Abstract
Introduction and hypothesis
This study synthesized the effects of unsupervised behavioral and pelvic floor muscle training (B-PFMT) programs on outcomes relevant to women’s storage lower urinary tract symptoms (LUTS) and pelvic floor muscle strength (PFMS).
Methods
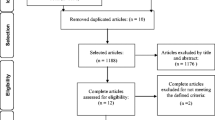
PubMed, CINAHL, Web of Science, and PsycINFO were searched since their inception to August 6, 2019. Randomized controlled trials (RCTs) and quasi-experimental articles that enrolled community women aged 18 years and older and reported storage LUTS outcomes including symptoms, severity, impact, self-reported symptom improvement, and PFMS were screened and extracted. Risk of bias was evaluated, and a narrative synthesis approach was used to synthesize evidence.
Results
Ten RCTs and three pretest-posttest articles were retrieved. Half of the RCTs had some concerns of bias; the remaining RCTs had high risk of bias. Three pretest-posttest articles had at least some risk of bias. Ten articles aimed to treat urinary incontinence (UI) primarily in middle-aged women, two aimed to prevent UI, and one aimed to improve PFMS in young continent women. Two months post-intervention, UI treatment effectiveness was observed, and cumulative effectiveness was evident in: (1) reduction in the number of incontinent episodes, (2) reduction in the International Consultation on Incontinence Questionnaire-Urinary Incontinence-Short Form and International Consultation on Incontinence Questionnaire-Lower Urinary Tract Symptoms Quality of Life scores, (3) increased patients’ global impression of improvement, and (4) improvement of PFMS.
Conclusions
Unsupervised B-PFMT programs improve outcomes relevant to UI and PFMS in midlife community women who have UI. Their effects on UI prevention and other storage LUTS remain unclear.

Similar content being viewed by others
Abbreviations
- LUTS:
-
Lower urinary tract symptoms
- UI:
-
Urinary incontinence
- SUI:
-
Stress urinary incontinence
- UUI:
-
Urgency urinary incontinence
- MUI:
-
Mixed urinary incontinence
- PFMT:
-
Pelvic floor muscle training
- PFME:
-
Pelvic floor muscle exercise
- RCT:
-
Randomized controlled trial
- PFMS:
-
Pelvic floor muscle strength
- MESA:
-
The standardized Medical Epidemiologic and Social Aspects of Aging questionnaire
- IUSS:
-
Indevus Urgency Severity Scale
- ICIQ-UI SF:
-
The International Consultation on Incontinence Questionnaire-Urinary Incontinence-Short Form
- PGI-I:
-
The Patient Global Impression of Improvement
- I-QOL:
-
Incontinence of Quality of Life
- UDI-6:
-
Urogenital Distress Inventory-6
- IIQ-7:
-
Incontinence Impact Questionnaire short form
- ICIQ-LUTSqol:
-
International Consultation on Incontinence Questionnaire-Lower Urinary Tract Symptoms Quality of Life
- EQ5D-VAS:
-
EuroQol 5D-Visual Analogue Scale
References
Abrams P, Cardozo LD, Wagg A, Wein AJ (2017) International consultation on incontinence. 6th ed. Plymouth, UK: Health Publications Ltd.
World Health Organization and Department of Reproductive Health and Research-ExpandNet (2010) Nine steps for developing a scaling-up strategy. https://www.who.int/reproductivehealth/publications/strategic_approach/9789241500319/en/.
Newman DK, Wein AJ. Office-based behavioral therapy for management of incontinence and other pelvic disorders. Urol Clin. 2013;40(4):613–35. https://doi.org/10.1016/j.ucl.2013.07.010.
Newman DK, Wein AJ (2008) Managing and treating urinary incontinence. 2nd ed. Health Professions Press.
Lamin E, Parrillo LM, Newman DK, Smith AL. Pelvic floor muscle training: underutilization in the USA. Curr Urol Rep. 2016;17(2):10. https://doi.org/10.1007/s11934-015-0572-0.
Newman DK, Borello-France D, Sung VW. Structured behavioral treatment research protocol for women with mixed urinary incontinence and overactive bladder symptoms. Neurourol Urodyn. 2018;37(1):14–26. https://doi.org/10.1002/nau.23244.
Newman DK, Burgio K (2016) Conservative management of urinary incontinence: behavioral and pelvic floor therapy and urethral and pelvic devices. Campbell-Walsh urology. 11th ed. Philadelphia, PA: Elsevier.
Pereira VS, Correia GN, Driusso P. Individual and group pelvic floor muscle training versus no treatment in female stress urinary incontinence: a randomized controlled pilot study. Eur J Obstet Gynecol Reprod Biol. 2011;159(2):465–71. https://doi.org/10.1016/j.ejogrb.2011.09.003.
Palmer MH, Cockerell R, Griebling TL, Rantell A, van Houten P, Newman DK. Review of the 6th international consultation on incontinence: primary prevention of urinary incontinence. Neurourol Urodyn. 2020;39(1):66–72. https://doi.org/10.1002/nau.24222.
Cacciari LP, Dumoulin C, Hay-Smith EJ. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women: a Cochrane systematic review abridged republication. Braz J Phys Ther. 2019;23(2):93–107. https://doi.org/10.1016/j.bjpt.2019.01.002.
Monteiro S, Riccetto C, Araújo A, Galo L, Brito N, Botelho S. Efficacy of pelvic floor muscle training in women with overactive bladder syndrome: a systematic review. Int Urogynecol J. 2018;29(11):1565–73. https://doi.org/10.1007/s00192-018-3602-x.
Bo K, Frawley HC, Haylen BT, Abramov Y, Almeida FG, Berghmans B et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for the conservative and nonpharmacological management of female pelvic floor dysfunction. Int Urogynecol J. 2017;28(2):191–213. https://doi.org/10.1007/s00192-016-3123-4.
Jones A, Skinner MA. The current status of physical therapy in China. Chinese J Rehabil Med. 2013;28(6):493–501.
Ostaszkiewicz J, Peden-McAlpine C, Northwood M, Eustice S, Bliss DZ, Nishimura K (2018) Advanced Practice Continence Nursing. In Management of Fecal Incontinence for the Advanced Practice Nurse (pp. 15–47). Springer, Cham.
Valenzuela T, Okubo Y, Woodbury A, Lord SR, Delbaere K. Adherence to technology-based exercise programs in older adults: a systematic review. J Geriatr Phys Ther. 2018;41(1):49–61. https://doi.org/10.1519/JPT.0000000000000095.
Field M (2019) Power and injustice: exploring the factors that limit Women's access to maternal health Care in rural Pennsylvania. Dissertation, Pennsylvania State University.
Newman DK, Wein AJ. Office-based behavioral therapy for management of incontinence and other pelvic disorders. Urol Clin North Am. 2013;40(4):613–35. https://doi.org/10.1016/j.ucl.2013.07.010.
Asklund I, Samuelsson E, Hamberg K, Umefjord G, Sjöström M. User experience of an app-based treatment for stress urinary incontinence: qualitative interview study. J Med Internet Res. 2019;21(3):e11296. https://doi.org/10.2196/11296.
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151(4):264–9. https://doi.org/10.7326/0003-4819-151-4-200908180-00135.
Sterne JA, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I et al. RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ. 2019;366:l4898. https://doi.org/10.1136/bmj.l4898.
Fletcher J. What is heterogeneity and is it important? BMJ. 2007;334(7584):94–6. https://doi.org/10.1136/bmj.39057.406644.68.
Popay J, Roberts H, Sowden A, Petticrew M, Arai L, Rodgers M, Britten N, Roen K, Duffy S (2006) Guidance on the conduct of narrative synthesis in systematic reviews. A product from the ESRC methods programme Version 1:b92.
Diokno AC, Sampselle CM, Herzog AR, Raghunathan TE, Hines S, Messer KL et al. Prevention of urinary incontinence by behavioral modification program: a randomized, controlled trial among older women in the community. J Urol. 2004;171(3):1165–71. https://doi.org/10.1097/01.ju.0000111503.73803.c2.
Diokno AC, Newman DK, Low LK, Griebling TL, Maddens ME, Goode PS et al. Effect of group-administered behavioral treatment on urinary incontinence in older women: a randomized clinical trial. JAMA Intern Med. 2018;178(10):1333–41. https://doi.org/10.1001/jamainternmed.2018.3766.
Diokno AC, Ocampo MS, Ibrahim IA, Karl CR, Lajiness MJ, Hall SA. Group session teaching of behavioral modification program (BMP) for urinary incontinence: a randomized controlled trial among incontinent women. Int Urol Nephrol. 2010;42(2):375–81. https://doi.org/10.1007/s11255-009-9626-x.
Sar D, Khorshid L. The effects of pelvic floor muscle training on stress and mixed urinary incontinence and quality of life. J Wound Ostomy Continence Nurs. 2009;36(4):429–35. https://doi.org/10.1097/WON.0b013e3181aaf539.
Sjöström M, Umefjord G, Stenlund H, Carlbring P, Andersson G, Samuelsson E. Internet-based treatment of stress urinary incontinence: a randomised controlled study with focus on pelvic floor muscle training. BJU Int. 2013;112(3):362–72. https://doi.org/10.1111/j.1464-410X.2012.11713.x.
Sjöström M, Umefjord G, Stenlund H, Carlbring P, Andersson G, Samuelsson E. Internet-based treatment of stress urinary incontinence: 1- and 2-year results of a randomized controlled trial with a focus on pelvic floor muscle training. BJU Int. 2015;116(6):955–64. https://doi.org/10.1111/bju.13091.
Asklund I, Nyström E, Sjöström M, Umefjord G, Stenlund H, Samuelsson E. Mobile app for treatment of stress urinary incontinence: a randomized controlled trial. Neurourol Urodyn. 2017;36(5):1369–76. https://doi.org/10.1002/nau.23116.
Hoffman V, Söderström L, Samuelsson E. Self-management of stress urinary incontinence via a mobile app: two-year follow-up of a randomized controlled trial. Acta Obstet Gynecol Scand. 2017;96(10):1180–7. https://doi.org/10.1111/aogs.13192.
Sampselle CM, Newman DK, Miller JM, Kirk K, DiCamillo MA, Wagner TH, et al. A randomized controlled trial to compare 2 scalable interventions for lower urinary tract symptom prevention: Main outcomes of the TULIP study. J Urol. 2017;197(6):1480–6. https://doi.org/10.1016/j.juro.2016.12.099.
Pereira-Baldon VS, Avila MA, Dalarmi CB, de Oliveira AB, Driusso P. Effects of different regimens for pelvic floor muscle training in young continent women: randomized controlled clinical trial. J Electromyogr Kinesiol. 2019;44:31–5. https://doi.org/10.1016/j.jelekin.2018.11.008.
Hung HC, Chih SY, Lin HH, Tsauo JY. Exercise adherence to pelvic floor muscle strengthening is not a significant predictor of symptom reduction for women with urinary incontinence. Arch Phys Med Rehabil. 2012;93(10):1795–800. https://doi.org/10.1016/j.apmr.2012.03.010.
Fan HL, Chan SS, Law TS, Cheung RY, Chung TK. Pelvic floor muscle training improves quality of life of women with urinary incontinence: a prospective study. Aust N Z J Obstet Gynaecol. 2013;53(3):298–304. https://doi.org/10.1111/ajo.12075.
Cavkaytar S, Kokanali MK, Topcu HO, Aksakal OS, Doğanay M. Effect of home-based Kegel exercises on quality of life in women with stress and mixed urinary incontinence. J Obstet Gynaecol. 2015;35(4):407–10. https://doi.org/10.3109/01443615.2014.960831.
Slade SC, Dionne CE, Underwood M, Buchbinder R. Consensus on exercise reporting template (CERT): explanation and elaboration statement. Br J Sports Med. 2016;50(23):1428–37. https://doi.org/10.1136/bjsports-2016-096651.
Hoffmann TC, Glasziou PP, Boutron I, Milne R, Perera R, Moher D, et al. Better reporting of interventions: template for intervention description and replication (TIDieR) checklist and guide. BMJ. 2014;348:g1687. https://doi.org/10.1136/bmj.g1687.
Sussman RD, Syan R, Brucker BM. Guidelines of the guidelines: urinary incontinence in women. BJU Int. 2020;125(5):638–55. https://doi.org/10.1111/bju.14927.
DeVellis RF (2016) Scale development: theory and applications. 4th ed. Sage publications.
Vidgen B, Yasseri T. P-values: misunderstood and misused. Front Phys. 2016;4(6). https://doi.org/10.3389/fphy.2016.00006.
Acknowledgements
We are grateful to Jamie Conklin, MLIS, for helping us retrieve articles from databases and to George Knafl, PhD, for providing methodological consultation for this study.
Author information
Authors and Affiliations
Contributions
C Wu, MH Palmer, and DK Newman: Protocol development.
C Wu, MH Palmer: Data management, data analysis, manuscript writing, manuscript editing.
DK Newman: Manuscript editing.
Corresponding author
Ethics declarations
Conflict of interests
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wu, C., Newman, D.K. & Palmer, M.H. Unsupervised behavioral and pelvic floor muscle training programs for storage lower urinary tract symptoms in women: a systematic review. Int Urogynecol J 31, 2485–2497 (2020). https://doi.org/10.1007/s00192-020-04498-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-020-04498-9