Abstract
Introduction and hypothesis
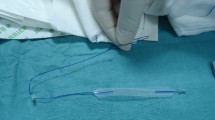
Single-incision slings are not considered a first-choice surgical treatment owing to a lack of data about long-term outcomes. We aimed to assess the long-term results of urinary incontinence treatment after single-incision sling implantation at 10 years’ follow-up and to investigate possible deterioration over time.
Methods
This retrospective study analyzed women with subjective and urodynamically proven stress urinary incontinence who underwent single-incision sling procedure. The objective cure rate was assessed with a 300-ml stress test. The subjective cure rate was determined by the Patient Global Impression of Improvement (PGI-I) questionnaire. International Consultation on Incontinence Questionnaire-Short Form (ICIQ-SF) questionnaire scores and self-answered patient-satisfaction scales were collected to assess symptom severity. Findings were compared with short-term outcomes in the same patients, available through our previous database, in order to detect possible outcome deterioration over time.
Results
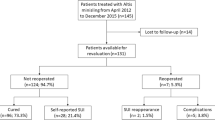
The records of 60 patients were analyzed. Nine patients (15%) were lost to follow-up. A total of 51 patients completed the evaluation, with a mean follow-up of 10.3 ± 0.7 years. Objective and subjective cure resulted 86.3% and 88.2% respectively. Mean PGI-I scores and ICIQ-SF were 1.5 ± 1.0 and 3.2 ± 4.8 respectively. Patients’ satisfaction scored 8.6 ± 2.6 out of 10. No long-term complications occurred. Comparison of short-term (2.6 ± 1.4 years after surgery) and long-term follow-up did not show a significant deterioration of outcome over time.
Conclusions
Single-incision slings were shown to be a procedure with a great efficacy and safety profile at very long-term follow-up. Cure rates and functional outcomes did not show any deterioration over time compared with short-term results.

Similar content being viewed by others
References
Bo K, Frawley HC, Haylen BT, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for the conservative and nonpharmacological management of female pelvic floor dysfunction. Neurourol Urodyn. 2017;36:221–44.
Ford AA, Rogerson L, Cody JD, Ogah J. Midurethral sling operations for stress urinary incontinence in women. Cochrane Database Syst Rev. 2015;(7):CD006375. https://doi.org/10.1002/14651858.CD006375.pub3.
Aydın S, Arıoğlu Aydın Ç. Effect of concomitant single incision vaginal surgery on mid urethral sling success. Neurourol Urodyn. 2016;35(8):995–9.
Rovner ES, Wein AJ. Treatment options for stress urinary incontinence. Rev Urol. 2004;6(Suppl 3):S29–47.
Cox A, Herschorn S, Lee L. Surgical management of female SUI: is there a gold standard? [published correction appears in Nat Rev Urol. 2013;10(4):188]. Nat Rev Urol. 2013;10(2):78–89. https://doi.org/10.1038/nrurol.2012.243.
Ulmsten U, Petros P. Intravaginal slingplasty (IVS): an ambulatory surgical procedure for treatment of female urinary incontinence. Scand J Urol Nephrol. 1995;29(1):75–82.
Geller EJ, Wu JM. Changing trends in surgery for stress urinary incontinence. Curr Opin Obstet Gynecol. 2013;25(5):404–9. https://doi.org/10.1097/GCO.0b013e3283648cdd.
Barber MD, Kleeman S, Karram MM, et al. Transobturator tape compared with tension-free vaginal tape for the treatment of stress urinary incontinence: a randomized controlled trial. Obstet Gynecol. 2008;111(3):611–21.
Milani R, Manodoro S, Cola A, Palmieri S, Frigerio M. Management of unrecognized bladder perforation following suburethral tape procedure. Int J Gynaecol Obstet. 2018;142(1):118–9.
Delorme E. [Transobturator urethral suspension: mini-invasive procedure in the treatment of stress urinary incontinence in women]. Prog Urol. 2001;11(6):1306–13.
Bianchi-Ferraro AM, Jarmy-DiBella ZI, De Aquino Castro R, et al. Randomized controlled trial comparing TVT-O and TVT-S for the treatment of stress urinary incontinence: 2-year results. Int Urogynecol J. 2014;25:1343–8.
Martan A, Masata J, Svabík K. [TVT SECUR system—tension-free support of the urethra in women suffering from stress urinary incontinence—technique and initial experience]. Ceska Gynekol. 2007;72(1):42–9.
Mostafa A, Lim CP, Hopper L, Madhuvrata P, Abdel-Fattah M. Single-incision mini-slings versus standard midurethral slings in surgical management of female stress urinary incontinence: an updated systematic review and meta-analysis of effectiveness and complications. Eur Urol. 2014;65(2):402–27.
Spelzini F, Frigerio M, Regini C, Palmieri S, Manodoro S, Milani R. Learning curve for the single-incision suburethral sling procedure for female stress urinary incontinence. Int J Gynaecol Obstet. 2017;139(3):363–7.
Palmieri S, Frigerio M, Spelzini F, Manodoro S, Milani R. Risk factors for stress urinary incontinence recurrence after single-incision sling. Neurourol Urodyn. 2018;37(5):1711–6.
Frigerio M, Regini C, Manodoro S, Spelzini F, Milani R. Mini-sling efficacy in obese versus non-obese patients for treatment of stress urinary incontinence. Minerva Ginecol. 2017;69(6):533–7.
Spelzini F, Cesana MC, Verri D, Polizzi S, Frigerio M, Milani R. Three-dimensional ultrasound assessment and middle term efficacy of a single-incision sling. Int Urogynecol J. 2013;24(8):1391–7.
Leone Roberti Maggiore U, Finazzi Agrò E, Soligo M, Li Marzi V, Digesu A, Serati M. Long-term outcomes of TOT and TVT procedures for the treatment of female stress urinary incontinence: a systematic review and meta-analysis. Int Urogynecol J. 2017;28(8):1119–30.
Manodoro S, Spelzini F, Frigerio M, Nicoli E, Verri D, Milani R. Is occult stress urinary incontinence a reliable predictive marker? Female Pelvic Med Reconstr Surg. 2016;22(4):280–2.
Schäfer W, Abrams P, Liao L, et al. Good urodynamic practices: uroflowmetry, filling cystometry, and pressure-flow studies. Neurourol Urodyn. 2002;21(3):261–74.
Tubaro A, Zattoni F, Prezioso D, et al. Italian validation of the international consultation on incontinence questionnaires. BJU Int. 2006;97(1):101–8.
Spelzini F, Manodoro S, Cola A, Palmieri S, Roselli F, Frigerio M. Single-incision sling for stress urinary incontinence: a video tutorial. Eur J Obstet Gynecol Reprod Biol. 2019;237:216–7.
Srikrishna S, Robinson D, Cardozo L. Validation of the patient global impression of improvement (PGI-I) for urogenital prolapse. Int Urogynecol J. 2010;21(5):523–8.
Haylen BT, de Ridder D, Freeman RM, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J. 2010;21(1):5–26.
Lo TS, Chua S, Tan YL, Patrimonio MC, Pue LB. Ultrasonography and clinical outcomes following anti-incontinence procedures (Monarc vs MiniArc): a 3-year post-operative review. PLoS One. 2018;13(12):e0207375. https://doi.org/10.1371/journal.pone.0207375.
Lo TS, Chua S, Kao CC, Uy-Patrimonio MC, Ibrahim R, Tan YL. Five-year outcome of MiniArc single-incision sling used in the treatment of primary urodynamic stress incontinence. J Minim Invasive Gynecol. 2018;25(1):116–23. https://doi.org/10.1016/j.jmig.2017.08.647.
Sun Z, Wang X, Lang J, et al. Comparison of outcomes between single-incision sling and transobturator sling for treating stress urinary incontinence: a 10-year prospective study. Neurourol Urodyn. 2019;38(7):1852–8.
Lucas MG, Bedretdinova D, Bosch JLHR, et al. European Association of Urology (EAU) guidelines. Guidelines on urinary incontinence. 2015. https://uroweb.org/wp-content/uploads/EAU-Guidelines-Urinary-Incontinence-2015.pdf
Cornu JN, Lizée D, Sèbe P, et al. TVT SECUR single-incision sling after 5 years of follow-up: the promises made and the promises broken. Eur Urol. 2012;62(4):737–8.
Mira Gon L, Zanettini Riccetto CL, Citatini de Campos CC, Iamashita Voris BR, Reis LO, Rodrigues Palma PC. Mini-sling Ophira at 8 years follow-up: does it sustain results? Urol Int. 2019;102(3):326–30.
Update on the Independent Medicines and Medical Devices Safety Review: written statement—HCWS841. Published July 2018.
Ford AA, Rogerson L, Cody JD, Aluko P, Ogah JA. Mid-urethral sling operations for stress urinary incontinence in women. Cochrane Database Syst Rev. 2017; 7(7):CD006375.
Seklehner S, Laudano MA, Xie D, Chughtai B, Lee RK. A metaanalysis of the performance of retropubic mid urethral slings versus transobturator mid urethral slings. J Urol. 2015;193:909–15.
ACQSHC. Care pathway for the management of Stress Urinary Incontinence 2018.
Haylen BT, Lee JKS, Sivagnanam V, Cross A. What if there were no tapes? Neurourol Urodyn. 2018;37(6):2026–34.
Author information
Authors and Affiliations
Contributions
M. Frigerio: project development, data collection, data analysis, manuscript writing; R. Milani: project development, data collection, data analysis, manuscript writing; M. Barba: project development, data collection, data analysis, manuscript writing; L. Locatelli: project development, data collection, data analysis, manuscript writing; G. Marino: project development, data collection, data analysis, manuscript writing; F. Spelzini: project development, data collection, data analysis, manuscript writing; G. Donatiello: project development, data collection, data analysis, manuscript writing; S. Manodoro: project development, data collection, data analysis, manuscript writing.
Corresponding author
Ethics declarations
Financial disclaimers/conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Frigerio, M., Milani, R., Barba, M. et al. Single-incision slings for the treatment of stress urinary incontinence: efficacy and adverse effects at 10-year follow-up. Int Urogynecol J 32, 187–191 (2021). https://doi.org/10.1007/s00192-020-04499-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-020-04499-8