Abstract
Introduction and hypothesis
To compare vaginal mesh exposure rates, adverse events and composite failure within 1 year postoperatively in patients who undergo vaginal hysterectomy with vaginal mesh attachment (TVH) versus laparoscopic hysterectomy with abdominal mesh attachment (TLH) for minimally invasive sacrocolpopexy.
Methods
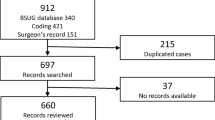
This multicenter retrospective cohort study is a secondary analysis of data collected retrospectively at one institution and the multicenter randomized control PACT trial. Women were excluded for no follow-up between 9 months and 2 years postoperatively or undergoing concurrent non-urogynecologic procedures.
Results
Between 2010 and 2019, 182 patients underwent TLH and 132 TVH. There were 15 (4.8%) vaginal mesh exposures: 12 (6.6%) in the TLH and 3 (2.3%) in the TVH group (p = 0.133) with zero mesh erosions. Logistic regression analysis for mesh exposure in the TLH vs. TVH groups controlling for BMI, posterior repair and surgeon training also showed no significant difference (OR 4.8, 95% CI 0.94, 24.8, p = 0.059). The overall intraoperative complication rate was low (19/314, 6.1%) with a higher rate of bladder injury in the TLH group (4.4% vs. 0.8%, p = 0.049). The TLH group had a higher rate of UTI (8.2% vs. 2.3%, p = 0.027) and clean intermittent catheterization (11% vs. 3%, p = 0.009). At 1-year follow-up, there was no difference in composite failure (6%), bulge symptoms (5%) or retreatment (1%) between groups.
Conclusions
At 1 year, there is no significant difference in vaginal mesh exposure rates between vaginal hysterectomy with vaginal mesh attachment and laparoscopic hysterectomy with abdominal mesh attachment. Both groups have equal efficacy with low rates of complications.
Similar content being viewed by others
References
Wu JM, Matthews CA, Conover MM, Pate V, Jonsson FM. Lifetime risk of stress urinary incontinence or pelvic organ prolapse surgery. Obstet Gynecol. 2014;123(6):1201–6. https://doi.org/10.1097/AOG.0000000000000286.
Smith FJ, Holman CD, Moorin RE, Tsokos N. Lifetime risk of undergoing surgery for pelvic organ prolapse. Obstet Gynecol. 2010;116(5):1096–100. https://doi.org/10.1097/AOG.0b013e3181f73729.
Nygaard I, Brubaker L, Zyczynski HM, Cundiff G, Richter H, Gantz M, Fine P, Menefee S, Ridgeway B, Visco A, Warren LK, Zhang M, Meikle S. Long-term outcomes following abdominal sacrocolpopexy for pelvic organ prolapse. JAMA. 2013;309(19):2016–24. https://doi.org/10.1001/jama.2013.4919. Erratum in: JAMA. 2013 Sep 11;310(10):1076.
Klauschie JL, Cornella JL. Surgical treatment of vaginal vault prolapse: a historic summary and review of outcomes. Female Pelvic Med Reconstr Surg. 2012;18(1):10–7. https://doi.org/10.1097/SPV.0b013e3182404189.
Paraiso MF, Walters MD, Rackley RR, Melek S, Hugney C. Laparoscopic and abdominal sacral colpopexies: a comparative cohort study. Am J Obstet Gynecol. 2005;192(5):1752–8. https://doi.org/10.1016/j.ajog.2004.11.051.
Wang LC, Al Hussein Al Awamlh B, Hu JC, Laudano MA, Davison WL, Schulster ML, Zhao F, Chughtai B, Lee RK. Trends in mesh use for pelvic organ prolapse repair from the medicare database. Urology. 2015;86(5):885–91. https://doi.org/10.1016/j.urology.2015.08.022.
Winkelman WD, Modest AM, Richardson ML. The surgical approach to abdominal sacrocolpopexy and concurrent hysterectomy: trends for the past decade. Female Pelvic Med Reconstr Surg. 2021;27(1):e196–201. https://doi.org/10.1097/SPV.0000000000000891.
Matthews CA, Geller EJ, Henley BR, Kenton K, Myers EM, Dieter AA, Parnell B, Lewicky-Gaupp C, Mueller MG, Wu JM. Permanent compared with absorbable suture for vaginal mesh fixation during total hysterectomy and sacrocolpopexy: a randomized controlled trial. Obstet Gynecol. 2020;136(2):355–64. https://doi.org/10.1097/AOG.0000000000003884.
Tan-Kim J, Menefee SA, Luber KM, Nager CW, Lukacz ES. Prevalence and risk factors for mesh erosion after laparoscopic-assisted sacrocolpopexy. Int Urogynecol J. 2011;22(2):205–12. https://doi.org/10.1007/s00192-010-1265-3.
Warner WB, Vora S, Hurtado EA, Welgoss JA, Horbach NS, von Pechmann WS. Effect of operative technique on mesh exposure in laparoscopic sacrocolpopexy. Female Pelvic Med Reconstr Surg. 2012;18(2):113–7. https://doi.org/10.1097/SPV.0b013e318249bd54.
Cundiff GW, Varner E, Visco AG, Zyczynski HM, Nager CW, Norton PA, Schaffer J, Brown MB, Brubaker L; Pelvic Floor Disorders Network. Risk factors for mesh/suture erosion following sacral colpopexy. Am J Obstet Gynecol. 2008;199(6):688.e1–5. https://doi.org/10.1016/j.ajog.2008.07.029.
Akyol A, Akca A, Ulker V, Gedikbasi A, Kublay A, Han A, Ark HC, Numanoglu C. Additional surgical risk factors and patient characteristics for mesh erosion after abdominal sacrocolpopexy. J Obstet Gynaecol Res. 2014;40(5):1368–74. https://doi.org/10.1111/jog.12363.
Bensinger G, Lind L, Lesser M, Guess M, Winkler HA. Abdominal sacral suspensions: analysis of complications using permanent mesh. Am J Obstet Gynecol. 2005;193(6):2094–8. https://doi.org/10.1016/j.ajog.2005.07.066.
Osmundsen BC, Clark A, Goldsmith C, Adams K, Denman MA, Edwards R, Gregory WT. Mesh erosion in robotic sacrocolpopexy. Female Pelvic Med Reconstr Surg. 2012;18(2):86–8. https://doi.org/10.1097/SPV.0b013e318246806d. Erratum in: Female Pelvic Med Reconstr Surg. 2012;18(4):255.
Nosti PA, Carter CM, Sokol AI, Tefera E, Iglesia CB, Park AJ, Gutman RE. Transvaginal versus transabdominal placement of synthetic mesh at time of sacrocolpopexy. Female Pelvic Med Reconstr Surg. 2016;22(3):151–5. https://doi.org/10.1097/SPV.0000000000000222.
Davidson ERW, Thomas TN, Lampert EJ, Paraiso MFR, Ferrando CA. Route of hysterectomy during minimally invasive sacrocolpopexy does not affect postoperative outcomes. Int Urogynecol J. 2019;30(4):649–55. https://doi.org/10.1007/s00192-018-3790-4.
Jones K, Thompson N, Imamoglu G, Solomon E, Rastegar V, Harmanli O. Short-term outcomes of vaginal hysterectomy at the time of robotic sacrocolpopexy. Female Pelvic Med Reconstr Surg. 2021;27(1):e223–6. https://doi.org/10.1097/SPV.0000000000000898.
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibañes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250(2):187–96. https://doi.org/10.1097/SLA.0b013e3181b13ca2.
Woodburn KL, Bradley SE, Ward SA, et al. Assessing the impact of vaginal hysterectomy with vaginal mesh attachment on outcomes and complications during minimally invasive sacrocolpopexy. [Short Oral 98]. Short orals. Female Pelvic Med Reconstr Surg. 2020;26(10S):S21-S77. https://doi.org/10.1097/SPV.0000000000000934.
Acknowledgements
The authors thank and acknowledge the participants and authors of the PACT study.
Author information
Authors and Affiliations
Contributions
KL Woodburn: Project development, data collection and analysis, manuscript writing.
A El Haraki: Project development, data collection, manuscript editing.
AI Sokol: Project development, manuscript editing.
RE Gutman: Project development, manuscript editing.
CA Matthews: Project development, data analysis, manuscript writing.
Corresponding author
Ethics declarations
Conflicts of interest
Dr. Matthews has received grant funding and consulting fees from Boston Scientific Corporation. She is an expert witness for Johnson & Johnson.
Dr. Gutman has received grant funding and consulting fees from Boston Scientific. He is an expert witness for Johnson & Johnson slings.
Dr. Sokol is an expert witness for Johnson & Johnson.
The other authors have no disclosures.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Woodburn, K.L., El Haraki, A.S., Sokol, A.I. et al. Mesh Exposure Following Vaginal Versus Laparoscopic Hysterectomy at the Time of Sacrocolpopexy. Int Urogynecol J 33, 3213–3220 (2022). https://doi.org/10.1007/s00192-022-05093-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-022-05093-w