Abstract
Introduction and hypothesis
The objective was to report the management of post-operative urinary incontinence after midurethral sling (MUS) revision for chronic pelvic pain (CPP), and to report functional outcomes.
Methods
From November 2004 to February 2018, a total of 89 women who underwent removal or section of MUS for CPP, were enrolled. Patients were divided into the transobturator tape (TOT) group (50 patients) and the tension-free vaginal tape (TVT) group (37 patients); 2 patients had had both slings implanted. We report the rate of stress urinary incontinence (SUI) recurrence, the rate of de novo urge urinary incontinence (UUI), the need for subsequent SUI or UUI surgery, and functional outcomes (pain and continence).
Results
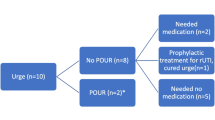
Median follow-up was 41.4 months [0.9–138.8]. SUI recurrence or de novo UUI occurred in 52 cases (58.4%): 19 (51.3%) patients in the TVT group, 31 (62%) in the TOT group, and both patients (100%) who underwent total removal of both slings. Among patients with SUI recurrence or de novo UUI, 39 (75%) had pain relief after sling removal. Seventeen patients (32.6%) refused any treatment, 14 (26.9%) were cured with conservative therapy, and 21 (40.3%) underwent SUI or UUI surgery. One patient had de novo pelvic pain after reoperation. The overall continence rate for all patients who underwent sling revision was 82% (73 out of 89) at the last follow-up.
Conclusion
After MUS revision for CPP, post-operative UI may occur in 58.4% of patients, of which, one-fourth may be managed with conservative measures only. Forty percent of them had redo surgery with a low risk of pain recurrence and a high rate of urinary continence.

Similar content being viewed by others
References
Lucas MG, Bosch RJL, Burkhard FC, et al. EAU guidelines on surgical treatment of urinary incontinence. Eur Urol. 2012;62:1118–29. https://doi.org/10.1016/j.eururo.2012.09.023.
Gurol-Urganci I, Geary RS, Mamza JB, et al. Long-term rate of mesh sling removal following midurethral mesh sling insertion among women with stress urinary incontinence. JAMA. 2018;320:1659–69. https://doi.org/10.1001/jama.2018.14997.
Ford AA, Rogerson L, Cody JD, et al. Mid-urethral sling operations for stress urinary incontinence in women. Cochrane Database Syst Rev. 2017;7:CD006375. https://doi.org/10.1002/14651858.CD006375.pub4.
Richter HE, Albo ME, Zyczynski HM, et al. Retropubic versus transobturator midurethral slings for stress incontinence. N Engl J Med. 2010;362:2066–76. https://doi.org/10.1056/NEJMoa0912658.
Berger AA, Tan-Kim J, Menefee SA. Long-term risk of reoperation after synthetic mesh midurethral sling surgery for stress urinary incontinence. Obstet Gynecol. 2019;134:1047–55. https://doi.org/10.1097/AOG.0000000000003526.
Latthe PM, Foon R, Toozs-Hobson P. Transobturator and retropubic tape procedures in stress urinary incontinence: a systematic review and meta-analysis of effectiveness and complications. BJOG. 2007;114:522–31. https://doi.org/10.1111/j.1471-0528.2007.01268.x.
Bourrat M, Armand C, Seffert P, Tostain J. Complications and medium-term functional results of TVT in stress urinary incontinence. Prog Urol. 2003;13:1358–64.
Leonard G, Perrouin-Verbe M-A, Levesque A, et al. Place of surgery in the management of post-operative chronic pain after placement of prosthetic material based on a series of 107 cases. Neurourol Urodyn. 2018;37:2177–83. https://doi.org/10.1002/nau.23544.
Palva K, Nilsson CG. Effectiveness of the TVT procedure as a repeat mid-urethra operation for treatment of stress incontinence. Int Urogynecol J Pelvic Floor Dysfunct. 2009;20:769–74. https://doi.org/10.1007/s00192-009-0849-2.
Parden AM, Gleason JL, Jauk V, et al. Incontinence outcomes in women undergoing primary and repeat midurethral sling procedures. Obstet Gynecol. 2013;121:273–8. https://doi.org/10.1097/AOG.0b013e31827c5de7.
Stav K, Dwyer PL, Rosamilia A, et al. Repeat synthetic mid urethral sling procedure for women with recurrent stress urinary incontinence. J Urol. 2010;183:241–6. https://doi.org/10.1016/j.juro.2009.08.111.
Rigaud J, Pothin P, Labat J-J, et al. Functional results after tape removal for chronic pelvic pain following tension-free vaginal tape or transobturator tape. J Urol. 2010;184:610–5. https://doi.org/10.1016/j.juro.2010.03.132.
Nambiar AK, Bosch R, Cruz F, et al. EAU guidelines on assessment and nonsurgical management of urinary incontinence. Eur Urol. 2018;73:596–609. https://doi.org/10.1016/j.eururo.2017.12.031.
Hermieu J-F, Conquy S, Leriche B, et al. Synthesis of the guidelines for the treatment of non-neurological urinary incontinence in women. Prog Urol. 2010;20(Suppl 2):S94–9. https://doi.org/10.1016/S1166-7087(10)70002-6.
Pikaart DP, Miklos JR, Moore RD. Laparoscopic removal of pubovaginal polypropylene tension-free tape slings. JSLS. 2006;10:220–5.
Rouprêt M, Misraï V, Vaessen C, et al. Laparoscopic surgical complete sling resection for tension-free vaginal tape-related complications refractory to first-line conservative management: a single-centre experience. Eur Urol. 2010;58:270–4. https://doi.org/10.1016/j.eururo.2010.04.025.
Goodall EJ, Cartwright R, Stratta EC, et al. Outcomes after laparoscopic removal of retropubic midurethral slings for chronic pain. Int Urogynecol J. 2018;30(8):1323–8. https://doi.org/10.1007/s00192-018-3756-6.
Marcus-Braun N, von Theobald P (2010) Mesh removal following transvaginal mesh placement: a case series of 104 operations. Int Urogynecol J 21:423–430. https://doi.org/10.1007/s00192-009-1050-3.
Starkman JS, Wolter C, Gomelsky A, et al. Voiding dysfunction following removal of eroded synthetic mid urethral slings. J Urol. 2006;176:1040–4. https://doi.org/10.1016/j.juro.2006.04.103.
King AB, Tenggardjaja C, Goldman HB. Prospective evaluation of the effect of thigh dissection for removal of transobturator mid urethral slings on refractory thigh pain. J Urol. 2016;196:1207–12. https://doi.org/10.1016/j.juro.2016.03.153.
Ramart P, Ackerman AL, Cohen SA, et al. The risk of recurrent urinary incontinence requiring surgery after suburethral sling removal for mesh complications. Urology. 2017;106:203–9. https://doi.org/10.1016/j.urology.2017.01.060.
Milose JC, Sharp KM, He C, et al. Success of autologous pubovaginal sling after failed synthetic mid urethral sling. J Urol. 2015;193:916–20. https://doi.org/10.1016/j.juro.2014.09.038.
Welk BK, Herschorn S. The autologous fascia pubovaginal sling for complicated female stress incontinence. Can Urol Assoc J. 2012;6:36–40. https://doi.org/10.5489/cuaj.11117.
Lee D, Murray S, Bacsu CD, Zimmern PE. Long-term outcomes of autologous pubovaginal fascia slings: is there a difference between primary and secondary slings? Neurourol Urodyn. 2015;34:18–23. https://doi.org/10.1002/nau.22502.
Funding
Not applicable.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None of the authors has any conflicts of interest to disclose.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The corresponding author confirms that this manuscript has not been submitted elsewhere
Rights and permissions
About this article
Cite this article
Baron, M., Le Normand, L., Paret, F. et al. Management of post-operative urinary incontinence after midurethral sling explantation for pelvic or perineal pain. Int Urogynecol J 33, 1001–1006 (2022). https://doi.org/10.1007/s00192-021-04759-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-021-04759-1