Abstract
Introduction and hypothesis
The levator ani muscle (LAM) plays an important role in pelvic support. Estimated levator ani subtended volume (eLASV) is an objective measurement of the anatomical volume of the LAM obtained from pelvic MRIs. The aim of this study was to assess the relationship between the anatomical volume of LAM to the age and body mass index (BMI) of a surgical patient based on our previous published cutoff value of increased LAM volume as measured by pelvic MRIs (eLASV > 38.5). We hypothesize that increasing age and BMI will both be correlated with the increasing volumes of LAM.
Methods
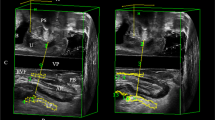
We conducted a secondary analysis of an Institutional Review Board-approved retrospective cohort study. Standard protocol pelvic MRI measurements, including the pubococcygeal line, H-line, and M-line, were collected along with the calculated width of the levator ani hiatus (eLASV = − 72.838 + 0.598H-line + 1.217 M-line + 1.136WLH). Comparison to patients’ age and BMI was assessed using the Wilcoxon-Mann-Whitney (continuous) and chi-square test (group). Spearman’s correlation analysis was used to explore the relationship between age and BMI to eLASV.
Results
Patients with elevated LAM volumes of eLASV were more likely to be older than patients with low volume of LAM, with median age 65 (37, 83) vs. 49.5 (28, 72), respectively (p < 0.001). We observed no difference in median BMI between patients with elevated volumes of eLASV compared with patients with low volumes of eLASV.
Conclusions
Increasing age of women appears to be directly related to elevated volumes for levator ani muscle morphology when measured with eLASV.


Similar content being viewed by others
References
Dietz HP. Pelvic floor trauma in childbirth. Australian and New Zealand J Obset Gynecol. 2013;53:220–30.
DeLancey JO, Morgan DM, Fenner DE, Kearney R, Guire K, Miller JM, et al. Comparison of levator ani muscle defects and function in women with and without pelvic organ prolapse. Obset Gynecol. 2007;109:295–302.
Dietz H, De Leon J, Shek K. Ballooning of the levator hiatus. Ultrasound Obstet Gynecol. 2008;31:676–80.
Dietz HP, Charntarason V, Shek KL. Levator avulsion is a risk factor for cystocele recurrence. Ultrasound Obstet Gynecol. 2010;36:76–80.
Wong V, Shek KL, Rane A, Goh J, Krause H, Dietz HP. Is levator avulsion a predictor of recurrence after anterior compartment mesh? UOG. 2013;42(2):230–4 14.
DeLancey JO, Morgan DM, Fenner DE, et al. Comparison of levator ani muscle defects and function in women with and without pelvic organ prolapse. Obstet Gynecol. 2007;109:295–302.
DeLancey JO, Hurd WW. Size of the urogenital hiatus in the levator ani muscles in normal women and women with pelvic organ prolapse. Obstet Gynecol. 1998;91:364–8.
Sammarco A, Nandikanti L, Kobernik E, et al. Interactions between pelvic organ protrusion, levator ani descent, and hiatal enlargement in women with and without prolapse. Am J Obstet Gynecol. 2017;217:614. e1–7.
Handa V, Blomquist J, Roem J, Munoz A. Longitudinal study of quantitiative changes in pelvic organ support among parous women. Am J Obstet Gynecol. 2018;218:320. e1–7.
Rodriques AA Jr, Bassaly R, McCullough M, Terwilliger HL, Hart S, Downes K, et al. Levator ani subtended volume: a novel parameter to evaluate levator ani muscle laxity in pelvic organ prolapse. Am J Obstet Gynecol. 2012;206:244.e1–9.
Rodriques AA Jr, Herrera-Hernadez MC, Bassaly R, McCullough M, Terwilliger HL, Downes K, et al. Estimates of the levator ani subtended volume based on magnetic resonance linear measurements. Neurourol Urodyn. 2016;35(2):199–205.
Wyman AM, Rodrigues AA Jr, Hahn L, Greene KA, Bassaly R, Hart S, et al. Estimated Levator Ani subtended volume (eLASV): a novel assay for predicting surgical failure after uterosacral ligament suspension. Am J Obstet Gynecol. 2016;214(5):611.e1–6.
Al-Mukhtar Othman J, Åkervall S, Milsom I, et al. Urinary incontinence in nulliparous women aged 25-64 years: a national survey. Am J Obstet Gynecol. 2017;216:149.e1–11.
Law YM, Fielding JR. MRI of pelvic floor dysfunction: review. AJR Am J Roentgenol. 2008;191:S45–53.
Maldonado G, Greenland S. Simulation study of confounder-selection strategies. Am J Epidemiol. 1993;138(11):923–36.
Norton P, Brubaker L. Urinary incontinence in women. Lancet. 2006;367:57–67.
DeLancey JOL, Kearney R, Chou Q, Speights S, Binno S. The appearance of levator ani muscle abnormalities in magnetic resonance images after vaginal delivery. Obstet Gynecol. 2003;101:46–53.
Mitchell WK, Williams J, Atherton P, Larvin M, Lund J, Narici M. Sarcopenia, dynapenia, and the impact of advancing age on human skeletal muscle size and strength; a quantitative review. Front Physiol. 2012;3:260.
Kyle UG, Genton L, Hans D, Karsegard L, Slosman DO, Pichard C. Age-related differences in fat-free mass, skeletal muscle, body cell mass and fat mass between 18 and 94 years. Eur J Clin Nutr. 2001;55:663–72.
Silva AM, Shen W, Heo M, et al. Ethnicityrelated skeletal muscle differences across the lifespan. Am J Hum Biol. 2009;22:7682.
Edenfield AL, Amundsen CL, Weidner AC, et al. Vaginal prolapse recurrence after uterosacral ligament suspension in normal weight compared with overweight and obese women. Obstet Gynecol. 2013;121:554–9.
Author information
Authors and Affiliations
Contributions
AM Wyman: Protocol/project development, data collection or management, data analysis, manuscript writing/editing.
JP Tanner: Data analysis, manuscript writing/editing.
R Bassaly: Protocol/project development, manuscript writing/editing.
L Hoyte: Protocol/project development, manuscript writing/editing.
KA Greene: Protocol/project development, data collection or management, manuscript writing/editing.
Corresponding author
Ethics declarations
Conflicts of interest
L Hoyte is a consultant for Cooper Surgical.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wyman, A.M., Tanner, J.P., Bassaly, R. et al. Levator ani muscle (LAM) anatomical volume compared to age and body mass index (BMI) of patients. Int Urogynecol J 31, 1457–1461 (2020). https://doi.org/10.1007/s00192-019-04141-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-019-04141-2