Abstract
Introduction and hypothesis
Our aim was to introduce a new affordable and easy-to-make pelvic model for training in complex urogynecological laparoscopic procedures.
Methods
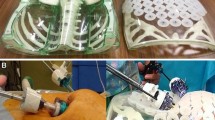
We modified a commercial female pelvic model consisting of sacrum, coccyx, two hip bones, the pubic symphysis, the fifth lumbar vertebra with intervertebral disc, and certain pelvic ligaments. We used sponge foam paper, felt fabric pieces, chenille stems, foam, plastic ties, fabric glue, and a thick, coated wire to create pelvic floor, uterus/vaginal cuff, bladder, both ureters, and anterior longitudinal and pectineal ligaments.
Results
We created two different pelvic models: one with the uterus and one with the vaginal cuff. They enable training for laparoscopic pectopexy and hysteropexy/sacrocolpopexy. Trainees can practice proper mesh placement and suture the mesh to the corresponding anatomical structures. Because of the wire inserted in the uterus/vaginal cuff, it is possible to move the uterus/vaginal cuff in the anterior–posterior direction, thus mimicking the use of the manipulator during surgery. Besides the basic pelvis, all other parts of the model can be easily replaced when necessary.
Conclusions
We believe that our pelvic model could provide a valuable tool for training complex urogynecological laparoscopic procedures and help to reduce the long learning curve of these procedures.




Similar content being viewed by others
References
Mustafa S, Amit A, Filmar S, et al. Implementation of laparoscopic sacrocolpopexy: establishment of a learning curve and short-term outcomes. Arch Gynecol Obstet. 2012;286:983–8. https://doi.org/10.1007/s00404-012-2391-6.
Akladios CY, Dautun D, Saussine C, et al. Laparoscopic sacrocolpopexy for female genital organ prolapse: establishment of a learning curve. Eur J Obstet Gynecol Reprod Biol. 2010;149:218–21. https://doi.org/10.1016/j.ejogrb.2009.12.012.
Shetty S, Zevin B, Grantcharov TP, et al. Perceptions, training experiences, and preferences of surgical residents toward laparoscopic simulation training: a resident survey. J Surg Educ. 2014;71:727–33. https://doi.org/10.1016/j.jsurg.2014.01.006.
Claerhout F, Verguts J, Werbrouck E, et al. Analysis of the learning process for laparoscopic sacrocolpopexy: identification of challenging steps. Int Urogynecol J. 2014;25:1185–91. https://doi.org/10.1007/s00192-014-2412-z.
Stolzenburg JU, Truss MC, Rabenalt R, et al. Training in laparoscopy. EAU-EBU Update Series. 2007;5:53–62. https://doi.org/10.1016/j.eeus.2006.12.001.
Smith MD, Norris JM, Kishikova L, et al. Laparoscopic simulation for all: two affordable, upgradable, and easy-to-build laparoscopic trainers. J Surg Educ. 2013;70:217–23. https://doi.org/10.1016/j.jsurg.2012.11.005.
Aggarwal R, Moorthy K, Darzi A. Laparoscopic skills training and assessment. Br J Surg. 2004;91:1549–58.
Sleiman Z, Atallah E, Rassi E, et al. Validation study of a portable home trainer using a pad for laparoscopic practice. Surg Innov. 2017;24:284–8. https://doi.org/10.1177/1553350617692481.
Bellows CF, Smith AA. Laparoscopic skills training of surgical residents: a comparison of two proficiency-based independent approaches. Mini-invasive Surg. 2017;1:126–32. https://doi.org/10.20517/2574-1225.2017.12.
Kantartzis K, Sutkin G, Winger D, et al. Introduction of laparoscopic sacral colpopexy to a fellowship training program. Int Urogynecol J. 2013;24:1877–81. https://doi.org/10.1007/s00192-013-2085-z.
Enani G, Watanabe Y, McKendy KM, et al. What are the training gaps for acquiring laparoscopic suturing skills? J Surg Educ. 2017;74:656–62. https://doi.org/10.1016/j.jsurg.2016.12.004.
Nezhat CH, Nezhat F, Nezhat C. Laparoscopic sacral colpopexy for vaginal vault prolapse. Obstet Gynecol. 1994;84:885–8.
Vandendriessche D, Giraudet G, Lucot JP, et al. Impact of laparoscopic sacrocolpopexy learning curve on operative time, perioperative complications and short term results. Eur J Obstet Gynecol Reprod Biol. 2015;191:84–9. https://doi.org/10.1016/j.ejogrb.2015.05.013.
Claerhout F, Roovers JP, Lewi P, et al. Implementation of laparoscopic sacrocolpopexy – a single centre’s experience. Int Urogynecol J. 2009;20:1119–25. https://doi.org/10.1007/s00192-009-0914-x.
Surgical Female Pelvic Trainer (SFPT) Mk 2. Limbs and Things, Bristol, United Kingdom, 2017. Available from: https://assets.limbsandthings.com/uploads/SFPT_UK_WEB.pdf. Accessed 10 Sept 2018.
Tunitsky-Bitton E, King CR, Ridgeway B, Barber MD, Lee T, Muffly T, et al. Development and validation of a laparoscopic sacrocolpopexy simulation model for surgical training. J Minim Invasive Gynecol. 2014;21:612–8. https://doi.org/10.1016/j.jmig.2013.12.124.
Acknowledgements
Present work was presented as a conference abstract at ESGE 27th Annual Congress in Vienna, Austria, in October 2018. We would like to thank our co-workers at the Department of General Gynecology and Urogynecology for their support during development of our pelvic models and Gregor Moleh for his help with the graphic material editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Serdinšek, T., Andrić, B.Ž. & But, I. A new affordable and easy-to-make pelvic model for training in complex urogynecological laparoscopic procedures. Int Urogynecol J 30, 1497–1501 (2019). https://doi.org/10.1007/s00192-018-3803-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-018-3803-3