nutrition Examination Survey. https://www.cdc.gov/nchs/nhanes/about_nhanes.htm. Accessed 5 Dec 2022.
Kupfer N, Clancy A, Maguire F, Stairs J. Prevalence and risk factors for urinary incontinence in nulliparous women: a contemporary, population-based cohort study. Urogynecology. 2022;5:520–7.
Minassian VA, Stewart WF, Wood GC. Urinary incontinence in women: variation in prevalence estimates and risk factors. Obstet Gynecol. 2008;111:324–31.
Centers for Disease Control and Prevention (CDC). National Center for Health Statistics (NCHS). National Health and Nutrition Examination Survey, 2015–2018: Sample Design and Estimation Procedures. Hyattsville: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2011–2018. https://www.cdc.gov/nchs/data/series/sr_02/sr02-184-508.pdf. Accessed 8 Apr 2023.
Delancey JOL, Low LK, Miller JM, Patel DA, Tumbarello JA. Graphic integration of causal factors of pelvic floor disorders: an integrated life span model. Am J Obstet Gynecol. 2008;199:610.e1–5.
Milsom I, Gyhagen M. The prevalence of urinary incontinence. Climacteric. 2019;22(3):217–22.
Sullivan R, McNicholas T, Claffey P, Kenny RA, Briggs R. Unreported urinary incontinence: population-based prevalence and factors associated with non-reporting of symptoms in community-dwelling people ≥ 50 years. Eur Geriatr Med. 2021;12:405–12.
Woodley SJ, Lawrenson P, Boyle R, et al. Pelvic floor muscle training for preventing and treating urinary and faecal incontinence in antenatal and postnatal women. Cochrane Database Syst Rev. 2020;5(5):CD007471.
Hage-Fransen MAH, Wiezer M, Otto A, et al. Pregnancy- and obstetric-related risk factors for urinary incontinence, fecal incontinence, or pelvic organ prolapse later in life: a systematic review and meta-analysis. Acta Obstet Gynecol Scand. 2021;100:373–82.
Author information
Authors and Affiliations
Contributions
K. Bonasia: project development, manuscript writing; A. Clancy: project development, manuscript editing; J. Stairs: project development, data management, data analysis, manuscript editing.
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bonasia, K., Clancy, A. & Stairs, J. Prevalence and risk factors for urinary incontinence up to 2 years postpartum: a cross-sectional population-based study. Int Urogynecol J 34, 2467–2472 (2023). https://doi.org/10.1007/s00192-023-05571-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-023-05571-9