Abstract
Introduction and hypothesis
The objective was to identify the best parameter (pubis–cervix measurement, pubis–uterine fundus measurement or pubis–pouch of Douglas measurement) on transperineal ultrasound, based on the difference between measurements taken at rest and with the Valsalva maneuver, for presurgical differential diagnosis between uterine prolapse (UP) and cervical elongation (CE) without UP.
Methods
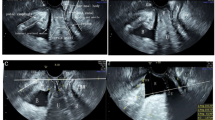
A prospective observational study of 60 consecutively recruited patients who underwent corrective surgery of the middle compartment (UP or CE without UP). A transperineal ultrasound was performed, and the descent of the pelvic organ was measured in relation to the posteroinferior margin of the pubis in the midsagittal plane, referencing the uterine fundus, pouch of Douglas and the cervix at rest and with the Valsalva test.
Results
Receiver operating characteristic (ROC) curves were constructed for the three evaluated measures, based on the difference between rest and Valsalva, for the diagnosis of UP. For the pubis–cervix distance, an area under the curve (AUC) of 0.59 was obtained; for the pubis–uterine fundus distance, the AUC was 0.81; and for the pubis–pouch of Douglas distance, the AUC was 0.69. Based on the best AUC (the difference in the pubis–uterine fundus distance at rest and with the Valsalva maneuver), a cut-off point of 15 mm was established for the diagnosis of UP (sensitivity: 75%; specificity: 95%; positive predictive value: 86%; and negative predictive value: 89%).
Conclusion
A difference of ≥15 mm in the pubis–uterine fundus distance at rest and with the Valsalva maneuver is useful for differentiating UP from CE without UP by ultrasound.



Similar content being viewed by others
References
Dietz HP, Lekskulchai O. Ultrasound assessment of prolapse: the relationship between prolapse severity and symptoms. Ultrasound Obstet Gynecol. 2007;29:688–91.
Shek KL, Dietz HP. What is abnormal uterine descent on translabial ultrasound? Int Urogynecol J. 2015;26(12):1783–7.
Eisenberg VH, Chantarasorn V, Shek KL, Dietz HP. Does levator ani injury affect cystocele type? Ultrasound Obstet Gynecol. 2010;36(5):618–23.
Green TH Jr. Urinary stress incontinence: differential diagnosis, pathophysiology, and management. Am J Obstet Gynecol. 1975;122(3):368–400.
Chantarasorn V, Dietz HP. Diagnosis of cystocele type by clinical examination and pelvic floor ultrasound. Ultrasound Obstet Gynecol. 2012 Jun;39(6):710–4.
Dietz HP, Steensma AB. Posterior compartment prolapse on two-dimensional and three-dimensional pelvic floor ultrasound: the distinction between true rectocele, perineal hypermotility and enterocele. Ultrasound Obstet Gynecol. 2005;26(1):73–7.
Hsiao SM, Chang TC, Chen CH, Li YI, Shun CT, Lin HH. Risk factors for coexistence of cervical elongation in uterine prolapse. Eur J Obstet Gynecol Reprod Biol. 2018;229:94–7.
Bump RC, Mattiasson A, Bø K, Brubaker LP, DeLancey JO, Klarskov P, et al. The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol. 1996;175:10–7.
Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U, et al. The standardisation of terminology of lower urinary tract function: report from the standardisation sub-committee of the international continence society. Neurourol Urodynam. 2002;21:167–78.
Dietz HP, Mann K. What is clinically relevant prolapse? An attempt at defining cutoffs for the clinical assessment of pelvic organ descent. Int Urogynecol J. 2014;25:451–5.
Dietz HP, Simpson JM. Levator trauma is associated with pelvic organ prolapse. BJOG. 2008;115:979–84.
Dietz HP, Shek KL. Tomographic ultrasound imaging of the pelvic floor: which levels matter most? Ultrasound Obstet Gynecol. 2009;33:698–703.
Orejuela F, Shek KL, Dietz HP. The time factor in the assessment of prolapse and levator ballooning. Int Urogynecol J. 2012;23:175–8.
García-Mejido JA, Bonomi-Barby MJ, Armijo-Sanchez A, Borrero-Fernández C, Castro-Portillo L, Vargas-Broquetas M, et al. Metodología para el estudio ecográfico transperineal del suelo pélvico. Clin Invest Ginecol Obstet. 2020;https://doi.org/10.1016/j.gine.2020.09.008.
Dietz H. Ultrasound imaging of the pelvic floor. I. Two-dimensional aspects. Ultrasound Obstet Gynecol. 2004;23:80–92.
Dietz HP, Haylen BT, Broome J. Ultrasound in the quantification of female pelvic organ prolapse. Ultrasound Obstet Gynecol. 2001;18:511–4.
Broekhuis SR, Kluivers KB, Hendriks JCM, Futterer JJ, Barentsz JO, Vierhout ME. POP-Q, dynamic MR imaging and perineal ultrasonography: do they agree in quantification of female pelvic organ prolapse? Int Urogynecol J. 2009;20:541–9.
Kluivers KB, Jan CM, Shek HC, Dietz HP. Pelvic organ prolapse symptoms in relation to POP-Q, ordinal stages and ultrasound prolapse assessment. Int Urogynecol J. 2008;19:1299–302.
Lone FW, Thakar R, Sultan AH, Stankiewicz A. Accuracy of assessing pelvic organ prolapse quantification points using dynamic 2D transperineal ultrasound in women with pelvic organ prolapse. Int Urogynecol J. 2012;23(11):1555–60.
Swenson CW, Smith TM, Luo J, Kolenic GE, Ashton-Miller JA, DeLancey JO. Intraoperative cervix location and apical support stiffness in women with and without pelvic organ prolapse. Am J Obstet Gynecol. 2017;216(2):155.e1–8.
Chen L, Ashton-Miller JA, DeLancey JO. A 3D finite element model of anterior vaginal wall support to evaluate mechanisms underlying cystocele formation. J Biomech. 2009;42:1371–7.
Luo J, Betschart C, Chen L, Ashton-Miller JA, DeLancey JO. Using stress MRI to analyze the 3D changes in apical ligament geometry from rest to maximal Valsalva: a pilot study. Int Urogynecol J. 2014;25:197–203.
Rodríguez-Mias NL, Subramaniam N, Friedman T, Shek KL, Dietz HP. Prolapse assessment supine and standing: do we need different cutoffs for “significant prolapse”? Int Urogynecol J. 2018;29(5):685–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
García-Mejido, J.A., Ramos-Vega, Z., Armijo-Sánchez, A. et al. Differential diagnosis of middle compartment pelvic organ prolapse with transperineal ultrasound. Int Urogynecol J 32, 2219–2225 (2021). https://doi.org/10.1007/s00192-020-04646-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-020-04646-1