Abstract
Introduction and hypothesis
The aims of this study were to evaluate the impact of body mass index (BMI) on the risk of reoperation for pelvic organ prolapse (POP) up to 5 years after first-time surgery.
Materials and methods
This nationwide register-based study includes first-time POP surgery in 2010 through 2016. The cumulative incidence proportions of reoperation were analyzed in a Cox regression model and described using Kaplan-Meier plots stratified in BMI categories.
Results
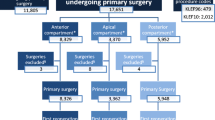
A total of 28,533 first-time procedures were performed in 22,624 women; 76.6% had single-compartment repair. The 1- and 5-year reoperation rate within the same compartment was 2.6% and 6.1% respectively for women with BMI < 25, and for women with BMI > 35 it was 3.7% and 11.2 respectively. In the anterior compartment there was a significantly increased adjusted hazard ratio for reoperation in the same compartment with increasing BMI (reference group BMI < 25), BMI 30–34.9 with an aHR = 1.34 (CI 95% 1.04–1.71) and BMI ≥ 35 aHR = 1.77 (CI 95% 1.17–2.67). The 1- and 5-year reoperation rate in an adjacent compartment was 0.6% and 1.6% respectively for women with BMI < 25, and for women with BMI > 35 it was 1.0% and 4.4 respectively. For reoperation in an adjacent compartment the adjusted results were BMI 30–34.9 aHR = 1.64 (95% CI 1.05–2.56) and BMI > 35 aHR = 2.64 (95% CI 1.36–5.14) when the first-time operation was in the anterior compartment.
Conclusions
If the woman had BMI > 35 and first-time surgery was in the anterior compartment, she had an almost doubled risk of reoperation within 5 years both in the same compartment and in an adjacent compartment compared to women with BMI < 35. In the apical and posterior compartment there was a trend towards increasing risk of reoperation with increasing BMI, although with a broad confidence interval.


Similar content being viewed by others
References
Abrams P, Cardozo L, Wagg A, Wein AJ (Alan J., International Continence Society. (2017) Incontinence: 6th International Consultation on Incontinence, Tokyo
Giri A, Hartmann KE, Hellwege JN, Velez Edwards DR, Edwards TL. Obesity and pelvic organ prolapse: a systematic review and meta-analysis of observational studies. Am J Obstet Gynecol. 2017;217:11–26.e3. https://doi.org/10.1016/j.ajog.2017.01.039.
Vergeldt TFM, Weemhoff M, IntHout J, Kluivers KB. Risk factors for pelvic organ prolapse and its recurrence: a systematic review. Int Urogynecol J. 2015;26:1559–73. https://doi.org/10.1007/s00192-015-2695-8.
Salvatore S, Siesto G, Serati M. Risk factors for recurrence of genital prolapse. Curr Opin Obstet Gynecol. 2010;22:420–4. https://doi.org/10.1097/GCO.0b013e32833e4974.
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL. Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol. 1997;89:501–6.
Tegerstedt G, Hammarström M. Operation for pelvic organ prolapse: a follow-up study. Acta Obstet Gynecol Scand. 2004;83:758–63. https://doi.org/10.1111/j.0001-6349.2004.00468.x.
Friedman T, Eslick GD, Dietz HP. Risk factors for prolapse recurrence: systematic review and meta-analysis. Int Urogynecol J. 2018;29:13–21. https://doi.org/10.1007/s00192-017-3475-4.
Løwenstein E, Møller LA, Laigaard J, Gimbel H. Reoperation for pelvic organ prolapse: a Danish cohort study with 15–20 years’ follow-up. Int Urogynecol J. 2018;29:119–24. https://doi.org/10.1007/s00192-017-3395-3.
Lynge E, Sandegaard JL, Rebolj M. The Danish National Patient Register. Scand J Public Health. 2011;39:30–3. https://doi.org/10.1177/1403494811401482.
Guldberg R, Brostrøm S, Hansen JK, Kaerlev L, Gradel KO, Nørgård BM, et al. The Danish urogynaecological database: establishment, completeness and validity. Int Urogynecol J Pelvic Floor Dysfunct. 2013;24:983–90. https://doi.org/10.1007/s00192-012-1968-8.
Hansen UD, Gradel KO, Larsen MD (2016) Danish Urogynaecological Database. 709–712.
Haya N, Baessler K, Christmann-Schmid C, De Tayrac R, Dietz V, Guldberg R, et al. Prolapse and continence surgery in countries of the Organization for Economic Cooperation and Development in 2012. Am J Obstet Gynecol. 2015;212:755.e1–755.e27. https://doi.org/10.1016/j.ajog.2015.02.017.
Price N, Slack A, Jwarah E, Jackson S. The incidence of reoperation for surgically treated pelvic organ prolapse: an 11-year experience. Menopause Int. 2008;14:145–8. https://doi.org/10.1258/mi.2008.008029.
Oversand SH, Staff AC, Spydslaug AE, Svenningsen R, Borstad E. Long-term follow-up after native tissue repair for pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2014;25:81–9. https://doi.org/10.1007/s00192-013-2166-z.
Bohlin KS, Ankardal M, Nüssler E, Lindkvist H, Milsom I. Factors influencing the outcome of surgery for pelvic organ prolapse. Int Urogynecol J. 2018;29:81–9. https://doi.org/10.1007/s00192-017-3446-9.
Manodoro S, Frigerio M, Cola A, Spelzini F, Milani R. Risk factors for recurrence after hysterectomy plus native-tissue repair as primary treatment for genital prolapse. Int Urogynecol J. 2018;29:145–51. https://doi.org/10.1007/s00192-017-3448-7.
Rappa C, Saccone G. Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight and overweight women. Am J Obstet Gynecol. 2016;215:601.e1–4. https://doi.org/10.1016/j.ajog.2016.06.022.
Nam K-H, Jeon M-J, Hur H-W, Kim S-K, Bai S-W. Perioperative and long-term complications among obese women undergoing vaginal surgery. Int J Gynecol Obstet. 2009;108:244–6.
Bradley CS, Kenton KS, Richter HE, Gao X, Zyczynski HM, Weber AM, et al. Obesity and outcomes after sacrocolpopexy. Am J Obstet Gynecol. 2008;199:690.e1–8. https://doi.org/10.1016/j.ajog.2008.07.030.
Thubert T, Naveau A, Letohic A, Villefranque V, Benifla JL, Deffieux X. Outcomes and feasibility of laparoscopic sacrocolpopexy among obese versus non-obese women. Int J Gynecol Obstet. 2013;120:49–52. https://doi.org/10.1016/j.ijgo.2012.07.020.
Acknowledgements
The study was supported by the Program for Clinical Research Infrastructure (PROCRIN) established by the Lundbeck Foundation and the Novo Nordisk Foundation.
Author information
Authors and Affiliations
Contributions
All authors have contributed to the project conception. All analyses were performed by MD Larsen. The manuscript was drafted by V Weltz and R Guldberg. All authors have contributed substantively to interpretation of the study results, development of the manuscript and approved the final submitted version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
V Weltz, G Lose and MD Larsen have no conflicts of interest to declare. R Guldberg has been a member of Advisory Board for Astellas and has received payment for tuition.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix
Anterior repairs:
KLEF00 = Anterior colporrhaphy
KLEF00A = Anterior colporrhaphy with mesh
KLEF60 = Vaginal lateral colporrhaphy
KLEF63 = Abdomial lateral colporrhaphy
KLEF64 = Laparoscopic lateral colporrhaphy
Apical repairs:
KLEF23 = Complete colpocleisis
KLEF50 = Abdominal apical colpopexy after previous hysterectomy
KLEF50A = Abdominal apical colpopexy after previous hysterectomy with mesh
KLEF51 = Laparoscopic apical colpopexy after previous hysterectomy
KLEF51A = Laparoscopic apical colpopexy after previous hysterectomy with mesh
KLEF53 = Vaginal apical colpopexy after previous hysterectomy
KLEF53A = Vaginal apical colpopexy after previous hysterectomy with mesh
KLEF53B = Vaginal apical colpopexy, sacrospinous ligament
Posterior repairs:
KLEF03 = Posterior vaginal apical colporrhaphy the sacrospineous ligament
KLEF03A = Posterior vaginal apical colporrhaphy with mesh
KLEF40 = Vaginal operation for enterocele
KLEF40A = Vaginal operation for enterocele with mesh
KLEF41 = Laparoscopic operation for enterocele
KLEF41A = Laparoscopic operation for enterocele with mesh
KLEF43 = Abdominal operation for enterocele
KLEF43A = Abdominal operation for enterocele with mesh
Rights and permissions
About this article
Cite this article
Weltz, V., Guldberg, R., Larsen, M.D. et al. Body mass index influences the risk of reoperation after first-time surgery for pelvic organ prolapse. A Danish cohort study, 2010–2016. Int Urogynecol J 32, 801–808 (2021). https://doi.org/10.1007/s00192-020-04482-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-020-04482-3