Abstract
Introduction and hypothesis
To determine whether delayed administration of CXCL12 alters anorectal manometric pressures and histology in rats following anal sphincterotomy compared to primary surgical repair alone.
Methods
Adult female rats were divided into three groups: A, a control group that did not undergo surgery; B, anal sphincterotomy with primary surgical repair; C, anal sphincterotomy with primary surgical repair and intra-sphincteric injection of CXCL12 at 6 weeks post-injury. All rats underwent anal manometry measurements at baseline and at 6 and 12 weeks post-injury. Histologic analysis of the anal sphincters was also performed.
Results
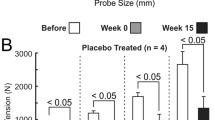
At baseline and 6 weeks, there were no statistically significant differences among D, Tmax and P∆ of Groups A, B and C. At 12-week manometry, the total duration of contractions on anal manometry was significantly less in Group C compared to Groups A and B (3.65, 5.5, 5.3 p < 0.01) as was time to peak of contraction at 12 weeks (1.6, 2.1, 3.1, p < 0.01); however, group C had a significantly higher P∆ at 12 weeks compared to Groups A and B (2.25, 1.4, 0.34, p < 0.01). There were no statistically significant differences in the ratio of muscle to collagen at the site of injury; however, muscle fibers were significantly smaller in group C and less per bundle than the other groups.
Conclusions
Administration of chemokine therapy at 6 weeks post-repair using CXCL12 enhanced the magnitude of anal sphincter contractions in a rat model of anal sphincter injury but decreased overall duration of contraction. Increased anal sphincter contraction magnitude was not explained by histologic differences in explanted specimens.


Similar content being viewed by others
Abbreviations
- Group A:
-
No intervention group
- Group B:
-
Sphincterotomy and primary repair
- Group C:
-
Sphincterotomy, primary repair and CXCL12
- D:
-
Duration of contraction
- Tmax :
-
Time to peak of contraction
- PΔ:
-
Change in contraction pressure from baseline
References
Snooks SJ, Henry MM, Swash M. Faecal incontinence due to external anal sphincter division in childbirth is associated with damage to the innervation of the pelvic floor musculature: a double pathology. Br J Obstet Gynaecol. 1985;92(8):824–8 5.
Allen RE, et al. Pelvic floor damage and childbirth: a neurophysiological study. Br J Obstet Gynaecol. 1990;97(9):770–9 6.
Sandridge DA, et al. Vaginal delivery is associated with occult disruption of the anal sphincter mechanism. Am J Perinatol. 1997;14(9):527–33 7.
Sultan AH, Kamm MA, Hudson CN, et al. Third Degree Obstetric Anal Sphincter Tears. British Med J. 1994;308(6933):887–91.
Gearhart S, Hull T, Floruta C, et al. Anal manometric parameters: predictors of outcome following anal sphincter repair? J Gastrointestinal Surg. 2005;9(1):115–20. https://doi.org/10.1016/j.gassur.2004.04.001.
Sangwan YP, Solla JA. Internal anal sphincter: advances and insights. Dis Colon Rectum. 1998;41(10):1297–311. https://doi.org/10.1007/bf02258232.
Chaliha C, Sultan A, Bland J, et al. Anal function: Effect of pregnancy and delivery. Am J Obstet Gynecol. 2001;185(2):427–32.
Hamdy S, Enck P, Aziz Q, et al. Laterality effects of human pudendal nerve stimulation on corticoanal pathways: evidence for functional asymmetry. Gut. 1999;45(1):58–63.
Azpiroz F, Fernandez-Fraga X, Merletti R, et al. The puborectalis muscle. Neurogastroenterol Motil. 2005;17:68–72.
Alavi K, Chan S, Wise P, et al. Fecal Incontinence: Etiology, Diagnosis, and Management. J Gastrointest Surg. 2015;19(10):1910–21. https://doi.org/10.1007/s11605-015-2905-1.
Saldana Ruiz N, Kaiser AM. Fecal incontinence - Challenges and solutions. World J Gastroenterol. 2017;23(1):11–24. https://doi.org/10.3748/wjg.v23.i1.11.
Lane FL, et al. In vivo recovery of the injured anal sphincter after repair and injection of myogenic stem cells: an experimental model. Dis Colon Rectum. 2013;56(11):1290–7 27.
Aghaee-Afshar M, et al. Potential of human umbilical cord matrix and rabbit bone marrow-derived mesenchymal stem cells in repair of surgically incised rabbit external anal sphincter. Dis Colon Rectum. 2009;52(10):1753–61 28.
Kajbafzadeh AM, et al. Functional external anal sphincter reconstruction for treatment of anal incontinence using muscle progenitor cell auto grafting. Dis Colon Rectum. 2010;53(10):1415–21 29.
Oh HK, et al. Functional and histological evidence for the targeted therapy using biocompatible polycaprolactone beads and autologous myoblasts in a dog model of fecal incontinence. Dis Colon Rectum. 2015;58(5):517–25.
Cottler-Fox MH, et al. Stem cell mobilization. Hematology Am Soc Hematol Educ Program. 2003;2003:419–37 34.
Lapidot T, Petit I. Current understanding of stem cell mobilization: the roles of chemokines, proteolytic enzymes, adhesion molecules, cytokines, and stromal cells. Exp Hematol. 2002;30(9):973–81.
Williams JK, et al. Cell versus chemokine therapy in a nonhuman primate model of chronic intrinsic urinary sphincter deficiency. J Urol. 2016;196(6):1809–15.
Koudy Williams J, et al. Efficacy and initial safety profile of CXCL12 treatment in a rodent model of urinary sphincter deficiency. Stem Cells Transl Med. 2017;6(8):1740–6.
Salcedo L, et al. Chemokine upregulation in response to anal sphincter and pudendal nerve injury: potential signals for stem cell homing. Int J Color Dis. 2011;26(12):1577–81.
Sideris M, McCaughey T, Hanrahan JG, et al. Risk of obstetric anal sphincter injuries (OASIS) and anal incontinence: A meta-analysis. Eur J Obstet Gynecol Reprod Biol. 2020;252:303–12. https://doi.org/10.1016/j.ejogrb.2020.06.048.
Sun L, Xie Z, Kuang M, et al. Regenerating the Anal Sphincter: Cytokines, Stem Cells, or Both? Dis Colon Rectum. 2017;60(4):416–25. https://doi.org/10.1097/dcr.0000000000000783.
Sun L, Kuang M, Penn M et al. Stromal Cell-Derived Factor 1 Plasmid Regenerates Both Smooth and Skeletal Muscle After Anal Sphincter Injury in the Long Term. Dis Colon Rectum. 2017;60(12). Retrieved from https://journals.lww.com/dcrjournal/Fulltext/2017/12000/Stromal_Cell_Derived_Factor_1_Plasmid_Regenerates.16.aspx
Salcedo L, Damaser M, Butler R, et al. Long-term effects on pressure and electromyography in a rat model of anal sphincter injury. Dis Colon Rectum. 2010;53(8):1209–17. https://doi.org/10.1007/DCR.0b013e3181de7fe0.
Zutshi M, Salcedo LB, Zaszczurynski PJ, et al. Effects of sphincterotomy and pudendal nerve transection on the anal sphincter in a rat model. Dis Colon Rectum. 2009;52(7):1321–9. https://doi.org/10.1007/DCR.0b013e31819f746d.
Vinograd I, Hanani M, Hadary A, et al. Animal model for the study of internal anal sphincter activity. Eur Surg Res. 1985;17(4):259–63. https://doi.org/10.1159/000128476.
Trébol J, Georgiev-Hristov T, Vega-Clemente L, et al. Rat model of anal sphincter injury and two approaches for stem cell administration. World J Stem Cells. 2018;10(1):1–14. https://doi.org/10.4252/wjsc.v10.i1.1.
Gras S, Tolstrup CK, Lose G. Regenerative medicine provides alternative strategies for the treatment of anal incontinence. Int Urogynecol J. 2017;28(3):341–50.
Wai CY, Rahn DD, White AB et al. Recovery of External Anal Sphincter Contractile Function After Prolonged Vaginal Distention or Sphincter Transection in an Animal Model. Obstet Gynecol. 2008;111(6). Retrieved from https://journals.lww.com/greenjournal/Fulltext/2008/06000/Recovery_of_External_Anal_Sphincter_Contractile.25.aspx
Author information
Authors and Affiliations
Contributions
AS El Haraki: Rat measurements and surgery, data analysis and manuscript writing
S Lankford: Rat measurements, data collection and surgery
Wencheng Li: qualitative histologic analysis
JK Williams: Project development, manuscript editing
C Matthews: Manuscript writing
GH Badlani: Principal investigator, project development, manuscript editing
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
El Haraki, A.S., Lankford, S., Li, W. et al. Chemokine therapy for anal sphincter injury in a rat model: a pilot study. Int Urogynecol J 33, 3283–3289 (2022). https://doi.org/10.1007/s00192-022-05195-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-022-05195-5