Abstract
Introduction and hypothesis
To compare postoperative rates of stress urinary incontinence (SUI) in patients with pelvic organ prolapse and SUI undergoing abdominal sacrocolpopexy (ASC) with Burch colposuspension or a transobturator tape (TOT) sling.
Methods
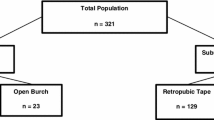
In this retrospective cohort study, medical records of 117 patients who underwent ASC with Burch (n = 60) or TOT (n = 57) between 2008 and 2010 at NYU Winthrop Hospital were assessed. Preoperative evaluation included history, physical examination, cough stress test (CST), and multichannel urodynamic studies (MUDS). Primary outcomes were postoperative continence at follow-up up to 12 weeks. Patients considered incontinent reported symptoms of SUI and had a positive CST or MUDS. Secondary outcomes included intra- and postoperative complications. Associations were analyzed by Fisher’s exact, McNemar’s and Wilcoxon-Mann-Whitney tests.
Results
The groups were similar regarding age, BMI, parity, Valsalva leak point pressure (VLPP), and prior abdominal surgery (p = 0.07–0.76). They differed regarding preoperative SUI diagnosed by self-reported symptoms, CST, or MUDS (TOT 89.5–94.7%, Burch 60.7–76.3%, p < 0.0001–0.007). The TOT group had lower rates of postoperative SUI (TOT 12.5%, Burch 30%, OR = 0.15, 95% CI 0.04, 0.62). Relative risk reduction (RRR) in postoperative SUI for the TOT group compared with the Burch group was 79%–86%. There were no differences concerning intra- and postoperative complications. The Burch group had a higher rate of reoperation for persistent/recurrent SUI (Burch 25%, TOT 12% p = 0.078).
Conclusions
The TOT group experienced a greater reduction in postoperative incontinence, and the Burch group underwent more repeat surgeries. The TOT sling may be superior in patients undergoing concomitant ASC.
Similar content being viewed by others
References
Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J. 2010;21:5–26. https://doi.org/10.1007/s00192-009-0976-9.
Bai SW, Jeon MJ, Kim JY, Chung KA, Kim SK, Park KH. Relationship between stress urinary incontinence and pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2002;13(4):256. https://doi.org/10.1007/s001920200053.
Maher C, Feiner B, Baessler K, Schmid C. Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev. 2013;4:CD004014. https://doi.org/10.1002/14651858.CD004014.pub5.
Ghoniem G, Hammett J. Female pelvic medicine and reconstructive surgery practice patterns: IUGA member survey. Int Urogynecol J. 2015;26(10):1489–94. https://doi.org/10.1007/s00192-015-2734-5.
Davila GW, Ghoniem GM, Kapoor DS, Contreras-Ortiz O. Pelvic floor dysfunction management practice patterns: a survey of members of the international urogynecological association. Int Urogynecol J Pelvic Floor Dysfunct. 2002;13(5):319–25. https://doi.org/10.1007/s001920200069.
Brubaker L, Cundiff G, Fine P, et al. A randomized trial of colpopexy and urinary reduction efforts (CARE): design and methods. Control Clin Trials. 2003;24(5):629–42.
Cosson M, Boukerrou M, Narducci F, Occelli B, Querleu D, Crépin G. Long-term results of the Burch procedure combined with abdominal sacrocolpopexy for treatment of vault prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2003;14(2):104–7. https://doi.org/10.1007/s00192-002-1028-x.
Brubaker L, Cundiff GW, Fine P, et al. Abdominal sacrocolpopexy with Burch colposuspension to reduce urinary stress incontinence. N Engl J Med. 2006;354(15):1557–66. https://doi.org/10.1056/NEJMoa054208.
Burgio KL, Nygaard IE, Richter HE, et al. Bladder symptoms 1 year after abdominal sacrocolpopexy with and without Burch colposuspension in women without preoperative stress incontinence symptoms. Am J Obstet Gynecol. 2007;197(6):647.e1-6. https://doi.org/10.1016/j.ajog.2007.08.048.
Brubaker L, Nygaard I, Richter HE, et al. Two-year outcomes after sacrocolpopexy with and without Burch to prevent stress urinary incontinence. Obstet Gynecol. 2008;112(1):49–55. https://doi.org/10.1097/AOG.0b013e3181778d2a.
Costantini E, Lazzeri M, Bini V, Del Zingaro M, Zucchi A, Porena M. Burch colposuspension does not provide any additional benefit to pelvic organ prolapse repair in patients with urinary incontinence: a randomized surgical trial. J Urol. 2008;180(3):1007–12. https://doi.org/10.1016/j.juro.2008.05.023.
Costantini E, Lazzeri M, Bini V, Del Zingaro M, Frumenzio E, Porena M. Pelvic organ prolapse repair with and without concomitant Burch colposuspension in incontinent women: a randomized controlled trial with at least 5-year followup. Obstet Gynecol Int. 2012;2012:967923. https://doi.org/10.1155/2012/967923.
Lapitan MC, Cody JD. Open retropubic colposuspension for urinary incontinence in women. Cochrane Database Syst Rev. 2016;2:CD002912. https://doi.org/10.1002/14651858.CD002912.pub6.
Holdø B, Verelst M, Svenningsen R, Milsom I, Skjeldestad FE. Long-term clinical outcomes with the retropubic tension-free vaginal tape (TVT) procedure compared to Burch colposuspension for correcting stress urinary incontinence (SUI). Int Urogynecol J. 2017;28(11):1739–46. https://doi.org/10.1007/s00192-017-3345-0.
Ford AA, Rogerson L, Cody JD, Aluko P, Ogah JA. Mid-urethral sling operations for stress urinary incontinence in women. Cochrane Database Syst Rev. 2017;7:CD006375. https://doi.org/10.1002/14651858.CD006375.pub4.
Trabuco EC, Linder BJ, Klingele CJ, Blandon RE, Occhino JA, Weaver AL, et al. Two-year results of Burch compared with midurethral sling with sacrocolpopexy: a randomized controlled trial. Obstet Gynecol. 2018;131(1):31–8. https://doi.org/10.1097/AOG.0000000000002415.
Delorme E. Transobturator urethral suspension: mini-invasive procedure in the treatment of stress urinary incontinence in women. Prog Urol. 2001;11(6):1306–13.
Burch JC. Urethrovaginal fixation to Cooper’s ligament for correction of stress incontinence, cystocele, and prolapse. Am J Obstet Gynecol. 1961;81:281–90.
Nygaard I, Brubaker L, Zyczynski HM, Cundiff G, Richter H, Gantz M, et al. Long-term outcomes following abdominal sacrocolpopexy for pelvic organ prolapse. JAMA. 2013;309(19):2016–24. https://doi.org/10.1001/jama.2013.4919.
Trabuco EC, Klingele CJ, Blandon RE, Occhino JA, Weaver AL, McGree ME, et al. Burch retropubic urethropexy compared with midurethral sling with concurrent sacrocolpopexy: a randomized controlled trial. Obstet Gynecol. 2016;128(4):828–35. https://doi.org/10.1097/AOG.0000000000001651.
Magon N, Chopra SVSM. Transobturator tape in treatment of stress urinary incontinence: it is time for a new gold standard. North Am J Med Sci. 2012;4(5):226–30. https://doi.org/10.4103/1947-2714.95905.
Mayekar RV, Bhosale AA, Kandhari KV, Nandanwar YS, Shaikh SS. A study of transobturator tape in stress urinary incontinence. Urol Ann. 2017;9(1):9–12. https://doi.org/10.4103/0974-7796.198867.
Abdel-Fattah M, Cao G, Mostafa A. Long-term outcomes for transobturator tension-free vaginal tapes in women with urodynamic mixed urinary incontinence. Neurourol Urodyn. 2017;36(4):902–8. https://doi.org/10.1002/nau.23192.
Al-Zahrani AA, Gajewski J. Long-term patient satisfaction after retropubic and transobturator mid-urethral slings for female stress urinary incontinence. J Obstet Gynaecol Res. 2016;42(9):1180–5. https://doi.org/10.1111/jog.13035.
Leone Roberti Maggiore U, Finazzi Agrò E, Soligo M, Li Marzi V, Digesu A, Serati M. Long-term outcomes of TOT and TVT procedures for the treatment of female stress urinary incontinence: a systematic review and meta-analysis. Int Urogynecol J. 2017;28(8):1119–30. https://doi.org/10.1007/s00192-017-3275-x.
Moon YJ, Jeon MJ, Kim SK, Bai SW. Comparison of Burch colposuspension and transoturator tape when combined with abdominal sacrocolpopexy. Int J Gynaecol Obstet. 2011;112(2):122–5. https://doi.org/10.1016/j.ijgo.2010.08.017.
Law TSM, Cheung RYK, Chung TKH, Chan SSC. Efficacy and outcomes of transobturator tension-free vaginal tape with or without concomitant pelvic floor repair surgery for urinary stress incontinence: five-year follow-up. Hong Kong Med J. 2015;21(4):333–8. https://doi.org/10.12809/hkmj144397.
Jeon MJ, Kim JY, Moon YJ, Bai SW, Yoo EH. Two-year urinary outcomes of sacrocolpopexy with or without transobturator tape: results of a prolapse reduction stress test-based approach. Int Urogynecol J. 2014;25(11):1517–22. https://doi.org/10.1007/s00192-014-2410-1.
Richardson ML, Elliot CS, Shaw JG, Comiter CV, Chen B, Sokol ER. To sling or not to sling at time of abdominal sacrocolpopexy: a cost-effective analysis. J Urol. 2013;190(4):1306–12. https://doi.org/10.1016/j.juro.2013.03.046.
Tubre RW, Padmanabhan P, Frilot CF, Porta W, Gomelsky A. Outcomes of three sling procedures at the time of abdominal sacral colpopexy. Neurourol Urodyn. 2017;36(2):482–5. https://doi.org/10.1002/nau.22959.
Acknowledgments
Special thanks to Dr. Anthony Vintzileos for his support and Dr. Salma Rahimi for her assistance with data collection.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Lazarou, G., Minis, E. & Grigorescu, B. Outcomes of stress urinary incontinence in women undergoing TOT versus Burch colposuspension with abdominal sacrocolpopexy. Int Urogynecol J 30, 245–250 (2019). https://doi.org/10.1007/s00192-018-3668-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-018-3668-5