Abstract
Introduction and hypothesis
Urinary incontinence is common among older adults with chronic conditions. The purpose of this study is to examine the association of urinary incontinence with chronic conditions in the US population.
Methods
We used data from the 2001–2014 National Health and Nutrition Examination Survey; 7226 women and 7239 men age > 50 years answered questions regarding urinary symptoms. The analysis accounted for the complex survey design, and prevalence reflects estimates within the non-institutionalized US population.
Results
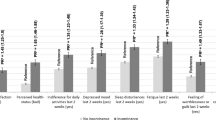
The mean age was 64.2 years [standard error (SE) 0.2] among women and 62.9 (SE 0.1) years among men. Bothersome stress, urgency and mixed incontinence were reported by 6.7% (SE 0.4), 4.8% (SE 0.4) and 19.3% (SE 0.59) of women, respectively, and 0.6% (SE 0.1), 3.5% (SE 0.2) and 1.9% (SE 0.2) of men, respectively. Among chronic conditions, heart failure was associated with higher prevalence of mixed incontinence in women and urgency incontinence in men. Among women, heart failure was associated with significantly increased odds of bothersome mixed incontinence (OR 2.35; 95% CI 1.62, 3.42) and lower odds of stress (OR 0.50; 95% CI 0.3, 0.9) or urgency incontinence (OR 0.43; 95% CI 0.19, 0.98) after adjustment for covariates. Among men, heart failure was associated with higher odds of stress (OR 1.99; 95% CI 0.39, 10.22), urgency (1.65; 95% CI 0.91, 2.99) and mixed incontinence (OR 1.54; 95% CI 0.91, 2.62) but associations were not statistically significant.
Conclusions
Heart failure is associated with higher odds of bothersome incontinence, especially among women.



Similar content being viewed by others
References
Dooley Y, Kenton K, Cao G, Luke A, Durazo-Arvizu R, Kramer H, et al. Urinary incontinence prevalence: results from the National Health and nutrition examination survey. J Urol. 2008;179:656–61.
Milson I, Altman D, Lapitan MC, Nelson R, Sillen U, Thom D. Epidemiology of urinary (UI) and faecal (FI) incontinence and pelvic organ prolape. In: Abrams P, Cardozo L, Khoury S, Wein A, editors. Incontinence. Paris, France: European Association of Urology; 2009. p. 35–111.
Markland AD, Richter HE, Fwu CW, Eggers P, Kusek JW. Prevalence and trends of urinary incontinence in adults in the United States, 2001 to 2008. J Urol. 2011;186:589–93.
(2008) Prevalence of and risk factors for urine leakage in a racially and ethnically diverse population of adults: the Boston Area Community Health (BACH) Survey. Am J Epidemiol 167:390–399.
Coyne KS, Wein A, Nicholson S, Kvasz M, Chen CI, Milsom I. Economic burden of urgency urinary incontinence in the United States: a systematic review. J Manag Care Pharm. 2014;20:130–40.
Dugan E, Roberts CP, Cohen SJ, Preisser JS, Davis CC, Bland DR, et al. Why older community-dwelling adults do not discuss urinary incontinence with their primary care physicians. J Am Geriatr Soc. 2001;49:462–5.
Yang E, Lisha NE, Walter L, Obedin-Maliver J, Huang AJ. Urinary incontinence in a National Cohort of older women: implications for caregiving and care dependence. J Women's Health (Larchmt). 2018;27:1097–103.
Phelan S, Kanaya AM, Subak LL, Hogan PE, Espeland MA, Wing RR, et al. Prevalence and risk factors for urinary incontinence in overweight and obese diabetic women: action for health in diabetes (look ahead) study. Diabetes Care. 2009;32:1391–7.
(2006) Prevalence of lower urinary tract symptoms and effect on quality of life in a racially and ethnically diverse random sample: the Boston Area Community Health (BACH) Survey. Arch Intern Med 166:2381–2387.
Tannenbaum C, Johnell K. Managing therapeutic competition in patients with heart failure, lower urinary tract symptoms and incontinence. Drugs Aging. 2014;31:93–101.
Tsakiris P, Oelke M, Michel MC. Drug-induced urinary incontinence. Drugs Aging. 2008;25:541–9.
Zipf G, Chiappa M, Porter KS, Ostchega Y, Lewis BG, Dostal J. National health and nutrition examination survey: plan and operations, 1999-2010. Vital Health Stat. 2013;1(56):1–37.
Inker LA, Schmid CH, Tighiouart H, Eckfeldt JH, Feldman HI, Greene T, et al. Estimating glomerular filtration rate from serum creatinine and cystatin C. N Engl J Med. 2012;367:20–9.
Tsui A, Kuh D, Cardozo L, Davis D. Vascular risk factors for male and female urgency urinary incontinence at age 68 years from a British birth cohort study. BJU Int. 2018;122:118–25.
Coyne KS, Wein A, Nicholson S, Kvasz M, Chen CI, Milsom I. Comorbidities and personal burden of urgency urinary incontinence: a systematic review. Int J Clin Pract. 2013;67:1015–33.
Roberts AW, Ogunwole SU, Blakeslee L, Rabe MA (2018) The population 65 years and older in the United States: 2016. Economics and statistics administration. US Census Bureau. https://www.census.gov/content/dam/Census/library/publications/2018/acs/ACS-38.pdf accessed may 15, 2019. American community survey reports ACS-38.
Flegal KM, Kruszon-Moran D, Carroll MD, Fryar CD, Ogden CL. Trends in obesity among adults in the United States, 2005 to 2014. JAMA. 2016;315:2284–91.
Bhupathiraju SN, Hu FB. Epidemiology of obesity and diabetes and their cardiovascular complications. Circ Res. 2016;118:1723–35.
Hwang R, Chuan F, Peters R, Kuys S. Frequency of urinary incontinence in people with chronic heart failure. Heart Lung. 2013;42:26–31.
Nie XF, Ouyang YQ, Wang L, Redding SR. A meta-analysis of pelvic floor muscle training for the treatment of urinary incontinence. Int J Gynaecol Obstet. 2017;138:250–5.
Diokno AC, Burgio K, Fultz NH, Kinchen KS, Obenchain R, Bump RC. Medical and self-care practices reported by women with urinary incontinence. Am J Manag Care. 2004;10:69–78.
Mitteness LS. The management of urinary incontinence by community-living elderly. Gerontologist. 1987;27:185–93.
DuBeau CE. Interpreting the effect of common medical conditions on voiding dysfunction in the elderly. Urol Clin North Am. 1996;23:11–8.
Potosky AL, Legler J, Albertsen PC, Stanford JL, Gilliland FD, Hamilton AS, et al. Health outcomes after prostatectomy or radiotherapy for prostate cancer: results from the prostate cancer outcomes study. J Natl Cancer Inst. 2000;92:1582–92.
Chen RC, Basak R, Meyer AM, Kuo TM, Carpenter WR, Agans RP, et al. Association between choice of radical prostatectomy, external beam radiotherapy, brachytherapy, or active surveillance and patient-reported quality of life among men with localized prostate cancer. JAMA. 2017;317:1141–50.
Sandvik H, Hunskaar S, Vanvik A, Bratt H, Seim A, Hermstad R. Diagnostic classification of female urinary incontinence: an epidemiological survey corrected for validity. J Clin Epidemiol. 1995;48:339–43.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors report no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 26 kb)
Rights and permissions
About this article
Cite this article
Daugirdas, S.P., Markossian, T., Mueller, E.R. et al. Urinary incontinence and chronic conditions in the US population age 50 years and older. Int Urogynecol J 31, 1013–1020 (2020). https://doi.org/10.1007/s00192-019-04137-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-019-04137-y