Abstract
Introduction and hypothesis
The objective was to assess the effectiveness of pelvic floor exercises performed with electromyographic (EMG) biofeedback or a vaginal cone on incontinence severity, muscle strength, social activity level, quality of life, treatment success, and treatment satisfaction in women with stress urinary incontinence (SUI).
Methods
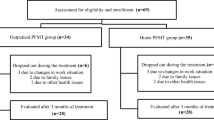
This prospective, randomized study included 40 female patients diagnosed with SUI. Patients were randomly divided into two groups as the group receiving pelvic floor muscle exercise (PFME) with a vaginal cone at home (n = 20) and the group receiving PFME with EMG biofeedback in the hospital (n = 20). The measurement of urinary incontinence severity with a 1-h pad test, assessment of social activity with the social activity index (SAI), assessment of incontinence-specific quality of life, manual measurement of pelvic floor muscle strength, and the assessment of treatment satisfaction were performed in the pre-treatment period and post-treatment at 3 and 6 months.
Results
In intragroup analyses, an improvement was observed in both groups in the pad test, muscle strength, SAI, quality of life, and treatment satisfaction measurement compared with the pre-treatment period (p < 0.05). No significant difference was found between the groups in terms of assessment parameters in intergroup analyses during follow-up (p > 0.05).
Conclusion
It was concluded that both EMG biofeedback assisted PFME and PFME with a vaginal cone had curative effects on incontinence in patients with SUI. We believe that both protocols can be used as acceptable and effective conservative therapy methods in the treatment of women with SUI considering their preference.

Similar content being viewed by others
References
Langa KM, Fultz NH, Saint S, et al. Informal caregiving time and costs for urinary incontinence in older individuals in the United States. J Am Geriatr Soc. 2002;50:733–7.
Melville JL, Katon W, Delaney K, et al. Urinary incontinence in US women: a population-based 369 study. Arch Intern Med. 2005;165:537–42.
Haylen BT, Ridder D, Freeman RM, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Neurourol Urodyn. 2020;29:4–20.
Moroni R, Magnani P, Haddad J, et al. Conservative treatment of stress urinary incontinence: a systematic review with meta-analysis of randomized controlled trials. Rev Bras Ginecol Obstet. 2016;38:97–111.
Dumoulin C, Hay Smith EJC, Mac Habée-Séguin G. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women. Cochrane Database Syst Rev. 2014;14:CD005654.
Bo K, Frawley HC, Haylen BT, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for the conservative and nonpharmacological management of female pelvic floor dysfunction. Neurourol Urodyn. 2017;36:221–44.
Hagen S, Elders A , Stratton S, et al. Effectiveness of pelvic floor muscle training with and without electromyographic biofeedback for urinary incontinence in women: multicentre randomised controlled trial. BMJ 2020;371:m3719.
Burns PA, Pranikoff K, Nochajski TH, et al. A comparison of effectiveness of biofeedback and pelvic floor muscle exercise treatment of stress incontinence in older community-dwelling women. J Gerontol. 1993;48:167–74.
Karantanis E, Allen W, Stevermer L. The repeatability of the 24 hour pad test centre for health service development. Int Urogynecol J Pelvic Floor Dysfunct. 2005;16:63–8.
Volloyhaug I, Morkved S, Salvasen O, et al. Assessment of pelvic floor muscle contraction with palpation, perineometry and transperineal ultrasound: a cross-sectional study. Ultrasound Obstet Gynecol. 2016;47:768–73.
Aksac B, Aki S, Karan A, et al. Biofeedback and pelvic floor exercises for the rehabilitation of urinary stress incontinence. Gynecol Obstet Invest. 2003;56:23–27
Cetin C, Sakallı M, Ay P. Validation of the short form of the incontinence impact questionnaire (IIQ-7) and the urogenital distress inventory (UDI6) in a Turkish population. Neurourol Urodyn. 2007;26:129–33.
Shah AD, Massagli MP, Kohli N, et al. A reliable, valid instrument to assess patient knowledge about urinary incontinence and pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19:1283–9.
Faiena I, Patel N, Parihar JS, et al. Conservative management of urinary incontinence in women. Rev Urol. 2015;17:129–39.
Hay-Smith EJ, Bo K, Berghmans LC, et al. Pelvic floor muscle training for urinary incontinence in women. Cochrane Database Syst Rev 2007;(1):CD001407.
Qaseem A, Dallas P, Forciea MA, et al. Nonsurgical management of urinary incontinence in women: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2014;161:429–40.
Gómez MFL, Abuín JMS, Criado FJG, et al. Treatment of stress urinary incontinence with perineal biofeedback by using superficial electrodes. Actas Urol Esp. 2008;32:629–36.
Huebner M, Riegel K, Hinninghofen H, et al. Pelvic floor muscle training for stress urinary incontinence: a randomized, controlled trial comparing different conservative therapies. Physiother Res Int. 2011;16:133–40.
Bø K, Talseth T, Holme I. Single blind, randomised controlled trial of pelvic floor exercises, electrical stimulation, vaginal cones, and no treatment in management of genuine stress incontinence in women. BMJ. 1999;318:487–93.
Santos PFD, Oliveira E, Zanetti MRD, et al. Electrical stimulation of the pelvic floor versus vaginal cone therapy for the treatment of stress urinary incontinence. Rev Bras Ginecol Obstet. 2009;31:447–52.
Funding
We do not have any financial relationship for this research and no conflicts of interest.
Author information
Authors and Affiliations
Contributions
N. Sahin: project development, data collection, manuscript writing; H. Yesil: data collection, analyzing, manuscript writing; B. Gorcan: project development, data collection, manuscript writing.
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sahin, N., Yesil, H. & Gorcan, B. The effect of pelvic floor exercises performed with EMG biofeedback or a vaginal cone on incontinence severity, pelvic floor muscle strength, and quality of life in women with stress urinary incontinence: a randomized, 6-month follow-up study. Int Urogynecol J 33, 2773–2779 (2022). https://doi.org/10.1007/s00192-021-05006-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-021-05006-3