Abstract
Introduction and hypothesis
This study aimed to estimate the incidence of fecal incontinence (FI) and identify risk factors in a cohort of older individuals.
Methods
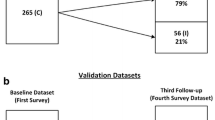
In 2006, individuals aged ≥ 60 years were selected from the SABE study. The dependent variable was FI in 2010. FI was assessed using the question: “In the last 12 months, have you ever lost control of bowel movements or stools?” Incidence was measured in units of per 1000 person-years. Multivariate analysis was used to assess risk factors for FI.
Results
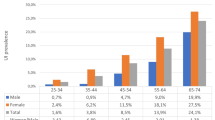
This study was the first to examine the incidence of FI in older Brazilian individuals. In total, 1413 individuals were included; mean age was 74.5 years, and 864 (61.8%) participants were women. FI prevalence rates were 4.7% for men and 7.3% for women. Incidence rate of FI was 16.3 and 22.2 per 1000 person-years for men and women, respectively. The risk of FI was greater among women aged ≥ 75 years, with severe symptoms of depression, cancer (other than skin) and chronic obstructive pulmonary disease (COPD). In men, the risk of FI was greater among those with poor literacy (up to 3 years of schooling), an Instrumental Activities of Daily Living (IADL) category of 1–4 and those who self-reported “bad/very bad” health status.
Conclusions
The FI incidence rate was high. The identified risk factors were age ≥ 75 years, with severe symptoms of depression, cancer and COPD (women); having up to 8 years of schooling; IADL category of 1–4 and self-reported health status (men).

Similar content being viewed by others
References
Rezvan A, Jakus-Waldman S, Abbas MA, Yazdany T, Nguyen J. Review of the diagnosis, management and treatment of fecal incontinence. Female Pelvic Med Reconstr Surg. 2015;21(1):8–17.
Sultan AH, Monga A, Lee J, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female anorectal dysfunction. Neurourol Urodyn. 2017;36(1):10–34.
Nelson RL, Norton N, Cautley E, et al. Comumunity-based prevalence of anal incontinence. JAMA. 1995;274:559–62.
Sharma A, Yuan L, Marshall RJ, et al. Systematic review of the prevalence of faecal incontinence. Br J Surg. 2016;103(12):1589–97.
Lopes MC, Teixeira MG, Jacob Filho W, et al. Prevalence of anal incontinence in the elderly population: an epidemiological study of the elderly population served at the geriatric ambulatory service of the Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo. Rev Hosp Clin Fac Med Sao Paulo. 1997;52(1):1–12.
Tamanini JTN, de Jesus FA, Castro RA, et al. The prevalence of fecal incontinence and associated risk factors in older adults participating in the SABE study. Neurourol Urodyn. 2016;35(8):959–64.
Palloni A, Pelaez M. SABE: Survey on health and well-being of elders: preliminary report. Washington, DC: Pan American Health Organization; 2002. Available at: www.ssc.wisc.edu/sabe/docs/informeFinal%20Ingles%20noviembre%202004. Accessed 16 Oct 2016.
Tamanini JT, Dambros M, D’Ancona CA, et al. Validation of the “International Consultation on Incontinence Questionnaire – Short Form” (ICIQ-SF) for Portuguese. Rev Saude Publica. 2004;38:438–44.
Silveira MS, Almeida JC, Freire RS, et al. Psychometric properties of the quality of life assessment instrument: 12-item health survey (SF-12). Cienc Saude Colet. 2013;18(7):1923–31.
Paradela EM, Lourenço RA, Veras RP, et al. Validation of geriatric depression scale in a general outpatient clinic. Rev Saude Publica. 2005;39(6):918–23.
Peduzzi P, Concato J, Kemper E, et al. A simulation study of the number of events per variable in logistic regression analysis. J Clin Epidemiol. 1996;49(12):1373–9.
Bharucha AE, Dunivan G, Goode PS, et al. Epidemiology, pathophysiology, and classification of fecal incontinence: state of the science summary for the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) workshop. Am J Gastroenterol. 2015;110(1):127–36.
Roslani AC, Ramakrishnan R, Azmi S, et al. Prevalence of faecal incontinence and its related factors among patients in a Malaysian academic setting. BMC Gastroenterol. 2014;14:95.
Ng K-S, Nassar N, Hamd K, et al. Prevalence of functional bowel disorders and faecal incontinence: an Australian primary care survey. Color Dis. 2014;17(2):150–9.
Saga S, Vinsnes AG, Mørkved S, et al. Prevalence and correlates of fecal incontinence among nursing home residents: a population-based cross-sectional study. BMC Geriatr. 2013;13:87.
Markland AD, Goode PS, Burgio KL, et al. Incidence and risk factors for fecal incontinence in black and white older adults: a population-based study. J Am Geriatr Soc. 2010;58(7):1341–6.
Cheetham MJ, Malouf AJ, Kamm MA. Fecal incontinence. Gastroenterol Clin N Am. 2001;30(1):115–30.
D’Orsi E, Xavier AJ, Steptoe A, et al. Socioeconomic and lifestyle factors related to instrumental activity of daily living dynamics: results from the English Longitudinal Study of Ageing. J Am Geriatr Soc. 2014;62(9):1630–9.
Goode PS, Burgio KS, Halli AD, et al. Prevalence and correlates of fecal incontinence in community-dwelling older adults. J Am Geriatr Soc. 2005;53(4):629–35.
Uduak UA, Vaughan CP, Burgio KL, et al. Shared risk factors for constipation, fecal incontinence, and combined symptoms in older U.S. adults. J Am Geriatr Soc. 2016;64(11):e183–8.
Stenzelius K, Mattiasson A, Hallberg IR, et al. Symptoms of urinary and faecal incontinence among men and women 75+ in relations to health complaints and quality of life. Neurourol Urodyn. 2004;23(3):211–22.
Deutekom M, Terra MP, Dobben AC, et al. Impact of faecal incontinence severity on health domains. Color Dis. 2005;7(3):263–9.
Heilbrun ME, Nygaard IE, Lockhart ME, et al. Correlation between levator ani muscle injuries on magnetic resonance imaging and fecal incontinence, pelvic organ prolapse, and urinary incontinence in primiparous women. Am J Obstet Gynecol. 2010;202(5):488.e1–6.
Huebner M, Gramlich NK, Rothmund R, et al. Fecal incontinence after obstetric anal sphincter injuries. Int J Gynaecol Obstet. 2013;121(1):74–7.
Lewicky-Gaupp C, Brincat C, Yousuf A, et al. Fecal incontinence in older women: are levator ani defects a factor? Am J Obstet Gynecol. 2010;202(5):491.e1–6.
Townsend DC, Carrington EV, Grossi U, et al. Pathophysiology of fecal incontinence differs between men and women: a case-matched study in 200 patients. Neurogastroenterol Motil. 2016;28(10):1580–8.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tamanini, J.T.N., Franceschi Júnior, O., Santos, J.L.F. et al. Fecal incontinence: incidence and risk factors from the SABE (Health, Wellbeing and Aging) study. Int Urogynecol J 33, 2993–3004 (2022). https://doi.org/10.1007/s00192-021-04914-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-021-04914-8