Abstract
Introduction and hypothesis
Obstetric anal sphincter injury causes anal incontinence in half of the women affected. However, most symptoms are mild. The objective of this study was to evaluate the prevalence of anal incontinence and quality of life in women at long term after delivery with obstetric anal sphincter injury. We also wanted to identify a relevant cutoff level of the Wexner score (also known as the Cleveland Clinic Incontinence Score) to indicate affected quality of life in these women.
Methods
We performed a population-based questionnaire cohort study with prospective follow-up, including all women in Denmark with obstetric anal sphincter injury and one subsequent delivery between 1997 and 2005. We performed uni- and multivariate analyses and calculated the area under the ROC curve.
Results
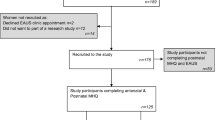
In Denmark, 3885 women had an obstetric anal sphincter injury in their first delivery and a second delivery between 1997 and 2005 and no subsequent deliveries until 2010–2011. Questionnaires were sent to 3259 eligible women, and the response rate was 74.6%. In total, 2004 women could be included in the final analyses. Of these, 29.2% (n = 584) reported affected quality of life due to anal incontinence at long-term follow-up. We found that all symptoms of anal incontinence were associated with affected quality of life. The median age at follow-up was 40.3 years.
The area under the ROC curve was 0.96 (95% CI 0.95–0.97) with a sensitivity of 0.94 (95% CI 0.92–0.96) and a specificity of 0.85 (95% CI 0.84–0.87) corresponding to an optimal cutoff level of the Wexner score of ≥ 2 to identify women with affected quality of life due to anal incontinence.
Conclusions
In women with obstetric anal sphincter injury, 29% reported affected quality of life due to anal incontinence at long-term follow-up, and we found a low Wexner score cutoff level of ≥ 2 to identify women with affected quality of life.


Similar content being viewed by others
Abbreviations
- aOR:
-
Adjusted odds ratio
- AUC:
-
Area under the curve
- CI:
-
Confidence interval
- cOR:
-
Crude odds ratio
- OASIS :
-
Obstetric anal sphincter injury
- ROC:
-
Receiver-operating characteristics
References
Jangö H, Langhoff-Roos J, Rosthøj S, Sakse A. Mode of delivery after obstetric anal sphincter injury and the risk of long-term anal incontinence. Am J Obstet Gynecol. 2016;214(6):733.e1–733.e13.
Wegnelius G, Hammarström M. Complete rupture of anal sphincter in primiparas: long-term effects and subsequent delivery. Acta Obstet Gynecol Scand. 2011;90(3):258–63.
Sultan AH, Monga A, Lee J, Emmanuel A, Norton C, Santoro G, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female anorectal dysfunction. Neurourol Urodyn. 2017;36(1):10–34.
Palm A, Israelsson L, Bolin M, Danielsson I. Symptoms after obstetric sphincter injuries have little effect on quality of life. Acta Obstet Gynecol Scand. 2013;92(1):109–15.
Avery KNL, Bosch JLHR, Gotoh M, Naughton M, Jackson S, Radley SC, et al. Questionnaires to assess urinary and anal incontinence: review and recommendations. J Urol. 2007;177(1):39–49.
Jorge JM, Wexner SD. Etiology and management of fecal incontinence. Dis Colon Rectum. 1993;36(1):77–97.
Vaizey CJ, Carapeti E, Cahill JA, Kamm MA, Park N. Prospective comparison of faecal incontinence grading systems. Gut. 1999;44:77–80.
Rothbarth J, Bemelman WA, Meijerink WJ, Stiggelbout AM, Zwinderman AH, Buyze-Westerweel ME, et al. What is the impact of fecal incontinence on quality of life? Dis Colon Rectum. 2001;44(1):67–71.
Damon H, Dumas P, Mion F. Impact of anal incontinence and chronic constipation on quality of life. Gastroenterol Clin Biol. 2004;28:16–20.
Sultan AH. Obstetric perineal injury and anal incontinence. Clinical Risk. 1999;5:193–6.
Abrams P, Cardozo L, Wein A, Wagg A. Incontinence: 6th International Consultation on Incontinence, Tokyo, September 2016. Icud. 2017.
Jangö H, Langhoff-Roos J, Rosthøj S, Sakse A. Recurrent obstetric anal sphincter injury and the risk of long-term anal incontinence. Am J Obstet Gynecol. 2017;216(6):610.e1–8.
Jangö H, Langhoff-Roos J, Rosthøj S, Saske A. Long-term anal incontinence after obstetric anal sphincter injury—does grade of tear matter? Am J Obstet Gynecol. 2018;218(2):232.e1–232.e10.
Due U, Ottesen M. The Danish anal sphincter rupture questionnaire: validity and reliability. Acta Obstet Gynecol Scand. 2009;88(1):36–42.
R: The R Project for Statistical Computing [Internet]. [cited 2016 Jan 4]. Available from: https://www.r-project.org/.
Kuismanen K, Nieminen K, Karjalainen K, Lehto K, Uotila J. Outcomes of primary anal sphincter repair after obstetric injury and evaluation of a novel three-choice assessment. Tech Coloproctol. 2018;22(3):209–14.
Norton C. Nurses, bowel continence, stigma, and taboos. J wound, ostomy, Cont Nurs Off Publ Wound, Ostomy Cont Nurses Soc. 2000;31(2):85–94.
Rockwood TH, Church JM, Fleshman JW, Kane RL, Mavrantonis C, Thorson AG, et al. Fecal incontinence quality of life scale: quality of life instrument for patients with fecal incontinence. Dis Colon Rectum. 2000;43(1):9–16 discussion 16-7.
Rockwood TH, Church JM, Fleshman JW, Kane RL, Mavrantonis C, Thorson AG, et al. Patient and surgeon ranking of the severity of symptoms associated with fecal incontinence the fecal incontinence severity index. Dis Colon Rectum. 1999;42:1525–31.
Cotterill N, Norton C, Avery KNL, Abrams P, Donovan JL. Psychometric evaluation of a new patient-completed questionnaire for evaluating anal incontinence symptoms and impact on quality of life: the ICIQ-B. Dis Colon Rectum. 2011;54:1235–50.
Lee JT, Madoff RD, Rockwood TH. Quality-of-life measures in fecal incontinence: is validation valid? Dis Colon Rectum. 2015;58:352–7.
Funding
The study was funded by Aase and Ejnar Danielsens Foundation, Denmark. The funding source had no influence or involvement in the study.
Author information
Authors and Affiliations
Contributions
• H Jangö: Design of study, development of questionnaire, data collection, data analysis, writing and critical revision of manuscript.
• J Langhoff-Roos: Design of study, development of questionnaire and critical revision of manuscript.
• S Rosthøj: Data analysis and critical revision of manuscript.
• A Sakse: Design of study, development of questionnaire, data analysis and critical revision of manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Presentation
Some preliminary data were presented as a podium presentation at the Nordic Urogynecological Associations biannual meeting, Copenhagen, 24–26 January 2019
Rights and permissions
About this article
Cite this article
Jangö, H., Langhoff-Roos, J., Rosthøj, S. et al. Wexner score and quality of life in women with obstetric anal sphincter injury. Int Urogynecol J 31, 1115–1121 (2020). https://doi.org/10.1007/s00192-019-04134-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-019-04134-1