Abstract
Introduction and hypothesis
Vesicovaginal fistulae (VVF) repair success rates for simple surgical fistulae are high, but constitute a significantly greater challenge when occurring in a radiotherapy field. We aim to evaluate the causes, assessment, closure rates and functional outcomes of VVF surgery in patients with previous radiotherapy.
Methods
Data on all VVF repairs were collected prospectively. A retrospective review of outcomes in those with VVF performed between 2009 and 2018 was carried out. Details including time from radiotherapy, pre-operative assessments, approach to surgery and functional outcome were analysed.
Results
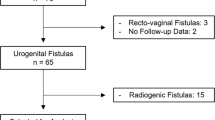
Twenty women with VVFs were identified. The mean age was 59 (range 25–88) years. Primary malignancy was cervical in 16 women, with the remaining 4 women having ovarian, urethral, endometrial and rectal cancer respectively. All women had external beam radiotherapy with 6 (30%) undergoing boosted brachytherapy. Mean interval between radiotherapy and fistula repair was 19 (range 0–40) years. Fistulae arose spontaneously in 14 patients, whereas 6 occurred following a further surgical intervention.Closure was attempted vaginally in 7 women and abdominally in 1, whereas 12 had a primary diversion owing to significant bladder contracture and ureteric involvement. The closure rate in those attempted was 62.5%, 40% in those with spontaneous fistulae compared with 100% for post-surgical fistulae, but only 20% for the total cohort.
Conclusions
Closure of VVF is a significant challenge, with an initial success rate of 20% and an overall success rate of only 25%. Seventy percent required primary or secondary urinary diversion. Vaginal surgery was utilised in the majority to try to avoid a hostile pelvis, but the surgical approach should be tailored to individual circumstances.

Similar content being viewed by others
References
Hillary CJ, Osman NI, Hilton P, Chapple CR. The aetiology, treatment, and outcome of urogenital fistulae managed in well- and low-resourced countries: a systematic review. Eur Urol. 2016;70(3):478–92. https://doi.org/10.1016/j.eururo.2016.02.015.
Cromwell D, Hilton P. Retrospective cohort study on patterns of care and outcomes of surgical treatment for lower urinary-genital tract fistula among English National Health Service hospitals between 2000 and 2009. BJU Int. 2013;111(Pt 4B):E257–62.
Bodner-Adler B, Hanzal E, Pablik E, Koelbl H, Bodner K. Management of vesicovaginal fistulas (VVFs) in women following benign gynaecologic surgery: a systematic review and meta-analysis. PLoS One. 2017;12(2):1–21.
Joye I, Haustermans K. Early and late toxicity of radiotherapy for rectal cancer. Recent Results Cancer Res. 2014;203:189–201.
Marks LB, Carroll PR, Dugan TC, Anscher MS. The response of the urinary bladder, urethra, and ureter to radiation and chemotherapy. Int J Radiat Oncol. 1995;31(5):1257–80.
Mondet F, Chartier-Kastler EJ, Conort P, Bitker MO, Chatelain C, Richard F. Anatomic and functional results of transperitoneal-transvesical vesicovaginal fistula repair. Urology. 2001;58(6):882–6.
Langkilde NC, Pless TK, Lundbeck F, Nerstrøm B. Surgical repair of vesicovaginal fistulae—a ten-year retrospective study. Scand J Urol Nephrol. 1999;33(2):100–3.
Hilton P. Urogenital fistula in the UK: a personal case series managed over 25 years. BJU Int. 2012;110(1):102–10.
Pushkar DY, Dyakov VV, Kasyan GR. Management of radiation-induced vesicovaginal fistula. Eur Urol. 2009;55(1):131–8.
Toia B, Seth J, Ecclestone H, Pakzad M, Hamid R, Greenwell T, et al. Outcomes of reconstructive urinary tract surgery after pelvic radiotherapy. Scand J Urol. 2019;53(2–3):156–60.
Liberman D, Mehus B, Elliott SP. Urinary adverse effects of pelvic radiotherapy. Transl Androl Urol. 2014;3(2):186–95.
Turesson I. Individual variation and dose dependency in the progression rate of skin telangiectasia. Int J Radiat Oncol Biol Phys. 1990;19(6):1569–74.
Perez CA, Grigsby PW, Lockett MA, Chao KS, Williamson J. Radiation therapy morbidity in carcinoma of the uterine cervix: dosimetric and clinical correlation. Int J Radiat Oncol Biol Phys. 1999;44(4):855–66.
Abrams P, Cardozo L, Khoury S, Wein AJ, International Continence Society. Incontinence: 5th International Consultation on Incontinence, Paris, February 2012. ICUD-EAU; 2013.
Miller EA, Webster GD. Current management of vesicovaginal fistulae. Curr Opin Urol. 2001;11(4):417–21.
Gousse AE, Evans DH, Madjar S, Politano VA, Bejany DE, Lynne CM. Interposition flaps in transabdominal vesicovaginal fistula repairs: are they really necessary? Urology. 2001;57(4):670–4.
Author information
Authors and Affiliations
Contributions
BT: data collection, manuscript writing; MP, RH, TG: project development; JO: project development, manuscript writing.
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Toia, B., Pakzad, M., Hamid, R. et al. Surgical outcomes of vesicovaginal fistulae in patients with previous pelvic radiotherapy. Int Urogynecol J 31, 1381–1385 (2020). https://doi.org/10.1007/s00192-019-04217-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-019-04217-z