Abstract
Introduction and hypothesis
“Dropped pabd at void” occurs when pabd decreases below the previous resting pressure during voiding time. We sought clinical factors associated with this phenomenon and evaluated whether its correction modifies the urodynamic diagnosis.
Methods
Retrospective cross-sectional study of non-neurological consecutive symptomatic women. The following definitions were used: “dropped pabd at void”: decrease in pabd at Qmax ≥ 5 cmH2O; bladder outflow obstruction (BOO) (pdetQmax ≥ 25 cmH2O + Qmax ≤ 12 ml/s and female BOO index (pdetQmax – 2.2*Qmax) > 18; “low detrusor contraction strength”: PIP1 (pdetQmax + Qmax) < 30. In patients with “dropped pabd at void”, pdetQmax was corrected.
Results
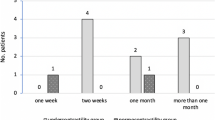
A total of 360 women were analyzed. Ninety-five percent of the women had a variation in pabd at Qmax between −13 and 53 cmH2O. “Dropped pabd at void” was found in 100 women (27.8%). History of stress urinary incontinence (SUI) surgery was significantly higher (p = 0.016) and symptoms of mixed urinary incontinence were significantly lower (p = 0.030) in patients with “dropped pabd at void”. On multivariate analysis only the history of SUI surgery maintained its significance (OR = 1.787 [95% CI: 1.058, 3.017], p = 0.030). When correcting pdetQmax in women with “dropped pabd at void”, 2 or 5 patients lost BOO diagnosis (depending on how it was diagnosed) and 7 patients gained a “low detrusor contraction strength” diagnosis.
Conclusions
Approximately one-quarter of women had “dropped pabd at void”, which was associated with a history of SUI surgery. Correction of pdetQmax would lead to a 2.5% to 3.33% diagnostic modification.

Similar content being viewed by others
References
Rademakers K, Apostolidis A, Constantinou C, et al. Recommendations for future development of contractility and obstruction nomograms for women. ICI-RS 2014, Neurourol Urodyn. 2016;35(2):307–11.
Smith PP, Valentini F, Mytilekas KV, et al. Can we improve our diagnosis of impaired detrusor contractility in women? An ICI-RS 2019 proposal. Neurourol Urodyn. 2020;39(Suppl 3):S43–9.
Devreese AM, Nuyens G, Staes F, et al. Do posture and straining influence urinary-flow parameters in normal women? Neurourol Urodyn. 2000;19(1):3–8.
Schaefer W, Clarkson B, Griffiths D, Tadic S, Resnick N. The urodynamics of voiding function in females: grading of bladder outflow conditions on a continuous scale. J Urol. 2011;185:e682.
Schäfer W. Analysis of active detrusor function during voiding with the bladder working function. Neurourol Urodyn. 1991;10:19–35.
Cormier L, Ferchaud J, Galas JM, Guillemin F, Mangin P. Diagnosis of female bladder outlet obstruction and relevance of the parameter area under the curve of detrusor pressure during voiding: preliminary results. J Urol. 2002;167(5):2083–7.
Defreitas GA, Zimmern PE, Lemack GE, Shariat SF. Refining diagnosis of anatomic female bladder outlet obstruction: comparison of pressure-flow study parameters in clinically obstructed women with those of normal controls. Urology. 2004;64(4):675–9 discussion 679–681.
Di Grazia E, Troyo Sanromán R, Aceves JG. Proposed urodynamic pressure-flow nomogram to diagnose female bladder outlet obstruction. Arch Ital Urol Androl. 2004;76(2):59–65.
Dybowski B, Bres-Niewada E, Radziszewski P. Pressure-flow nomogram for women with lower urinary tract symptoms. Arch Med Sci. 2014;10(4):752–6.
Tan TL, Bergmann MA, Griffiths D, Resnick NM. Stop test or pressure-flow study? Measuring detrusor contractility in older females. Neurourol Urodyn. 2004;23(3):184–9.
Rosier PFWM, Schaefer W, Lose G, et al. International Continence Society Good Urodynamic Practices and Terms 2016: urodynamics, uroflowmetry, cystometry, and pressure-flow study. Neurourol Urodyn. 2017;36(5):1243–60.
Abrams P, Cardozo L, Fall M, et al. The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Neurourol Urodyn. 2002;21(2):167–78.
Schäfer W, Abrams P, Liao L, et al. Good urodynamic practices: uroflowmetry, filling cystometry, and pressure-flow studies. Neurourol Urodyn. 2002;21(3):261–74.
Haylen BT, de Ridder D, Freeman RM, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J. 2010;21(1):5–26.
Chancellor MB, Rivas DA. American Urological Association Symptom Index for women with voiding symptoms: lack of index specificity for benign prostate hyperplasia. J Urol. 1993;150(5 Pt 2):1706–8.
Solomon E, Yasmin H, Duffy M, Rashid T, Akinluyi E, Greenwell TJ. Developing and validating a new nomogram for diagnosing bladder outlet obstruction in women. Neurourol Urodyn. 2018;37(1):368–78.
Soper D. Free statistics Calculator. Version 4.0. 2006–2022. Post-hoc statistical power calculator for multiple regression. https://www.danielsoper.com/statcalc/calculator.aspx?id=9. Accessed 2 March 2022.
Griffiths DJ, Höfner K, van Mastrigt R, et al. The standardisation of terminology of lower urinary tract function: pressure-flow studies of voiding, urethral resistance and urethral obstruction. Neurourol Urodyn. 1997;16(1):1–18.
Karram MM, Partoll L, Bilotta V, Angel O. Factors affecting detrusor contraction strength during voiding in women. Obstet Gynecol. 1997;90(5):723–6.
Nygaard I, Kreder K, Mueller E, et al. Does urethral competence affect urodynamic voiding parameters in women with prolapse? Neurourol Urodyn. 2007;26(7):1030–5.
Pauwels E, De Laet K, De Wachter S, Wyndaele JJ. Healthy, middle-aged, history-free, continent women—do they strain to void? J Urol. 2006;175(4):1403–7.
Bhatia NN, Bergman A, Karram M. Changes in urethral resistance after surgery for stress incontinence. Urology. 1989;34:200–4.
Gammie A. Artefacts in urodynamics. In: Drake M, Hashim H, Gammie A, editors. Abrams’ Urodynamics. 4th ed: Wiley; 2021. p. 383–93.
Abrams P. Bladder outlet obstruction index, bladder contractility index and bladder voiding efficiency: three simple indices to define bladder voiding function. BJU Int. 1999;84(1):14–5.
Valentini FA, Marti BG, Robain G, Zimern PE, Nelson PP. Comparison of indices allowing an evaluation of detrusor contractility in women. Prog Urol. 2020;30(7):396–401.
Acknowledgements
We thank Ariel Castro-Lara, MSc in Clinical Epidemiology, from the “Oficina de Apoyo a la Investigación Clínica”, Hospital Clínico Universidad de Chile, for his important assistance in the calculation of the post-hoc statistical power of the multivariate regression model.
Author information
Authors and Affiliations
Contributions
J.P. Valdevenito: protocol/project development, data collection or management, data analysis, manuscript writing/editing; A. Mercado-Campero, L. López-Fando, C.I. Calvo, V. Manríquez, L. Medina: data analysis, manuscript writing/editing.
Corresponding author
Ethics declarations
Conflicts of interests
J.P. Valdevenito, A. Mercado-Campero, C.I. Calvo, V. Manríquez, L. Medina: nothing to disclose. L. López-Fando: speaker’s fees from Astellas, Coloplast, Neomedic, not related to this study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Valdevenito, J.P., Mercado-Campero, A., López-Fando, L. et al. Dropped abdominal pressure at void in women. Int Urogynecol J 33, 3275–3281 (2022). https://doi.org/10.1007/s00192-022-05202-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-022-05202-9