Abstract
Introduction and hypothesis
Stress urinary incontinence is the most prevalent type of urinary incontinence and childbirth is a risk factor. The aim of this study is to evaluate the association between delivery mode and urethral sphincter function as measured by the maximum urethral pressure (MUP).
Methods
A retrospective study on women seen in a tertiary urogynaecological center for urodynamic testing between January 2017 to December 2019. Women were classified into the following groups: (1) nulliparous; (2) caesarean section only; (3) at least one spontaneous vaginal delivery but no instrumental deliveries; (4) at least one vacuum delivery but no forceps; (5) at least one forceps delivery.
Results
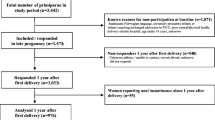
The complete data sets of 1238 women were analysed; 1112 (90%) were vaginally parous. Mean age was 58 (18–95) years. Mean parity was 2.6 (0–9); 57 (4.6%) were nulliparous, 69 (5.6%) had only been delivered by caesarean section, 762 (61.6%) had at least one spontaneous vaginal delivery but no instrumental deliveries, 41 (3.3%) had at least one vacuum but no forceps delivery, and 309 (25%) had at least one forceps delivery. Mean MUP was 41.8 cmH2O. There was a significant association between vaginal parity and MUP (P < 0.001). On ANOVA test, delivery mode was significantly associated with MUP. This became nonsignificant on regression analysis, with only age significantly associated with MUP (P < 0.001).
Conclusions
The effect of childbirth on urethral sphincter function seems to be largely due to the first vaginal birth. We failed to show an effect of instrumental delivery.


Similar content being viewed by others
References
Chiarelli P, Brown W, McElduff P. Leaking urine: prevalence and associated factors in Australian women. Neurourol Urodyn. 1999;18:567–77.
Hunskaar S, Lose G, Sykes D, Voss S. The prevalence of urinary incontinence in women in four European countries. BJU Int. 2004;93(3):324–30.
Hannestad YS, Rortveit G, Sandvik H, Hunskaar S. A community-based epidemiological survey of female urinary incontinence: the Norwegian EPINCONT study. Epidemiology of Incontinence in the County of Nord-Trondelag. J Clin Epidemiol. 2000;53(11):1150–7.
Cundiff G. The pathophysiology of stress urinary incontinence: a historical perspective. Rev Urol. 2004;6:S10–S8.
Ashton-Miller J, Howard D, Delancey J. The functional anatomy of the female pelvic floor and stress continence control system. Scand J Urol Nephrol Suppl. 2001;35:1–7.
Rud T, Andersson KE, Asmussen M, Hunting A, Ulmsten U. Factors maintaining the intraurethral pressure in women. Invest Urol. 1980;17(4):343–7.
Strohbehn K, Quint LE, Prince MR, Wojno KJ, DeLancey JO. Magnetic resonance imaging anatomy of the female urethra: a direct histologic comparison. Obstet Gynecol. 1996;88(5):750–6.
Pirpiris A, Shek KL, Kay P, Dietz HP. Urethral mobility and urinary incontinence. UOG. 2010;36:505–11.
Dietz HP, Clarke B, Herbison P. Bladder neck mobility and urethral closure pressure as predictors of genuine stress incontinence. Int Urogynecol J. 2002;13:289–93.
Abufaraj M, Xu T, Cao C, et al. Prevalence and trends in urinary incontinence among women in the United States, 2005-2018. Am J Obstet Gynecol. 2021;225(2):166.e1–e12.
Rortveit G, Hannestad YS, Daltveit AK, Hunskaar S. Age- and type-dependent effects of parity on urinary incontinence: the Norwegian EPINCONT study. Obstet Gynecol. 2001;98(6):1004–10.
Blomqis JL, Muñoz A, Carroll M, Handa VL. Association of delivery mode with pelvic floor disorders after childbirth. JAMA. 2018;320(23):2438–47.
Tähtinen RM, Cartwright R, Veronooij RWM, Rortveit G, Hunskaar S, Guyatt GH, et al. Long-term risks of stress and urgency urinary incontinence after different vaginal delivery modes. Am J Obstet Gynecol. 2019;220(2):181.e1–8.
Shek KL, Dietz HP, Kirby A. The effect of childbirth on urethral mobility. J Urol. 2010;184(2):629–34.
Dickie K, Shek KL, Dietz HP. The relationship between urethral mobility and parity. BJOG. 2010;117:1220–4.
Van Geelen JM, Lemmens WA, Eskes TK, Martin CB Jr. The urethral pressure profile in pregnancy and after delivery in healthy nulliparous women. Am J Obstet Gynecol. 1982;144:636–49.
Bump R, Mattiasson A, Bo K, Brubaker L, DeLancey J, Klarskov P, et al. The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol. 1996;175(1):10–7.
Dietz HP, Mann K. What is clinically relevant prolapse? An attempt at defining cutoffs for the clinical assessment of pelvic organ descent. Int Urogynecol J. 2014;25(4):451–5.
Rosier P, Schaefer W, Lose G, et al. International Continence Society Good Urodynamic Practices and Terms 2016: Urodynamics, uroflowmetry, cystometry, and pressure-flow study. Neurourol Urodyn. 2017;36(5):1243–60.
Kamisan Atan I, Lin S, Dietz HP, Herbison P. Wilson PD, for the ProLong Study Group. It is the first birth that does the damage: a cross-sectional study 20 years after delivery. Int Urogynecol J. 2018;29:1637–43.
Li YP, Shek KL, Subramaniam N, Friedman T, Dietz HP. Parity and anal sphincter trauma. Int Urogynecol J. 202. 31:553–6.
Atan IK, Gerges B, Shek KL, Dietz HP. The association between vaginal parity and hiatal dimensions: a retrospective observational study in a tertiary urogynaecological centre. BJOG. 2015;122:867–72.
Handa VL, Blomquist JL, Knoepp LR, Hoskey KA, McDermott KC, Munoz A. Pelvic floor disorders 5–10 years after vaginal or caesarean childbirth. Obstet Gynecol. 2011;118(4):777–84.
Rahmanou P, Caudwell-Hall J, Kamisan Atan I, Dietz HP. The association between maternal age at first delivery and risk of obstetric trauma. Am J Obstet Gynecol. 2016;215(451):e1–7.
Friedman T, Eslick GD, Dietz HP. Delivery mode and the risk of levator muscle avulsion: a meta-analysis. Int Urogynecol J. 2019;30(6):901–7.
Lino SA, Shek KL, Caudwell-Hall J, Gillor M, Dietz HP. Has the prevalence of levator avulsion after forceps delivery changed over the last six decades? A retrospective study in a urogynaecological population. EJOGRB. 2021;264:184–8.
Miller EBE, McDonald K, Gossett D. Association between obstetrician forceps volume and maternal and neonatal outcomes. Obstet Gynecol. 2014;123:248–54.
Perucchini D, DeLancey JO, Ashton-Miller JA, Peschers U, Kataria T. Age effects on urethral striated muscle. I. Changes in number and diameter of striated muscle fibers in the ventral urethra. Am J Obstet Gynecol. 2002;186(3):351–5.
Dietz HP, Clarke B. The urethral pressure profile and ultrasound imaging of the lower urinary tract. Int Urogynecol J. 2001;12(1):38–41.
Klarskov N, Lose G. Urethral pressure reflectometry and pressure profilometry in healthy volunteers and stress urinary incontinent women. Neurourol Urodyn. 2008;27:807–12.
Author information
Authors and Affiliations
Contributions
KL Shek: Project development, data analysis and interpretation, manuscript writing
HP Dietz: Project development, data collection, data analysis and interpretation, manuscript editing
Corresponding author
Ethics declarations
Conflicts of interest
The authors have received lecture honoraria and travel assistance from GE Medical and Mindray.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shek, K.L., Dietz, H.P. Is urethral pressure associated with parity and delivery mode?. Int Urogynecol J 33, 3435–3439 (2022). https://doi.org/10.1007/s00192-022-05233-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-022-05233-2