Abstract
Introduction and hypothesis
This study aimed to compare the difference in levator ani muscle (LAM) volumes between 'normal' and those with sonographically visualized LAM defects. We hypothesized that the 'muscle damage' group would have a significantly lower muscle volume.
Methods
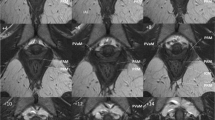
The study included patients who had undergone a 3D endovaginal ultrasound. The normal (NM) and damage (DM) muscle groups’ architectural changes were evaluated based on anterior-posterior (AP), left-right (LR) diameter, and minimal levator hiatus (MLH) area. The puboanalis-puboperinealis (PA), puborectalis (PR), and pubococcygeus-iliococcygeus (PC) were manually segmented using 2.5 vs. 1.0 mm to find the optimal sequence and to compare the volumes between NM and DM groups. POPQs were compared between the NM and DM groups.
Results
The 1.0-mm segmentation volumes created superior volume analysis. Comparing NM to the DM group showed no significant difference in LAM volume. Respectively, the mean total LAM volumes were 17.27 cm3 (SD = 3.97) and 17.04 cm3 (SD = 4.32), p = 0.79. The mean MLH measurements for both groups respectively were 10.06 cm2 (SD = 2.93) and 12.18 cm2 (SD = 2.93), indicating a significant difference (p = 0.01). POPQ analysis demonstrated statistically significant differences at Ba and Bp parameters suggesting that the DM group had worse prolapse (p = 0.05, 0.01, respectively).
Conclusions
While LAM volumes are similar, there is a significant difference in the physical architecture of the LAM and the POPQ parameters in muscle-damaged patients compared to the normal group.



Similar content being viewed by others
References
Memon HU, Handa VL. Vaginal Childbirth and Pelvic Floor Disorders. Women's Health (Lond Engl). 2013;9:265–77. https://doi.org/10.2217/WHE.13.17.
Quiroz LH, Pickett SD, Peck JD, Rostaminia G, Stone DE, Shobeiri SA. Increasing age is a risk factor for decreased postpartum pelvic floor strength. Female Pelvic Med Reconstr Surg. 2017;23:136–40. https://doi.org/10.1097/SPV.0000000000000376.
Alshiek J, Wei Q, Jalalizadeh M, Chitnis P, Shobeiri SA. The Effect of Aging on Pelvic Floor Pressure Measurements in Nulliparous Women. Open J Obstet Gynecol. 2020;10:751–69. https://doi.org/10.4236/ojog.2020.1060070.
Friedman S, Blomquist JL, Nugent JM, McDermott KC, Muñoz A, Handa VL. Pelvic Muscle Strength After Childbirth. Obstet Gynecol. 2012;120:1021–8. https://doi.org/10.1097/AOG.0b013e318265de39.
Rostaminia G, White D, Hegde A, Quiroz LH, Davila GW, Shobeiri SA. Levator Ani Deficiency and Pelvic Organ Prolapse Severity. Obstet Gynecol. 2013;121:1017–24. https://doi.org/10.1097/AOG.0b013e31828ce97d.
Rostaminia G, White DE, Quiroz LH, Shobeiri SA. Levator plate descent correlates with levator ani muscle deficiency. Neurourol Urodyn. 2015;34:55–9. https://doi.org/10.1002/nau.22509.
Sindhwani N, et al. Semi-automatic outlining of levator hiatus. Ultrasound Obstet Gynecol. 2016;48:98–105. https://doi.org/10.1002/uog.15777.
Delft K, Thakar R, Shobeiri SA, Sultan AH. Levator hematoma at the attachment zone as an early marker for levator ani muscle avulsion. Ultrasound Obstet Gynecol. 2014;43:210–7. https://doi.org/10.1002/uog.12571.
Javadian P, O'Leary D, Rostaminia G, North J, Wagner J, Quiroz LH, Shobeiri SA. How does 3D endovaginal ultrasound compare to magnetic resonance imaging in the evaluation of levator ani anatomy? Neurourol Urodyn. 2017 Feb;36(2):409–13. https://doi.org/10.1002/nau.22944.
Santoro GA, Wieczorek AP, Shobeiri SA, Mueller ER, Pilat J, Stankiewicz A, Battistella G. Interobserver and interdisciplinary reproducibility of 3D endovaginal ultrasound assessment of pelvic floor anatomy. Int Urogynecol J. 2011 Jan;22(1):53–9. https://doi.org/10.1007/s00192-010-1233-y.
Rostaminia G, Manonai J, Leclaire E, Omoumi F, Marchiorlatti M, Quiroz LH, Shobeiri SA. Interrater reliability of assessing levator ani deficiency with 360° 3D endovaginal ultrasound. Int Urogynecol J. 2014;25(6):761–6. https://doi.org/10.1007/s00192-013-2286-5 Epub 2013 Dec 13. Erratum in: Int Urogynecol J. 2014 Apr;25(4):565.
Delft K, Sultan AH, Thakar R, Shobeiri SA, Kluivers K. Agreement between palpation and transperineal and endovaginal ultrasound in the diagnosis of levator ani avulsion. Int Urogynecol J. 2014;26:33–9. https://doi.org/10.1007/s00192-014-2426-6.
Shobeiri SA, White D, Quiroz LH, Nihira MA. Anterior and posterior compartment 3D endovaginal ultrasound anatomy based on the direct histologic comparison. Int Urogynecol J. 2012;23:1047–53. https://doi.org/10.1007/s00192-012-1721-3.
Shobeiri SA, LeClaire E, Nihira MA, Quiroz LH, O'Donoghue D. Appearance of the Levator Ani Muscle Subdivisions in Endovaginal Three-Dimensional Ultrasonography. Obstet Gynecol. 2009;114:66–72. https://doi.org/10.1097/AOG.0b013e3181aa2c89.
Rostaminia G, Peck JD, Quiroz LH, Shobeiri SA. How well can levator ani muscle morphology on 3D pelvic floor ultrasound predict the levator ani muscle function? Int Urogynecol J. 2015;26:257–62. https://doi.org/10.1007/s00192-014-2503-x.
Rostaminia G, Shobeiri SA. Endovaginal Imaging: Pelvic Floor. Practical Pelvic Floor Ultrasonography: A Multicompartmental Approach to 2D/3D/4D Ultrasonography of the Pelvic Floor. Springer. 2017.
Rostaminia G, White D, Quiroz LH, Shobeiri SA. Is a New High-Resolution Probe Better than the Standard Probe for 3D Anal Sphincter and Levator Ani Imaging? Ultrason Imaging. 2015;37:168–75. https://doi.org/10.1177/0161734614534831.
Shobeiri SA, Rostaminia G, White D, Quiroz LH. The determinants of minimal levator hiatus and their relationship to the puborectalis muscle and the levator plate. BJOG Int J Obstet Gynaecol. 2013;120:205–11. https://doi.org/10.1111/1471-0528.12055.
Hoyte L, Ye W, Brubaker L, Fielding JR, Lockhart ME, Heilbrun ME, Brown MB, Warfield SK. Pelvic Floor Disorders Network. Segmentations of MRI images of the female pelvic floor: a study of inter- and intra-reader reliability. J Magn Reson Imaging. 2011;33(3):684–91. https://doi.org/10.1002/jmri.22478.
Bonmati E, Hu Y, Sindhwani N, Dietz HP, D'hooge J, Barratt D, Deprest J, Vercauteren T. Automatic segmentation method of pelvic floor levator hiatus in ultrasound using a self-normalizing neural network. J Med Imaging (Bellingham). 2018;5(2):021206. https://doi.org/10.1117/1.JMI.5.2.021206.
Da Silva AS, Asfour V, Digesu GA, Cartwright R, Fernando R, Khullar V. Levator Ani avulsion: The histological composition of this site. A cadaveric study. Neurology and Urodynamics. 2019;38:123–9. https://doi.org/10.1002/nau.23847.
Acknowledgments
The authors do not have any conflicts of interest and received no assistance writing this manuscript. The research project was the Master project for Ms. Zara and was supported by the George Mason University Department of Bioengineering and INOVA Department of Obstetrics and Gynecology.
Author information
Authors and Affiliations
Contributions
Z Asif: Data collection, Data analysis, Manuscript writing
R Tomashev: Manuscript writing
V Peterkin: Data analysis, Manuscript writing
J Alshiek: Data collection, Data analysis
Q Wei: Manuscript writing
Y Baumfeld: Data analysis
SA Shobeiri: Project development, Data analysis, Manuscript writing
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This work was presented during the IUGA 46th Annual Meeting.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Asif, Z., Tomashev, R., Peterkin, V. et al. Levator ani muscle volume and architecture in normal vs. muscle damage patients using 3D endovaginal ultrasound: a pilot study. Int Urogynecol J 34, 581–587 (2023). https://doi.org/10.1007/s00192-022-05366-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-022-05366-4